Chapter 1 Rationale for Dental Implants
The goal of modern dentistry is to restore the patient to normal contour, function, comfort, esthetics, speech, and health, whether by removing caries from a tooth or replacing several teeth. What makes implant dentistry unique is the ability to achieve this goal, regardless of the atrophy, disease, or injury of the stomatognathic system.1 However, the more teeth a patient is missing, the more challenging this task becomes. As a result of continued research, diagnostic tools, treatment planning, implant designs, materials, and techniques, predictable success is now a reality for the rehabilitation of many challenging clinical situations.
The number of dental implants used in the United States increased more than tenfold from 1983 to 2002, and another fivefold from 2000 to 2005. More than 1 million dental implants are inserted each year. This number continues to increase steadily, with almost $550 million of implant products sold to North American dentists in 2005, compared with $10 million in 1983, with an expected yearly growth sustained at 12% to 15% for the next several years.2,3 When bone grafting materials are included in implant products, it is estimated the field of implant dentistry will sell $10 billion in services to patients by 2010.4 More than 90% of interfacing surgical specialty dentists currently provide dental implant treatment on a routine basis in their practices, 90% of prosthodontists restore implants routinely, and more than 80% of general dentists have used implants to support fixed and removable prostheses, compared with 65% 15 years ago.5–9
EFFECTS OF AN AGING POPULATION
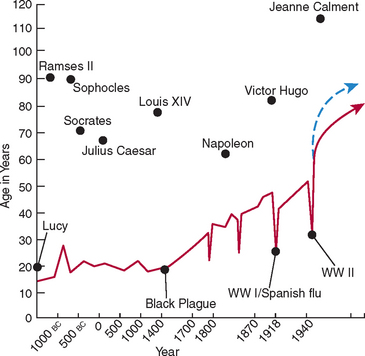
According to the literature, age is directly related to every indicator of tooth loss.10,11 Therefore the aging population is an important factor to consider in implant dentistry. When Alexander the Great conquered the ancient world, he was only 17 years old. However, life expectancy at that time was only 22 years of age. From 1 000 bc to ad 1 800, life span remained less than 30 years (Figure 1-1). Since 1960, the increase in life expectancy has been more rapid than at any other time in history. In 1980, 30% of the U.S. population was older than age 45, 21% was older than 50, and 11% was older than 65. In 1995, 15 years later, all these individuals were older than age 60. The group older than age 65 is projected to increase from 12% in 2000 to more than 20% of the population within the next 25 years12 (Figure 1-2).
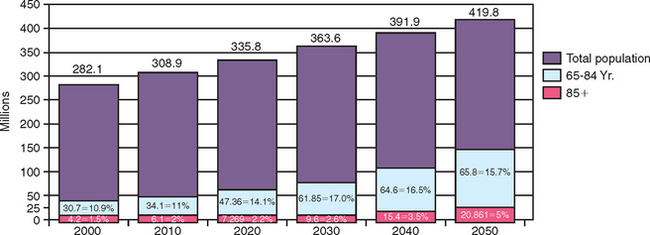
In addition, not only is the percentage of the population over 65 years increasing, but the overall population is also increasing. The population in 2000 was 282 million and is projected to increase 49% to 420 million by 2050. Considering the effect of both a population increase and a greater percentage of that population being older than age 65, a dramatic overall increase in patient numbers can be expected. In 2003, 35 million people were older than age 65. This number is expected to increase 87% by 2025, resulting in almost 70 million people being older than age 6513 (Figure 1-3). Because older people are more likely to be missing teeth, the need for implant dentistry will dramatically increase over the next several decades.
