Orthodontists have always tried to develop ways to move teeth while minimizing the unwanted reciprocal movement of the teeth they pull against. This constant battle is more easily won when ideal anchorage is in place to move teeth in an efficient manner. Whereas dental implants were used as absolute orthodontic anchorage in the past, they had not become popular for a number of reasons, including cost, time of sequencing for osseointegration, and their primary use for dental restoration purposes, not orthodontic mechanics. These concepts of skeletal anchorage are not new, but have gained more attention in the literature as a result of a number of innovations in design and technique. Even as this chapter is being written, advances in materials and technique are poised to change how these procedures are planned and performed in the near future. The reader is encouraged to review the literature regularly because the pace of change is currently rapid.
The goals of orthodontic therapy include optimizing occlusion, aesthetics, and facial balance. Traditional orthodontic mechanics are very efficient at accomplishing these goals for clinical scenarios that require mild to moderate compensation. However, those patients that have more significant discrepancies require additional techniques. This is most evident to the oral and maxillofacial surgeon when one examines patients with moderate to severe skeletal discrepancies. Some of these patients who are beyond the envelope of discrepancy for standard orthodontic therapy can be compensated by using growth modification and/or orthognathic surgery in combination with comprehensive orthodontic therapy. Now patients with moderate discrepancies may benefit from skeletal anchorage devices to further compensate for malocclusions that were not heretofore possible to treat with traditional orthodontic mechanics. Additionally a whole host of problems encountered by the orthodontist on a regular basis are now more efficiently treated with skeletal anchorage as an adjunct to traditional mechanics.
This chapter discusses the basic concepts of skeletal anchorage devices of various types and reviews the current literature on their success. A primer on orthodontic mechanics is required to adequately treat patients with skeletal anchorage devices, and the reader is encouraged to review principles of orthodontic mechanics in conjunction with this chapter. Much like the concepts introduced during the beginnings of orthognathic dentofacial teams, treatment that uses skeletal anchorage requires interdisciplinary collaboration and planning with regular interaction, continuing education, and a regular review of the literature. This constant communication between orthodontist and oral and maxillofacial surgeon is necessary to achieve superior results.
▪
HISTORY OF SKELETAL ANCHORAGE FOR ORTHODONTICS
Recent attention has increased the interest in orthodontic skeletal anchorage, although the concepts of using implantable devices for orthodontic anchorage have been present for at least one half of a century. Only recently have innovations in materials, new outcome data, and improved techniques thrust this concept forward as a more mainstream option for treatment. In the 1940s, Gainsforth and Higley experimented with Vitallium screws and wires in the dog ramus used for skeletal anchorage. This initial experiment was not considered a success. Linkow used blade-type implants in the posterior mandible to apply Class II elastics for retraction of maxillary incisors. This cross-arch technique was apparently successful, but has the disadvantage of requiring a blade implant placement and its osseointegration before use as an anchor. Sherman used dental implants in dogs for anchorage with marginal success. In 1979, Smith noted that dental implants could act like ankylosed teeth during orthodontic movement. In 1988, Sharpiro and Kokich discussed how dental implants could be used for orthodontic anchorage before their prosthodontic use, and a number of practitioners used this technique from this point forward. In 1995, Block and Hoffman used a hydroxyapatite-coated onplant placed in the midline palatal tissues for use with an orthodontic anchor device. This was moderately successful, but required the orthodontist to rethink anchorage in terms of palatal mechanics instead of what was typically used with brackets and bands. Costa used titanium miniscrews borrowed from plating fixation systems for orthodontic anchorage with some success. In 1999, Umemori et al. described techniques for using a modified rigid fixation plate for use as orthodontic anchorage. This was a particular leap in innovation because the plating system could be easily placed and significant force could be used without loosening of the device. This had been a major drawback of screw systems in the past. Sugawara et al. and a number of other groups worldwide subsequently described a number of interesting compensation techniques for a variety of problems that traditionally would have required orthognathic surgery to treat effectively, such as the anterior open bite and significant Class III deformity.
