1
Oral embryology, histology and anatomy
- Oral embryology
- Early tooth development
- Development of the dental tissues
- Histology of oral tissues
- Histology of dental tissues
- Oral anatomy
- Tooth morphology
Introduction
A basic understanding of the development, structure and relationship of the tissues and structures which constitute the oral cavity and its associated environment is fundamental to the practice of clinical dentistry. It enables the clinician better to appreciate how subsequent pathology change may be influenced by adjacent anatomical structures or tissues and therefore helps to provide a better understanding of the rationale for potential treatment options.
Oral embryology
Development of the face
4 weeks of intrauterine life
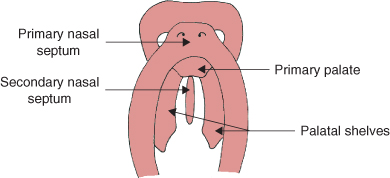
The primitive oral cavity, which is known as the stomodeum, develops five facial swellings (Figure 1.1): one frontonasal process, two maxillary processes and two mandibular processes. The frontonasal process eventually develops to form the forehead, nose and philtrum; the two maxillary processes form the middle face and upper lip; and the two mandibular processes form the mandible and lower lip.
Development of the palate
5 weeks of intrauterine life
The frontonasal process produces the medial and lateral nasal processes. Failure of fusion of the maxillary and medial nasal processes produces a cleft lip.
6 weeks of intrauterine life
The primary nasal septum and primary palate are formed, both derived from the fronto-nasal process (Figure 1.2). Two lateral palatal shelves develop behind the primary palate from the maxillary process. A secondary nasal septum grows behind the primary nasal septum from the roof of the primitive oral cavity dividing the nasal cavity into two.
8 weeks of intrauterine life
The palatal shelves contact each other forming the secondary palate; the shelves also contact anteriorly with the primary palate dividing the oral and nasal cavities.
Development of the jaws
The mandible
6 weeks of intrauterine life
The mandible appears as a band of dense fibrous tissue known a Meckel’s cartilage; this cartilage provides a framework around which the bone will form.
7 weeks of intrauterine life
Bone formation commences at the mental foramen area and begins to spread backwards, forwards and upwards outlining the future body of the mandible. As the bone grows backwards, two small secondary cartilages develop, which eventually form the condyle and coronoid processes. Anteriorly, the left and right mandibular plate of bone is separated by cartilage at the mandibular symphysis; these two plates eventually unite to form a single bone approximately 2 years after birth. The upward growth of bone increases the height of the mandible forming the alveolar process which will surround the developing tooth germ.
Figure 1.1 Facial development at 4 weeks of intrauterine life.
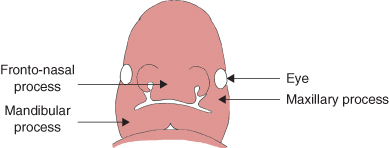
Figure 1.2 Palatal development at 6 weeks of intrauterine life.
The maxilla
8 weeks of intrauterine life
Ossification of the maxilla commences at the area of the developing primary (deciduous) canines; from this area, bone formation spreads, developing the maxillary processes: palatal, zygomatic, frontal and alveolar. Growth of the maxilla occurs by remodelling of bone and by sutural growth. The stimulus for sutural bone growth is thought to be related to the tension produced by the displacement of bone. Growth carries the maxilla forwards and downwards as it increases in size.
Early tooth development
Development of primary epithelial band
- The first sign of tooth development occurs at the 6th week of intrauterine life.
- Underneath the oral ectodermal epithelium there is a condensation of mesenchymal cells in areas where teeth will eventually form.
- The ectodermal epithelium thickens in these areas and protrudes into the mesenchymal cells forming the primary epithelial band.
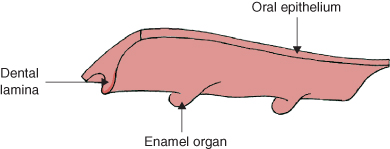
Figure 1.3 Dental lamina showing enamel organs. Reproduced by kind permission of R. Ireland.
Development of the vestibular band and dental lamina
- At 7 weeks of intrauterine life.
