Treating the special care patient is challenging for the treating dentist and dentist anesthesiologist. The goal is to have a patient free of disease and pain restored with aesthetic and functional use of his/her oral cavity. The challenge is to incorporate the patient’s medical, physical, behavioral, financial, and oral hygiene considerations into this goal. This article describes clinical techniques used to treat special care patients under intravenous sedation in an outpatient dental clinic setting. The discussion includes how to make a preoperative dental diagnosis, how to start an intravenous line painlessly, intravenous medications used in outpatient sedation, clinical tips for dentistry with special care patients, and postoperative evaluation.
One group of patients is beyond the scope of the general dentist to treat in the office without some form of sedation. Developmental or acquired mental disability is said to affect 3% of our population. Mental disability is a general term, applied when an individual’s intellectual development is significantly lower than average and his/her ability to adapt to the environment is consequently limited. The condition varies in cause and severity. Mental retardation is a form of developmental disability that varies in severity and is usually associated with physical problems. It is a disorder of intellectual and adaptive functioning; affected individuals are challenged by the skills they use in everyday life. A method of grouping these patients is by IQ into categories of mild, moderate, severe, and profound mental retardation ( Table 1 ). Although patients who fall into the slight category can possibly be treated by a dentist without sedation training, as their mental diagnosis worsens or the complication of their dentistry increases, an option is to treat them with sedation or general anesthesia.
| Degree of Mental Disability | SB-IV | WISC-III | Communication |
|---|---|---|---|
| Mild | 67–52 | 69–55 | Should be able to speak well enough for most communication needs |
| Moderate | 51–36 | 54–40 | Has vocabulary and language skills such that the child can communicate at a basic level with others |
| Severe or profound | ≤35 | ≤39 | Is mute or communicates in grunts; little or no communication skills |
Many handicapped patients, especially higher-functioning patients, live with their families when they are young. As they age, they become more difficult to attend to. Their parents are aging, too, and it is difficult after a period of 10 to 20 years for a parent to manage his/her child, who could still be functioning at a mental age of 5 to 7 years, although the chronologic age could be 20 years. At this point, many are placed into group home facilities where they can be managed by professionals who can address their medical, dental, dietary, and social needs and general welfare and development. These facilities give patients a degree of independence where they can still be supervised.
In group home facilities managed by nonprofit organizations, federal law requires the patients to be seen by a dentist at least once per year. The facility may have more restrictive regulations, requiring more than one visit per year. What the treating dentist recommends regarding recall appointments also needs to be followed by the facility, and this situation could require much more frequent recall appointments for examinations and cleanings.
Once the patient presents to the dental office, the type and quality of the treatment varies, depending on the skills of the dentist and the cooperativeness of the patient.
Patients functioning in the mild-to-moderate categories of mental disability may be cooperative or manageable in the private dental office with minimal treatment modifications. A full range of dental treatment can be offered.
As the degree of disability worsens, a private dental office might not be the optimal setting for the delivery of care. Uncooperative or violent patients may require more staff, with additional training, to control their behavior. Other equipment, such as a papoose board (Olympic Medical Corp., Seattle, Washington) to restrain the patient from hurting him/herself or the dental staff, might be necessary. The severe-to-profound developmentally disabled patient can yell or scream, run through the office, physically hurt others or him/herself, or damage equipment. Other patients in the office, or neighbors, might not understand what the commotion in the office is all about.
A partial solution is to treat the developmentally disabled patients at a specific time of the day when only they will be treated, which is not always possible.
If patients are unamenable to treatment in the conventional manner and need referral, many dentists are unaware of to whom or where to refer this set of patients for further care.
Referral to an office or to a hospital dental clinic outpatient setting geared for treating the developmentally disabled might be the solution. In a hospital setting, especially one with a general practice residency program, dental specialists are available to treat the needs of these individuals. Dentist anesthesiologists can help with behavior management by administering sedation in the clinic. An option of general anesthesia in the operating room is always available for patients unmanageable with sedation or for those needing extensive dental treatment.
Many group residencies are interested in providing the maximum treatment in the fewest possible visits. Although the patient will need to be physically evaluated as if undergoing general anesthesia, treatment with intravenous (IV) sedation will need less laboratory work, requiring fewer visits. The day of treatment will require less treatment time than general anesthesia in the operating room, making IV sedation an attractive option for the group residency staff.
Preoperative evaluation
On the day the patient presents for preoperative evaluation, the evaluation starts before the patient sits in the chair. The cooperativeness of the patient on entering the dental operatory (if he/she comes at all) is assessed.
