The oral ulcerations caused by aphtous lesions, herpetic lesions, candidiasis, ulcerative lichen planus, mucous membrane pemphigoid, and pemphigus vulgaris are managed in a step-up approach that can involve topical, intarlesional, and systemic pharmacologic management. This article reviews the common treatment agents, modalities, and dosages. The emphasis is on local pharmacologic therapies, yet systemic conditions that often present with such oral lesions are briefly reviewed, along with the appropriate management.
Key points
- •
Topical therapy is the first line of treatment of aphtous, herpetic, candida, and lichen planus lesions of the oral mucosa.
- •
Topical medications can be used in the management of oral pemphigus and pemphigoid lesions.
- •
Intralesional injections allow maximum local benefit with minimal systemic effect.
- •
Systemic conditions need to be ruled out in patients with recurrent or persistent oral lesions.
Introduction
The general dentist should be able to identify the presence of soft tissue lesions in the oral cavity. Some of these lesions may be symptomatic, others could be incidental findings. Their cause could be local or systemic. This article provides an overview of the current pharmacologic modalities available to treat aphthous lesions, herpetic lesions, candidiasis, ulcerative lichen planus, mucous membrane pemphigoid, and pemphigus vulgaris. The emphasis is on local pharmacologic therapies, yet systemic conditions that often present with such oral lesions are briefly reviewed along with the appropriate management.
Introduction
The general dentist should be able to identify the presence of soft tissue lesions in the oral cavity. Some of these lesions may be symptomatic, others could be incidental findings. Their cause could be local or systemic. This article provides an overview of the current pharmacologic modalities available to treat aphthous lesions, herpetic lesions, candidiasis, ulcerative lichen planus, mucous membrane pemphigoid, and pemphigus vulgaris. The emphasis is on local pharmacologic therapies, yet systemic conditions that often present with such oral lesions are briefly reviewed along with the appropriate management.
Aphthous lesions, also known as canker sores
Aphthous lesions are perhaps the most common form of oral ulcerations, the prevalence in the US population being approximately 20%. These lesions can occur as an isolated event or may reoccur at intervals as often as a few days in isolated or multiple foci. In such cases, the condition is known as recurrent aphthous ulcers or recurrent aphthous stomatitis (RAS) and it seems to be more frequent in women, patients younger than 40 years, white persons, nonsmokers, and those of high socioeconomic status. No precise cause has been identified; the cause is thought to be of genetic predisposition, immune mechanisms, anemia, possible nutritional deficiencies, or stress.
The typical features of aphthous ulcers are their predilection for nonkeratinized mucosa ( Figs. 1 and 2 ) and the associated pain. Lesions less than 1 cm usually heal within 1 to 2 weeks and larger lesions may take more than 6 weeks, yet scarring is uncommon. If the patient is immunocompromised, the lesion can become secondarily infected with bacteria or fungi.
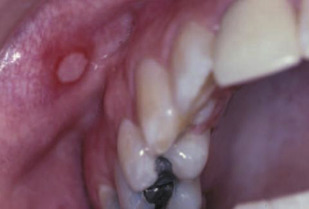
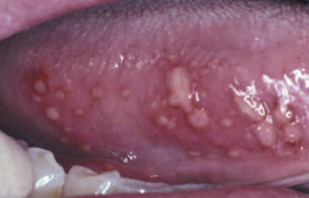
The treatment of aphthous ulcers is palliative, the goal being to reduce the duration, size, and recurrence of lesions. First-line treatment options comprise antiseptics, such as chlorhexidine, anti-inflammatory drugs, and analgesics for as long as the lesions persist ( Table 1 ).
| Medication | Class | Form | Dispense | Instructions | Notes |
|---|---|---|---|---|---|
| Chlorhexidine | Antibiotic | 0.12% | 480-mL bottle | 15-mL rinse and spit tid | Safe |
| Dexamethasone | Steroid | Elixir 0.05/5 mL | 100-mL bottle | 5-mL rinse and spit tid | Risk of mucosal atrophy Risk of systemic absorption with prolonged use |
| Minocycline | Antibiotic | 0.2% aqueous solution | 200-mL bottle | 5-mL rinse and spit qid for 10 d | Safe |
| Kenalog (triamcinolone) | High-potency steroid | 0.1% or 0.5% ointment in Orabase | 15-g tube | Apply to affected areas tid | Risk of mucosal atrophy Risk of systemic absorption with prolonged use |
| Clobetasol | High-potency steroid | 0.05% ointment in Orabase | 15-g tube | Apply to affected areas tid | Risk of mucosal atrophy Risk of systemic absorption with prolonged use |
| Fluocinomide | High-potency steroid | 0.05% ointment in Orabase | 15-g tube | Apply to affected areas tid | Risk of mucosal atrophy Risk of systemic absorption with prolonged use |
Topical steroids can decrease the symptoms and improve healing time, but do not affect recurrence rate. If multiple lesions are present, an aqueous solution is preferred. A dexamethasone rinse can be considered. In the case of isolated lesions, a high-potency topical steroid (kenalog, clobetasol, or fluocinomide ) in an adherent carrier, such as orabase or denture adhesive paste, can be applied in small amount to the specific area. Steroids should not be used for more than 2 weeks and the patient should be monitored for yeast superinfection. Also, topical steroids should not be placed on viral lesions, which could aggravate the lesion.
