Study
Allocation concealment
Outcome assessor blind
Withdrawals
Risk of bias
Stellingsma et al. [33]
Unclear
No
Yes, reasons given
High
Chiapasco et al. [7]
Inadequate
No
None
High
Raghoebar et al. [27]
Unclear
Yes
None
High
Raghoebar et al. [26]
Unclear
No
None
High
Chiapasco et al. [8]
Adequate
Yes, when possible
None
Low
Meijndert et al. [22]
Unclear
Yes
Yes, reasons given
High
Merli et al. [23]
Adequate
Yes, when possible
None
Low
Bianchi et al. [3]
Adequate
Yes, when possible
None
Low
Felice et al. [15]
Inadequate
Yes, when possible
None
High
Fontana et al. [18]
Adequate
Yes
None
Low
Schortinghuis et al. [30]
Adequate
Yes
None
Low
Felice et al. [14]
Adequate
Yes
None
Low
Felice et al. [16]
Adequate
Yes
None
Low
13.4.7 Allocation Concealment
While assessing the information presented in the articles, allocation concealment was scored adequate for three trials (18, 26, 32), inadequate for one trial (29) and unclear for all other trials. All authors replied to our request for clarification [7, 14, 15, 23]. While evaluating authors’ replies, one trial scored as being adequately concealed became not concealed 18; five trials were judged to be properly concealed (24, 28, 30, 31, 33), whereas four trials remained unclear 21, 23, 25, 34 [3, 6–8, 14–16, 18, 23, 26, 27, 30].
13.4.8 Blinding
While assessing the information presented in the articles for the outcome measures of interest in the present review that were possible to be masked, blinding of the outcome assessor was scored as unclear for all trials with five exceptions [15, 22, 23, 27, 30]. Three trials were scored as blinded (21, 25, 31) and two as blinded when possible (26, 29) [15, 22, 23, 27, 30]. All authors replied to our request for clarification. When evaluating authors’ replies, the outcome assessors of two trials were considered blinded (30, 33), of three trials blinded when possible (24, 28, 32) since complete blinding was not possible, and those of three trials as not blinded (18, 23, 34) [3, 7, 8, 14, 16, 18, 26, 32].
13.4.9 Completeness of Follow-Up
When assessing the information presented in the articles, information on drop outs was clearly presented in all trials, with one exception [7]. The authors confirmed that there were no withdrawals [7].
13.4.9.1 Main Inclusion Criteria
-
Severely resorbed mandibles, i.e. symphyseal height 6–12 mm as measured on standardised lateral radiographs of patients who have been ed entulous for at least 2 years and experienced severe functional problems with their lower dentures [32].
-
Residual bone height over the mandibular canal of 5–9 mm [3].
-
Residual bone height over the mandibular canal of 5–7 mm and bone width of at least 5 mm [15].
-
Residual bone height over the mandibular canal of 7–8 mm and bone width of at least 5.5 mm [14].
-
Residual bone height over the mandibular canal of at least 4.5–11 mm and bone width of at least 5 mm [16].
-
Patients with bilateral posterior mandibular partial edentulism (Applegate-Kennedy Class I) having a defect of more than 3 mm considering the deepest portion of the edentulous ridge in relation to the bone adjacent the last tooth [18].
-
Horizontal bone deficiency in a maxillary site (incisor, cuspid or first bicuspid) requiring a single implant [22].
13.4.9.2 Main Exclusion Criteria
13.4.10 Sample Size
A priori calculation for the sample size was undertaken in three trials [14, 15, 23]. The calculation of one trial was based on the complications that occurred in another similar RCT [19, 23]. Twenty-one patients were needed in each group to detect a difference between a proportion of complications from 0.27 to 0.80. However, the trial included only 11 patients per group, thus the sample size requirement was not fulfilled. In one trial of split-mouth design, the sample size was calculated to detect patient preference of one procedure over the other against the alternative hypothesis that treatments were equally preferred [15]. This reduced to a simple one sample proportion scenario. A one group chi-square test with a 0.050 two-sided significance level had 80% power to detect the difference between the null hypothesis proportion of 0.500 and the alternative proportion of 0.900 when the sample size is ten. The sample size was achieved. The calculations for another trial were based on implant failures [14]. A two group continuity corrected chi-square test with a 0.050 two-sided significance level had 80% power to detect the difference between a proportion of 0.100 and a proportion of 0.300 for patients experiencing at least one implant failure (odds ratio of 3.857) when the sample size in each group was 72. However, only 30 patients were recruited in each group and the size requirement was not fulfilled.
