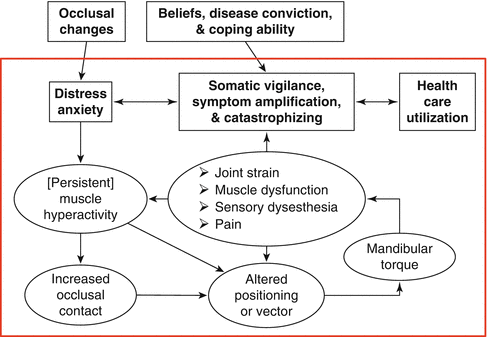
Fig. 4.1
General model for functional disorders. Physical and psychological processes directly associated with functional disorders are shown inside the larger box. Outside the large box are exogenous processes that represent life events, trait characteristics in the form of beliefs and coping style, and medical illness. All of these are illustrated as existing separate from the functional disorder (Modified from Sullivan and Katon [12])
It is noteworthy that TMDs, through the publication of the Research Diagnostic Criteria for TMD (RDC/TMD) [13], have led the pain field in terms of explicit recognition and assessment of the psychosocial aspects of pain disorders, with other disease domains now building related approaches [14]. As science progresses, the nature and number of psychosocial constructs deemed relevant to a pain disorder may change, but the critical clinical issue is that the psychosocial aspect of the patient must be assessed in some form, rather than being sidestepped because the clinician (or researcher) believes that this particular pain does not have any psychosocial significance. When a pain disorder is regarded as purely a physical process, that is, a disease and associated nociception, the clinical view is, most often, one of regarding only the body as relevant. As a result, various kinds of tests, imaging, and the like are requested because they are believed to be critical, whereas assessing the biobehavioral status of the person or requesting a pain psychology consultation is considered irrelevant, too expensive, or both. But we now know that how a person functions – before the pain disorder emerges, or as a consequence of pain, or in relation to different aspects of physically oriented treatment – has been shown to be critical [15–21].
The obvious tendency in the orthodontic consulting room is to regard a malocclusion as a purely physical aberration of the body; yet, the evidence from many studies clearly demonstrates that the majority of individuals seek orthodontic treatment for reasons of aesthetics and not functional limitation. [22, 23] A case series by one of the present authors (AM) revealed that individuals with severe skeletal malocclusions also seek care mostly for aesthetics, not functional limitation [24]. Equally striking is that restoration of those patients to a functional Angle’s Class I (mal)occlusion generally satisfies their chief complaint regarding aesthetics while simultaneously not providing any notable functional improvement. The latter absence of treatment effect, given the extreme physical impairment of such malocclusions prior to the treatment, remains a mystery. One salient point remains: malocclusions of all types are primarily aesthetic problems, and most individuals functionally adapt to severe malocclusions in an apparently sufficient manner, at least as indicated by the available data. One conclusion from this observation about structural problems versus aesthetics is that structural factors from malocclusions are clearly less important for understanding TMDs in comparison to psychosocial factors related to pain.
An assessment of TMD that incorporates the biopsychosocial domain can be as open ended as the practitioner wishes, and of course the direction and scope of such an evaluation will be determined by the nature of the chief complaint and what emerges in a symptom history as well as past history. From a pragmatic clinical perspective, where time in the consultation room is limited, and cognitive resources for gathering a history and putting the information together are equally limited, some type of structured evaluation for the psychosocial domain is generally both more efficient and clearly more reliable. The present authors have found that the structured format of the biobehavioral axis of the DC/TMD (as an update on the previously used RDC/TMD) is a very good place to start. Specifically, self-report instruments exist for each of the constructs of pain intensity, pain-related disability, functional limitation of the jaw, functional physical symptoms of the body, anxiety symptoms, depressive symptoms, and overuse oral behaviors. Collectively, these instruments adequately assess the current Diagnostic Criteria for TMD (DC/TMD) biobehavioral domain. Catastrophizing, not included in the DC/TMD at this stage, is the remaining pain-relevant construct that should be considered. These constructs are listed in Table 4.1, along with suggested instruments for their assessment.
