Diagnosis and treatment planning are critical in preparation for implant placement. Adequate evaluation, preoperative imaging, and surgical planning minimize early and late-stage soft tissue injuries. Correct placement of dental implants can be challenging with several contributing factors such as lack of proper preoperative soft tissue evaluation and surgical experience in dealing with soft tissue incisions and flap reflection, resulting in injury and complications involving the soft tissues.
Key points
- •
Proper medical and clinical evaluations of patients is imperative to avoid soft tissue complications in implant planning.
- •
Several grafting techniques are available, and proper clinical judgment should be used to evaluate which technique patients may benefit most from.
- •
Patient anatomy should be taken into consideration when planning for soft tissue grafting.
- •
Soft tissue grafting may be indicated before, at time of, or after implant placement in order to reduce risk of soft tissue complications.
Overview of grafting principles
Soft Tissue Evaluation
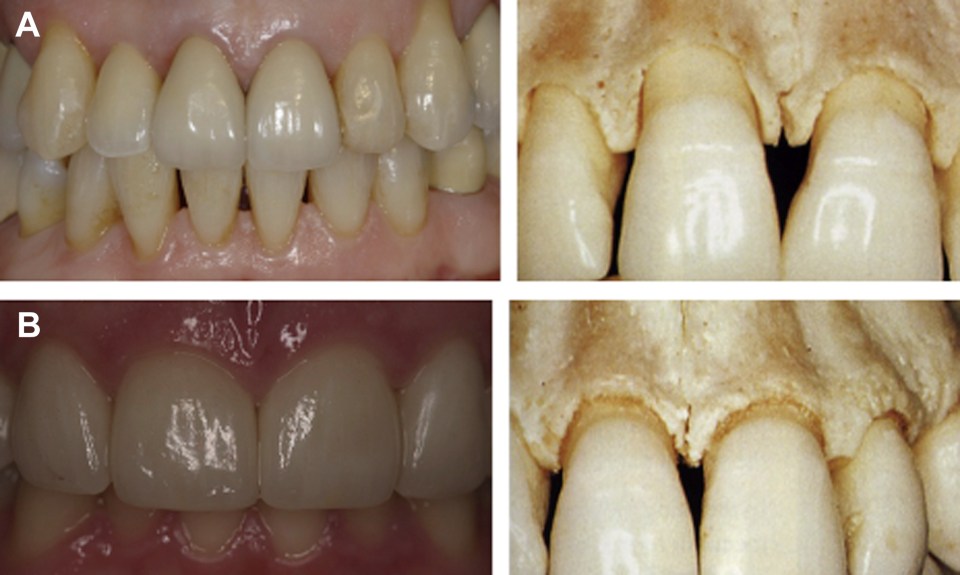
Evaluation of adequate quality and quantity of soft tissue is imperative before implant placement in order to optimize success. Attached tissue around dental implants allows for increased soft tissue stability, a decreased risk of soft tissue complications, and a favorable esthetic outcome. Evaluation begins with the gingival biotype as described by Olsson and Lindhe : thin scalloped versus thick flat ( Fig. 1 ). Gingival biotype is determined by variances in soft tissue, bone, and tooth morphology. Thin scalloped biotype reacts to insult with recession as opposed to thick flat biotype that reacts with pocket formation. The underlying buccal plate in thin biotype is thin with frequent fenestration and dehiscence type of defects, whereas the underlying bone of thick flat biotype is typically much thicker and rarely has dehiscences or fenestrations. The bony architecture in thin biotype tends to extensively remodel after extraction of teeth including increased loss of height and buccal plate and socket dimension, whereas thicker plates tend to undergo lesser remodeling. In thin biotype, teeth tend to be more triangular in shape with narrow contact areas in the incisal one-third, whereas in thick biotype, teeth are squarer in shape with long contact areas extending to the cervical one-third with a more pronounced emergence profile. Soft tissue grafting in patients with thin scalloped biotype results in improved esthetic outcomes and improves long-term soft tissue stability.
General Principles
Following the general principles in soft tissue grafting increases the chances of success and decreases complications. These principles involve the proper creation of recipient site, recipient site vascularity, adequate operative hemostasis, good graft adaptation to recipient site, graft thickness, proper immobilization, and closure.