Baseline comparability between treatment groups
13.4.11 Effects of Interventions
Different techniques for horizontal bone augmentation.
13.4.11.1 Is the Augmentation Procedure Necessary? (No Trial)
Which is the most effective augmentation technique? (3 trials with 106 patients)
-
One trial compared two techniques for augmenting resorbed maxillae including atrophic maxillary sinuses [27]. Only patients with less than 5 mm of alveolar bone height in the sinus floor were included. Five patients were treated with a split-mouth approach with two-stage sinus lift with autogenous bone together with buccal onlays grafts, harvested from the iliac crest, one side with PRP and the other without. All patients were followed for 2 years after implant loading and there were no drop outs. No serious complications occurred at the grafted sites: one sinus membrane was perforated during surgery, but healing was uneventful. A small incision breakdown occurred in the first week at the non-PRP side of one patient. A seroma that healed uneventfully was the only complication that occurred at the donor sites. During the prosthetic phase one implant failed in the PRP side, but no prostheses failed. There was no statistically significant difference for any of the outcomes considered in this review. The difference in cost and treatment time was the use of PRP. Prostheses were inserted about 10 months after augmentation. The trial was judged to be at high risk of bias.
-
One split-mouth trial compared two titanium vs. two resorbable screws for fixating two-stage buccal onlay grafts, harvested from the iliac crest, to resorbed maxillae [26]. Eight patients were followed for 2 years after implant loading and there were no drop outs. No serious complications occurred at the grafted and donor sites. Two resorbable screws broke at insertion (one because of incorrect handling), but they could be removed and replaced. A small incision breakdown occurred in the first week at the titanium screw side of one patient. Another patient developed a slight submucosal swelling with redness of the mucosa above a resorbable screw 3 months after the augmentation procedure, which disappeared after implant placement. No prostheses or implant failed. There was no statistically significant difference for any of the outcomes considered in this review. The difference in cost and treatment time was the use of different screws. Prostheses were inserted about 10 months after augmentation. The trial was judged to be at high risk of bias.
-
One trial compared three two-stage techniques to horizontally augment bone at maxillary sites (incisor, cuspid or first bicuspid) to allow placement of single implants [22]. Thirty-one patients were included in each group and were followed up for 1 year after loading. The following procedures were tested: (1) autogenous bone block from the chin; (2) autogenous bone block from the chin plus a resorbable barrier; (3) 100% Bio-Oss plus a resorbable barrier. No patients dropped out. Not a single complication occurred. Two single implants failed early in the group treated with Bio-Oss plus resorbable barrier, though this difference was not statistically significant. Many other outcome measures (peri-implant bone level changes, patient satisfaction, aesthetics judged by patients and by an independent dentist) could not be used in the present review because data were aggregated and not presented by study groups. With respect to cost and treatment time, the additional costs for the barriers, and Bio-Oss should be considered. Patients had to wait 9 months (bone block groups) or 1 year (Bio-Oss plus barrier group) to be rehabilitated. The trial was judged to be at high risk of bias.