▪
BASIC ORTHODONTIC MECHANICS AND SKELETAL ANCHORAGE
To understand the indications for skeletal anchorage, the practitioner placing the devices must have a baseline understanding of orthodontic mechanics to ensure superior results. Planning for a team approach to a skeletal anchorage case is in many ways similar to planning for orthognathic surgery. Issues that arise in the preoperative, intraoperative, and postoperative phases of treatment concern both the orthodontist and surgeon. As such, constant collaboration must occur to ensure the best outcomes.
Anchorage is the resistance to unwanted tooth movement. Orthodontic tooth movement obeys Newton’s third law that states that for every action, there is an equal and opposite reaction. For every movement of a tooth in one direction, the force is distributed to the anchorage segment, thus potentially affecting the position of those teeth within the anchorage segment. If an orthodontist wishes to move a canine posteriorly (distally) but only one molar is present, then the molar will have a tendency to drift towards the mesial if the molar is used as an anchor for that movement. However, if more anchorage is provided to that area, then the movement can occur without unwanted mesial movement of the molar.
Skeletal anchorage devices do not allow faster movement of teeth or the ability to overcome exceptionally large discrepancies—the devices have limitations. However, they do provide absolute anchorage for orthodontic movement and do so in a number of novel ways. They allow for more efficient movement of teeth and address a number of anchorage problem areas that previously were difficult or impossible to resolve with traditional orthodontic mechanics alone.
Anchorage can be provided using intraoral or extraoral techniques. Intraoral techniques commonly use tooth-borne appliances to improve anchorage. This can be achieved by increasing the number of teeth in the anchorage unit. For example, teeth can be tied together with ligature wire to resist unwanted tooth movement in another area. Another way of increasing teeth in the anchorage segment is to use a transpalatal arch. A transpalatal arch can be fabricated to distribute force to another segment of teeth across the arch. Alternatively, elastic bands can be used between the opposing arches to provide additional anchorage. This technique is commonly used to close space after maxillary premolar extraction by retracting the anterior dentition of the maxilla with elastic bands bilaterally and attaching the elastic to the maxillary posterior teeth. These Class II elastics also help to minimize the unwanted mesial movement of the maxillary posterior anchorage segments. This technique is based on compliance and can be ineffective if the patient does not wear the elastics regularly.
Another way to provide maximum anchorage to the posterior teeth is to use a Nance button appliance that holds the posterior molars in position with an acrylic button on the anterior palate. Force can then be applied to the posterior teeth to close premolar space, and the tendency for the molar teeth to move mesially is resisted by the acrylic button on the palate near the incisive foramen. These appliances may irritate the tissue and become uncomfortable. Extraoral appliances, such as headgear, can also be used to provide additional anchorage, but are often subject to compliance issues and rarely offer more than 6 to 10 hours of force per day. They are also not readily accepted by some patients, particularly adults.
Skeletal anchorage appliances provide anchorage that is not tooth-borne, but rather based on stability within the bone. These devices are advantageous for a number of reasons, including:
- •
No or minimal reliance on existing dentition
- •
Patient compliance is not required
- •
Continuous rather than intermittent force may be applied
- •
Surgical procedures are necessary, but they are simple in most instances
- •
May be significantly less expensive than other surgical options, such as orthognathic surgery
- •
Force may be applied very soon or immediately after placement of the device
- •
The devices are easily removed
The anchorage applied may be considered direct or indirect. Direct techniques are those that apply force directly from the anchor to the segment that is to be moved. For example, maxillary plates placed at the zygomatic buttresses may be designed to provide intrusion force to the maxillary molars with the intent of closing an anterior open bite. This would be a direct technique because the force is applied from the anchor directly to the molar teeth. Indirect techniques tie the anchor device to the segment of teeth that requires more anchorage so that more traditional mechanics can be used in the area. Rather than an active, elastic connection between the anchor and the archwire, indirect anchorage involves an inelastic or even rigid connection between the anchor and the orthodontic appliances. For example, if a maxillary anchor is tied by a steel ligature to the anterior teeth to provide more anchorage to that segment, a coil spring could be used on the archwire to distalize the molar teeth. This would represent an indirect technique because the force used is along the archwire via the coil spring and represents a traditional type of mechanics in orthodontics. The advantage to the indirect technique is that most orthodontists already design their movements of teeth based on traditional mechanics. Providing additional anchorage via a skeletal device simply increases efficiency without necessitating a new appliance design or vectors and moments difficult to achieve in commonly used orthodontic techniques. Either a direct or indirect technique can be used in most situations, and each case requires careful planning to ensure ideal placement of the anchor for these purposes.