During the initial healing stages (first 24 hours), a graft receives its nutrients by plasmatic diffusion, a process known as imbibition. This plasmatic diffusion is guided by the hypoxic gradient between graft and recipient site, providing initial nutrition to the graft. Following this, during days 2 to 3, the process of inosculation takes place and vessels from the graft anastomose with vessels from the recipient site. As graft healing proceeds during days 3 to 7, revascularization begins and ingrowth of new vessels into the graft takes place. After vascularity is achieved, remodeling takes place restoring normal histologic architecture.
Early graft mobility disrupts revascularization and increases chances of necrosis. Failure to achieve intimate adaptation of the graft to the recipient bed decreases plasmatic diffusion and increases capillary travel distance; similarly uncontrolled hemostasis can cause hematoma or blood clot formation hindering adequate nutrient support. Graft thickness also plays an important factor in healing. Thin and intermediate-thickness grafts tend to have higher survival rates. Thicker grafts also have less secondary contracture leading to better clinical outcomes.
Timing of soft tissue grafts can be variable, depending on several factors including the type of graft being used. No difference has been seen in outcome between simultaneous and phased soft tissue augmentation in implant placement when keratinized tissue width and soft tissue thickness are considered. They may be performed before, during, or after bone grafting, during or after implant placement, during second-stage abutment placement, or after crown placement. However, successful outcomes decrease when soft tissue grafting procedures are performed after crown placement.
Types of Soft Tissue Grafts
There are various options for soft tissue grafting, including connective tissue autografts, vascularized interpositional periosteal connective tissue flaps, palatal roll technique, and epithelialized palatal grafts.
Connective soft tissue autografts are commonly harvested from the hard palate or alternatively the maxillary tuberosity. The palate provides maximum volume, whereas the maxillary tuberosity provides a greater thickness. Palatal soft tissue is composed of 3 layers: epithelium, subepithelial connective tissue, and submucosa. Connective tissue grafts can be categorized as either subepithelial connective tissue grafts or epithelial connective tissue grafts.
Subepithelial connective tissue grafts are typically harvested between the palatal root of the first molar and the canine tooth for optimal thickness. Careful consideration should be given to the location of the greater palatine artery in this region to avoid injury. Reiser and coworkers reported the greater palatine artery enters the palate in the area of the greater palatine foramen and travels anteriorly in the direction of the incisive foramen ( Fig. 2 A). The greater palatine foramen most commonly is at the junction of the horizontal and vertical shelf of the palatine bone corresponding with the position between the second and third molar. The neurovascular bundle is located between 7 and 17 mm from the cementoenamel junction of the teeth with an average of 12 mm distance, with the distance being shorter in patients with a shallow palatal vault and longer in patients with a higher palatal vault ( Fig. 2 B). Dissection should therefore be limited to 8 mm in height to avoid injuring the greater palatine artery.

Vascularized interpositional periosteal connective tissue flaps were initially described by Sclar. The technique involves a rotation of a pedicled subepithelial finger flap to the anterior maxilla with a random pattern blood supply. This technique has several advantages as compared with free soft tissue grafts: it allows for effective simultaneous hard and soft tissue augmentation, provides superior soft tissue augmentation in both vertical and horizontal directions, and provides greater stability with decreased secondary shrinkage. It is ideal to correct large defects, and it is an optimal graft for compromised tissue beds. The main disadvantages are that this flap cannot be used with concomitant temporization or if the implant is not submerged.
The palatal roll technique as first described by Abrams is a split-thickness palatal flap that is reflected separating the epithelium from the connective tissue. The connective tissue is reflected from the palate and rolled onto the buccal to correct deficiencies in the buccolingual direction. The palatal roll technique was modified by Scharf and Tarnow in 1992 and is commonly indicated to correct minor buccal soft tissue defects during the time of implant placement or placement of the healing abutment.