13.4.12 Different Techniques for Vertical Bone Augmentation
13.4.12.1 Augmentation Necessary? (Two Trials with 100 Patients)
-
One trial evaluated the need to augment anterior atrophic mandibles (residual bone height between 6 and 12 mm) up to 2 years after loading (Fig. 13.1) [33]. Twenty patients received four short implants (8–11 mm), whereas 20 patients received interposed iliac bone grafts and four longer implants (13–18 mm) to support overdentures. Two patients dropped out, one from each group about 3 months after overdenture delivery due to death and moving. In the short implant group two complications occurred: bleeding during surgery and permanent unilateral hypoaesthesia, and no early implant failure. In the augmented group six complications occurred: one life threatening complication (post-operative sublingual oedema which left the patient in intensive care for 3 days); two wound dehiscences; two unilateral dysaesthesiae, one of which completely recovered; and one necrosis of the osteotomized cranial fragment of the mandibles. In the augmented group four patients lost one implant each and a fifth patient lost all implants (possibly for necrosis of the osteotomized cranial fragment of the mandible and had to be re-treated), before or at abutment connection. Although the RevMan P value for the odds ratio (OR) was not statistically significant (p > 0.08), Fisher’s exact test (two sided) found a significant difference (p > 0.048), with higher implant failure for the augmented mandibles, confirming the findings of the original article. Statistically significant differences were also found at 3 weeks after the first surgical intervention: (1) 85% of the patients in the augmentation group reported serious pain for more than 1 week vs. 20% of the patients in the short implant group (OR 22.7; 95% confidence interval (CI) 4.4–117.5); (2) 30% of the patients in the augmentation group reported no improvement in their facial appearance vs. 80% of the patients in the short implant group (in this group, 70% reported no change, and 10% reported a deterioration of their facial appearance) (OR 0.11; 95% CI 0.03–0.46). The article also reported a statistically significant difference with 50% of the patients in the augmentation group experienced the operation more negatively than expected vs. 25% of the patients in the short implant group; however, we did not find this difference significant. With respect to prosthetic aftercare, four unplanned interventions were required in the short implant group vs. ten interventions in the graft group. Numerous aspects of patient satisfaction including aesthetics were investigated using validated questionnaires at 1 year and no statistically significant differences among groups were found. With respect to cost and treatment time, while short implants were placed under local anaesthesia, the graft procedures required general anaesthesia, a mean of 5.9 days of hospitalisation (range 3–9; SD 1.3) and the double healing time (about three additional months), and patients could not wear the lower denture for 6 months. The trial was judged to be at high risk of bias.
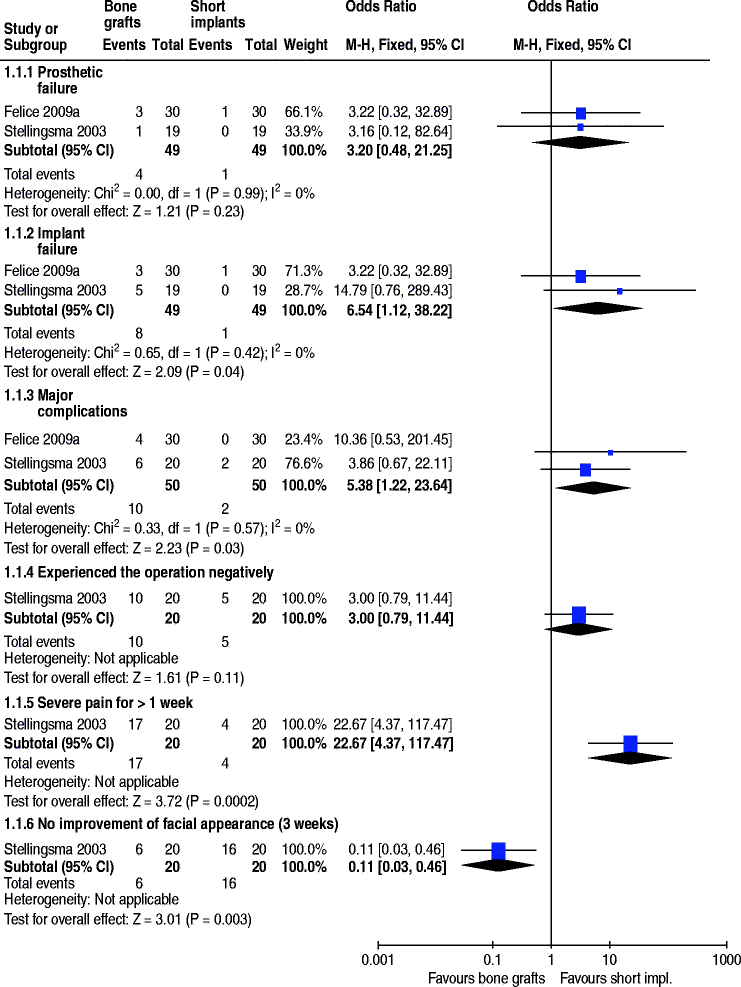 Fig. 13.1Forest plots illustrating the meta-analysis of two trials comparing short implants vs. augmentation of the mandible. Shot implants had statistically less implant failures and complications than longer implants placed in augmented mandibles
Fig. 13.1Forest plots illustrating the meta-analysis of two trials comparing short implants vs. augmentation of the mandible. Shot implants had statistically less implant failures and complications than longer implants placed in augmented mandibles -
