Introduction
The aim of this prospective clinical trial was to examine the predictability of the protocol for premolar transplantation when applied by an inexperienced surgeon. Additional objectives were to examine the hard and soft tissues and to compare the findings with control premolars and also to record the patients’ opinions of the treatment provided.
Methods
The sample comprised 23 consecutively transplanted developing premolars in 19 patients. Their mean age at surgery was 12 years 8 months (range, 9 years 10 months-17 years). The mean observation time was 35 months (range, 6-78 months). Plaque accumulation, pocket depth, gingival recession, mobility, and pulp sensitivity were recorded for the transplanted and the control teeth. Standardized radiographs were used to examine hard tissues and crown-to-root ratios. Questionnaires were used to register each patient’s opinion about the treatment and its outcome.
Results
The survival rate was 100%, and the success rate was 91.3%. No significant differences were recorded between transplanted and control teeth. The patients’ perceptions of the surgical management and the treatment outcome were favorable.
Conclusions
The protocol for autotransplantation of developing premolars in growing patients was successfully adopted, regardless of lack of previous experience with this type of treatment.
Protocols for tooth transplantation described in the literature differ regarding the type of donor teeth and their stage of root development, the surgical technique, and the storage of the donor teeth before transplantation. The high diversity of the examined samples results in differing survival and success rates of treatment outcomes. Tooth transplantation might be perceived as an unpredictable alternative by surgeons unfamiliar with the procedure. It is therefore important for the orthodontist to reassure the surgeons that a predictable and simple transplantation protocol exists; with their help, this exciting approach can be used for many orthodontic patients with missing teeth.
In the1960s, Slagsvold and Bjercke established a protocol for autotransplanting teeth at the University of Oslo in Norway. It includes indications for transplantation, the surgical procedure, and follow-up guidelines described in these articles. The predictability of this method was further supported in a long-term follow-up of their material, which demonstrated that the transplanted teeth had a survival rate of 90% and generally did not differ from normal teeth 2 to 4 decades later.
The general orthodontic indication for selecting a donor tooth is a need or a possibility of a tooth extraction. Surgical indications require sufficient space at the donor and recipient sites and favorable root morphology, enabling atraumatic removal of the graft without damage to the root surface. Developing, unerupted, or erupting premolars with half to three quarters of the final root length are preferable donors because they have a high potential for pulp revascularization, normal healing of the periodontal tissues, and further root growth. Premolars are often extracted for orthodontic purposes. Their morphology and position in the dental arch facilitate atraumatic removal when selected as donor teeth. Zachrisson et al described the main orthodontic indications for transplantation of premolars: (1) agenesis of the mandibular second premolars in low-angle face types (normal or weak profiles) ( Fig 1 ), (2) traumatic loss of maxillary incisors ( Fig 2 ), and (3) unevenly distributed multiple agenesis ( Fig 2 ). The transplanted teeth should be observed for a minimum of 2 years to monitor eruption, pulp healing, and root development, which are required for a successful outcome.
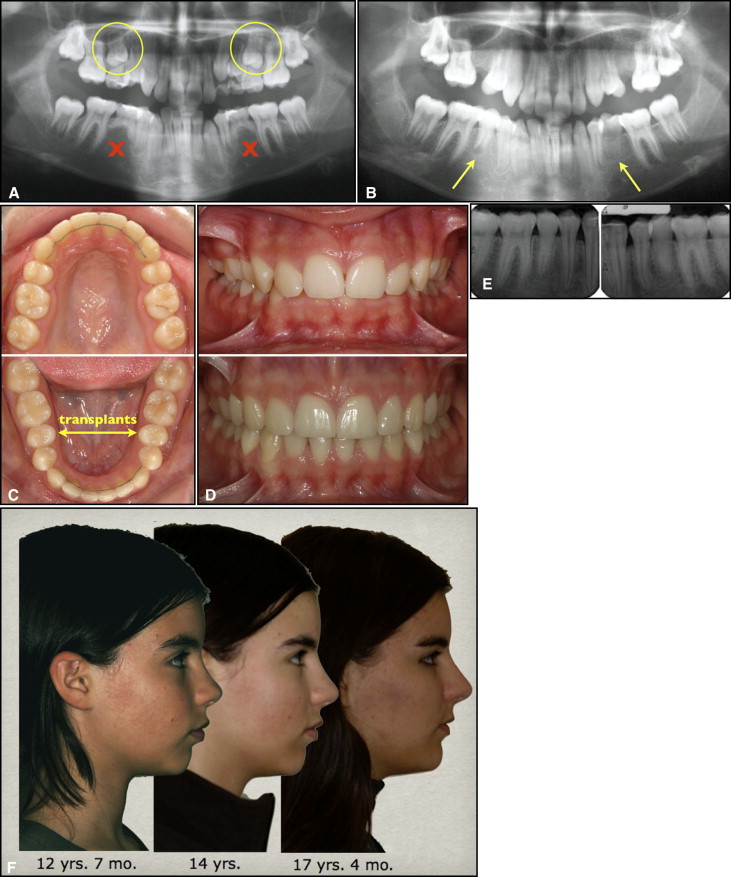
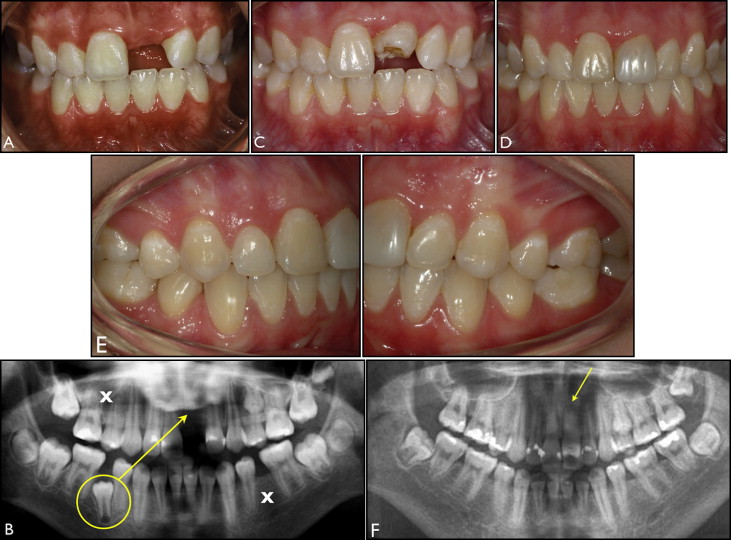
When a premolar is transplanted to replace a missing maxillary incisor, its crown needs to be reshaped with composite resin or porcelain veneer to match the natural contralateral incisor ( Fig 2 , D ). The clinical and radiologic statuses of premolars transplanted to the maxillary incisor region were similar to those of the neighboring incisors in a follow-up study. Premolars replacing incisors have the potential for satisfactory esthetics from both the patient’s and a professional perspective.
This protocol was adopted in Poland, a country without previous experience in tooth transplantation. The aim of this prospective clinical trial was to examine its predictability when used by an inexperienced surgeon. The study was performed by assessing the survival and success rates of a consecutive sample of autotransplanted developing premolars. Additional objectives were to examine the hard and soft tissues, to compare the findings with control premolars, and also to record the patients’ opinions of the treatment provided.
Material and methods
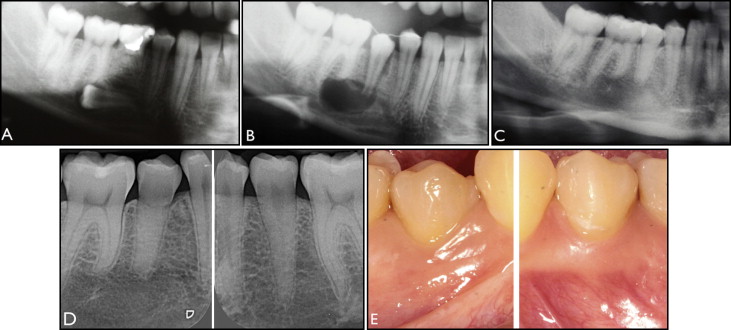
The sample included 23 consecutively autotransplanted second premolars with developing roots. The mean stage of root development was 4 (two thirds of the final root length), ranging from 2 (a quarter of the final root length) to 6 (full root length, wide open apex). The mean observation time after surgery was 35 months (range, 6-78 months). The teeth were transplanted in 19 patients (10 girls, 9 boys); the mean age at the surgery was 12 years 8 months (range, 9 years 10 months-17 years). Seventeen maxillary and 6 mandibular second premolars served as donor teeth to replace 2 maxillary and 13 congenitally missing mandibular second premolars and 4 maxillary central incisors lost from trauma. One maxillary and 3 mandibular ectopic second premolars were transplanted to a correct position (transalveolar transplantation) because orthodontic traction was considered impossible ( Fig 3 ). All premolars were transplanted by the same oral surgeon (P.P.) and had 2 months of clinical follow-up of tooth transplantation at the Department of the Oral Surgery and Oral Medicine at the University of Oslo in 2000 before this study.
Twelve second premolars, contralateral to the donor sites, served as the controls for intraindividual comparisons in the subsample having control teeth (12 pairs). No control premolars were available for 11 transplants (subsample without available controls) because 4 patients (8 transplants) had agenesis of both mandibular second premolars; consequently, both maxillary second premolars were transplanted ( Fig 1 , A-E ), and 3 patients (3 transplants) had agenesis or previous extraction of the contralateral premolar ( Fig 2 , B and F ).
All transplantations were performed under local anesthesia (articaine 4% with epinephrine 1:100,000). The first stage of the surgery aimed to gain access to a developing donor tooth because all teeth, except for 2 premolars in 1 patient, had not erupted ( Figs 1 , A, 2 , B, and 3 , A ). When a deciduous molar was present at the donor or recipient site, it was extracted at the beginning of the surgery. The first incision was made along the gingival margin followed by a vertical release of a flap on the buccal side at the donor site. The labial cortical plate covering the donor tooth was carefully demarcated with a bur under copious saline-solution irrigation. A thin layer of trabecular bone adjacent to the graft was gently removed with an excavator to prevent any damage to the root surface. The donor tooth was assessed for whether it could be removed atraumatically with intact dental follicle, cementum, and Hertwig’s epithelial root sheath. If this assessment was positive, then the recipient site (second stage of the surgery) was prepared using a conical bur under copious saline-solution irrigation until the size of the new socket could easily accommodate the donor tooth with surplus space of 1 mm around the root. When a recipient site was prepared in the anterior maxilla, the new socket was sometimes partially open on the labial side, as the result of bone loss after trauma and surgical dehiscence created by the preparation. If a further adjustment in size or shape of the recipient bed was necessary, the donor tooth was kept in the saline solution to protect it from drying for a maximum of 15 minutes.
In the third stage of the surgery, the donor tooth was transferred and positioned in the recipient site, ensuring no occlusal contacts during the initial healing. The donor was stabilized with sutures that crossed over the premolar’s cusps. When the transplantation was performed in the anterior maxilla, the bone dehiscences on the labial aspect were filled with remnants of the donor’s follicle.
The operating time was approximately 60 to 90 minutes. In all patients, healing was uneventful, with no signs of edema or inflammation.
The patients were recalled 2 weeks after the surgery for suture removal, at 1 month and every 3 months during the first year, and then once a year. Intraoral radiographs, mobility tests, and electric pulp testing were performed to detect possible complications (resorption, arrested root development, or pulp necrosis). At the final clinical examination, all transplanted and control premolars had erupted and were in contact with the opposing teeth. All transplants and controls had completed their root formations.
Four transplanted premolars were subsequently bonded with orthodontic brackets. Three of the 4 premolars transplanted to the maxillary anterior segment were reshaped with composite 12 to 24 months after the surgery.
The percentage of transplanted premolars present at the examination relative to the number of all transplanted teeth was called the survival rate. The success rate was calculated as the percentage of transplanted premolars fulfilling established success criteria in relation to the number of transplanted teeth. The criteria included no progressive root resorption, normal hard and soft periodontal tissues, and a crown-to-root ratio less than 1.
The clinical examination was performed by a trained and calibrated examiner (P.P.) using an electronic probe system (Florida Probe, Gainesville, Fla). The examination included plaque accumulation (0, not present; 1, present; recordings at 3 locations on the buccal side and 1 on the lingual side of a tooth), gingival recession height, and pocket depths. For each examined tooth, recession height and pocket depths were recorded at 6 locations (medial, central, and distal) on the lingual and buccal sides. For 2 transplanted and 2 control premolars, no pocket depth measurements were available. Tooth mobility was tested using the Mühlemann index. The percussion test, radiographs, and a distinct infraocclusion were used to detect signs of ankylosis (replacement resorption). Electric pulp testing was performed to determine pulp sensitivity when the electric pulp testing probe was brought into the contact with the buccal surfaces of the tooth.
Standardized, intraoral film radiographs (long cone-beam parallel technique) were used to examine the hard tissues, the outline of the alveolar socket (presence of lamina dura), and the pulp obliteration ( Figs 1 , E , and 3 , D ). The radiographs were taken using a positioner (x-ray holders), which was placed on a film, 30.5 × 40.5 mm, parallel to the long axis of the tooth and perpendicular to the x-ray central cone. The intraoral radiographs were assessed by 2 examiners (P.P. and E.M.C.), and the results were registered when both examiners agreed. Crown and root lengths were measured using digital calipers for calculation of the crown-to-root ratios. The measurements were repeated twice 8 weeks later, and the measurement errors were estimated using Dahlberg’s formula and Houston’s coefficients of reliability ( Table I ).
| Measurement | Dahlberg’s calculation | Houston’s coefficient of reliability (%) |
|---|---|---|
| Crown length (T) | 0.18 | 94 |
| Root length (T) | 0.19 | 96 |
| Crown length (C) | 0.20 | 94 |
| Root length (C) | 0.29 | 92 |
All patients were asked to fill in a questionnaire that included 7 questions ( Fig 4 ). The questionnaire addressed how the surgical procedure was perceived (5 questions) and asked the patient’s opinion about the current status of the transplanted tooth (2 questions). The answers were recorded using a 57-mm visual analog scale.

Statistical analysis
For the intraindividual comparisons (transplants vs controls) in 12 pairs, the exact McNemar test was applied to assess differences between the transplanted and control premolars for plaque, gingival recession height, and mobility. Linear mixed-effects models were used to test the differences between the transplants and the controls for mean pocket depth. The models were adjusted for correlations between 6 measurements of pocket depth and recession height for each tooth (3 measurements on the buccal side and 3 on the lingual side of the transplanted and control teeth) using treatment*side-specific random intercepts, and they contained the main effect of the side and the effect of transplantation nested in the side. The estimates of the probability of sensing the impulse during electrical pulp testing were computed with the Kaplan-Meier method. The exact Wilcoxon signed rank test was used to test differences between the transplanted and control premolars for crown-to-root ratio.
The subsample without control teeth (n = 11) was compared with the subsample having control teeth (n = 12) to test for any differences between them.
The Fisher exact test was used to compare the presence of plaque, recession height, and mobility. Differences in the pocket depths between the subsamples were investigated using linear mixed-effects models. The models were adjusted for correlation between the 6 measurements of pocket depth for each transplanted tooth and control premolar. The exact Wilcoxon rank sum test was applied to compare the distribution of the crown-to-root ratios between the subsamples. All computations were performed using software (version 9.1.3; SAS, Cary, NC). All tests were 2-sided at the 0.05 significance level.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


