Patient/problem
Diabetic ICU patients
Intervention
Nurse-driven continuous IV insulin protocol
Comparison
Intermittent subcutaneous insulin protocol
Outcome
Tightened glucose control
4.3.2 Finding and Evaluating the Evidence
Although much literature has been published on searching for and evaluating the available evidence to guide practice, a review is oftentimes needed for a better understanding of the search and evaluation of what constitutes “best evidence.” As noted earlier, evidence can include research findings, expert opinion, and scientific principles (e.g., theories based on biological plausibility). A fundamental principal of the evidence-based practice paradigm is a hierarchy of evidence that places findings from rigorous scientific research at the top, and expert authority and unproven inference from scientific principles at the bottom. According to this paradigm, the best evidence on which to base clinical decisions arises from a methodologically strong and clinically relevant research [23, 33, 37]. A variety of evidence pyramids have been proposed to rank the relative strength of research methodologies in answering practice questions; the highest level of available evidence is usually preferred to inform decisions [17] (Fig. 4.1).
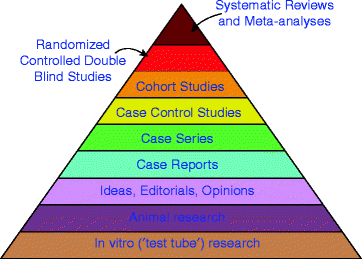

Fig. 4.1
The Evidence Pyramid. Available 25 February 2010 at http://library.downstate.edu/EBM2/2100.htm (with permission of the Medical Research Library of Brooklyn of the State University of New York (SUNY) Downstate Medical Center, New York, USA)
Although there is no absolute consensus within nursing or other disciplines about how best to define and rank evidence, it is generally accepted that the research methods that can provide the strongest evidence will vary depending on the question being asked [41, 44, 54]. The ability to identify the category of study that will best address a question is a core skill in evidence-based health care, and practitioners must be familiar with the study methodologies that offer the best evidence on the questions likely to arise in their practices and organizational settings.
Evaluating a study requires the identification of the appropriateness of a study’s methodology to answer a question. The study’s quality is then evaluated on the extent to which its design, conduct, and analysis minimized factors that might lead to bias or error [40]. If the study is of high quality and reported significant outcomes, practitioners must assess whether the findings can be used to improve outcomes for their individual patients in their unique practice environments. Textbooks and journal articles such as the User’s Guides to the Medical Literature series published in the Journal of the American Medical Association (JAMA) offer guidance on in-depth critical assessment of research studies [23, 32, 33].
To make optimal evidence-based decisions, practitioners should consider the whole body of evidence on a topic and not just the results from a single study. Systematic reviews and clinical guidelines are the prime examples of evidence-based resources to support practice. Systematic reviews of the evidence are usually considered to offer the highest level of evidence to answer a question [33]. Systematic reviews use explicit and rigorous methods to summarize data from primary studies in order to answer a focused clinical question. They require a comprehensive literature search to locate as much research as possible, and use predefined quality criteria to select the studies to include in the review. The selected studies are then rigorously appraised and synthesized, sometimes using techniques of meta-analysis. Like any other evidence, users must critically appraise a systematic review’s methodological rigor and the strength of its findings before applying those findings to patient care. Also, because systematic reviews often take months or years to conduct, users must make sure that their findings have not been superseded by newer evidence.
Clinical practice guidelines, like systematic reviews, are developed using systematic and explicit methods to locate, evaluate, and synthesize the evidence from as many studies as possible. Practice guidelines, however, usually go beyond systematic reviews in balancing a broader range of issues in a clinical context. The evidence basis of guidelines varies considerably; when research to support or refute a recommendation is lacking, authors must rely on expert consensus to make recommendations. The systematic evaluation of a body of evidence is usually done by small groups of experts, and guidelines are almost always developed under an organizational or society sponsorship [24].
It is clearly more difficult and time-consuming to evaluate a body of evidence than to evaluate the quality and strength of the evidence of an individual study. In most cases, an individual practitioner with clinical responsibilities will be unable to conduct a rigorous review of all of the research on a topic.
Finding the best evidence may seem challenging for health professionals. However, the rapid uptake of evidence-based health care has lead to the growth and development of specialized publications and databases that make it easier to find and apply the best evidence. Some of these resources have been specifically developed to support nursing decisions. To support optimal clinical decision and to standardize best practice, nurses frequently use protocols, clinical pathways, quality improvement (QI) programs, and similar guides. Other evidence-based resources available for nurses to support decision and practice include preprocessed resources (such as evidence-based topic overviews, structured abstracts, systematic reviews, and some textbooks), journal articles, and databases.
1.