One trial evaluated the need to augment posterior atrophic mandibles (residual bone height above the mandibular canal between 7 and 8 mm and width of at least 5.5 mm) up to 4 months after loading (Fig. 13.1) [14]. Thirty patients received 2–3 7 mm short implants and 30 patients received an interposed anorganic bovine bone block (Bio-Oss) and, after 5 months of healing, 2 to 3 10 to 15 mm long implants to support fixed partial restorations. No patient dropped out. No complications occurred in the short implant group vs. four complications (wound dehiscence/infections) in the augmented group: three of these dehiscence persisted until implant placement, and in two patients, partial loss of the bone graft occurred. Two augmentation procedures were considered a complete failure because the planned augmentation was not obtained and 7 mm short implants had to be used instead of the planned 10 mm or longer implants. These graft failures were associated with the fracture of the Bio-Oss blocks at the augmentation procedure. In the augmented group three patients lost one implant each vs. one patient in the short implant group and the related prostheses could not be placed when planned; however, all failed implants were successfully replaced and loaded. No statistically significant differences between groups were observed. With respect to cost and treatment time, short implants were loaded about 4 months after initiation of the treatment, whereas longer implants placed in augmented bone about 9 months after treatment start. The cost of one additional surgical intervention and of the Bio-Oss block for patients treated with the augmentation procedure should also be considered. The trial was judged to be at low risk of bias.
The meta-analysis of these two trials for the outcome measures (prostheses failures, implant failures and complications) resulted in statistically significant more implant failures OR > 6.54 (95% CI 1.12–38.22) and complications OR > 5.38 (95% CI 1.22–23.64) in the vertically augmented group (Fig. 13.1) [14, 33].
13.4.13 Which is the Most Effective Augmentation Technique? (8 Trials with 118 Patients)
-
One trial compared distraction osteogenesis in 11 patients vs. GBR with non-resorbable barriers and particulate autogenous bone grafts taken from the mandibular ramus (if not sufficient also from the chin) in ten patients for vertically augmenting edentulous ridges for 3 years after loading [7]. No patient dropped out. Two complications occurred in two patients of the osteodistraction group: the bone fragment inclined lingually during the distraction phase probably due to the traction on the osteotomized segment by muscle forces of the floor of the mouth. The complications were successfully treated by applying an orthodontic traction until the bone segment consolidated in the desired position. Five complications occurred in four patients of the GBR group: three barrier exposures occurred, one of which was associated with an infection, and two transient paraesthesiae of the chin area lasting 1 and 4 weeks. Both paraesthesiae were associated with the only two procedures for harvesting bone from the chin. All procedures for harvesting bone from the ramus were complication free. There was no statistically significant difference for complications between the two procedures. No implants or prostheses failed over the 3-year follow-up period. The mean bone gain after the augmentation procedure was reported for both groups, but without explaining how it was recorded or which were the reference points. Also data on peri-implant bone loss were unclear and could not be used. With respect to cost and treatment time, in the GBR group the cost of the barriers and the fixing pins should be considered vs. the cost of the intraoral distractor and related orthodontic therapy when needed. In the osteodistraction group, the time of exposing the implants ranged between 6 and a half months (mandibles) to 9 and a half months (maxillae) and patients were not allowed to use prostheses for about 3 and a half months. In the GBR group, the time of exposing the implants ranged between 6 and 7 months, when implants were placed simultaneously with the GBR procedure, and to 9–12 months, when implants were placed after the ridge had been vertically augmented. Patients were left without removable prostheses for 6–7 months. The trial was judged to be at high risk of bias.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


