This article examines the differences and interaction between sex and gender, and how they affect women’s oral and general health. The authors provide a definition of women’s health, and examples of how this definition can be used to describe various oral health conditions and diseases in women. The article reviews the research on sex and gender and provides examples of their interactions. Examples of oral diseases that affect primarily women are reviewed. Advice for clinicians on the diagnosis, management, and prevention of these conditions is provided.
Key points
- •
Understand the differences and interactions between sex and gender.
- •
List how sex and gender can affect health in women.
- •
Identify oral health issues that predominately affect women.
- •
Discuss systemic health issues that have different presentation, management, and treatment in women compared with men.
- •
Describe long-term care issues affecting women’s oral health.
Introduction
Sex and gender, separately and together, serve as important determinants of health and play a role in cause or pathophysiology of certain illnesses. The relative importance of them varies depending on the chronologic and contextual life stage, and social and cultural contexts.
In 2009, there were more female (155.6 million) than male (151.4 million) residents in the United States. Women today are more likely to participate in the healthcare system, and the issues facing them are often different from those of men. Women also comprise disproportionally higher numbers of other social and cultural groups that are at risk for poor health outcomes (low income, ethnic minority, low education). It has been recognized in science by the Institute of Medicine’s Report “Exploring the biologic contributions to human health: does sex matter?” and in society and policy with the 1994 change in the National Institutes of Health policy recommending inclusion of women and minorities as subjects in clinical research that sex and gender do matter in health. How to conceptualize and operationalize the sex and gender aspects in health, however, remains complex.
This article provides a framework for sex and gender considerations as they affect the unique oral health needs that women face throughout their lives. The article addresses hormonal changes during a woman’s life that affect oral health and disease; certain chronic diseases, such as cardiovascular disease (CVD) and diabetes, which may present differently in women; and diseases that affect primarily women, such as Sjögren syndrome (SS) and breast cancer. Practical considerations are provided to assist oral health practitioners in caring for their patients.
Sex and Gender in Human Health
The Institute of Medicine defines sex as “The classification of living things, generally as male or female according to their reproductive organs and functions assigned by chromosomal complement.” Gender is defined as “A person’s self representation as male or female, or how that person is responded to by social institutions based on the individual’s gender presentation. Gender is rooted in biology and shaped by environment and experience.” Recent research and subsequent guidelines have suggested that basic biomedical reductionist framework (ie, sex as a dichotomous variable) is insufficient to understand these issues. This argument stems from the notion that sex is frequently used as a proxy for biologic factors, even for those that do not involve reproductive issues. Recently Springer and colleagues in 2012 suggested that “the vast majority of male-female health differences are due to the effects of the irreducibly entangled phenomenon of ‘sex/gender’ and therefore this entanglement should be theorized, modeled, and assumed until proven otherwise.” They point out that the notion where sex (biologic) and gender (social) overlap is outdated, and one should construe sex and gender as simultaneously biologic and social without preconceived notions about causality to either direction. Furthermore, one should focus more on understanding the biologic mechanisms and impact of social status as drivers of male-female health differences.
CVD, which is the leading cause of death among women, provides an example. Historically it was considered to be a “male-disease” until it was found that CVD also affects women significantly, although later in life and with different presentation, progression, and response to treatments. How sex and gender are interwoven can be illustrated in an example where psychosocial stress among women, often a result of complex social and cultural roles (ie, gender), induces ovarian dysfunction, which in turn is considered as biologic, and hence, sex-related. Social and cultural issues can have a great impact on what presents itself biologically. Tobacco use, a leading preventable cause of mortality, provides an example of how current health policies may not be as effective in women as men. The adverse health consequences of the global tobacco use manifest themselves uniquely among women. Smoking is a causal risk factor for cervical cancer and increases risk for breast cancer and maternal smoking impacts fetuses. Unfortunately, many of the tobacco control policies and cessation programs have been found to be more effective in men than women.
Arain and colleagues reviewed the complexity of sex and gender at a physiologic level. Biologically driven sex dimorphisms have to be understood even at the intracellular level where the sex of the cell and its hormonal environment may affect the etiology, progression, and efficacy of medications.