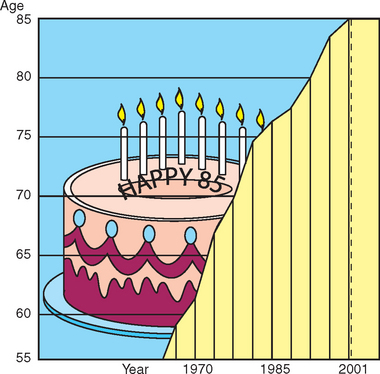
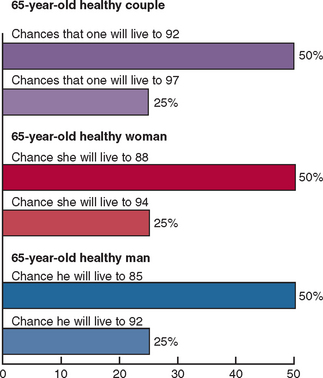
Life expectancy has increased significantly past the age of retirement. In 1965 the average life span was 65 years; in 1990 it was 78 years. Life expectancy in 2001 was 85 years for a nonsmoking individual of normal weight.14 A 65-year-old person can now expect to live more than 20 additional years, and an 80 year old can expect to live 9.5 more years15–17 (Figure 1-4). Women represent two thirds of the population older than age 65.18 It is not unusual for a 70-year-old patient to ask, “Is it worth it for me to spend $30,000 to repair my mouth at my age?” The response should be very positive, as the patient’s life expectancy will extend for two more decades, and their current oral situation will normally become worse if not corrected.
Social pleasures, including dining and dating, continue throughout advanced life. In the past, geriatric dentistry meant inexpensive treatment emphasizing nonsurgical approaches. The poverty rate for the elderly, however, is less than 10%, and retiree median income has grown 8% in recent years. According to the last census, the median net worth of retirees is 15 times the net worth of those younger than age 35 and three times as high as “working families” ages 35 to 44 years.18,19 Close to 20% of today’s retirees have a net worth of more than a quarter of a million dollars. Today, the full scope of dental services for elderly patients is increasing in importance to both the public and the profession because of the increasing age of our society. Treatment alternatives that consider fixed prostheses with implant support should be presented to almost any patient. Only when all treatment options are discussed can a person’s desires related to the benefit of implant dentistry be truly appreciated.
Dental services for elderly patients clearly represent a growing demand for the dental profession. In 2000, 28.8% of all income from a dentist came from patients age 60 and older—a group that represented only 12% of income in 1988. When the dentist is older than age 40, income from those older patients represents 64.3% of the dentist’s income, whereas in 1988 it was 30.3%.20 Clearly, the demographics of our population have dramatically changed the economics of dental practice.
AGE-RELATED TOOTH LOSS
Single-Tooth Edentulism
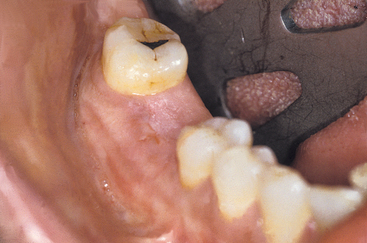
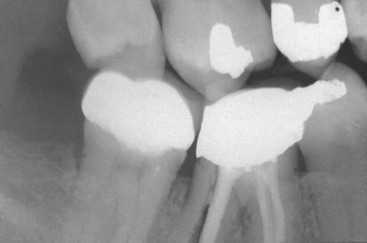
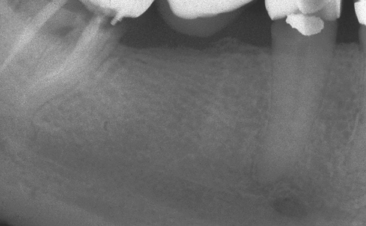
The posterior regions of the mouth often require the replacement of a single tooth21–23 (Figure 1-5). The first molars are the first permanent tooth to erupt in the mouth and, unfortunately, are often the first teeth lost as a result of decay, failed endodontic therapy or fracture (usually after endodontics). They are important teeth for maintenance of the arch form and proper occlusal schemes. In addition, the adult patient often has one or more crowns, as a consequence of previous larger restorations required to repair the integrity of the tooth. Longevity reports of crowns have yielded very disparate results. The mean life span at failure has been reported as 10.3 years. Other reports range from a 3% failure rate at 23 years to a 20% failure rate at 3 years. The primary cause of failure of the crown is caries followed by endodontic therapy.24–33 The tooth is at risk for extraction as a result of these complications, which are the leading causes of single posterior tooth loss in the adult (Figure 1-6). It has been estimated that a $425 crown for a 22-year-old patient will cost $12,000 during the patient’s lifetime to replace and/or repair.26
Fixed Partial Dentures
In the United States, 70% of the population is missing at least one tooth. Almost 30% of the 50 to 59 year olds examined in a U.S. National Survey exhibited either single or multiple edentulous spaces bordered by natural teeth. In 1990, more than 4 million FPDs were placed in the United States.23–25 Treatments to replace single teeth with a fixed prosthesis represent 7% of the annual dental reimbursement from insurance companies and more than $3 billion each year. Only one third of our population in the United States has dental insurance and of those who do, only 50% of treatment costs are reimbursed. Hence, the entire three- to four-unit FPD costs in the United States may approach more than $10 billion each year.