The medical history must be reviewed, including medications, allergies, reason for wanting/needing sedation, dental history, physical examination, American Society of Anesthesiology (ASA) classification ( Table 2 ), surgical history, and any general anesthetics or sedations for past treatments. Referrals for laboratory work and for physician evaluation should be given as needed.
| ASA I | A patient without systemic disease; a normal healthy patient |
| ASA II | A patient with mild systemic disease |
| ASA III | A patient with severe systemic disease that limits activity but is not incapacitating |
| ASA IV | A patient with incapacitating systemic disease that is a constant threat to life |
| ASA V | A moribund patient not expected to survive 24 hours with or without operation |
The dental history is elicited from the aide or parents who brought the patient. This history may be known (parents) or not known. What was done in the past and how it was done (with or without sedation/general anesthesia) will help give the practitioner a better understanding of how to manage the patient.
The aide/parent will know how cooperative and thorough the patient is in brushing his/her teeth or if he/she lets another caretaker brush for him/her.
An oral evaluation at this point can be attempted. If the patient will sit in the dental chair and allow an examination, a more accurate treatment plan can be formulated. If the patient will not sit in the dental chair, he/she might sit in a regular chair and open his/her mouth. At times, the patient will not be cooperative at all. At this point, two options are available. The patient can be placed in a papoose board, the head stabilized, and an examination done using manual manipulation and mouth props. Alternatively, the patient might allow just the lower lip to be pulled down. Even if the patient refuses to open fully, much can be learned from observing the lower anterior dentition. The practitioner will determine if the patient has teeth and will evaluate his/her oral hygiene and periodontal condition.
Mental disability can be associated with other forms of physical disabilities, illnesses, and genetic disorders. Examples of these are Down syndrome, pervasive developmental disorder under which autism falls, cerebral palsy, fragile X syndrome, and other genetic disorders. The specific dental component of these entities, and the medical conditions that might affect dental treatment and IV sedation, need to be evaluated before treatment commences.
In evaluating proposed dental treatment, consideration should be made to try to save teeth wherever possible. Periodontally involved teeth that are mobile but not infected, should not be extracted. Many times, the mentally handicapped will have an uncorrected malocclusion or severely decimated dentition caused by extractions, which places an increased occlusal force on the remaining teeth and actually increases the mobility of the teeth in occlusion.
Another situation to consider is the parent who wants his/her child’s dentition restored after an extraction. This situation frequently occurs when dealing with the upper anterior teeth. Before an extraction in this area, inquiries to the parent or aide should be made to determine if the patient would be a candidate for a removable partial denture. A patient might not tolerate a removable appliance in his/her mouth. He/she may also be unable to remove it to clean it or to allow an aide to do it. Some might take it out and throw it away. An implant might not be the solution either because the surgical site might be mutilated by the patient, not allowing proper healing or the maintenance of oral hygiene. A fixed partial denture might be a better option if enough teeth remain to support a bridge, and oral hygiene and occlusion are favorable. This option will also necessitate multiple sedations for treatment. Because many mentally disabled patients are covered under state-sponsored insurance programs, costs for fixed bridgework and implants are usually not covered. If this treatment is desired, the costs would have to be financed privately.
The practitioner will have to take all of these considerations into account in formulating a dental treatment plan customized to each individual patient’s situation.
Medical consultation or laboratory work, if needed, can be ordered at this time. Based on the collected information, a sedation and dental treatment plan can be formulated.
Consent forms for sedation can be given to the aide accompanying the patient or mailed directly to the legal guardian/parent if the legal guardian/parent will not be present on the day of sedation. Group homes can forward the consent to the legal guardian/parent for signature too. In the treatment section of the consent, the area can be written as “oral rehabilitation under IV sedation, which may include examination, radiographs, cleaning, fillings, extractions, root canals as needed,” which will cover most treatment when a presedation treatment plan cannot be fully assessed. The original consent form is returned on or before the day of treatment.
Points to be noted include the following: How extensive is the dentistry that needs to be done? Can the patient’s treatment plan be completed in one to three 2-hour sedation visits or will the treatment take a longer amount of time? How manageable is the patient? Is the patient cooperative enough to get into the dental chair with a papoose board on his/her own or with gentle urging by the residency staff, or is the patient combative and does he/she pose a physical danger to you, your staff, or him/herself? What is the medical and physical condition of the patient? Is the patient obese and unable to fit into a papoose board? Is the patient considered an ASA III patient and not a candidate for outpatient IV sedation?