The role of sex and gender must be conceptualized, researched, and reported as an interactive, interdisciplinary, and intersectional approach to health. As scientific understanding increases around these issues, translational research will remain a critical determinant of human well-being.
Women’s Health
Women’s health spans multiple health disciplines including medicine, public health, pharmacy, nursing, social work, psychology, and oral health. Women’s health is defined as diseases or conditions unique to, more prevalent in, or more severe in women, including those for which manifestations, risk factors, and interventions differ in women. CVD with its risk factors, such as hypertension, obesity, diabetes, tobacco use, and lipoprotein disorders, has received increased attention in the scientific literature during the past 10 years. Tobacco use is an illustration of how a given risk factor disproportionately impacts women. Women’s tobacco use confers a 25% greater relative risk compared with men for CVDs. Women are also more likely to be exposed to second-hand tobacco smoke, which has been shown to be a causal risk factor for CVD.
In addition to CVD and breast cancer, there are numerous conditions and diseases that affect women in disproportionate degrees and across the life span. Examples include cervical dysplasia and cancer; lung cancer; temporomandibular joint disorders; sexually transmitted diseases; migraine headache; bone and joint disorders; and autoimmune disorders, such as SS, rheumatoid arthritis, scleroderma, and systemic lupus erythematosis. In addition, behavior and mental health issues (eg, depression), interpersonal violence, and HIV-AIDS also affect women in greater proportion than men. In preventive medicine, human papilloma virus vaccination, pap smears, mammograms, and colon cancer screenings are of critical importance for women’s health.
Women’s Health Across the Lifespan
There are many ways to construe health and its determinants. Koh and colleagues suggested a model where determinants could be construed by population (ethnicity, sex); by disease (CVD, cancer); by risk factor (immunization status, drug use); or by geography (urban vs rural). Chronologic age, hormonal cycle (puberty, menopausal status), and life stages (pregnancy and motherhood) make understanding sex and gender differences across the lifespan more intuitive. However, women’s health issues need to be considered also from the perspective of social status and other social determinants of health and within cultural contexts.
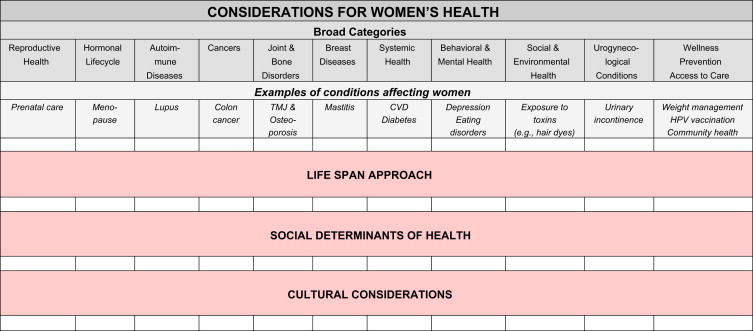
The social determinants of health include individual demographics and environmental concerns (urban vs rural; living conditions), whereas cultural considerations focus on women’s health by exploring the intersection of social status, such as race and ethnicity, income, parenthood, and sexual orientation. Fig. 1 illustrates women’s health issues with examples within three perspectives in health (life span, social determinants, and cultural context). These three approaches are overlapping but also individually may shape health trajectories. For example, a postmenopausal African American woman living in a poor inner-city neighborhood with limited access to care has a higher risk for CVD than a premenopausal highly educated white woman with good access to care.
Interactions of Sex and Gender
Although it is not clear how to dissect sex and gender, one’s biologic sex remains an important issue in health and wellness. However, it is critical to understand the specific biologic processes and mechanisms that drive the observed sex differences. One must consider data regarding sex and gender differences and similarities within the context of social and cultural aspects across the lifespan. The goal is to translate these findings to improve health outcomes for women and men. To promote a greater understanding of the complexity of sex and gender issues in women’s oral health, the term “sex and gender” is used throughout this article.