A three-unit FPD also presents survival limitations to the restoration and, more importantly, to the abutment teeth.30,32 In an evaluation of 42 reports since 1970, Creugers et al. calculated a 74% survival rate for FPDs for 15 years.29 Mean life spans of 9.6 to 10.3 years have been reported by Walton et al.31 and Schwartz et al.,24 respectively. However, reports are very inconsistent, with as little as 3% loss over 23 years to 20% loss over 3 years.23–32 Caries and endodontic failure of the abutment teeth are the most common causes of prostheses failure.31,32 Up to 15% of abutment teeth for an FPD require endodontic therapy, compared with 3% of nonabutment teeth that have crown preparations. The long-term periodontal health of the abutment teeth, including bone loss, may also be at greater risk.29
Unfavorable outcomes of FPD failure include both the need to replace the failed prosthesis and the loss of an abutment and the need for additional pontics and abutment teeth in the replacement bridge. The abutment teeth of an FPD may be lost at rates as high as 30% within 14 years.30 Approximately 8% to 12% of the abutment teeth holding an FPD are lost within 10 years. The most common reason for single tooth loss is endodontic failure or fracture of a tooth (usually after endodontic therapy). Because 15% of abutment teeth require endodontics, and root canal therapy may be 90% successful at the 8-year mark, abutment teeth are at increased risk of loss. In addition, abutment teeth are more prone to caries when splinted together with an intermediary pontic. Individual crowns have decay rates below 2%; however, the risk of caries in abutment teeth is approximately 20%, mainly because the pontic region acts as a plaque reservoir. The carious lesion at the crown margin may cause structural failure, even if endodontic treatment is possible (Figure 1-7).
Almost 80% of abutments prepared for a three-unit FPD have no existing or only minimal restorations.34 Rather than removing sound tooth structure and crowning two or more teeth—thus increasing the risk of decay and endodontic therapy (and splinting teeth together with pontics, which have the potential to cause additional tooth loss)—a dental implant may replace the single tooth (Box 1-1).
Single-Tooth Implants
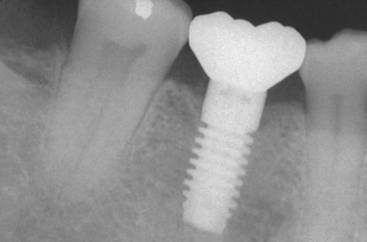
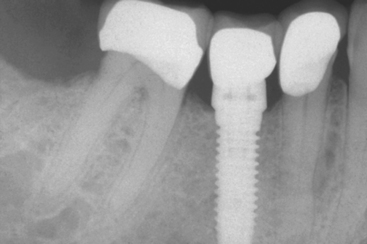
A treatment option to replace a posterior single missing tooth is a single-tooth implant (Figure 1-8). For years, patients were advised to put their desires aside and accept the limitations of an FPD. However, many feel the most natural method to replace a tooth is to use an implant, rather than preparing adjacent teeth and joining them together with a prosthesis. The primary reasons for suggesting the FPD were its clinical ease and reduced treatment time. However, if this concept were expanded, extractions would replace endodontics and dentures could even replace orthodontics. The primary reason to suggest or perform a treatment should not be related to treatment time or difficulty of the procedure, but instead should consider the best possible long-term solution for each individual.
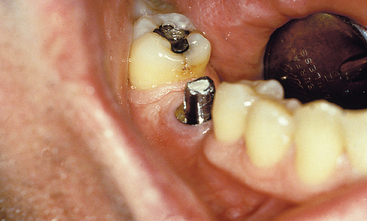
Figure 1-8 A single-tooth implant in the posterior region of the mouth is most often the treatment of choice.