Skeletal anchorage devices allow orthodontic movements to be designed that were previously thought to be difficult, if not impossible. Thus, compensation beyond the typical envelope of discrepancy is possible for many clinical indications.
▪
BASIC ORTHODONTIC MECHANICS AND SKELETAL ANCHORAGE
To understand the indications for skeletal anchorage, the practitioner placing the devices must have a baseline understanding of orthodontic mechanics to ensure superior results. Planning for a team approach to a skeletal anchorage case is in many ways similar to planning for orthognathic surgery. Issues that arise in the preoperative, intraoperative, and postoperative phases of treatment concern both the orthodontist and surgeon. As such, constant collaboration must occur to ensure the best outcomes.
Anchorage is the resistance to unwanted tooth movement. Orthodontic tooth movement obeys Newton’s third law that states that for every action, there is an equal and opposite reaction. For every movement of a tooth in one direction, the force is distributed to the anchorage segment, thus potentially affecting the position of those teeth within the anchorage segment. If an orthodontist wishes to move a canine posteriorly (distally) but only one molar is present, then the molar will have a tendency to drift towards the mesial if the molar is used as an anchor for that movement. However, if more anchorage is provided to that area, then the movement can occur without unwanted mesial movement of the molar.
Skeletal anchorage devices do not allow faster movement of teeth or the ability to overcome exceptionally large discrepancies—the devices have limitations. However, they do provide absolute anchorage for orthodontic movement and do so in a number of novel ways. They allow for more efficient movement of teeth and address a number of anchorage problem areas that previously were difficult or impossible to resolve with traditional orthodontic mechanics alone.
Anchorage can be provided using intraoral or extraoral techniques. Intraoral techniques commonly use tooth-borne appliances to improve anchorage. This can be achieved by increasing the number of teeth in the anchorage unit. For example, teeth can be tied together with ligature wire to resist unwanted tooth movement in another area. Another way of increasing teeth in the anchorage segment is to use a transpalatal arch. A transpalatal arch can be fabricated to distribute force to another segment of teeth across the arch. Alternatively, elastic bands can be used between the opposing arches to provide additional anchorage. This technique is commonly used to close space after maxillary premolar extraction by retracting the anterior dentition of the maxilla with elastic bands bilaterally and attaching the elastic to the maxillary posterior teeth. These Class II elastics also help to minimize the unwanted mesial movement of the maxillary posterior anchorage segments. This technique is based on compliance and can be ineffective if the patient does not wear the elastics regularly.
Another way to provide maximum anchorage to the posterior teeth is to use a Nance button appliance that holds the posterior molars in position with an acrylic button on the anterior palate. Force can then be applied to the posterior teeth to close premolar space, and the tendency for the molar teeth to move mesially is resisted by the acrylic button on the palate near the incisive foramen. These appliances may irritate the tissue and become uncomfortable. Extraoral appliances, such as headgear, can also be used to provide additional anchorage, but are often subject to compliance issues and rarely offer more than 6 to 10 hours of force per day. They are also not readily accepted by some patients, particularly adults.
