Understanding the nature of the caries lesion, disease activity, and the patient’s caries risk are all used in determining the nature of dental care to be delivered. An examination should include a health and social history and clinical examination using appropriate technologies. This allows proper assessment and suggests a logical management intervention. Minimally invasive dentistry is a concept based on an assessment of a patient’s caries risk and the application of the current therapies to prevent, control, and treat the disease. The history of the dental examination and the variety of current technologies are discussed.
“Any dentist who cannot find any cavity of decay on any tooth with the explorer and mouth glass needs a competent assistant to make his examinations for him, and not a roentgen-ray machine.”
C. Edmund Kells before the American Dental Association November 10–14, 1924
Finding an accurate method for detecting and diagnosing any disease has been the goal of the healing arts since the time of Socrates. In the opening quote, Dr. Kells, speaking before the American Dental Association, voiced his opinion that bitewing radiographs should not be used to identify teeth with interproximal caries. His concern focused on: who would take the radiographs (a radiodontist was emerging as a dental specialty), who would pay for the radiographs, and, more significantly, would the radiographs disclose findings of clinical importance to patient care or would they result in overtreatment? This debate took place nearly 100 years ago, yet never has the diagnostic quandary over the detection of dental caries been greater and never has the importance of appropriate detection and diagnosis been more significant. Today, European and American caries experts do not share the same criteria in diagnosing caries and use a distinctly different language than most practitioners. In clinical practice, we describe dental caries with terms such as Class I or Class II caries with a surface attached to that “diagnosis.” Unfortunately, that classification tells us little about the actual surface with caries. For instance, is the caries on the mesial surface or the mesial and occlusal surface in the Class II? How deep has the carious lesion penetrated? What was the dynamic process of caries? Is the lesion active or has it become inactive? The decision of how and what to treat related to dental caries is no less confusing. Clinical research has demonstrated very different thresholds for the need for surgical caries treatment than have traditionally been practiced in the dental community. To best understand the controversy in how we diagnose dental caries, we need to understand the genesis of how the American diagnostic philosophy developed.
Miller proposed a two-step process whereby mixed bacteria, when exposed to fermentable carbohydrates, produced acids. In the second step, it acted on tooth structure to dissolve the hydroxyapatite and release free calcium and phosphates. The dental examination evolved in the late 1800s and was described by Green Vardiman Black in multiple writings. He defined caries as “a chemical dissolution of the calcium salts of the tooth by lactic acid, followed by the decomposition of the organic matrix…” This was consistent with Miller’s observations and fits the model of a destructive disease of the teeth. Black recognized that caries needed to be recognized early if it were to be prevented, stating that “decays must be discovered early, before the etching of the enamel has made much progress, if the preparation of a cavity and placing of a restoration is to be avoided” Essentially it was believed that caries could be “avoided” but there was no indication that it could be reversed. He advocated that the use of “small right and left explorers with curved tines, sharply pointed, are very effective in detecting the slightest estchings.” He suggested the use of firm pressure in the examination as well as a gentle pass over clean dry tooth surface. Black recommended an examination technique that started with the removal of surface deposits, using three explorers and a mouth mirror in a methodical process that would “reveal the beginnings of decay anywhere.” The only treatment available for dental caries, even for the slightest of enamel etching, was a restoration. Black developed a caries classification system that defined how we spoke about caries for the following century. He stated, “This classification is especially intended for use in technical procedures” and classified caries as Class I through V depending on the surfaces involved. The therapeutic modalities available in 1900 were extremely limited. Black’s amalgam formulation, cavity preparation, and restorations were effective and this classification system made perfect sense. There was only one bullet available: restoration; no fluoride, no modern toothpaste, and no remineralizing technologies. A simple caries classification system was perfectly effective. By the mid-twentieth century, the accumulation of plaque, subsequent production of acids within that plaque (in response to a glucose exposure), and subsequent recovery of the plaque pH to near neutrality had been demonstrated by Stephan. It was demonstrated that the introduction of dietary carbohydrate, even in thin layers of plaque, resulted in significant production of acid. The extent of the pH drop and the longevity of that drop are heavily regulated by both a patient’s saliva and their salivary components. This process of acid production in the demineralization of tooth structure (enamel and dentin) and the subsequent development of caries-generated tooth cavitation is a broadly accepted model.