- The primary epithelial band develops two processes the vestibular band and the dental lamina.
- The vestibular band forms buccally and will eventually form the vestibule, separating the lips and checks from the teeth and gingivae.
- The dental lamina forms lingually and develops into an arch shape band on which the tooth germs will develop (Figure 1.3).
Development of the tooth germ
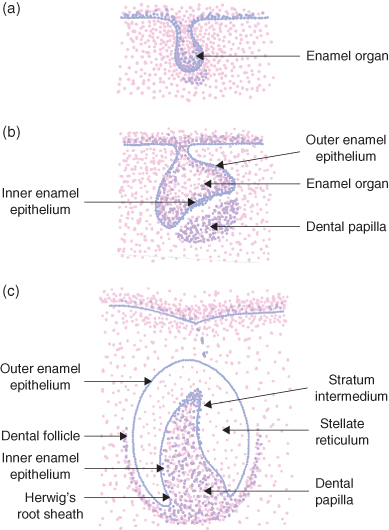
The tooth germ develops in three stages: bud, cap and bell (Figure 1.4).
Bud
At 8 weeks of intrauterine life, clumps of mesenchymal cells induce the dental lamina to form swellings known as enamel organs. Each enamel organ will be responsible for the development of each tooth (Figure 1.4a).
Cap
As the enamel organs grow and increase in size, the inner aspect becomes concave resembling skull caps. By the late cap stage, at 12 weeks of intrauterine life, cells on the inner aspect of the enamel organ change from cuboidal to columnar forming the inner enamel epithelium. The outer layer of cells remains cuboidal and is known as the outer enamel epithelium. (Figure 1.4b)
Beneath the inner enamel epithelium the condensation of mesenchymal cells is termed the dental papilla; this will eventually become the pulp. A fibrous capsule surrounds each enamel organ and this is termed the dental follicle; this will eventually become the periodontal ligament.
Figure 1.4 Stages in the development of the tooth germ.
Bell
By 14 weeks of intrauterine life (Figure 1.4c) the enamel organ consists of the following:
- Inner enamel epithelium:
- Cells lining the inner surface of the enamel organ which are columnar in shape.
- The inner enamel epithelium defines the shape of the crown.
- They will eventually differentiate into enamel forming cells (ameloblasts).
- Stratum intermedium:
- Lies over the inner enamel epithelium.
- Consists of two to three layers of cells.
- Transports nutrients to and from the ameloblasts.
- Stellate reticulum:
- Lies between the stratum intermedium and the outer enamel epithelium.
- It consists of star-shaped cells that protect the underlying dental tissues.
- It also maintains the shape of the tooth.
- Outer enamel epithelium:
- Cells lining the outer surface of the enamel organ. They are cuboidal in shape.
- They maintain the shape of the enamel organ.
- The outer enamel epithelium meets with the internal enamel epithelium at the cervical loop.
- Eventually the inner and outer enamel epithelium grows downwards at the cervical loop forming Hertwig’s root sheath, which maps out the shape of the root.
At the late bell stage the dental lamina disintegrates and is ready for the formation of dental hard tissue. Dentine formation always precedes enamel formation.
Development of the dental tissues
Dentine formation – (dentinogenesis)
- Late bell stage the inner enamel epithelium cells have mapped out the shape of the crown.
- The inner enamel epithelium cells induce cells at the periphery of the dental papilla to form columnar odontoblast cells (dentine-forming cells).
- Odontoblast cells begin to secrete an unmineralised dentine matrix.
- As more dentine matrix is deposited, the odontoblast cells retreat in the direction of the pulp leaving an elongated process known as the odontoblast process.
- The dentine matrix formed prior to mineralisation is termed predentine. A narrow layer of predentine is always present on the surface of the pulp.
- Mineralisation of dentine begins when the predentine is approximately 5 μm thick.
- Spherical zones of hydroxyapatite called calcospherites are formed within the dentine matrix.
- Mineralisation of the dentine matrix starts at random points and eventually these calcospherites fuse together to form mineralised dentine.
- Dentinal tubules form around each odontoblast process (Figure 1.5).