Table 4.1
Recommended psychosocial domains for patient assessment
|
Domain
|
Suggested instrument
|
# items
|
Screening evaluation
|
Comprehensive evaluation
|
|---|---|---|---|---|
|
Pain intensity and pain-related disability
|
Graded Chronic Pain Scale (GCPS)
|
7
|
✔
|
✔
|
|
Pain locations
|
Pain drawing
|
1
|
✔
|
✔
|
|
Limitation
|
Jaw Functional Limitation Scale-short form (JFLS)
|
8 or 20
|
✔
|
✔
|
|
Distress
|
Patient Health Questionnaire-4 (PHQ-4)
|
4
|
✔
|
|
|
Depression
|
Patient Health Questionnaire-9 (PHQ-9)
|
9
|
✔
|
|
|
Anxiety
|
Generalized Anxiety Disorder-7 (GAD-7)
|
7
|
✔
|
|
|
Physical symptoms
|
Patient Health Questionnaire-15 (PHQ-15)
|
15
|
✔
|
|
|
Parafunction
|
Oral Behaviors Checklist (OBC)
|
21
|
✔
|
✔
|
Body dysmorphic disorder (BDD) is a particular psychosocial disorder of substantial relevance to both the orthodontic consulting room and this chapter. BDD is characterized by the belief that one’s own appearance is particularly defective, and those concerns interfere with normal functioning [25]. Even if only a slight defect is present, the concern is markedly excessive. Clinically, the individual is noted to have pervasive thoughts about the defect, which tend to be intrusive and are thereby distressing. Patients with a malocclusion (of any magnitude) who present with an obsession regarding an imagined or a greatly exaggerated defect in their appearance may be more accurately diagnosed as having a BDD. These individuals can be easily misdiagnosed in terms of the source of the distress (i.e., the belief about the malocclusion rather than the malocclusion itself). This becomes particularly true if pain is an accompanying symptom, because that pain may automatically be attributed to a nociceptive response to a physical stimulus. Once nociception is inferred, then a structural or physical cause for the nociception becomes the clinical focus for identification.
Consequently, if the orthodontic consultation overemphasizes the significance of the particular features of the malocclusion and contrasts those features with the importance of having an “ideal” occlusion, the orthodontist unintentionally can create the perception of the malocclusion as a serious defect in the person’s appearance, and therefore deserving of the patient’s concerns. This may then contribute to the iatrogenic development (or worsening) of BDD [26–28].
4.3 Why Behavior Matters in the Differential Diagnosis of TMD?
The best way to appreciate why behavioral assessment should be a part of diagnosing a TMD patient is to describe a prototypical individual presenting with a malocclusion to an orthodontist. That patient could have a masticatory muscle myofascial pain disorder simultaneous with a clinically important TMJ disc disorder. These may arise originally as two separate disorders, stemming from separate causes at two unrelated points in time, or they may exist as interrelated disorders emerging at the same time from a single cause. The distinction in the time course and potentially different etiologies may or may not be important for clinical management – the clinician must make an assessment from the history. Simultaneous with these two Axis I diagnoses (physical categories in the DC/TMD), there might be clinically important Axis II symptoms (psychosocial categories in the DC/TMD). These could include depression and anxiety, catastrophizing, and poor coping skills, which might be pain related or, as previously illustrated, could be focused on the malocclusion. There also may be ongoing and likely enduring life stressors as well as substantial interference in function from the myofascial pain disorder, and these problems would be revealed as part of an Axis II evaluation.
Some of the Axis II characteristics in this hypothetical patient might be intrinsically related to the current Axis I problems, and others, for example, anxiety, may exist due to wholly separable aspects of the person’s life and may have no impact on the pain. Alternatively, the anxiety may impact the patient’s pain greatly; the clinician needs to take a history to make this determination. While the extent of these Axis II symptoms can be readily assessed with standardized self-report instruments (see Table 4.1), the relevance to the chief complaint or to a differential diagnosis must be determined from the history. In addition, the individual may exhibit sleep bruxism as an enduring aspect of a sleep parasomnia. This behavior might aggravate the disc disorder and, because there is a malocclusion, the impact of the sleep bruxism upon the disc disorder may be interpreted to be occlusion-mediated. Finally, the malocclusion might be fully functional and adaptive for the individual but aesthetically is unacceptable. Given the other regional problems (pain, interference in functioning from the joint, and tooth grinding), all of which have specific diagnoses based on current knowledge, the significance of the malocclusion is not likely to be great in this patient.
In this example, part of the differential diagnosis is to place each complaint, each disease, and each illness characteristic into context. Initially, the patient presents with the chief complaints of a malocclusion (notably highlighted here as problems in aesthetics) and a pain problem, so the clinician needs to use assessment and diagnostic criteria that are presumably validated for each respective characteristic. For example, the anxiety disorder is assessed based on the validated features of anxiety, not because the person “seems” anxious, and not because someone with all of the other problems would surely be anxious. A validated and standardized self-report assessment instrument for anxiety will rapidly indicate the extent of any anxiety symptoms, and an interview will identify their context and relation to the complaints and clinical problems under consideration. The clinician might say, “I notice that you are reporting a number of symptoms of anxiety. Does your pain get worse when you are more anxious? And, when you are more anxious, do you tend to focus more on how your teeth appear?”