The epithelialized palatal graft was first described by Bjorn and coworkers and was later modified by Sullivan and colleagues to describe full-thickness versus split-thickness grafts. Full-thickness grafts consist of epithelium and the entire zone of lamina propria, whereas split-thickness grafts contain epithelium and only partial thickness of lamina propria. Split-thickness grafts are further divided into thick, intermediate, or thin based on the width of lamina propria included. Epithelialized palatal grafts are indicated for mucogingival defects as well as the need to increase the zone of keratinized tissue.
Soft tissue complications during implant preparation
Soft tissue injuries and complications can result without proper evaluation of soft tissue sites before implant placement. An adequate preoperative medical evaluation also plays an important role in decreasing risk of complications, especially in smokers, alcoholics, immunocompromised patients, or those suffering from cancer, cardiovascular, or hematologic disorders. Although sometimes inevitable, surgical complications can be minimized through ensuring adequate planning and preparation of the soft tissue of the implant recipient site. Injuries and complications may occur before implant placement, after grafting, during implant placement, or after implant placement.
Infection
Surgical site infection can arise during the initial postoperative days and present as excessive edema, pain, erythema, and discharge. Adequate use of surgical asepsis may decrease the risk of this complication. Additional preventive measurements such as the use of preoperative antibiotics, appropriate oral hygiene, and the use of chlorhexidine 0.12% rinses during the first 2 weeks has also shown benefits. A study by Lambert and colleagues reported that there is a significant reduction in infectious complications when chlorhexidine rinses were used perioperatively during implant surgery. With chlorhexidine, there was a reduction of infection complications from 8.7% in the control group to 4.1% infection rate in the study group. Use of antibiotics is advised; however, they are not indicated in every case.
Edema
Swelling is caused by excess plasma fluid (transudate) accumulation in the interstitial space of tissues, defined as at least a 10% increase. It is correlated with the extent of surgical trauma and to the duration of surgery, and can cause severe discomfort to the patient and may negatively affect overall healing. Minimizing traumatic damage, the use of postoperative cold compresses postoperatively (<48 hours) and warm compress (after >48 hours), and corticosteroids may prevent or decrease edema after implant surgery.
Bleeding
Bleeding can occur due to traumatic handling of soft tissue during implant placement. This bleeding can be caused by failure to stabilize the flap, tearing of soft tissue caused by placing too much tension on soft tissue during closure, or a sharp suture material. Other causes of soft tissue bleeding include masticatory trauma from the opposing dentition or failing to appropriately modify a prostheses to be used after implant placement. Eliminating the cause of bleeding and use of local measures to promote hemostasis are included in treatment. Continuous bleeding after local measures are used will require reevaluation of the flap and exploration, followed by reapproximation of the flap to fully immobilize the soft tissue in order to promote clot formation and stabilization.
Ecchymoses and Hematomas
Ecchymoses are blood effusions infiltrating surface tissues, and hematomas are circumscribed blood collections. These can be dramatic and more prominent in elderly patients due to their increased capillary fragility. Several factors can contribute to these injuries such as longer and more complex surgical time, lack of surgical experience, traumatic surgical techniques, lack of postoperative patient compliance, elderly patients, and failure to discontinue antiplatelets medications (if indicated) before surgery. Intraoperative and postoperative ecchymoses and hematomas can be extensive if there is poor hemostasis during the surgical procedure.
Soft tissue ecchymoses typically resolve on their own, but the use of intermittent ice packs in the first 24 hours followed by moist heat after 48 hours can aid in resolution. If a hematoma is present between bone and the mucoperiosteal flap, it should be drained and external compression applied on soft tissue to avoid relapse.
Loss of the Graft
Partial or complete loss of connective tissue grafts is possible despite their high success rates ( Fig. 3 ). Adequate healing of graft sites depends on vascularity, thus immobilization of the graft at the time of surgery is imperative. Creating a flap at the recipient site allowing for primary closure may also decrease the risk of graft necrosis. Immediately postoperatively, the grafted site may seem pale and may turn grayish after 48 hours due to tissue ischemia. If adequate neovascularization is achieved by day 14, tissue will return to normal pink color and edema will resolve. Observation or conservative debridement is recommended depending on the extent of graft necrosis. The use of local measures such as gentle saline irrigations may also be beneficial.