- The odontoblasts retreat in S-shaped curves towards the dental papilla.
- The first layer of mineralised dentine is called mantle dentine and the remaining bulk of the mineralised dentine is known as circumpulpal dentine.
Enamel formation (amelogenesis)
- Immediately after the first layer of dentine is formed, the inner enamel epithelium ameloblast cells (enamel forming cells).
- The ameloblast cell is columnar in shape with its base attached to cells of the stratum intermedium.
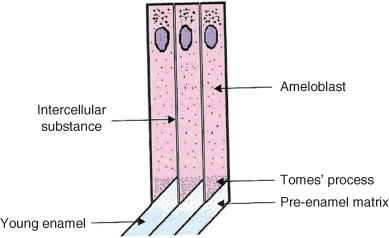
- At the secretory end of ameloblast cells is a pyramidal extension called the Tomes’ process (Figure 1.6).
- The enamel matrix is secreted through the Tomes’ process at the amelodentinal junction.
- Calcium and phosphate ions are secreted into the enamel matrix and mineralisation of enamel occurs immediately, forming hydroxyapatite crystallites.
- As more enamel matrix is secreted and mineralised, the ameloblast cells move away from the amelodentinal junction forming a pattern of crystallites, which are contained within enamel prisms.
- Enamel prisms are also known as enamel rods they run from the amelodentinal junction to the enamel surface.
Figure 1.5 Diagram of odontoblast process and dentine tubules.
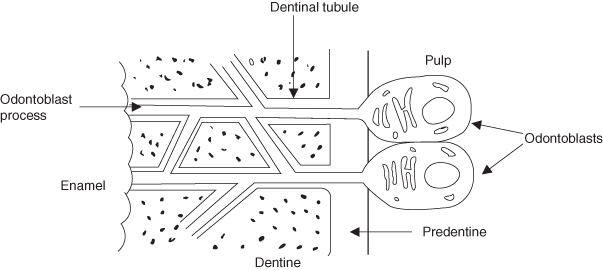
Figure 1.6 Diagram of enamel prism formation showing Tomes processes.
Enamel maturation
- During maturation from pre-enamel to mature enamel, the enamel crystallites increase in size and the organic content is reduced.
- On completion of enamel formation the ameloblast cell loses the Tomes’ process, flattens and becomes the reduced enamel epithelium.
- The reduced enamel epithelium protects the enamel during eruption and will eventually become the junctional epithelium.
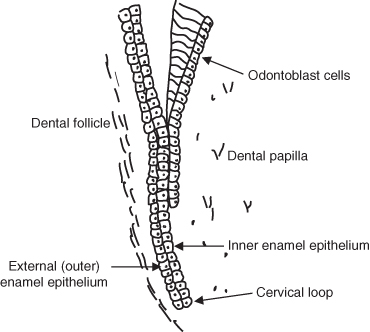
Figure 1.7 Diagram of Hertwig’s root sheath.
Formation of the root
- Occurs when the crown has completed.
- The internal and external enamel epithelium grows downwards at the cervical loop to form a double layered epithelial wall – Hertwig’s root sheath (Figure 1.7).
- The Hertwig’s root sheath grows apically mapping out the shape of the root enclosing the dental papilla.
- The dental follicle lies external to the Hertwig’s root sheath.
Cementum formation (cementogenesis)
- The Hertwig’s root sheath induces the formation of odontoblast cells.
- When root dentine has formed, Hertwig’s root sheath fragments allowing adjacent cells from the dental follicle to come into contact with the root dentine.
- These cells differentiate into cementoblasts (cementum-forming cells).
- Cementoblasts are cuboidal in shape and form a single layer on the surface of the root dentine.
- The cementoblasts secrete cementum matrix and crystallites of hydroxyapatite are deposited in this matrix and mineralisation occurs.
- During formation, a thin layer of unmineralised cementum is always present on the surface; this is known as cementoid.