Preprocessed resources
It is generally most efficient to begin a search by examining “filtered” or “preprocessed” resources. Pre processed resources are the ones where the authors have surveyed the literature, filtered out flawed studies, and selected those that are methodologically the strongest. Evidence-based topic overviews, structured abstracts, and systematic reviews are three examples of filtered resources [23, 27, 33]. In the United States, the National Guideline Clearinghouse (NGC) [34] an initiative of the Agency for Health care Research and Quality (AHRQ) and the Department of Health and Human Services (DHHS), provides a comprehensive database of clinical practice guidelines. NGC provides “structured abstracts” that facilitate the critical appraisal of a guideline’s recommendations. The structured abstracts systematically summarize each guideline and describe the methodology that the guideline developers used to collect and select the evidence; to assess the quality and strength of the evidence; and to formulate the guideline’s recommendations. A guideline comparison tool allows users to generate side-by-side comparisons for any combination of two or more guidelines. Many guidelines can also be identified through databases such as Medline/PubMed [51] and the Cumulative Index to Nursing and Allied Health Literature (CINAHL) [16].
(a)
Clinical topic review databases
This is a type of online “textbook” that has emerged over the last decade to support evidence-based practice. Clinical topic reviews filter and summarize the evidence to provide overviews to support decisions at the point of care. They are updated on an ongoing basis. UpToDate and BMJ Clinical Evidence are popular clinical topic review databases that have in-text citations to the evidence. BMJ Clinical Evidence provides systematic reviews on the prevention and treatment of clinical conditions, and ranks interventions on a scale ranging from “Beneficial” to “Likely to be ineffective or harmful” [6]. Although currently clinical topic review databases are oriented toward supporting medical practice, they provide in-depth information on a wide range of topics and may be especially useful to advanced practice nurses.
(b)
Structured abstracts
Structured abstracts use systematic and explicit methods to summarize a study’s objectives, methods, results, and conclusions. The abstract is enhanced by an expert commentary on the context, methods, and clinical applications of the study’s findings. Journals of structured abstracts free practitioners from having to look through all the journals in their field to identify articles of possible importance, and they facilitate the appraisal of the evidence, thereby streamlining the translation of valuable new research to patient care. Journals of structured abstracts of particular interest to nurses are Evidence-Based Nursing and Database of Abstracts of Reviews of Effects (DARE) [28]. Many journals of structured abstracts, such as Evidence-based Nursing, are indexed in the Medline database. DARE, however, is not indexed in the Medline. DARE contains over 10,000 structured abstracts of systematic reviews, and as noted above, systematic reviews are considered to provide the best evidence to support clinical decisions.
(c)
Systematic reviews
The single most important source of systematic reviews of health care treatments is the Cochrane Collaboration, an intentional consortium of review groups that develops and maintains systematic reviews and meta- analyzes. Cochrane Reviews are published in the Cochrane Database of Systematic Reviews (CDSR) [19]. Many consider the methodology used in Cochrane Reviews to be the gold standard for systematic reviews of treatments. Cochrane Review Groups of particular importance to nursing include the Cochrane Incontinence Review Group and the Cochrane Wounds Group. Completed Cochrane reviews can be found in the Cochrane Library, and they may also be identified through the Medline/PubMed and CINAHL databases, among others. Abstracts of Cochrane Reviews are freely available online, but a license is needed to obtain the full-text of the reviews. Systematic reviews that focus on nursing topics may be found in the JBI Library of Systematic Reviews [70] and the Worldviews on Evidence-Based Nursing Journal [67]. The Worldviews on Evidence-Based Nursing from The Honor Society of Nursing, Sigma Theta Tau International, is a source of knowledge synthesis articles as well as structured abstracts and original studies that aim to support decision making for clinical practice, nursing administration, nursing education, and public health care policies.
2.
Textbooks
In keeping with the evidence-based practice movement, textbooks (many now available in digital format) increasingly integrate evidence from primary studies and systematic reviews into their recommendations [31]. Given the rapid pace of change in health care, a major weakness of textbooks has been their lack of currency. A few medical textbooks are now updated regularly, but at this time we are unaware of nursing textbooks that are updated on an ongoing basis.
3.
Primary studies
If filtered resources do not answer a question, practitioners can obtain research evidence for decision making from primary research studies, which are usually published in the journal literature. The journal literature is usually accessed through electronic databases that contain citations and abstracts – and increasingly, links to the full-text – of the articles. The ability to search the journal literature for evidence is an important skill for evidence-based practice [11, 57].
4.
Database
The most important databases for retrieving studies of interest to nursing are Medline and CINAHL, although depending on the topic, it may be necessary to examine psychology, education, population health, sociology, or social work databases. Since nursing topics are interdisciplinary, it may also be necessary to search more than one database. Interdisciplinary databases such as ProQuest and Web of Science may also be useful. Conducting a literature search may appear daunting to time-pressed clinicians overwhelmed by the vast quantity of electronic information. Only a small percentage of the published literature contains evidence that is ready for clinical application [43]. The goal of a database search is to identify that subset of evidence that addresses the clinician’s question and that it is applicable in a local practice setting. At issue is the need to develop and maintain familiarity with the continuously evolving search interfaces of the databases most likely to provide evidence in a practice area.
Some nurses (generally, those prepared at the doctoral level) have the knowledge and skills of the statistical and analytical methods needed for in-depth appraisal of research evidence to determine best practices [62]. Nurses with other educational preparation can, however, learn to use the hierarchy of evidence to gauge the strength of a study. Nurses can assess whether the outcomes of the study would be significant to their patient population, and judge whether the findings could be applied in their clinical setting.
4.3.3 Making the Change
Knowledge for integration into practice can be generated through a new research and/or evidence-based project or through the synthesis of available research, or expertise of other sources of information [66]. Rogers’s theory of diffusion of innovations [59] defines concepts and describes processes to promote knowledge diffusion and utilization. Diffusion or dissemination of knowledge is defined as the process by which an innovation or new idea is communicated over a time period among the members of the social system. The major components of diffusion include the following:
1.
Innovation or idea perceived to be new by the individual or unit of adoption.
2.
Communication is the process in which participants create and share information to reach a mutual understanding through one to one, one to group, or through journals, periodicals, books, the internet, or media channels.
3.
Time spanning from introduction of an idea to rejection or adoption.
4.
A social system or set of interrelated units connected to accomplish a goal.
Roger identifies five stages in the innovation to decision process:
1.
Knowledge
2.
Persuasion
3.
Decision when the innovation or change is either rejected or accepted
4.
Implementation
5.
Confirmation (Fig. 4.2)
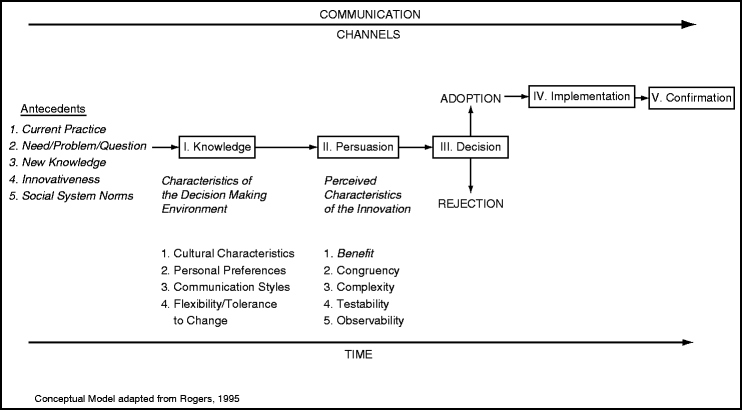

Fig. 4.2
Conceptual Model of Roger’s Diffusion of Innovations process from first knowledge of the innovation to implementation and confirmation
Opinion leaders present in health care can influence the rejection or adoption of an innovation during the knowledge phase. Rogers recognizes the importance of opinion leaders and the need to identify them in seeking adoption of evidence or research-based change. Advanced practice nurses among others are considered opinion leaders based on their clinical expertise and expanded education. Rogers describes the degree and agility with which adopters such as individual nurses will accept new ideas as (1) innovators or active seekers of new ideas, (2) early adopters who are often opinion leaders who learn about new ideas rapidly and then act as role models (3) the early majority or those who are active followers and will readily use a new innovation, (4) the late majority or those who are skeptical of new ideas and change but will change when the pressure is great and (5) laggards who are resistant to change and may or may not be persuaded to make the change and may leave the organization.
4.3.4 Evaluation and Maintenance
Knowledge generated, accepted, and successfully implemented requires ongoing evaluation to determine the quality, consistency, and applicability of the evidence over time and circumstance. The final stage in the evidence-based practice model process is evaluation and maintenance. Outcomes of evidence-based practice may be evaluated on a broad range of endpoints including the impact on patients, practitioners, and the system [69]. Evaluation methods may include QI monitors, surveys, and endorsement by respected peers [60]. Maintaining change supported by an evidence base is achieved by providing resources to practitioners to sustain the change and integrating the evidence into protocols, texts, procedures, policies, and the educational process. Change is most likely adopted and sustained when people affected participate in the process to make the change [59].
4.4 Summary
Demands of the current health care system provide a powerful reason for evidence-based practice. For nurses, moving forward to evidence-based decision making can be challenging. However, it is undeniably a responsible approach to providing best possible care to patients. Nurses are required to make clinical decisions in the moment, to know what to do and how to do it instantly, without conscious deliberation [14]. The judgments that nurses make in the moment have a moral component that guides what must be done in a responsible way based on nursing knowledge [14]. Evidence-based guidelines appropriately applied to clinical decision making can reduce uncertainty and diminish variation in practice promoting quality and safety for patients [59].
Evidence-based nursing practice as a concept is widely embraced by nurses as a means to improve quality outcomes for patients receiving care. It is also considered to be important to the discipline of nursing for expressing nursing practice as scientific competence [14
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