From 1993 to the present, single-tooth implant survival reports have validated this procedure as the most predictable method of tooth replacement. There are more refereed reports in the literature for single-tooth implant replacement than for any other method of tooth replacement,35–47 and all reports demonstrate a higher survival rate for single-tooth implants. Goodacre et al. performed a Medline literature review from 1980 to 2001 and found the single-tooth implant success rate to be in the range of 97%—higher than any other implant restoration.35 In 1995, Haas et al. reported on 76 single-tooth implants over a 6-year period and found a 97% survival rate and a 2.6% implant loss.38 Fugazzotto evaluated 1472 implants over a 13-year period and found a 97% survival rate during that period.39
Although posterior single-tooth replacement is a relatively new treatment alternative, many studies have been published since 1990, and survival rates reported range from a low of 94.6% to a high of 100% for 1 to 15 years.35–45 The median of these reports is a 2.8% implant loss with a mode of 5 years. In comparison, FPD failure rates may be as high as 20% within 3 years, and 50% rates at 10 years are expected. As a result, the single-tooth implant exhibits the highest survival rates presented for single-tooth replacement. As important, no reports indicate a loss of an adjacent tooth, which is a considerable advantage. On the other hand, the longevity of the implant crown has not been adequately determined, as these reports do not extend as long as those of other treatment options.
Despite some limitations and obvious clinical challenges, the single-tooth implant represents the treatment of choice from both a health and value standpoint. When adjacent teeth are healthy, or when the patient refuses their preparation for the fabrication of a traditional three-unit fixed partial restoration, a posterior single-tooth implant is an excellent solution (Figure 1-9). Health-related advantages of this modality over a fixed partial restoration are listed in Box 1-2 and include a decreased risk of decay and periodontal disease, decreased risk of abutment tooth loss from endodontic failure or caries, and improved esthetics (Figure 1-10). Psychological advantages, especially with congenitally missing teeth or the loss of a tooth after a crown restoration, are significant as well. These advantages are so significant to the health and periodontal condition of the adjacent teeth and maintenance of the arch form that the single-tooth implant has become the treatment of choice in most situations. Economical considerations may play in disfavor of the implant restoration only during the first 7 years. The single-tooth implant becomes more advantageous economically, not only for health considerations, after the break-even point of 7 years, at which time the patient will not need a replacement prosthesis. The savings will offset the initial higher cost.47
Partial Edentulism
The prevalence of partial edentulism is also of interest because a growing number of implants are used in these patients. A 1988 to 1991 survey in the United States found that only 30% of these patients had all 28 teeth. Partially dentate patients had an average of 23.5 teeth.10,23,48 In the 1999 to 2002 follow-up survey, the average number of missing teeth was fewer than two of 28 teeth for the 20- to 39-year-old group. However, this number rapidly increased to an average of nine teeth missing in adults older than age 60. Partially edentulous seniors older than age 60 age have lost an average of 10 teeth, with older seniors having lost three more teeth than the younger seniors. Statistics for partial edentulism are similar for both men and women. The greatest transition from an intact dental arch to a partially edentulous condition in the 1987 study occurred in the 35- to 54-year-old group.20,23 The growth rate of this baby boomer portion of the population was approximately 30% in 1982 and is continuing to increase, more than any other age group. For example, in 1982 the baby boomer age group (born from 1946 to 1964) increased from 39 million Americans to 79 million in 2005. Although the number of teeth missing per patient may seem to decrease, the overall number of missing teeth will continue to increase. Therefore the need for implant services in partially edentulous patients will dramatically increase during the next several decades.15
The most common missing teeth are molars.22 Partial free-end edentulism is of particular concern because in these patients, teeth are often replaced with removable partial prostheses. This condition is rarely found in persons younger than age 25. Mandibular free-end edentulism is greater than its maxillary counterpart in all age groups. Unilateral free-end edentulism is more common than bilateral edentulism in both maxillary and mandibular arches in the younger age groups (ages 25 to 44). About 13.5 million persons in these younger age groups have free-end edentulism in either arch.