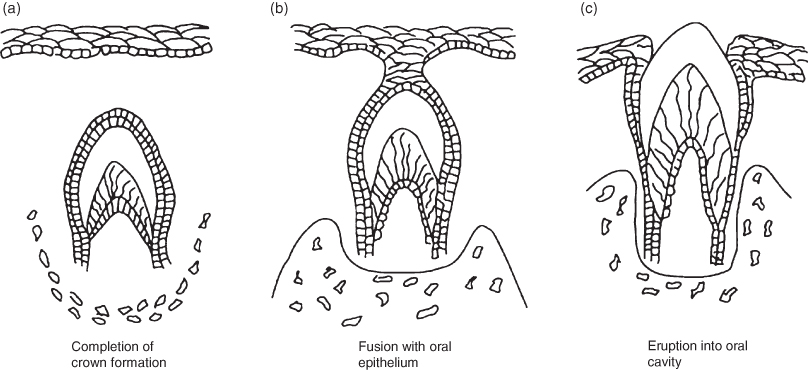
Figure 1.8 Diagram showing phases of tooth eruption.
Formation of the periodontal ligament
- Cells within the dental follicle give rise to fibroblasts that secrete collagen.
- Once cementum formation has begun, collagen fibres within the dental follicle orientate themselves into bundles, which are perpendicular to the root surface.
- These fibres will form the principal fibres of the periodontal ligament.
- The ends of these fibres become embedded in the developing cementum and alveolar bone and are known as Sharpey’s fibres.
Tooth eruption
Tooth eruption is the bodily movement of a tooth from its development position into its functional position in the oral cavity. It can be broken down into two phases; the per-functional eruptive phase and the functional eruptive phase (Figure 1.8).
Prefunctional phase
- During the prefunctional phase, crown formation has completed.
- As root formation begins the developing tooth begins to erupt.
- The overlying alveolar bone is resorbed by osteoclasts and gradually the tooth moves in an axial direction towards the oral cavity.
- The enamel surface of the tooth is covered by the reduced enamel epithelium which fuses with the oral epithelium.
- The pressure from the tip of the tooth breaks down the oral epithelium allowing the tooth to emerge into the oral cavity without any rupturing of blood vessels.
- Once the tooth has emerged, the reduced enamel epithelium is known as the epithelial attachment.
- Tooth eruption continues until the tooth contacts (occludes with) the opposing tooth in the opposite jaw.
Functional eruptive phase
- The functional eruptive phase continues throughout life due to functional changes.
- The alveolar bone continuously remodels in response to tooth movement and enamel wear allowing teeth to maintain contact with each other and with opposing teeth.
Mechanisms of tooth eruption
The eruptive force of tooth eruption is unclear; however, several theories have been put forward although there is little evidence to support them. These are:
- Root growth generates a force beneath the tooth, elevating the tooth towards the oral cavity.
- Remodelling and deposition of the bone beneath the developing tooth pushes the tooth upwards.
- Traction of the periodontal fibres exerts an upward pull on the tooth.
- Cellular proliferation at the base of the pulp creates pressure that pushes the tooth from the dental follicle.
- An increase in tissue fluid or blood pressure generates an eruptive force on the tooth.
The approximate initial calcification and eruption dates are listed in Tables 1.1 and 1.2.
Table 1.1 Approximate dates of tooth development, eruption and exfoliation for the primary dentition.
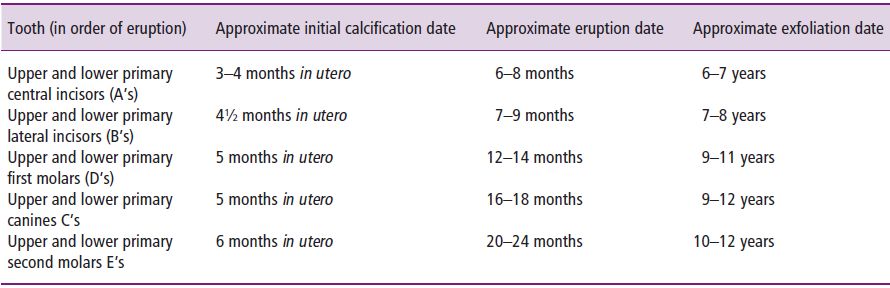
Table 1.2 Approximate dates of tooth development and eruption for the permanent dentition.