Today it is recognized that dental caries is a dynamic process fluctuating between demineralization and remineralization over time. It is the net gain or loss of mineral over time that determines whether cavitation eventually occurs. The failure of naturally occurring and ongoing remineralization processes to keep up with the rate or severity of the demineralization challenge produces the eventual cavitation. The dynamic nature of the caries disease mandates that the recognition of the lesion be descriptive and specific enough to allow monitoring and assessment if the lesion advances over time (with advancing severity of the lesions being de facto evidence of ongoing disease activity). Because caries is a dynamic process, ideally the assessment of disease activity would be made over time. In clinical practice this is not practical. It is critical that the diagnosis of caries be improved to permit immediate and appropriate clinical decisions. Black’s edict to treat the earliest of all lesions with surgical modalities is no longer acceptable because there are multiple treatment and prevention technologies that can reverse early carious disease. Proper and comprehensive detection is critical.
Caries detection in the twenty-first century
Caries detection starts before the physical examination with a patient’s medical and social history. Like any of the healing arts, listening to the patient often tells the doctor the nature of the conditions afflicting them and, more importantly, the cause. No longer is starting a patient examination with just a medical history adequate. It must be comprehensive in that it includes the patient’s past dental treatment, dietary habits, and their oral health knowledge. This often discloses the cause of a patient’s caries problem, as well as their risk of developing new disease. This comprehensive history is critical in developing a patient-centered care plan tailored to their actual risk.
Visual and Visual-tactile Detection
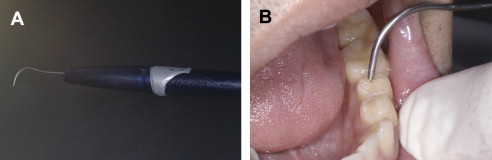
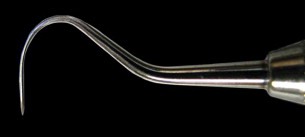
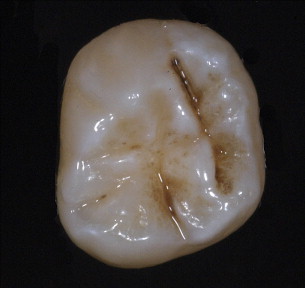
The physical detection of caries starts with a process of careful examination. The use of the sharp explorer to locate carious teeth was described by Taft in his text, A Practical Treatise to Operative Dentistry , in 1859 and later editions 1888, but there was no mention of the use of any pressure in the examination. Radike (1968) enhanced Black’s original diagnostic criteria by describing areas as carious when the explorer catches with moderate to firm pressure in the pits and fissures, as well as translucency around the fissures. On the smooth surface, evidence of demineralization or white spot, even without softness, was classified as a carious lesion, even without cavitation. The determination that an area was diagnosed as carious because it was a demineralization or white spot unfortunately continued to lend credence to the need for surgical restoration of these early lesions. Though diagnosis of caries with an explorer continued to have strong acceptance in the United States through the twentieth century, European cariologists had begun to use a different criteria for the diagnosis of caries. Including the early signs of caries during diagnosis favors the tracking of the disease process that is a fluid continuum. Visual or tactile examination using an explorer with moderate pressure, as recommended by Black and Radike, has fallen into significant disfavor. Ekstrand and colleagues (1987) demonstrated that use of a sharp explorer in a compressive fashion when examining the occlusal surface of teeth produced irreversible traumatic defects in the occlusal fissures that actually favored lesion progression. Further, a study of 34 dentists examining 61 teeth for occlusal caries revealed that there was no difference in diagnostic accuracy between those that used the traditional explorer and those that used visual-only examinations. The explorer did not add to the accuracy of the examination. The percentage of “clinically” correct treatment decisions was about 73% for both techniques with examinations using explorers having higher incidence of overtreatment and examinations using only visual having a higher incidence of “undertreatment.” Teeth classified in the undertreatment category using the visual only examination technique probably should be recommended for sealant therapy, rendering this underdiagnosis probably nonclinically significant. The findings of overtreatment with the explorer were reported earlier by Bergman and Linden (1969). In addition, their experiments indicated that the explorer could convert a white spot lesion into actual cavitation. Ekstrand and colleagues (2007) demonstrated that the use of a periodontal probe lightly moved across the lesion to detect roughness improved a practitioner’s ability to determine lesion activity. Roughness detected when lightly stroking the periodontal probe across the enamel in question is a sign of the current acid activity on the enamel surface. By 2001, the National Institutes of Health Consensus Development Conference on Dental Caries Diagnosis and Management Throughout Life concluded that “the use of sharp explorers in the detection of primary occlusal caries appears to add little diagnostic information to other modalities and may be detrimental” ( Fig. 1 ). The use of the explorer in a compressive force mode does not add diagnostic reliability if proper visual and radiographic examinations are conducted first. In fact, the use of the explorer after visual and radiographic examination is minimally likely to locate undiagnosed lesions and rather more likely to inappropriately diagnose as carious lesions that at best should be sealed ( Fig. 2 ). Avoiding damage created by explorers is important as Ismail (2004) emphasized that the “disease process may reverse or stop, resulting in complete healing of the demineralized dental tissue or in preservation of minutely damaged tissue.”