Skeletal anchorage appliances provide anchorage that is not tooth-borne, but rather based on stability within the bone. These devices are advantageous for a number of reasons, including:
- •
No or minimal reliance on existing dentition
- •
Patient compliance is not required
- •
Continuous rather than intermittent force may be applied
- •
Surgical procedures are necessary, but they are simple in most instances
- •
May be significantly less expensive than other surgical options, such as orthognathic surgery
- •
Force may be applied very soon or immediately after placement of the device
- •
The devices are easily removed
The anchorage applied may be considered direct or indirect. Direct techniques are those that apply force directly from the anchor to the segment that is to be moved. For example, maxillary plates placed at the zygomatic buttresses may be designed to provide intrusion force to the maxillary molars with the intent of closing an anterior open bite. This would be a direct technique because the force is applied from the anchor directly to the molar teeth. Indirect techniques tie the anchor device to the segment of teeth that requires more anchorage so that more traditional mechanics can be used in the area. Rather than an active, elastic connection between the anchor and the archwire, indirect anchorage involves an inelastic or even rigid connection between the anchor and the orthodontic appliances. For example, if a maxillary anchor is tied by a steel ligature to the anterior teeth to provide more anchorage to that segment, a coil spring could be used on the archwire to distalize the molar teeth. This would represent an indirect technique because the force used is along the archwire via the coil spring and represents a traditional type of mechanics in orthodontics. The advantage to the indirect technique is that most orthodontists already design their movements of teeth based on traditional mechanics. Providing additional anchorage via a skeletal device simply increases efficiency without necessitating a new appliance design or vectors and moments difficult to achieve in commonly used orthodontic techniques. Either a direct or indirect technique can be used in most situations, and each case requires careful planning to ensure ideal placement of the anchor for these purposes.
Skeletal anchorage devices allow orthodontic movements to be designed that were previously thought to be difficult, if not impossible. Thus, compensation beyond the typical envelope of discrepancy is possible for many clinical indications.
▪
DEVICES FOR SKELETAL ANCHORAGE
A number of devices have been used to provide additional anchorage for orthodontic purposes. As mentioned earlier, the early attempts that were successful used dental implants placed with the intention of using them for total skeletal anchorage. These had the significant drawback of requiring osseointegration before use in addition to the high cost. They also required aggressive surgery for removal. Although some could be kept in place for prosthetic use, it was often difficult to determine the exact position required at the end of orthodontic treatment when placing them for anchorage purposes before treating the malocclusion. Consequently, the implants were often not in ideal position for the final crown or prosthesis, either rendering them useless or requiring specialized prosthodontic techniques to compensate for poor position.
Various dental implants, including miniature dental implants, were used in a similar fashion and placed in the retromolar region for anchorage purposes. These also required osseointegration before use and surgical removal and, thus, had the same types of drawbacks. Similar devices continue to be used in the palate, either in the midline or parasagittal to the midline. The anatomy in this region does not support full bony integration of an implant in most instances. Midline insertion into the septum may provide initial stability, but may also create problems at the septum, such as septal perforation, either at the time of placement or at the time of removal. If the implants are placed parasagittally, a fistula may result when the implant is removed as a result of the thin bone in this region of the nasal floor and hard palate.
An attempt to get around these inadequacies of the endosseous implant approach was the onplant system with attachments that would penetrate through the palatal tissues for orthodontic anchorage. These onplants were coated with titanium or hydroxyapatite in the hope of osseointegration after a small palatal incision was made for a subperiosteal placement. Long-term outcomes of this technique have not been reported, and it has mostly been supplanted by single screws or plates at other locations. As with any palatal implant, the additional drawback of redesigning orthodontic mechanics around a device positioned on the palate requires significant planning by the orthodontist in a manner that is not conventional.
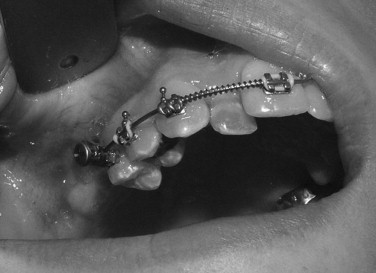
Placement of a bone screw for orthodontic mechanics has been described using a number of different screw devices. Recently, there has been an explosion of these screws commercially available for use. Originally, fixation screws used for craniomaxillofacial surgery were placed and then attached to the orthodontic appliance for use as additional anchorage. Other screw systems used for alternative purposes, such as maxillomandibular fixation, were modified for use as skeletal anchorage. Eventually, screws specifically designed for use in orthodontic skeletal anchorage were manufactured with versatile orthodontic attachments to optimize their use ( Figure 13-1 ). Both self-tapping and self-drilling systems are currently available.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