| Tooth (in order of eruption) | Approximate initial calcification date | Approximate eruption date |
| Upper and lower permanent first molars (6’s) | At birth | 6–7 years |
| Upper and lower permanent central incisors (1’s) | 3–4 months | 6–7 years |
| Upper and lower permanent lateral incisors (2’s) | Upper 10–12 months | 7–8 years |
| Lower 3–4 months | ||
| Lower permanent canines (3’s) | 4–5 months | 9–10 years |
| Upper and lower permanent first premolars (4’s) | 1–2 years | 10–11 years |
| Upper and lower permanent second premolars (5’s) | 2–3 years | 11–12 years |
| Upper permanent canines (3’s) | 4–5 months | 11–12 years |
| Upper and lower permanent second molars (7’s) | 2–3 years | 12–13 years |
| Upper and lower permanent third molars (8’s) | 7–10 years | 18+ years |
Histology of oral tissues
The three primary layers of an embryo are described as:
- Ectoderm (the outermost layer). This develops into structures such as the nervous system, the epidermis and epidermal derivatives and the lining of various body cavities such as the mouth.
- Mesoderm (the middle layer), which forms into many of the bodily tissues and structures such as bone, muscle, connective tissue and skin.
- Endoderm (the innermost layer), which develops to form the digestive tract and part of the respiratory system.
The oral mucosa
The surface of the oral mucosa consists of epithelial tissue. Epithelial tissue is first classified according to the shape of the cells as being squamous (flat cells), cuboidal (cube shaped) or columnar (tall, narrow cells) and second by the number of cell layers. A single layer of epithelial cells is called simple and where there are several layers it is called stratified.
The oral mucosa consists of:
- A surface layer of stratified squamous epithelium.
- Underneath this there is a layer of highly vascular connective tissue, the lamina propria (Figure 1.9).
- The mucous membrane is attached to underlying structures by connective tissue of varying thickness (the submucosa layer), which contains larger arteries, veins and nerves.
Figure 1.9 Diagram of the structure of the oral mucosa. Reproduced by kind permission of R. Ireland.
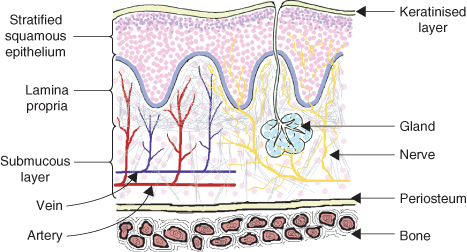
The structure of the mucous membrane varies in different parts of the oral cavity according to the variation in function. In areas subject to chewing such as the hard palate and the attached gingivae, the mucosa has a firm keratinised epithelial layer of fibrous protein (also found on the palms of the hands and soles of the feet). In other areas such as the cheeks and floor of the mouth that require more flexibility, this is reduced or absent. The cells of this keratin layer have no nuclei and no nerve supply.
Underneath the keratinised layer of cells is a non-keratinised layer of epithelial cells which have nuclei and act as cushion against mechanical forces. The deepest layer of these cells is known as the basal layer and is attached to the basal lamina.
The oral cavity is kept lubricated by mucus secretions from the major and minor salivary glands; this epithelium is sometimes termed mucous membrane.
There are three types of oral mucosa found in the oral cavity.
- Lining mucosa:
- This covers the inside of the cheeks, lips, alveolar mucosa, soft palate, under surface of tongue and floor of the mouth.
- This mucosa is non-keratinised and loosely attached.
- It has a submucosa layer, which contains blood vessels and nerves.
- Between the muscle layer and epithelium lay numerous minor salivary glands; sometimes these salivary ducts may become obstructed and a mucocele may develop.
- Masticatory mucosa:
- This covers the hard palate and gingiva.
- This mucosa has to withstand the friction of mastication; it is keratinised and firmly attached to the underlying bone.
- A layer of connective tissue lies between the masticatory mucosa and bone and the submucosa layer is absent.
- Specialised mucosa:
- This covers the dorsum of the tongue.
- It is keratinised and contains special taste receptors.
