Chapter 1
Fundamentals of Endodontic Disease
Aim
To describe the fundamental clinical biology of pulp and periapical disease, and lay the foundations for rationally based endodontic treatment.
Outcome
After studying this chapter, the reader should have clear understanding of the role of microbial infection in pulp and periapical disease, and the need for this knowledge to translate into action at each stage of clinical root canal treatment.
An Introduction to Endodontics
Endodontics is the branch of clinical dentistry concerned with the prevention, diagnosis and treatment of diseases of the dental pulp and their sequela. The discipline therefore has a broad scope, encompassing procedures which aim to:
-
preserve all or part of the pulp in health (pulp capping and pulpotomy)
-
preserve and restore teeth with irreversibly inflamed and necrotic pulps (pulpectomy and root canal treatment)
-
preserve and restore teeth with lesions which have failed to respond to root canal treatment, or which were damaged in the course of such treatment (endodontic retreatment and surgery).
In reality, “endodontic treatment” is usually synonymous with “pulpectomy and root canal treatment”, an exacting, technical and rapidly developing element of everyday practice, with its emphasis on line, length, and the attainment of a radiographically pleasing root filling. This book will focus almost exclusively on adult root canal treatment and provide a rational framework for the appraisal and safe application of established and emerging clinical methods.
The Technological Focus of Root Canal Treatment
Endodontics has never been shy of technology. New systems, devices and materials appear frequently, promising simpler, quicker, more consistent or aesthetically satisfying results. Many of us have invested heavily and repeatedly over the years, convinced and excited by the benefits to follow. Many of us have also known the brief honeymoon of interest and satisfaction which quickly evaporated into disappointment (Fig 1-1); another expensive system relegated to the back of a dark cupboard in preference for an old trusty method, or to be superseded by the next bright hope.
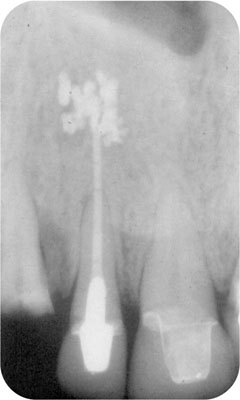
Fig 1-1 Excitement and conviction evaporate into disappointment once again.
The truth is that most of us find root canal treatment technically challenging, and wish there were simpler, more predictable and more efficient ways to do it. This, combined with a growing demand for tooth preservation, has seen unprecedented growth in world markets for endodontic product, and an insatiable hunger for new and attractively packaged materials and devices. To the dispassionate observer, this may seem to be pure commercial opportunism as we focus on technology and attaining the currently fashionable postoperative “look” rather than returning to the disease process and how it can best be managed.
At the start of a practical handbook on root canal treatment, it is important to ground ourselves in the fundamental biology of the pulp and periapical lesions we wish to prevent and heal. Only then can we rationalise the mechanical stages of treatment and reveal where new and older techniques can optimise operator efficiency and successful outcomes for patients.
Laying Foundations: The Basic Biology of Endodontic Disease
Root canal treatment is concerned with preventing and healing apical periodontitis (Fig 1-2a), a disease which affects 40% of over 30s and 62% of over 60s in western society.
Apical periodontitis is important because:
-
It causes local pain and morbidity.
-
Acute exacerbation can result in serious, potentially life-threatening extension (e.g. facial cellulitis, brain abscess).
-
There are growing concerns about the possible systemic consequences of chronic infection and inflammatory lesions associated with teeth.
Apical periodontitis develops by extension of disease in the dental pulp (Fig 1-5). It can be prevented by:
-
maintaining pulp health
-
managing pulp disease before changes can progress to involve the periapical tissues (Fig 1-3).
Established apical periodontitis is caused by infected material in the pulp canal space and is known to heal predictably if the causative agents can be eliminated and prevented from returning (Fig 1-2a,b).
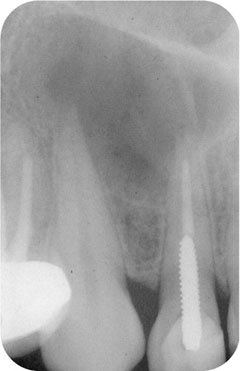
Fig 1-2a Apical periodontitis, an important and common disease in western society.
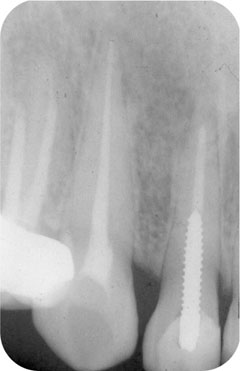
Fig 1-2b Control of aetiological factors allows apical periodontitis to heal.
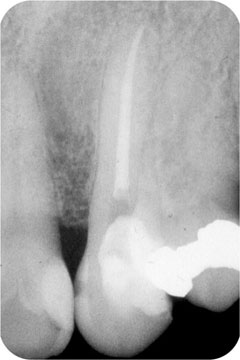
Fig 1-3 Early root canal treatment of a tooth with a dying pulp relieves pain and prevents apical periodontitis from developing.
The Aetiology of Pulp Injury and Death
Dentine and pulp are intimately related. In pristine health, the so-called “dentine-pulp complex” lies protected by an impervious layer of enamel and a sound investing periodontium. Breakdown of this protection by caries, operative dentistry or trauma (Fig 1-4) exposes porous, tubular dentine to the oral environment and leaves the pulp vulnerable to chemical, physical and microbial injury. The threat posed by microorganisms is by far the most serious.
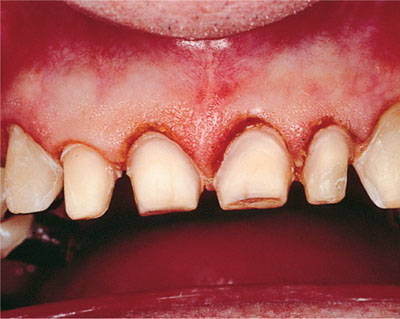
Fig 1-4 Frank exposure of the pulp, or via porous dentine leaves it vulnerable />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