Introduction
Sex and gender, separately and together, serve as important determinants of health and play a role in cause or pathophysiology of certain illnesses. The relative importance of them varies depending on the chronologic and contextual life stage, and social and cultural contexts.
In 2009, there were more female (155.6 million) than male (151.4 million) residents in the United States. Women today are more likely to participate in the healthcare system, and the issues facing them are often different from those of men. Women also comprise disproportionally higher numbers of other social and cultural groups that are at risk for poor health outcomes (low income, ethnic minority, low education). It has been recognized in science by the Institute of Medicine’s Report “Exploring the biologic contributions to human health: does sex matter?” and in society and policy with the 1994 change in the National Institutes of Health policy recommending inclusion of women and minorities as subjects in clinical research that sex and gender do matter in health. How to conceptualize and operationalize the sex and gender aspects in health, however, remains complex.
This article provides a framework for sex and gender considerations as they affect the unique oral health needs that women face throughout their lives. The article addresses hormonal changes during a woman’s life that affect oral health and disease; certain chronic diseases, such as cardiovascular disease (CVD) and diabetes, which may present differently in women; and diseases that affect primarily women, such as Sjögren syndrome (SS) and breast cancer. Practical considerations are provided to assist oral health practitioners in caring for their patients.
Sex and Gender in Human Health
The Institute of Medicine defines sex as “The classification of living things, generally as male or female according to their reproductive organs and functions assigned by chromosomal complement.” Gender is defined as “A person’s self representation as male or female, or how that person is responded to by social institutions based on the individual’s gender presentation. Gender is rooted in biology and shaped by environment and experience.” Recent research and subsequent guidelines have suggested that basic biomedical reductionist framework (ie, sex as a dichotomous variable) is insufficient to understand these issues. This argument stems from the notion that sex is frequently used as a proxy for biologic factors, even for those that do not involve reproductive issues. Recently Springer and colleagues in 2012 suggested that “the vast majority of male-female health differences are due to the effects of the irreducibly entangled phenomenon of ‘sex/gender’ and therefore this entanglement should be theorized, modeled, and assumed until proven otherwise.” They point out that the notion where sex (biologic) and gender (social) overlap is outdated, and one should construe sex and gender as simultaneously biologic and social without preconceived notions about causality to either direction. Furthermore, one should focus more on understanding the biologic mechanisms and impact of social status as drivers of male-female health differences.
CVD, which is the leading cause of death among women, provides an example. Historically it was considered to be a “male-disease” until it was found that CVD also affects women significantly, although later in life and with different presentation, progression, and response to treatments. How sex and gender are interwoven can be illustrated in an example where psychosocial stress among women, often a result of complex social and cultural roles (ie, gender), induces ovarian dysfunction, which in turn is considered as biologic, and hence, sex-related. Social and cultural issues can have a great impact on what presents itself biologically. Tobacco use, a leading preventable cause of mortality, provides an example of how current health policies may not be as effective in women as men. The adverse health consequences of the global tobacco use manifest themselves uniquely among women. Smoking is a causal risk factor for cervical cancer and increases risk for breast cancer and maternal smoking impacts fetuses. Unfortunately, many of the tobacco control policies and cessation programs have been found to be more effective in men than women.
Arain and colleagues reviewed the complexity of sex and gender at a physiologic level. Biologically driven sex dimorphisms have to be understood even at the intracellular level where the sex of the cell and its hormonal environment may affect the etiology, progression, and efficacy of medications.
The role of sex and gender must be conceptualized, researched, and reported as an interactive, interdisciplinary, and intersectional approach to health. As scientific understanding increases around these issues, translational research will remain a critical determinant of human well-being.
Women’s Health
Women’s health spans multiple health disciplines including medicine, public health, pharmacy, nursing, social work, psychology, and oral health. Women’s health is defined as diseases or conditions unique to, more prevalent in, or more severe in women, including those for which manifestations, risk factors, and interventions differ in women. CVD with its risk factors, such as hypertension, obesity, diabetes, tobacco use, and lipoprotein disorders, has received increased attention in the scientific literature during the past 10 years. Tobacco use is an illustration of how a given risk factor disproportionately impacts women. Women’s tobacco use confers a 25% greater relative risk compared with men for CVDs. Women are also more likely to be exposed to second-hand tobacco smoke, which has been shown to be a causal risk factor for CVD.