Muscular tissue
Muscle develops from mesodermal tissue and is specialised tissue in that it has both the ability to contract and the ability to conduct electrical impulses. Muscles are classified both functionally as either voluntary or involuntary and structurally as either striated or smooth.
There are therefore three types of muscles:
- Smooth involuntary muscle (e.g. intestinal).
- Striated voluntary muscle (e.g. skeletal).
- Striated involuntary muscle (e.g. cardiac).
All the oral musculature consists of striated voluntary muscle. The cells are cylindrical, unbranched and multinucleate. They contain actin and myosin which are contractile proteins. The cells are arranged in bundles (fascicles) surrounded by connective tissue which also serves to anchor the muscle to bone in the form of a tendon.
Glandular tissue
The most important glands of the oral cavity are the salivary glands. The principal salivary glands are the parotid (situated buccal to the upper molars), submandibular and sublingual (located in the floor of the mouth). There are in addition a number of minor salivary glands on the surface of the tongue, the internal surfaces of the lips and in the buccal mucosa.
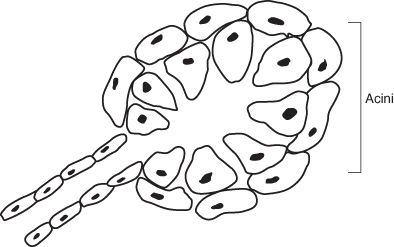
Figure 1.10 Diagram of secretory cells of salivary gland.
Production of saliva
- Each gland is made up of lobules, which resemble a bunch of grapes.
- The basic secretory units of salivary glands are clusters of cells called acini (Figure 1.10).
- These acinous epithelial cells consist of two types; serous cells which secrete a watery fluid low in mucous and mucous cells producing a glycoprotein (mucin) rich secretion.
- The serous cells are polyhedral in shape and produce a thin watery secretion.
- The mucous cells are cuboidal and produce a viscous secretion containing mucin.
- When mixed, the serous cells form a cap (demilune) around the periphery of the mucous cells.
- The parotid glands produce a serous secretion, the submandibular produce a mixture of serous and mucous and the sublingual glands produce a mainly mucous secretion.
- Secretion is under the control of the autonomic nervous system which controls both the volume and type of saliva produced.
- Saliva passes through the intercalated ducts, then the striated ducts and finally passes through the excretory ducts carrying the saliva to the oral cavity.
Constituents of saliva
The composition of saliva is subject to individual variation. It consists of 99.5% water and 0.5% dissolved substances that are made up of:
- Salivary proteins: these include:
- Glycoproteins (mucoids): lubricate oral tissues; the acquired pellicle provides tooth protection.
- Enzyme amylase: converts starch to maltose.
- Lactoferrins: ferric iron is an essential microbial nutrient; lactoferrins bind to ferric ions producing an antibacterial effect.
- Lysozomes: attack the cell walls of bacteria protecting the oral cavity from invading pathogens.
- Silaloperoxidase (lactoperoxidase): controls established oral flora by controlling bacterial metabolism.
- Histatins: inhibit Candida albicans.
- Statherin: inhibits precipitation of calcium phosphates.
- Proline-rich proteins: encourages adhesion of selected bacteria to the tooth surface. They inhibit precipitation of calcium phosphates.
- Salivary immunoglobulins: produce protective antibodies which help to prevent infection.
- Inorganic ions: bicarbonate and phosphate ions provide a buffering action, which regulates the pH of the oral cavity. Calcium and phosphate ions maintain the integrity of teeth by providing minerals for newly erupted teeth, which helps with the posteruptive maturation of enamel and prevents tooth dissolution by enhancing the remineralisation of enamel. Small amounts of sodium, potassium, chloride, and sulphate can also be found in saliva.
- Gases formed: newly formed saliva contains dissolved oxygen, carbon dioxide and nitrogen.
- Other additives: urea is formed as a waste product. Saliva also contains a vast number of microorganisms and remnants of food substances.