Minocycline, an antibiotic with immunomodulatory effect suppressing neutrophils, T lymphocytes, and collagenase activity, can also be used. A blind crossover study shows significant reduction in duration and severity of pain compared with placebo.
Intralesional treatment with triamcinolone (0.1–0.5 mL per lesion) can be considered for a painful single aphtha. In case of severe lesions resistant to topical or local treatment, a systemic steroid, such as prednisone, is recommended. It is started at 1 mg/kg/day as a single dose in patients with severe lesions and tapered after 1 to 2 weeks. The recommendation is to use less than 50 mg per day, preferably in the morning, for 5 days.
Severe cases of RAS can be treated with colchicine, pentoxyfiline, dapsone, or infliximab but these modalities should be reserved to oral medicine specialists because of the multiple side effects.
Additional therapies that have been reported to be effective are chlorhexidine, daily vitamin B 12 sublingually, and low-level laser therapy. A small study showed lower RAS recurrence in subjects using chewable nicotine tablets.
When treating RAS, the clinician should thoroughly review the medical history of the patient to rule out systemic conditions that are known to cause aphthous ulcers. The most common are Behçet syndrome, cyclic neutropenia, periodic fever with aphthae pharyngitis and adenitis syndrome, Reiter syndrome, and Sweet syndrome ( Table 2 ). Other possible conditions are Crohn disease, ulcerative colitis, immune deficiencies, and gluten-sensitive enteropathy.
| Disease | Specific Characteristics |
|---|---|
| Behçet syndrome | Severe aphthous ulcers, and recurrent genital ulceration, ocular disease, and a range of neurologic, renal, and hematologic abnormalities |
| Cyclic neutropenia | Recurrent oral ulcerations, fever, upper respiratory tract infections, and lymphadenopathy caused by cyclic reduction in the circulating levels of neutrophils, about every 21 d |
| Periodic fever with aphthae pharyngitis and adenitis syndrome | It occurs mostly in children and the condition usually improves with tonsillectomy |
| Reiter syndrome | Is an uncommon disease characterized by arthritis, urethritis, conjunctivitis, and oral ulcers |
| Sweet syndrome | Patients have aphthous lesions accompanied by fever, leukocytosis, and well-demarcated, plum-colored skin papules or plaques; there is an associated malignancy (eg, acute myeloid leukemia) in half of patients |
Oral herpes
In oral herpes, the principal symptom is the appearance of vesicles and ulcers that heal spontaneously within 5 to 10 days. The primary cause is often herpes simplex virus type 1 but epidemiology has been changing and herpes simplex virus-2, which was associated with herpes genitalis, can be equally found in herpes labialis.
The primary herpes simplex virus-1 infection can be asymptomatic or can cause gingivostomatitis; the virus then ascends the sensory axons of the trigeminal nerve, establishing latency in the sensory ganglia. It can become reactivated under various stimuli: stress, fever, ultraviolet light, trauma, or mensturation. On reactivation, the patient first experiences the prodromal symptoms of itching, burning, or paresthesia. The lesions first develop as vesicles ( Fig. 3 ) that eventually erupt forming ulcerations ( Fig. 4 ) and ultimately scabbing. The recurrent herpes labialis occurs typically at the junction of the vermillion and the cutaneous lip. Intraorally, it usually occurs on the keratinized mucosa, which distinguishes it from the recurrent aphthous lesions.
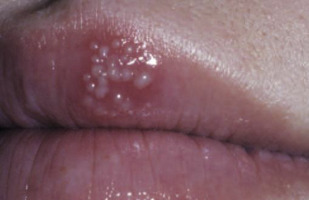
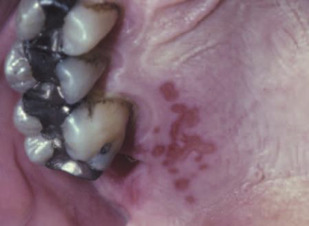
The aim of antiviral therapy is to block viral replication. Peak viral titers occur in the first 24 hours after lesion onset, when most lesions reach the vesicular stage. Thus, for the treatment to be effective, it should be started at the first signs, ideally during the prodromal stage.
For recurrent herpes labialis, the most common topical treatment options are acyclovir and pencyclovir ( Table 3 ). Because of the need of frequent applications, oral formulations are available for acyclovir, famciclovir, and valacyclovir. For prophylaxis treatment, such as before dental procedures, valacyclovir (1 g or 2 g twice a day) or acyclovir (400 mg two or three times a day) can be prescribed. Patients with severe recurrent lesions that do not experience prodromal symptoms may be candidates for long-term antiviral therapy.
| Medication | Form | Dispense | Instructions | Notes |
|---|---|---|---|---|
| Acyclovir | 5% ointment | 15 g | Every 3–4 h for 4 d | Must be started at first prodromal signs |
| Pencyclovir | 1% ointment | 5 g | Every 2 h for 4 d | Must be started at first prodromal signs |
| Acyclovir | 200 mg | 25 tablets | 1 tablet 5 times daily for 5 d | Must be started at first prodromal signs Can cause headache, gastrointestinal disturbance, rash |
| Famciclovir | 750 mg | 2 tablets | 2 tablets as a single dose | Must be started at first prodromal signs Can cause headache, gastrointestinal disturbance, nausea |
| Valacyclovir | 500 mg | 8 tablets | 2 g bid for 1 d | Must be started at first prodromal signs Can cause headache, gastrointestinal disturbance, rash |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