In addition to CVD and breast cancer, there are numerous conditions and diseases that affect women in disproportionate degrees and across the life span. Examples include cervical dysplasia and cancer; lung cancer; temporomandibular joint disorders; sexually transmitted diseases; migraine headache; bone and joint disorders; and autoimmune disorders, such as SS, rheumatoid arthritis, scleroderma, and systemic lupus erythematosis. In addition, behavior and mental health issues (eg, depression), interpersonal violence, and HIV-AIDS also affect women in greater proportion than men. In preventive medicine, human papilloma virus vaccination, pap smears, mammograms, and colon cancer screenings are of critical importance for women’s health.
Women’s Health Across the Lifespan
There are many ways to construe health and its determinants. Koh and colleagues suggested a model where determinants could be construed by population (ethnicity, sex); by disease (CVD, cancer); by risk factor (immunization status, drug use); or by geography (urban vs rural). Chronologic age, hormonal cycle (puberty, menopausal status), and life stages (pregnancy and motherhood) make understanding sex and gender differences across the lifespan more intuitive. However, women’s health issues need to be considered also from the perspective of social status and other social determinants of health and within cultural contexts.
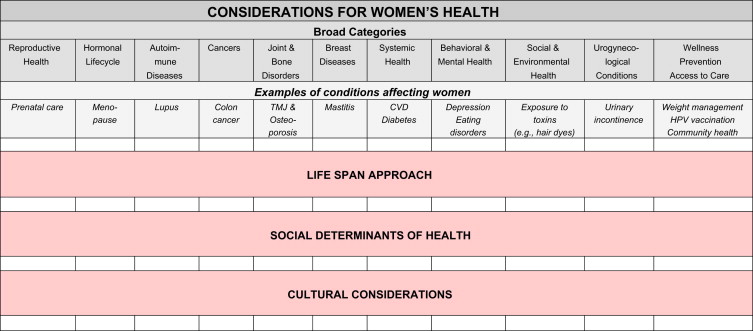
The social determinants of health include individual demographics and environmental concerns (urban vs rural; living conditions), whereas cultural considerations focus on women’s health by exploring the intersection of social status, such as race and ethnicity, income, parenthood, and sexual orientation. Fig. 1 illustrates women’s health issues with examples within three perspectives in health (life span, social determinants, and cultural context). These three approaches are overlapping but also individually may shape health trajectories. For example, a postmenopausal African American woman living in a poor inner-city neighborhood with limited access to care has a higher risk for CVD than a premenopausal highly educated white woman with good access to care.
Interactions of Sex and Gender
Although it is not clear how to dissect sex and gender, one’s biologic sex remains an important issue in health and wellness. However, it is critical to understand the specific biologic processes and mechanisms that drive the observed sex differences. One must consider data regarding sex and gender differences and similarities within the context of social and cultural aspects across the lifespan. The goal is to translate these findings to improve health outcomes for women and men. To promote a greater understanding of the complexity of sex and gender issues in women’s oral health, the term “sex and gender” is used throughout this article.
Women’s oral health
Puberty
At puberty, girls experience an increase in levels of estrogen and progesterone. These hormonal changes increase blood flow to the gingival tissues. This can cause a greater reaction to any irritation caused by plaque or food particles. During this time, the gums may become edematous, erythematous, and feel tender. Microbial changes in oral flora have also been reported during puberty. These changes have clear implications for young female patients. For the 11-year-old girl who has not yet gone through puberty, she may not experience gingivitis even though she does not her brush her teeth frequently or well. However, several months later when this young woman experiences puberty, she may find that the plaque and debris on her teeth as a result of her poor tooth brushing habits now cause red, swollen, and bleeding gums. Changes in the oral microflora and the inflammatory response as a result of puberty can result in an altered gingival tissue response.