Bone
Bone is a specialised form of dense connective tissue. Two types of bone can be distinguished:
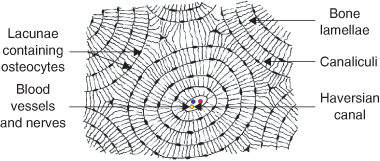
- Compact (cortical or lamellar) bone: forms the outer layer of all bones and consists almost entirely of extracellular substance (matrix). It is built up of numerous vascular canals (Haversian canals) running along the long axis of the bone around which bone is deposited by osteoblasts in a series of concentric layers (lamellae) As the matrix is deposited, the osteoblasts become trapped in small hollows (lacunae) and cease to be active in laying down bone and become osteocytes (Figure 1.11). Osteocytes have several thin processes, which extend from the lacunae into small channels within the bone matrix (canaliculi).Compact bone is surrounded by a layer of dense connective tissue, the periosteum.
- Trabecular bone (cancellous or spongy bone): consists of delicate bars and sheets of bone (trabeculae), which branch and intersect to form a sponge like network but there are no Haversian systems.
Bone is subject to constant remodelling by osteoblastic and osteoclastic (bone destroying) activity. The bone tissue of the maxilla is more vascular and less dense than that of the mandible.
Figure 1.11 Cross-section of compact bone. Reproduced by kind permission of R. Ireland.
Histology of dental tissues
Dentine
Physical characteristics of dentine
- Dentine is mineralised tissue forming the bulk of the tooth.
- It underlies the enamel in the crown area and is covered by the cementum in the root area.
- Dentine is pale yellow in colour and is harder than bone and cementum but not as hard as enamel.
Chemical composition of dentine
- 70% inorganic material (by weight) of which the main inorganic component is hydroxyapatite [Ca10(PO4)6(OH)2].
- 20% organic material (by weight).The main organic component is collagen fibres embedded in amorphous ground substance.
- 10% water (by weight).
Structure of dentine
- Dentine consists of many dentinal tubules that run parallel to each other following a double curved course and extend from the pulp to the amelodentinal junction.
- Each dentinal tubule contains an odontoblast process surrounded by intercellular ground substance composed of fine collagenous fibrils.
- The odontoblast cells are a layer of closely arranged cells on the pulpal surface of the dentine with their nuclei situated at the basal (pulpal) end of each cell.
Features of dentine
The following features of dentine are significant:
- Peritubular dentine: this is highly mineralised dentine found within each dentinal tubule surrounding the odontoblast process and can be visualised as similar to ‘furred’ pipes.
- Interglobular dentine: these are areas of dentine that remain unmineralised.
- Incremental lines: these are produced due to the rhythmic pattern of dentinogenesis often referred as contour lines of Owen. These lines are seen when dentinogenesis is disrupted (as with amelogenesis).
- Neonatal line: this is only seen in primary teeth and first permanent molars as a line that marks dentine formation before and after birth.
- Granular layer of Tomes: this is a narrow layer of granular dentine found in root dentine immediately beneath the cementum.
Age changes in dentine
Secondary dentine
Dentine is a living tissue and with age more dentine continues to form slowly; this dentine is termed secondary dentine. Secondary dentine is laid down at the pulpal end of the primary dentine. As a result of this the pulp chamber reduces in size with age.
Peritubular dentine
Peritubular dentine tends to increase with age reducing the diameter of the dentinal tubules.
Translucent/sclerotic dentine
The tubules may also become completely obliterated and when this happens the dentine becomes more translucent; this is termed translucent or sclerotic dentine.
Reparative dentine
Reparative dentine or irregular secondary dentine is laid down on the pulpal surface of the dentine in response to an external stimulus, such as caries, cavity preparation or excessive wear. Following a severe stimulus, the odontoblast process may be destroyed and the contents of the tubule then necrose leaving the dentinal tubule empty; this is termed a dead tract.
Dentine hypersensitivity
There are many theories for the mechanism of dentine sensitivity. The principal current theories are:
- Innervation theory: the nerve fibres of the pulp pass into the dentinal tubules.
- Odontoblast receptor theory: the odontoblasts act as a receptor transmitting nerve impulses.
- Brännström’s hydrodynamic theory: this suggests that there is movement of fluid within the dentinal tubules.