In 45- to 54-year-old patients, 31.3% have mandibular free-end edentulism and 13.6% have free-end edentulism in the maxillary arch. Approximately 9.9 million persons in the 45- to 54-year-old group have at least one free-end edentulous quadrant, and almost half of these have bilateral partial edentulism.11 The pattern of posterior edentulism evolves in the 55- to 64-year-old group, in which 35% of mandibular arches show free-end edentulism, compared with 18% of maxillary arches. As a result, approximately 11 million individuals in this age group are potential candidates for implants. An additional 10 million show partial free-end edentulism at age 65 or older. Additional studies have documented that in the population of noninstitutionalized U.S. civilians, 1 of 5 had a removable prosthesis of some type.49–51 The total number of potential patients in the U.S. survey with at least one quadrant of posterior missing teeth is more than 44 million people.11 If each of these arches requires three implants to support a fixed prosthesis, 132 million implants added to the 192 million for edentulous patients would be required.
Total Edentulism
Edentulism is not an eventual, healthy occurrence in an adult population. Rather it is most often the result of repeated tooth extractions from the combined pathologic processes of dental caries, periodontal disease, or a method to reduce the costs associated with dental treatment.52–54 Similar to other pathologic outcomes of disease, the occurrence of total loss of teeth is directly related to the age of the patient. The rate of edentulism increases at 4% per 10 years in early adult years and increases to more than 10% per decade after age 70.54
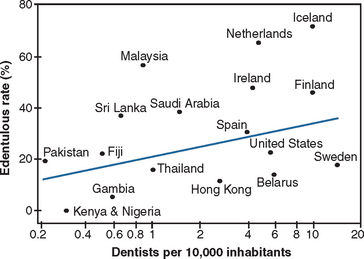
The average total edentulous rate around the world is 20% at age 60, although there is wide disparity from the countries with the highest and lowest rates54 (Figure 1-11). For example, from the 65- to 74-year age group, the total edentulous rate in Kenya and Nigeria was 0%, whereas the Netherlands and Iceland have a 65.4% and 71.5% rate, respectively. The edentulous Canadian rate was 47% at 65 to age 69 and 58% from ages 70 to 98 (with Quebec at 67% for those older than age 65, compared with Ontario with a 41% rate). One of the main factors influencing total edentulism was the level of education. In data from the Canadian Health Promotion Survey from 1990, the least educated had an edentulous rate of 50%, whereas those with a college education had a low 4% rate.55 The United States showed a similar pattern in the period 1988 to 1994, with an edentulous rate of 22% for those with less than 8 years of education, 12% for those with 9 to 11 years of school, 8% for those with 12 years of school, and 5% for individuals with more than 12 years of education.48 Income is often related to education and may also play a role in the rate of edentulism.
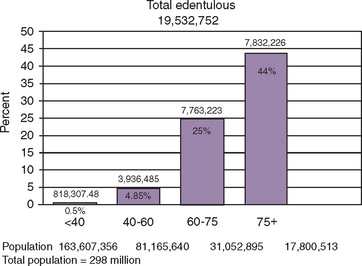
The 1999 to 2002 survey found that total edentulism of both arches occurred in 7.7% of the adult population in the United States, or almost 20 million people.48 The present younger population is benefiting from today’s advanced knowledge and restorative techniques. Edentulism has been noted in 5% of employed adults ages 40 to 44, gradually increasing to 26% at age 65, and almost 44% in seniors older than age 7510 (Figure 1-12). As expected, older persons are more likely to be missing all their teeth. Gender was not found to be associated with tooth retention or tooth loss once adjustments were made for age.
The percentages of one- or two-arch edentulism translate into more than 30 million people or about 17% of the entire U.S. adult population.17 To put these numbers in perspective, 30 million people represent approximately the entire U.S. African American population, or the whole population of Canada. Although the edentulism rate is decreasing every decade, the elderly population is rising so rapidly that the adult population in need of one or two complete dentures will actually increase from 33.6 million adults in 1991 to 37.9 million adults in 2020. The total number of edentulous arches is estimated at 56.5 million in 2000, 59.3 million in 2010, and 61 million in 2020.56 Complete edentulism, therefore, remains a significant concern, and affected patients often require implant dentistry to solve several related problems. If four implants were used to help support each complete edentulous arch in 2000, a total of 226 million implants would be required. Yet only 1 million implants were inserted for all patient treatment (partially or completely edentulous) each year. Almost 70% of dentists spend less than 1% to 5% of their treatment time on edentulous patients, leaving a great unfulfilled need for implant dentistry.