Dental practitioners caring for girls about to experience puberty should provide oral hygiene education. Girls should understand that the hormonal changes they are about to undergo also can affect their oral health. Mild cases of gingivitis respond well to scaling and improved daily oral hygiene care. Severe cases of gingivitis may require more aggressive care (scaling, antimicrobial therapy, and possibly surgery). These patients may require more frequent recalls until the condition improves or resolves.
A caries risk assessment should be conducted to identify the patient’s potential risk for dental caries. Risk studies have shown that the best predictor for future caries is present caries. Good oral hygiene and plaque control is especially important because the increase in hormones results in an exaggerated inflammatory response to local irritants. Education in proper oral self-care techniques is a critical component of the preventive treatment plan. Scaling and root planing may be performed when needed to treat any periodontal infection.
Menses
Oral changes have been reported during menses and vary considerably among women. Although evidence-based reports on the epidemiology of oral changes with menses are lacking, anecdotal reports of oral changes include red, swollen gingival tissues, activation of herpes labialis, oral apthous ulcers, or halitosis. A good medical and clinical history is essential to understanding oral changes a woman may experience during menstruation.
Pregnancy
Dental professionals today can still hear a pregnant woman state that she believes that you “lose a tooth for each pregnancy.” This misconception arose from the belief that the calcium needed for the developing fetal bones was available from the teeth. Calcium in the teeth does not serve as a reservoir for the calcium needed for fetal development.
The relationship between caries and pregnancy is not well defined. Very little epidemiologic data exist on the caries incidence rates of pregnant women. Because pregnant women often have food cravings, if the food she craves is cariogenic, it may increase her risk of caries. A clinical study on the effect of prenatal fluoride on the caries rates of the pregnant woman’s offspring showed no differences in caries rates of the mothers who took the prenatal fluoride and the children of the mothers who did not take the prenatal fluoride. As a result, prenatal fluoride vitamins are not recommended for pregnant women.
Bleeding gums or gingivitis is the most common oral condition experienced during pregnancy. It can range from mild inflammation to severe gingivitis, localized or generalized, and occurs in 60% to 75% of pregnant women. As with puberty and menses, the increase in hormones exaggerates the gum tissue’s response to bacterial plaque. The gingival tissue is usually red, swollen, and bleeds easily. It often occurs in the anterior part of the mouth. Patients can notice these changes at any time during the pregnancy.
A localized area of severe inflammation can also be called a “pregnancy tumor” or pyogenic granuloma. If the granuloma becomes large and interferes with functioning, such as speaking or chewing, it may require treatment and removal before the birth of the baby. Pregnancy granulomas excised before delivery may recur and patients should be warned of such occurrences.
Premature Births
In the United States, each year approximately 500,000 babies are born prematurely. A preterm low-birth-weight baby is defined as a baby born before 37 weeks and weighing less than 2500 g (5 lb, 8 oz). Prematurity is a major risk for newborn death, chronic health problems, and developmental disabilities.
Periodontal disease has been investigated as a potential risk factor for preterm low-birth-weight babies. The mechanism of action suggests that throughout pregnancy, cytokines and prostaglandins increase until a critical threshold is reached that induces labor and delivery. The bacteria associated with periodontal infection can stimulate excessive production of the mediators, which then induce labor and delivery prematurely. Although the scientific evidence on the effect of treatment of maternal periodontal disease is still unclear, dental professionals can provide advice and counsel on the importance of good oral health and periodontal disease prevention to their patients who are pregnant or considering becoming pregnant.
Women with periodontal disease who are considering becoming pregnant should seek treatment of their periodontal infection as a matter of good health. Eliminating infection in the body allows the body’s immune system to function more efficiently. Good periodontal health should be considered as part of a healthy approach to pregnancy. An example is folic acid. Women considering or trying to become pregnant are recommended to start taking folic acid before they become pregnant to prevent neural tube defects.
Evaluation of the pregnant woman begins with a thorough medical history, including a review of systemic illnesses, particularly hypertension, previous miscarriages, recent cramping, or bleeding. A recent clinical trial demonstrated the safety of providing dental care to pregnant women. Providing oral health for the pregnant woman is discussed elsewhere in this issue.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