Radiology
Described in 1923 as “the most revolutionary aid in dental diagnosis which has come into general application during the present decade,” the dental x-ray has always been used with some controversy. With the introduction of early dental radiology techniques questions arose about who should administer the radiographs (a dentist or a specialized dental radiologist), then questions about their diagnostic quality (problems with tooth overlap and film positioning), and, through decades of x-ray use, concerns about ionizing radiation dose and exposure have existed. Bitewing radiology has demonstrated the ability to identify caries in the approximal region earlier than by visual examination alone. During the past decade, considerable discussion has been had about the quality of caries detection with the varied speed of the films available (eg, D-, E-, or F-speed film), but the one noted change is that film-based radiology is rapidly being replaced by digital capture and display. Film-based radiology has always been plagued by problems. The most noted were improper exposure time, inadequate processing quality, and poor positioning of the film. Digital radiology with generally lower radiation exposures has many of the same possible problems with the quality of the image. However, with digital radiology, postexposure manipulation of an image often enhances the image to produce results that are at least as satisfactory as film and often better. As the technology has continued to improve, many manufacturers have developed image analysis software that can highlight areas of discrepancy in image density, consistent with approximal caries, thus, alerting practitioners to areas that need closer evaluation. Currently in the research environment, technologies are available to monitor changes both in the density of the tooth as well as changes in the size of the lesion. This technique, subtraction radiography, requires extreme standardization of exposure, both dose and position, to optimize the accuracy of the data collected. The practicality in a private practice environment is poor.
Within dental clinical practice, the appropriate interval for radiographic reexamination has changed over the past 50 years in recognition that ionizing radiation has the potential for side effects that may be harmful to the patient’s health. The current therapeutic interval should be adjusted to the patient’s caries disease risk always using as low as reasonably achievable (ALARA) exposure.
Caries diagnosis using light
Light has always been used in dental diagnosis. Early dental offices were designed to allow the use of daylight through windows to improve the diagnosis of dental disease. Dentists wore reflectors and early candle-powered “head-lamps” to illuminate the dental cavity with light. Today, the varied spectrums of light are used in different ways to examine for dental caries.
Transillumination
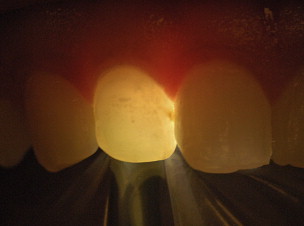
Transillumination is whole-spectrum high-intensity light narrowly focused to use light to penetrate the tooth structure and permit the identification of varied tooth density and light scattering to identify caries (similar to the variations in tooth density detected using the ionizing radiation, x-ray). As the light scatters passing through the lesion, it appears darker against a light background ( Fig. 3 ). It can be easily moved and compared without the negative effects of ionizing radiation allowing a three-dimensional rendering of the lesion. Fiberoptic transillumination (FOTI), when used to identify carious lesions on the occlusal surface, demonstrated its value with high correlations to both visual and histologic determinations with the greatest difficulty in both sensitivity and specificity in lesions just penetrating the dentinoenamel junction. When looking at small approximal lesions, it was found that FOTI was significantly less sensitive in lesion detection than bitewing radiographs. In an era of conservative nonsurgical intervention, the clinical significance of underdetecting lesions could have a significant effect on the clinical decision. When combined with other diagnostic techniques, FOTI improves both sensitivity and specificity.
Laser Fluorescence
Laser fluorescence has become a commonly used caries diagnostic aid. The principle of this device is that a monochromatic light source (655 nm wavelength) passes unhindered through a mature enamel crystal with little or no alteration. The 655 nm light has the ability to excite bacterial photoporphyrins, resulting in fluorescence. With changes in the enamel, increasing amounts of the light are scattered. Changes in fluorescence can be quantified to describe the presence and severity of the caries ( Fig. 4 ). Readings from the laser fluorescence can be confounded by the presence of stain in the pits and fissure and many restorative agents. These devices have been found to have high sensitivity of detection, but have only moderate specificity when readings are used without other detection aids and techniques. Good and proper clinical practice mandates that the practitioner have the knowledge that these devices may have the potential of overdiagnosis. It is critical that the practitioner use these devices in conjunction with good visual and radiographic detection, not as a sole diagnostic.
Quantitative Light- (or Laser-) Induced Fluorescence
Quantitative light- (or laser-) induced fluorescence (QLF) is an intraoral imaging technique that uses a specific wave-length of light to cause the fluorescence of dentin. Fluorescence is the emission of light by a substance that has been exposed to or has absorbed light of a different wavelength. In dental caries, as enamel lesions progress deeper, more of the light is scattered and there is less fluorescence from dentin present. The image of demineralization is seen as a dark area against a green background. The image captured can be quantified for the loss of fluorescence and the surface area using digital image software. The image from a baseline measurement can be superimposed on the image from a later date, allowing the ability to track the changes in the size and volume of a lesion with a wide variety of therapeutic methods. Differences are measured in the change in fluorescence and changes in the surface area. QLF has been heavily used by the research community in multiple research projects to assess both the presence of caries on smooth surfaces and to follow the natural process of remineralization. Examination of teeth with QLF demonstrated an extremely high sensitivity (95.5%) for locating demineralized regions, but if used without a visual examination the sensitivity (overdiagnosis) was only 11%. Utilizing a visual examination to eliminate obvious noncarious teeth, the specificity rose to 90.9%. Obviously, QLF needs to be performed in adjunct to a visual examination. QLF can detect precavitated demineralized dentin, monitor and quantify changes in mineral content, and can be used in short-term studies to evaluate the impact of dental products on tooth health. QLF units are expensive, limited to identifying caries on the surfaces of readily accessible teeth, and complicated to use, making use in private clinical practice rare.
Light-Induced Fluorescence and Light-Emitting Diode Caries Detectors
A recently released device uses the light-induced fluorescence technologies and developed a light-emitting diode (LED) technology. The diodes emit light at the 450 nm wavelength and the device focuses on the autofluorescence of the different layers of the tooth. Changes in the mineralization of the tooth can be identified in the process. The device records large areas of the tooth in one image and isolates areas of altered fluorescence. Organic deposits (as in stain), porosities, and crystalline destructuring disrupt the autofluorescence signal and may lead to incorrect assessment of the tooth surface with false-positive renderings.
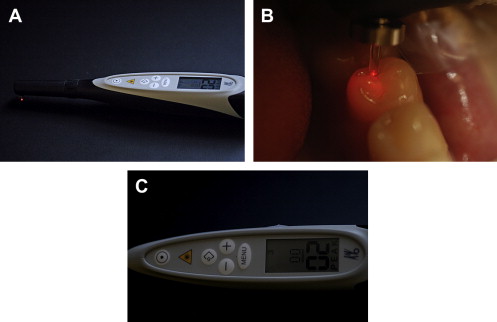
Another LED technology uses two LEDs (infrared 880 nm and red 660 nm) corresponding to a spectral area where differences are found between healthy and decayed areas. This technology provides a simple output in which a color indicator changes from green to red and an audible alarm that sounds more rapidly as caries is found ( Fig. 5 ). Both this technology and the light-induced fluorescence have few nonindustrial-sponsored published research studies and are scientifically supported principally by abstracts presented at conferences. All the research available has been conducted by the sponsors and none has been published in major dental journals.