ANATOMICAL CONSEQUENCES OF EDENTULISM
Consequences on the Bony Structures
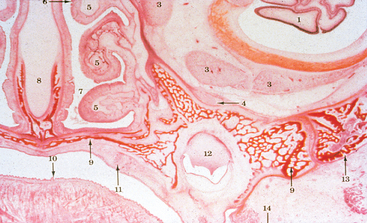
Basal bone forms the dental skeletal structure, contains most of the muscle attachments, and begins to form in the fetus before teeth develop. Alveolar bone first appears when Hertwig’s root sheath of the tooth bud evolves57 (Figure 1-13). The alveolar bone does not form in the absence of primary or secondary tooth development. The close relationship between the tooth and the alveolar process continues throughout life. Wolff’s law (1892) states that bone remodels in relationship to the forces applied.58 Every time the function of bone is modified, a definite change occurs in the internal architecture and external configuration.59 In dentistry, the consequences of complete edentulous and remaining bone volume was noted by Misch in 1922, where he described the skeletal structure of a 90-year-old woman without teeth for several decades.60
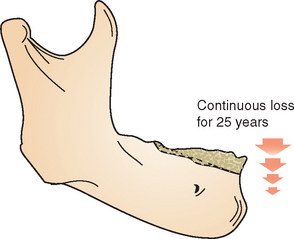
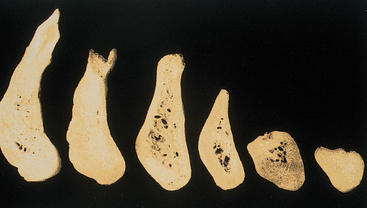
Bone needs stimulation to maintain its form and density. Roberts et al.61 report that a 4% strain to the skeletal system maintains bone and helps balance the resorption and formation phenomena. Teeth transmit compressive and tensile forces to the surrounding bone. These forces have been measured as a piezoelectric effect in the imperfect crystals of durapatite that compose the inorganic portion of bone.62 When a tooth is lost, the lack of stimulation to the residual bone causes a decrease in trabeculae and bone density in the area, with loss in external width, then height, of the bone volume.63 There is a 25% decrease in width of bone during the first year after tooth loss and an overall 4-mm decrease in height during the first year after extractions for an immediate denture.64 In a longitudinal 25-year study of edentulous patients, lateral cephalograms demonstrated continued bone loss during this time span; a fourfold greater loss was observed in the mandible65 (Figure 1-14). However, because initially the mandible height is twice that of the maxilla, maxillary bone loss is also significant in the long-term edentulous patient.
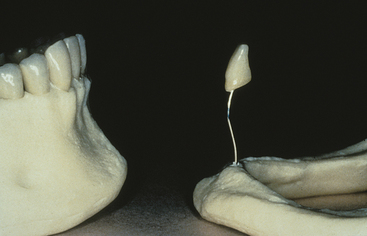
A tooth is necessary to the development of alveolar bone, and stimulation of this bone is required to maintain its density and volume. A removable denture (complete or partial) does not stimulate and maintain bone; rather, it accelerates bone loss. The load from mastication is transferred to the bone surface only, not the whole bone. As a result, blood supply is reduced and total bone volume loss occurs.66 This issue, which is of utmost importance, has been observed but not addressed in the past by traditional dentistry. Doctors most often overlook the insidious bone loss that will occur after tooth extraction. The patient is often not educated about the anatomical changes and the potential consequences of continued bone loss. The bone loss accelerates when the patient wears a poorly fitting soft tissue-borne prosthesis. Patients do not understand that bone is being lost over time and at a greater rate beneath poorly fitting dentures (Figure 1-15). Patients do not return for regular visits for evaluation of their condition; instead, they return after several years when denture teeth are worn down or can no longer be tolerated. Hence the traditional method of tooth replacement often affects bone loss in a manner not sufficiently considered by the doctor and the patient. The doctor should inform the patient that a denture replaces more bone and soft tissue than teeth, and every 5 years a reline or new denture is suggested to replace the additional bone loss by atrophy (Figure 1-16).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses