Introduction
The purpose of this study was to compare maxillary arch dimensional and inclination changes during alignment with conventional brackets and self-ligation.
Methods
Ninety-six patients, ages 16 years and above, were included in this multicenter, 3-group parallel randomized trial. The main outcome measures were changes in maxillary intercanine, interpremolar, and intermolar dimensions, and molar and incisor inclination changes. The patients were randomly allocated in permuted blocks of 12 subjects into 3 equal groups with the allocations concealed in opaque sealed envelopes. Each participant underwent alignment with a standard Damon Q (Ormco, Orange, Calif) wire sequence for a minimum of 34 weeks. Blinding of clinicians and patients was not possible. Data were analyzed on a per-protocol basis, since losses to follow-up were minimal.
Results
Complete data were obtained from 87 subjects. Bracket type had no significant effect on any of the transverse dimensional changes. No difference in molar inclination was found between passive self-ligation and conventional brackets (0.67°; 95% CI, −2.24, 3.58; P = 0.65) or active self-ligation (0.91°; 95% CI, −1.95, 3.78; P = 0.53). Similarly, incisor inclination changes with the Damon Q could not be differentiated from those developing with either conventional system (0.44°; 95% CI, −1.93, 2.8; P = 0.71) or In-Ovation C (−0.22°; 95% CI, −2.58, 2.14; P = 0.85). No harms were encountered.
Conclusions
No difference in the arch dimensional or inclination changes during alignment can be expected between conventional brackets and either active or passive self-ligation.
The desire to treat patients on a nonextraction basis has been a persistent quest punctuated by apparent success, by resignation to failure, and recently by renewed fervor. Among the techniques and mechanics with the potential to facilitate nonextraction treatment are headgears, fixed sagittal correctors, and self-ligating brackets. Although each of these approaches necessitates an increase in arch length to produce alignment without extraction, it has been purported that passive self-ligating brackets can introduce specific, uniquely stable arch dimensional changes.
Self-ligating brackets have been advanced as a technique to streamline clinical procedures and reduce overall treatment time. However, although there is limited evidence proving clinical time savings and advantages relating to inventory requirements and chair-side assistance, there is a lack of evidence suggesting shorter treatment times with these systems. Nevertheless, the belief that these brackets expedite treatment and facilitate nonextraction approaches is firmly held by many clinicians. It has been claimed that passive self-ligating brackets promote posterior expansion without concomitant labial movement of the incisors; this claim has not, however, been made about active self-ligating brackets in which the clip encroaches on the archwire during the later stages of alignment. Previous randomized trials comparing arch dimensional changes with self-ligating and conventional systems have been restricted to the mandibular arch. These trials have also been equivocal, with 2 studies reporting statistically greater amounts of intermolar expansion with self-ligating systems.
It is widely accepted that both the magnitude and the nature of arch dimensional changes have an influence on prolonged stability. In particular, widening of the mandibular intercanine dimension is regarded as unstable. Similarly, tipping movements are typically impermanent. Moreover, there are defined limits to the dentition and negative esthetic connotations of excessive maxillary incisor proclination. Consequently, in many cases, a panacea would involve posterior bodily expansion with little change in incisor position.
The aims of this randomized controlled trial were therefore to quantify maxillary arch dimensional changes and maxillary incisor and molar inclination changes during orthodontic alignment by directly comparing a passive self-ligating bracket (Damon Q; Ormco, Orange, Calif), an active self-ligating system (In-Ovation C; Dentsply GAC International, Islandia, NY), and a conventional bracket system (Ovation, Dentsply GAC International).
Material and methods
Ethical approval for this multicenter, 3-arm, parallel-group randomized trial was obtained from the Cambridgeshire 1 research ethics committee in the United Kingdom (09/H0304/45). Participants were recruited from the orthodontic treatment waiting lists from April 2009 to June 2011 at East Kent Hospitals, Royal London Dental Institute, and Southend NHS Foundation Trust. The patients were given written and verbal explanations about the study. Those agreeing to participate completed a written consent form.
Based on previous research, 81 participants (27 in each group) were required with a power of 90% to detect a minimum difference of 1 mm (SD, 1 mm) between the largest and the smallest means among the 3 groups in intermolar width changes at the 0.05 level of statistical significance. To compensate for attrition of the sample and to enhance statistical power, a further 15 subjects (18.75%) were recruited, culminating in a total sample of 96 subjects. The power calculation was performed with Stata software (version 12.1; StataCorp, College Station, Tex) by using the fpower command for 1-way analysis of variance (ANOVA) power analysis.
