Case 1
Biomaterials: Dental Implants and Peri‐implantitis
Review of Symptoms
- Vital signs
- Blood pressure: 120/75 mmHg
- Pulse: 60 beats/min
- Respiration: 14 breaths/min
Medical History
The medical history reveals no significant findings. The patient is not on any medications and takes an over‐the‐counter (OTC) multivitamin daily.
Social History
The patient smoked marijuana occasionally in his late teens but does not smoke anymore. He has never used tobacco. He drinks two to three beers on the weekend and drinks one cup of coffee daily.
Extraoral Examination
No significant findings
Intraoral Examination
The intraoral exam reveals maxillary third molars have been extracted. Tooth #20 is congenitally missing. The patient had an implant placed to replace tooth #20 at age 24.
Occlusion
Class I occlusion.
The patient had orthodontic treatment from age 13–15 to correct an underbite.
Radiographic Examination
Four bitewings and one periapical were recommended of tooth #20. A cone beam computed tomography (CBCT) scan was obtained from the patient’s previous oral health‐care provider.
Diagnosis and Prognosis
The patient’s general oral health is good. He brushes twice daily, and flosses at least three times a week. No other auxiliary aids are used. Light plaque accumulation is present with localized inflammation around teeth #17, #30, #31, and #32. The gingiva around the implant replacing tooth #20 is inflamed and the implant is mobile. Prognosis for tooth #20 is poor (see Figure 8.1.1).
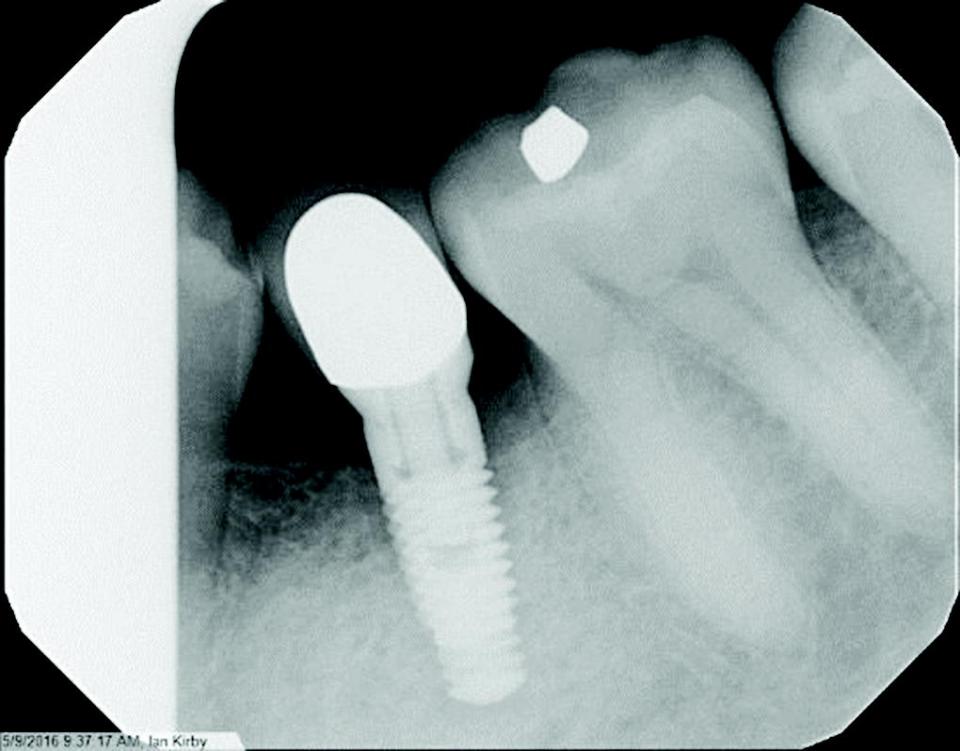
Figure 8.1.1: Tooth #20, implant with peri‐implantitis.
Dental Hygiene Diagnosis/Treatment Plan
| Problems | Related to risks and etiology |
| Bleeding upon probing, teeth #s 17, 30, 31, and 32 | Localized periodontal disease, difficulty removing biofilm in mandibular molar areas |
| 4 mm periodontal pocket on distal of #17 and 4 mm periodontal pockets on mesial of #30 and #31, 5 mm periodontal pocket on distal of #32 | Localized periodontal disease, difficulty removing biofilm in mandibular molar areas |
| Peri‐implantitis, implant tooth #20 | Poor bone quality, loss of integration |
Planned Interventions
| Clinical | Educational/counseling | Oral Hygiene Instructions |
| Evaluate soft and hard tissue Dental prophylaxis with selective SRP on #s 17, 30, 31, 32 with 4 to 8 week periodontal re‐evaluation, After completion of localized scaling and root planing (SRP) Refer to Doctor of Dental Surgery (DDS) for extraction of #20, bone grafting, implant replacement |
Encourage brushing daily and flossing daily Stress importance of maintaining recare visits, continued flossing, increase to daily, and brushing twice daily Stress importance of full mouth plaque control to reduce transfer of microorganisms to implant site where periodontal pathogens can colonize |
Soft bristle brush/ modified Bass technique Emphasize importance of flossing and accessing third molar areas when brushing and flossing Use of soft toothbrush with end rounded filaments, spongy filament floss, and end tufted brush with soft filaments |
See Figures 8.1.2–8.1.5.

Figure 8.1.2: Bone grafting: allograft (cortical/cancelous) with collagen membrane.

Figure 8.1.3: Implant guidance.

Figure 8.1.4: Implant placement.

Figure 8.1.5: Implant with healing cap.
Discussion
The design and selection of a biomaterial depends on the specific application in order to be useful and assure its properties as long as required, without rejection. In order to be considered a biomaterial it should, besides not inducing inflammation, toxic reactions, and allergenic symptoms in the body, be biocompatible, biofunctional, bioactive, bioinert, and sterilizable. The biomaterial surface being directly exposed to the living organism plays a crucial role in regards to biocompatibility. When this issue is considered, the physical, morphological, and biologic characteristics can be adapted to promote improvement in the interaction of biomaterial and tissue. In recent years the concept of biocompatibility has changed. At first it was believed that a material was biocompatible by being completely inert to the human body without any response from the biological medium to its presence. The idea of a totally inert material was abandoned when it could be observed that the presence of any kind of material always entails some response from the body, varying as a function of the kind of application and the patient’s characteristics (age, sex, etc.) (dos Santos et al. 2017).
Dental implants represent a reliable treatment option in oral rehabilitation of partially or fully edentulous patients in order to restore function and esthetics. Single tooth replacement with a dental implant has become the standard in esthetic treatment, providing advantages, but also challenges in some cases.
More than 45 years ago, Branemark et al. (2001) first described the process of osseointegration, which began an era of research on the shape and materials of dental implants. But more recently the focus of biomedical research shifted from shape and materials used to the oseoinductive potential of implant surfaces. Today there are over 1000 different implant systems with variations in shape, dimension, bulk, surface material, thread design, implant‐abutment connection, surface topography and chemistry, wettability, and surface modification.
Although long‐term survival rates of dental implants are excellent, failures do still occur in a small number of patients. Of these failures, 1–2% occur in the first few months due to insufficient osseointegration, and 5% of failures develop after several years due to peri‐implantitis.
As with any disease process the presence of certain risk factors will increase the likelihood of disease development and progression, (Alani and Bishop 2014). Awareness of these risk factors when planning implant treatment is important in the prevention of peri‐implantitis and failure of the implant. Among these factors both bone quality and poor oral hygiene may potentially play a role as a risk factor in peri‐implantitis (Alani and Bishop 2014). Patients with advanced clinical conditions, such as those with diabetes mellitus, osteoporosis, bisphosphonate use, or those having undergone radiation therapy also continue to be a great challenge in terms of achieving successful osseointegration.
Patients need to be made aware that implants are susceptible to plaque related disease in much the same way as natural teeth. At the treatment planning stage it is critical that an objective assessment of oral hygiene is completed and that treatment should be postponed until adequate plaque control is achieved (Alani and Bishop 2014).
Among the other factors that may play a role in development of peri‐implantitis is the quality of bone in the implant site. In the case of a congenitally missing tooth at the site of implant placement, several factors may lead to peri‐implantitis and ultimately failure of the implant: inadequate consistency and quality of bone, a decreased collateral blood supply from remnant periodontal ligament, a missing tooth space larger than tooth to be replaced, and occlusal discrepancy.
Success in the case of a patient presenting with the above conditions will depend on several factors, among these, the skill of the clinician, the success of bone grafting, the stability and position of the implant and patient compliance, which should include regularly scheduled recare and maintenance visits as well as case specific oral hygiene instruction.
Research efforts have been focused on designing novel topographies of implant surfaces to increase osteoblastic migration, adhesion, proliferation, and differentiation.
Numerous studies have shown that use of particular surface modifications, such as laser ablation, and surface coatings with proteins, drugs, and growth factors may improve the success and survival rates of implants.
The goal of biomedical research on surface modifications is to promote early osseointegration and ensure a long‐term bone‐to‐implant contact without substantial marginal bone loss.
Take‐Home Hints
- At the treatment planning stage it is critical that an objective assessment of oral hygiene is completed by the dental hygienist. If the patient has poor oral hygiene, implant placement should be postponed until the patient is compliant with home care, biofilm removal, and preventive procedures.
- After implant placement, a case‐specific oral hygiene regimen should be created for the patient based on individual needs.
- Patients should be made aware that implant placement is a life‐time commitment and implants require as much care, if not more, as natural teeth.
- Regularly scheduled recare appointments are critical for maintenance and success of implants.

VIDEdental - Online dental courses