Similarly, a malocclusion is diagnosed based on its own parameters, and not because the person has symptoms of a TMD which according to the biopsychosocial model could exist as a result of a variety of presumed causes. In summary, differential diagnosis requires consideration of all measurable and classifiable problems, placed into a context, and ranked according to plausible mechanisms. In a case scenario like the one described above, the present authors would place the functional but unaesthetic malocclusion at the bottom of a problem list in terms of priorities, to be addressed only after adequately resolving all of the other complaints and identified problems.
4.3.1 Parafunctional Behaviors
Oral parafunction takes many forms, including tooth-to-tooth behaviors (such as clenching, grinding, and pressing of the teeth together), teeth-separated behaviors (such as bracing or guarding the jaw), soft tissue behaviors (such as cheek biting or tongue posturing), and others (such as musical instrument placement or telephone cradling with the jaw). Among these parafunctions, teeth clenching and grinding, nail and object biting, and gum chewing are the most commonly reported [29–32]. While all oral parafunctions were once regarded as a result of malocclusion (e.g., sleep bruxism was the body’s response to correcting an occlusal discrepancy; bracing the jaw was due to not having a comfortable centric occlusion), no causal relationship between any occlusal feature and oral parafunction has ever been supported by any evidence. In contrast, stress reactivity and habitual behavior have varying but sufficient levels of support as important features of oral parafunctions, and each of these belongs to the domain of psychosocial factors [33–36]. In addition, nocturnal bruxism has been identified as a sleep-related movement disorder with a multifactorial etiology.
The importance of oral parafunctional behaviors to both TMD and orthodontic treatment is becoming increasingly supported by research. Multiple studies have found significant associations between daytime oral parafunction (typically, clenching, and grinding) and myofascial pain [33, 35–37]. In addition, diurnal parafunctional activities can be a risk factor for disc displacement as well [37]. One proposed mechanism for parafunctional behaviors contributing to TMD is that such behaviors may overload the dentition and masticatory system [38, 39]. More specifically, the mechanism has been postulated to involve damage of muscle fibers [40] or to a reduction of blood supply [41]. Because most oral parafunction occurs at a low intensity level, but often for prolonged periods, the hypotheses of “overload” to the masticatory system and “damage” to muscle fibers clearly need better evidence and explanation regarding mechanism; at present, however, we do not know how parafunction exerts its apparently pathologic effects. A malocclusion coupled with a particular pattern of clenching or grinding might aggravate a disc displacement with reduction. However, not everyone with such malocclusions engages in parafunctional behaviors as described here, and those behaviors generally emerge independent of the malocclusion. The presence of the particular occlusal features will often be seen by some clinicians as causing the patients to do the particular parafunctional behavior, but this represents attribution bias, not causation.
The mechanism by which parafunction may affect the dentition and masticatory system (whether by “overload” or other mechanism) is equally relevant for orthodontic diagnosis, treatment, and posttreatment retention. According to the belief of an “occlusion-centered” etiology for masticatory system overload, an orthodontist may focus on the evaluation of centric condylar position, dental or skeletal discrepancies, and occlusal interferences [42, 43]. However, during orthodontic treatment, teeth are moved considerably, and this induces a stream of constantly changing occlusal interferences and continuous bouts of occlusal instability. As a consequence of the continuous change in the occlusal pattern, the achievement of any “ideal centric” condylar position cannot be guaranteed.
Finally, during posttreatment retention, attention is given again to the potential presence of occlusal interferences, and sometimes a limited occlusal adjustment is suggested to finalize and stabilize the orthodontic treatment results [44, 45]. This entire process often has the unfortunate side effect of inducing patients and their dentists to focus their attention on the necessity of an ideal and perfect intercuspation and on checking for potential occlusal interferences. The increased attention of the patients on their teeth can be detrimental if, during the posttreatment retention phase, even a little relapse of the achieved “ideal” occlusion occurs, inducing worries and fears. Interestingly, empirical data exist in support of this observation; a recent study showed that individuals with a history of TMD developed symptoms and adapted less well to the introduction of an active occlusal interference when compared to subjects without a TMD history [46].