The following selection criteria were applied. The inclusion criteria were (1) young adults 16 years of age and over; (2) fit and healthy, and taking no medication; (3) in the permanent dentition with the maxillary second molars erupted; (4) maxillary arch crowding less than 6 mm; and (6) amenable to nonextraction treatment in the maxillary arch. The exclusion criteria were (1) cleft lip and palate, and other craniofacial anomalies; (2) previous orthodontic treatment; (3) complex medical history and taking medications; and (4) congenital absence of teeth in the maxillary arch other than third molars.
All participants had study models and lateral cephalograms taken not more than 1 month before placement of the fixed appliance. An unpredictable, stratified subject allocation sequence was generated by using an electronic randomization program with stratified randomization for each center. Randomization was carried out in random permuted blocks of 12 patients in a ratio of 1:1:1. The assignment of each subject was implemented by 1 researcher (P.S.F.) and concealed from the clinician until the appointment at which the appliance was to be placed in sequentially numbered, opaque, and sealed envelopes. Corresponding envelopes were opened only after the participants completed all baseline assessments and were due to commence active treatment. The visibility of the orthodontic appliances precluded blinding of either the operator or the participant to the allocated arm during treatment. However, outcome assessors and data analysts were blind to the appliance type during data analysis.
Self-ligating preadjusted edgewise brackets (Damon Q and In-Ovation C) with Roth values for tip and torque and 0.022-in slots were placed in the intervention groups, and Ovation was used in the comparison group in the maxillary arch based on the random allocation procedure. A 0.013-in or 0.014-in round copper-nickel-titanium archwire (Damon; Ormco) of uniform arch form was placed in all patients with attachments placed on all teeth from the maxillary second molar to second molar. The conventional twin brackets were ligated with elastomeric modules. Areas with marked irregularity in the group with conventional brackets were tied with elastomerics in a figure-eight configuration or with stainless steel ligatures to permit complete engagement. Subjects underwent treatment with a predetermined Damon archwire sequence comprising 0.013-in or 0.014-in round copper-nickel-titanium, 0.014 × 0.025-in copper-nickel-titanium, 0.018 × 0.025-in copper-nickel-titanium, and 0.019 × 0.025-in stainless steel. All wires had Damon arch form and were uncoordinated to the original arch form or dimensions. The nickel-titanium wires were changed after intervals of 10, 10, and 6 weeks, respectively. The 0.019 × 0.025-in stainless steel wire was left in place for a minimum of 8 weeks. In relation to the maxillary fixed appliance, the archwire was cut distal to the second molar tube; the wire was not cinched distally. No bite planes, palatal arches, quad-helices, palatal expanders intermaxillary elastics, or headgear to the maxillary arch were used during the study period. All operators were given a copy of the treatment protocol before treatment. In cases of appliance breakage, every effort was made for the patient to be seen by a principal operator. If it was deemed impossible to religate a wire of the same dimension, this wire was replaced with a narrower wire within the wire sequence used throughout the study.
Alginate impressions of the maxillary arch were taken before treatment and at the end of alignment, a minimum of 34 weeks after appliance placement, when a 0.019 × 0.025-in stainless steel archwire was engaged passively. Models were measured as serial pairs and numbered for identification purposes with brackets obscured with wax on the posttreatment models during measurement. Measurements were made consecutively on each cast by an examiner (P.S.F.). Cephalograms taken before treatment and after arch alignment and leveling were traced.
The following transverse dimensions were recorded with digital calipers (150 mm ISO 9001 electronic caliper; Tesa Technology, Renens, Switzerland): (1) intercanine width, the distance between the maxillary canine cusp tips; (2) interpremolar widths, the distances between the buccal cusp tips of both the maxillary first and second premolars; and (3) intermolar width, the distance between the mesiobuccal cusp tips of the maxillary first molars.
The measurements were made in duplicate, and the average of the 2 readings was taken to a resolution of ±0.01 mm. The maxillary arch was viewed from above, and the calipers were held parallel to the occlusal plane. The degree of crowding on each model was determined by measuring the combined mesiodistal widths of the teeth from the mesial aspect of the first molar to the mesial aspect of the first molar (space required) and subtracting the arch perimeter (space available).
The gypsum reference models were digitized by using a scanner (AR250; 3Shape, Copenhagen, Denmark) comprising high-resolution charge-coupled device cameras, a laser projector, and an articulating table. The digital models were subsequently viewed and measured with proprietary software, by using a magnifying function (Orthoanalyzer; 3Shape).
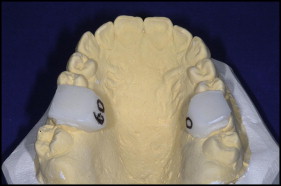
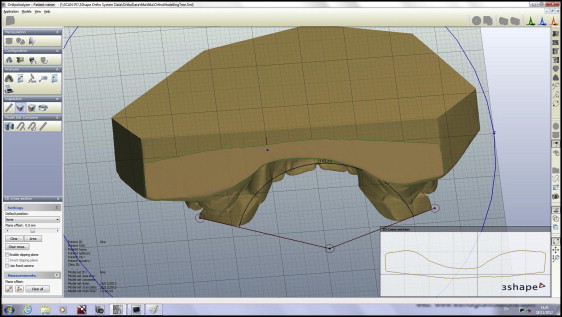
To improve the validity and reproducibility of estimation of the long axis of the teeth, opaque white polymethyl methacrylate caps with a flat upper surface were fabricated and fitted to the maxillary first permanent molars. The acrylic extended approximately 5 mm above the palatal and occlusal surfaces, and projected onto the buccal surface to withstand rotation of the model during the scanning process. The acrylic jigs were covered with an opaque sealer to prevent light penetration and involution of the jig on the resultant image; opaque stickers were added to the upper surface for the same reason while preserving the flat surface ( Fig 1 ). When necessary, before fabrication, marked occlusal fissures were blocked out with wax to permit a reproducible fit. Angular measurements were made by using a splicing function with the Orthoanalyzer software, visualizing the virtual models from the front or the rear view, whichever was thought to be more clear ( Fig 2 ). The orientation in which the model was measured was recorded, and this view was maintained during measurement of both pretreatment and posttreatment models.
In addition, 10 models were also scanned after removal and replacement of the jigs on the first molars. This permitted assessment of both the reproducibility of the measurement technique and the fit and placement of the jigs. The reproducibility of the technique was confirmed by repeating the measurements in random order 2 weeks after the initial readings, with a mean difference of 0.51° (SD, 2.01°) and 95% Bland-Altman limits of −3.42 and 4.45.
Angular changes in axial inclination of the long axis of the maxillary incisor relative to the maxillary plane were measured by assessing both lateral cephalograms. Radiographs were traced and measured as serial pairs. Two sets of readings were obtained for each measurement and their values averaged. Individual angles were retraced if differences between the values exceeded 5°. Maxillary incisor inclination was measured to a tolerance of 0.5°.
Statistical analysis
A descriptive summary of baseline demographic and clinical characteristics of participants in the study was undertaken ( Table I ) including sex, ethnicity, age, malocclusion, operator, crowding, and baseline inclination for each bracket system. Analysis of covariance (ANCOVA) was used to compare the influence of the 3 bracket systems on the transverse dimensional changes and the incisor and buccal segment inclination changes. Separate analyses were conducted for canines, premolars, and molars. Pretreatment crowding and pretreatment scores for incisor inclination or transverse dimensions were treated as covariates in the analysis to allow for differences in these potential confounders. An exploratory assessment of the effect of pretreatment intercanine dimensions on expansion of the maxillary interfirst premolar, intersecond premolar, and intermolar widths was also undertaken. Assumptions for linear regression were assessed by plotting residuals. All statistical analyses were conducted with Stata statistical software with a prespecified level of statistical significance of P <0.05.
| Appliance | ||||
|---|---|---|---|---|
| Damon Q n (%) or mean (SD) | In-Ovation C n (%) or mean (SD) | Ovation n (%) or mean (SD) | Overall n (%) or mean (SD) | |
| Site | ||||
| East Kent Hospitals | 21 (66) | 22 (69) | 22 (69) | 65 (68) |
| Royal London Dental Institute | 11 (34) | 10 (31) | 8 (25) | 29 (30) |
| Southend NHS Foundation Trust | 0 (0) | 0 (0) | 2 (6) | 2 (2) |
| Sex | ||||
| Male | 14 (44) | 14 (44) | 21 (66) | 49 (51) |
| Female | 18 (56) | 18 (56) | 11 (34) | 47 (49) |
| Ethnicity | ||||
| White | 26 (81) | 27 (84) | 28 (88) | 81 (84) |
| Asian Caucasian | 5 (16) | 3 (9) | 2 (6) | 10 (10) |
| Afro-Caribbean | 1 (3) | 2 (2) | 1 (3) | 4 (4) |
| Oriental | 0 (0) | 0 (0) | 1 (3) | 1 (4) |
| Malocclusion | ||||
| Class I | 9 (28) | 5 (16) | 6 (19) | 20 (21) |
| Class II Division 1 | 7 (22) | 8 (25) | 8 (25) | 23 (24) |
| Class II Division 2 | 1 (3) | 9 (28) | 1 (3) | 11 (11) |
| Class III | 15 (47) | 10 (31) | 17 (53) | 42 (44) |
| Operator | ||||
| 1 | 24 (75) | 27 (84) | 22 (69) | 73 (76) |
| 2 | 2 (6) | 3 (9) | 2 (6) | 7 (7) |
| 3 | 4 (13) | 0 (0) | 1 (3) | 5 (5) |
| 4 | 2 (6) | 0 (0) | 2 (6) | 4 (4) |
| 5 | 0 (0) | 0 (0) | 1 (3) | 1 (1) |
| 6 | 0 (0) | 2 (6) | 1 (3) | 3 (3) |
| 7 | 0 (0) | 0 (0) | 1 (3) | 1 (1) |
| 8 | 0 (0) | 0 (0) | 2 (6) | 2 (2) |
| Age (y) | 18.9 (2.9) | 22.5 (8.5) | 18.6 (3.4) | 19.7 (5.9) |
| Crowding (mm) | 2.3 (2.64) | 2.59 (1.99) | 2.56 (2.22) | 2.47 (2.28) |
| Maxillary transverse dimensions (mm) | ||||
| Intercanine | 32.21 (3.07) | 32.64 (2.89) | 33.5 (2.64) | 32.91 (2.88) |
| Interfirst premolar | 38.01 (3.5) | 38.94 (3.61) | 39.42 (2.64) | 38.9 (3.67) |
| Intersecond premolar | 44.16 (3.66) | 43.95 (3.55) | 44.72 (3.73) | 44.13 (3.63) |
| Intermolar | 49.36 (3.62) | 49.06 (4.26) | 50.02 (3.5) | 49.48 (3.79) |
| Maxillary incisor inclination (°) | 112.5 (6.47) | 109.25 (6.73) | 111.25 (7.23) | 111.24 (6.94) |
| Total | 32 (100) | 32 (100) | 32 (100) | 96 (100) |
Results
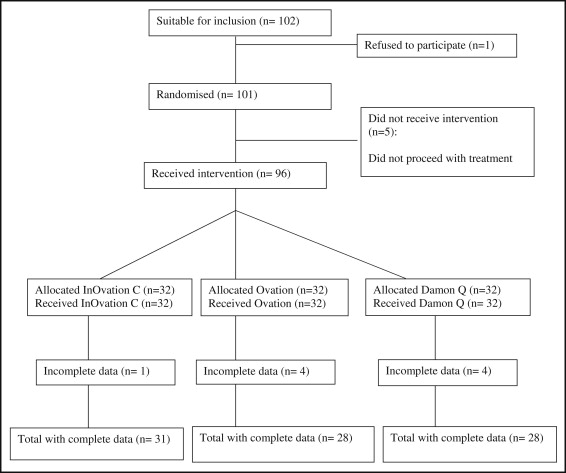
Overall, 101 participants were recruited; of these, 96 received an intervention. Nine participants had missing data; however, the data were analyzed on a per-protocol basis, since the attrition rate was relatively minor and unlikely to be attributable to bracket design ( Fig 3 ). There was little difference between the 3 groups in terms of demographic characteristics ( Table I ). There were slightly more male (n = 49, 51%) than female subjects. The majority were white subjects (n = 81, 84%). The participants represented a wide range of malocclusions with a large proportion of Class III cases (n = 42, 44%). Overall, there were 8 operators, although most participants were treated by the first author (P.S.F.) (n = 73, 76%). Subjects in the In-Ovation group were slightly older than those in the other groups, with their mean overall age 20 years. The degree of crowding in all 3 groups was mild (mean, 2.48 mm; SD, 2.28).
Intercanine dimensions increased in all 3 groups, with slightly greater increases in the Damon Q group ( Table II ). A slightly smaller increase in intercanine width arose with both In-Ovation C (−0.19 mm; 95%CI, −0.95, 0.57; P = 0.62) and Ovation (−0.66 mm; 95% CI, −1.44, 0.12; P = 0.10) compared with Damon Q after adjusting for initial intercanine width and pretreatment crowding. Those differences did not reach statistical significance. In the adjusted analysis, initial intercanine width was a significant predictor of the posttreatment value (β, 0.45; 95% CI, 0.34, 0.56; P <0.01), whereas a significant effect of pretreatment crowding was not identified (β, 0.02; 95 CI%, −0.16, 0.11; P = 0.73).