Enamel
Physical characteristics of enamel
- Enamel is highly mineralised and is the hardest tissue in the body.
- Enamel covers the anatomical crown of the tooth and varies in thickness.
- It is semi-translucent and its colour can vary from bluish white to hues of yellow.
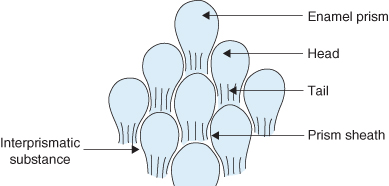
Figure 1.12 Diagram of magnified appearance of enamel prisms.
Chemical composition of enamel
- 96–97% inorganic material (by weight), the main inorganic component being hydroxyapatite.
- 1% organic material (by weight), the main organic component being protein.
- 2–3% water (by weight)
Structure of enamel
- Enamel is made up of millions of enamel prisms or rods, which run from the amelodentinal junction to the enamel surface.
- Each prism is made up of a large number of enamel crystallites.
- When viewed under a light microscope each prism resembles the rounded ‘head’ portion of a keyhole (Figure 1.12).
- The enamel crystallites run parallel to the long axis of the prism and in the ‘tail’ portion the enamel crystallites are inclined away from the long axis of the enamel prism.
Enamel is laid down in layers which produce incremental growth lines. After each successive layer the ameloblasts retreat so as not to be trapped within their matrix. Some growth lines mark daily deposits which are about 4 μm thick; these are called cross striations.
Features of enamel
The following features of enamel are significant:
- Brown striae of Retzius: these are brown lines indicating variations in weekly deposits that run obliquely from the amelodentinal junction towards the enamel surface. When the striae emerge onto the enamel surface a series of grooves may be seen; these are termed perikymata grooves.
- Hunter–Schreger bands: when viewed under a light microscope, broad dark and light bands can be seen running obliquely from the amelodentinal junction to two-thirds of the thickness of the enamel. They are curved with the convexity of the curve always facing rootwards.
- Neonatal line: since this line marks the disruption in amelogenesis at birth, it can only be seen in primary teeth and first permanent molars. It can provide an important forensic landmark.
- Enamel spindles: this is when the dentinal tubules extend into the enamel and are found most frequently beneath cusps.
- Lamellae: these are sheets like faults that run vertically through the entire thickness of the enamel.
- Enamel tufts: these are pieces of incomplete mineralised enamel that resemble tufts of grass. They extend from the amelodentinal junction and follow the direction of the enamel prisms.
- Amelodentinal junction: the enamel and dentine meet at the amelodentinal junction; this junction has a scalloped appearance.
Cementum
Physical characteristics of cementum
- Cementum is a pale yellow calcified tissue covering the root dentine.
- It is softer than dentine and can easily be worn away resulting in exposure of the dentine.
- Its thickness varies according to location; it is thickest towards the apical third of the root and thinnest cervically.
Chemical composition of cementum
- 65% by weight inorganic (mainly hydroxyapatite).
- 23% organic (mainly collagen).
- 2% water.
Structure of cementum
Cementum has a similar structure to bone. It may be classified by the presence or absence of cells:
- Acellular cementum: it is the first cementum to form and is sometimes termed primary cementum. It covers the root dentine from the cement-enamel junction to near the root apex and does not contain cells.
- Cellular cementum: this is found as a thin layer at the apical third of the tooth. It is sometimes termed secondary cementum. As cellular cementum develops, the cementoblasts that have created the cementum become embedded within the cementum matrix and become inactivated; these cells are termed cementocytes. Cementocytes are contained in lacunae and their tiny processes spread along canaliculi to join up with other cementocytes. Their processes are directed towards the periodontal ligament, from which they obtain nutrients.
Features of cementum
The following features of cementum are significant:
- Cementoenamel junction: this can be variable. In approximately 60% of teeth the cementum overlaps the enamel: in approximately 30% of teeth the cementum and enamel meet exactly and in approximately 10% of teeth the cementum and enamel do not meet thus leaving an area of dentine exposed.
- Functional changes of cementum: cemen/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


