Chapter 1
Countdown to Edentulousness: Managing the Transition Successfully
Aim
The aim of this chapter is to describe how the transition to the edentulous state can be managed successfully.
Outcome
At the end of this chapter, the clinician should be aware that the loss of all natural teeth in old age is undesirable. It should be recognised that maintenance of a healthy, functioning natural dentition for life is the ideal goal for older adults. The prognosis for the natural dentition should be monitored and if total tooth loss becomes inevitable, then a gradual transition to the edentulous state should be planned. The practitioner should be aware of the various strategies possible for achieving this, beginning with the use of transitional removable partial dentures.
Introduction
A substantial body of evidence exists in the scientific literature, which documents the sequelae of total tooth loss. Although the number of adults losing their natural teeth is diminishing, there are still large numbers of edentulous adults in the population. This situation is likely to continue for many years to come, as the generation of adults rendered edentulous early in life ages. If a dentist can successfully rehabilitate edentulous patients, especially those with denture-wearing difficulties, then this will have a positive influence on the perception of their practice. Increasingly, the impact of poor quality diet on general health has been emphasised, and loss of teeth has an influence on this. Dentists have an important role to play in providing good quality complete dentures and in encouraging their edentulous patients to improve the quality of their diet. In addition to successfully managing the problems of the edentulous patient, a further requirement is to manage the transition to edentulousness. As the problems of older adults with an ageing dentition have become more challenging, it is vital that the clinician anticipates problems and plans dental care accordingly.
Adult Dental Health Trends
Population surveys of adult dental health indicate that older adults are retaining their teeth longer, and that the prevalence of edentulousness is decreasing rapidly. However, there are many threats to tooth retention, and there has been a shift towards total tooth loss occurring later in life. Clinical experience suggests that successful adaptation to edentulousness is less predictable in old age, as the ability to develop the complex skills required to control complete replacement dentures diminishes with age.
As well as the decrease in edentulousness, population surveys also indicate that there is a high level of dental disease in older adults, particularly loss of periodontal attachment and root surface caries. A further problem is the cumulative sequelae of a lifetime of the treatment of disease and of large restorations. For the most part, the increased retention of teeth in older adults is not as a result of lower levels of disease but of higher levels of treatment. For many, the goal of retaining teeth in old age may be beyond reach, and total tooth loss may be inevitable. Consequently, major challenges for dentists include:
-
Predicting the likelihood of their patients retaining teeth into old age and recognising the threats to this ideal goal.
-
Planning care based on retaining sufficient numbers of teeth for satisfactory oral function.
-
Managing the transition to the edentulous state when retention of teeth seems unlikely.
Edentulous Maxilla Opposing Partially Dentate Mandible
At the present time, large numbers of adults have edentate maxillary arches opposed by partially dentate mandibular arches. Further clinical presentations include partially dentate adults with unrestored tooth spaces. These patients may lose the remainder of the natural dentition late in life, and they present a significant management challenge to dentists. They may have a removable partial denture to replace posterior teeth, but in many cases they do not have a mandibular prosthesis. A common problem when such a combination presents is that of “flabby” tissue in the anterior maxilla. This may make the maxillary complete denture unstable, because the flabby tissue displaces during function. The problem of the displaceable (“flabby”) anterior ridge is discussed in more detail in Chapter 3. A further difficulty may be that there are insufficient occlusal contacts to maintain a stable maxillary denture. When molar and premolar teeth are missing, occlusal forces are directed through the anterior aspect of the maxillary denture, resulting in a tipping force which displaces the denture posteriorly. The clinical challenge is to decide how many occlusal contacts are required to overcome this situation, and this varies from patient to patient. In addition to making a complete maxillary denture, the following treatment options for the mandible should be considered:
-
Accepting that the number of natural mandibular teeth present is sufficient, and aim to balance the occlusion using a semi-adjustable articulator to construct the maxillary denture.
-
Restoring missing teeth with a removable partial denture (RPD).
-
Extending the shortened dental arch using cantilevered bridgework. Conventional retainers can be used if the last standing teeth are heavily restored or resin-bonded bridges can be used if the teeth are unrestored.
-
Extending shortened dental arches with implant-retained crowns or bridges.
There are a number of factors to consider when deciding which of these options is appropriate for the patient. If the maxillary complete denture is stable, then it is likely that the patient has sufficient occlusal contacts, and preserving the mandibular dentition without a prosthesis is indicated. The clinician must also bear in mind that there should be a good long-term prognosis for the remaining mandibular teeth when choosing this option. If further teeth are lost at a later date, this may compromise the patient’s ability to wear a removable prosthesis. Consequently, this treatment option is contraindicated if the remaining natural teeth are mobile, have significant (>5 mm) pocketing or show signs of advanced tooth wear (Fig 1-1).
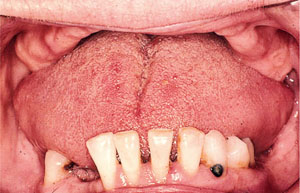
Fig 1-1 Mandibular dentition with a poor prognosis. Application of the shortened dental arch concept is contraindicated.
Removable partial dentures are widely used, but bilateral, unbounded (free-end) dentures are frequently discarded. In many cases, they are poorly constructed, and this is a significant influence on poor compliance by the patient. Factors which may improve tolerance of bilateral free-end saddle dentures include: (a) using the RPI system of clasp design to reduce torque forces on abutment teeth; (b) using the altered cast impression technique to reduce sinking of the saddle areas of the denture into the underlying tissues; (c) reducing the size of the occlusal table to reduce the load transmitted to the underlying ridges. In some cases, despite the use of good clinical technique, the patient feels uncomfortable and discards the denture.
If the mandibular dental arch extends to the first premolar teeth, and if the patient has had difficulty with a removable partial denture, the arch can be extended by one premolar unit on each side using bridgework. This will increase the number of posterior occlusal contacts thereby increasing the stability of the maxillary denture. There should be a good prognosis for the remaining teeth when considering this treatment option. Full coverage retainers are indicated if large restorations a/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