If the dentistry is extensive or delicate, the patient might better be served if treated under general anesthesia in the operating room. Also, patients who are combative can be premedicated with intramuscular ketamine to make them more manageable for starting an IV. This treatment will depend on the training of the dentist and the recovery facilities available because the recovery time could be much longer than with IV sedation alone. In the author’s clinic setting, they like to have the patients move in and out quickly, so having the longer recovery period usually seen with ketamine is not appealing. If medical or physical issues are a problem or if the patient has an ASA III classification or higher, he/she will be disqualified for IV sedation as an outpatient in the author’s dental clinic and will be worked up for the operating room.
Written preoperative instructions are given, which include nothing by mouth status for 8 hours preoperatively for adult patients (except for their usual medications with a small sip of water), comfortable loose clothing, and no jewelry.
Day of treatment
The day of treatment begins with a telephone call to the patient’s legal guardian. Although a written signed consent form is brought to the clinic by the person accompanying the patient, the legal guardian of adult patients in group homes usually does not accompany them. The legal guardians are informed of the date of the sedation in advance and are asked to be available for a phone call on that morning. Informed consent is discussed, including proposed procedures and other options. An opportunity to ask questions is given. The conversation is witnessed by a second person and a note to this effect is placed in the dental chart and signed before treatment.
The aide accompanying the patient is then asked, “What did the patient eat or drink today?” as opposed to “Did the patient eat?” It requires more than a yes/no response. Patients are allowed to take their usual medications with a small sip of water.
The patient is placed on a papoose board over the dental chair. The chair is in a flat position and the patient is told to “lie down on the bed.” If the patient is cooperative, blood pressure and EKG leads are placed at this time. An oxygen saturation reading can be taken. Lungs are auscultated for bilaterally clear breath sounds. If the patient is noncooperative, he/she is placed on the papoose board without the monitors. The patient is wrapped in the papoose with one arm left out. A tourniquet is placed medial to the antecubital fossa. When the patient lies down on the chair, the chair should be at its lowest point to make it more appealing for the patient to lie down and minimize any injury should the patient fall or jump off the chair before being secured by the papoose board. After the patient is secured, the head is tilted up from the flat position.
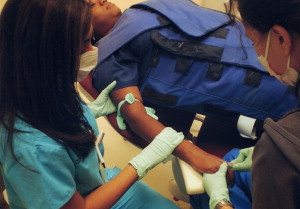
With one arm out of the papoose, two people can then start the IV. The second person stabilizes the arm by leaning it on the arm of the chair or on his/her leg as a fulcrum. One of the stabilizer’s hands is placed under the patient’s arm, with the second hand above the forearm ( Fig. 1 ). With the tourniquet medial to the antecubital fossa, the whole length of the arm can be examined at one time for an appropriate vein. To aid in IV cannulation, the following steps are taken. First, the vein needs to be below the level of the heart for it to fill up, which is accomplished by tipping the head of the chair up and then raising the chair so the patient’s arm hangs down. Second, adequate light at a 45° angle is needed to help visualize the vein. The back of the practitioner’s finger is used to tap the vein to irritate it and have it engorge with blood. Slapping the hand or arm with a full open hand, as some practitioners do, can appear aggressive to the patient (especially a child). The vein is cannulated by first injecting a small amount of lidocaine (for infiltration and nerve-block; not with epinephrine) subcutaneously with a small 25-gauge needle. This procedure is accomplished by placing the needle on the skin with the bevel pointing downwards, maintaining a “seal” of the needle flush with the skin ( Fig. 2 ). The syringe is then forced in a downward and backward direction while pressing on the plunger, forcing anesthetic solution through the skin without needle penetration. The solution is pushed subcutaneously through the skin’s semipermeable membrane to develop a skin wheal. With practice, it can be done painlessly. The needle from the lidocaine syringe is removed and is replaced by the IV catheter. This whole unit is easier to manipulate than holding the catheter by itself. The catheter is slightly bent at 45°, allowing a different approach to the vein ( Fig. 3 ). The catheter tip penetrates the skin through the skin wheal of local anesthesia, with no sensation felt by the patient. After venous cannulation, the plunger is aspirated to check for a blood backflow confirming successful venous access. If a vein is small or has collapsed and no backflow is noted, 0.5 mL of lidocaine can be injected to see that no extravasation of the solution occurs, which serves as confirmation of a successful cannulation. The lidocaine is a vasodilator that enlarges the vein and also decreases the sensation of the venous injection of certain drugs, which can irritate the vein. It is important to never remove one’s hand from the IV catheter after it is successfully inserted until after it is secured with tape, to prevent loss of the IV catheter by movement of the patient’s hand or by the patient managing to pull it out. A microdrip IV tubing of 60 drops/mL is attached to the catheter. A microdrip, as opposed to an adult IV line of 15 drops/min, will assure that the patient is not overloaded with fluid quickly, and the microdrip will allow a slower, more even drug release.