In summary, oral parafunctions are behaviors that are not caused by malocclusion of any type. Rather, they are a function of mental states such as anxiety, stress reactivity, or simple habit; in the case of sleep bruxism, it is part of the sleep disorder phenomenology. Therefore, it is not the kind of malocclusion a person has but rather what the person does with it (e.g., parafunction) that matters in terms of symptoms that appear to be caused by the occlusion but are not.
4.3.2 Psychological Traits
Trait anxiety, somatosensory amplification, and hypervigilance are three psychological constructs with specific relevance to the focus of this chapter. While trait anxiety has been studied for decades with respect to its strong relationship to health and disease, somatosensory amplification and hypervigilance were identified more recently as core constructs involved in functional disorders. Functional disorders are also known as idiopathic pain syndromes when pain is the primary symptom, and as medically unexplained symptoms in other contexts. A primary characteristic of such disorders is that the extent of illness greatly exceeds the extent of objectively measured disease.
Trait anxiety refers to a general pattern of physical dysregulation and worry that is an inherent characteristic of an individual [47–49]. Somatosensory amplification refers to the tendency of the individual to perceive a given somatic sensation as intense, noxious, and disturbing [50]. And, hypervigilance is an increased awareness of the discrepancy between the perceived sensation vs. what is expected as “normal”, with a heightened attention typically focused on weak sensations. While each construct can occur independently of the others, together they appear to constitute a substantial triad linking a variety of psychosocial states with a variety of clinical disorders that overlap with TMD and problematic occlusions.
Trait anxiety might predispose to somatosensory amplification [51]. A number of studies have shown that somatosensory amplification is correlated with several indices of general distress including anxious and depressive symptoms [52–54]. Anxiety appears to influence the perception of orthodontic pain [55, 56], and individuals with prolonged pain during orthodontic treatment exhibit higher anxiety scores as compared to individuals with pain of short duration [57]. Orthodontic pain perception has been found to be significantly greater in individuals with high trait anxiety and somatosensory amplification [58]. Perhaps either of these processes could underlie pain complaints during orthodontic treatment that are misdiagnosed as TMD.
Moreover, anxiety and somatosensory amplification could jointly contribute to a more pronounced attention bias toward a potentially threatening stimulus represented by occlusal interferences. It is likely that individuals with high anxiety and/or somatosensory amplification are also hypervigilant against a perceived discrepancy in perceived vs. expected sensation. Such individuals may exhibit an increased awareness of their occlusion, reacting to those somatic sensations with emotional affect and cognitions that intensify them and transform them into more alarming, threatening, and disturbing sensations [51].
Individuals with high trait anxiety also exhibit greater amounts of parafunction [59]. Indeed, high levels of trait anxiety indicate an anxious personality disposition, which can be associated with a high rate of environmental scanning and reduced ability to switch attention away from the threatening stimulus. So, it could be hypothesized that patients presenting with high-frequency parafunctional activity are occlusally hypervigilant and are more disturbed by the occlusal interferences and changes induced by orthodontic therapy, resulting in pain and dysfunction. Occlusal hypervigilance may be explained by the Generalized Hypervigilance Hypothesis, according to which hypervigilance is a “perceptual habit” that involves subjective amplification of a variety of aversive sensations, not just painful ones [60]. According to this hypothesis, if attention is habitually focused on sensations of a particular type, their amplification increases and became autonomous [61]. Moreover, it has also been reported that some myofascial pain patients have high levels of somatosensory amplification that is characterized by a general bodily hypervigilance to unpleasant sensations [62]. This hypothesis could explain why, during the orthodontic treatment process, which creates several occlusal interferences throughout a long period, some patients do not adapt to the occlusal changes. These individuals may develop TMD signs and symptoms, which are then misdiagnosed as being “caused” by the constantly changing occlusion during orthodontic treatment.
The general model for functional disorders in Fig. 4.1 can be applied more specifically to the orofacial region, as shown in Fig. 4.2; the lower section (in regular font) is modified after Ohrbach & McCall [63]. Indeed, an occlusal interference in individuals who exhibit somatic hypervigilance, symptom amplification, or catastrophizing can induce a muscle hyperactivity that becomes persistent, which in turn leads to additional hypervigilance, symptom amplification, or catastrophizing, and ultimately more distress. Health care utilization that results in a focus on structure as the source of the individual’s distress will reinforce the hypervigilance, symptom amplification, catastrophizing, and distress. Collectively, these processes can lead to TMD pain, masticatory dysfunction, or both. Different levels of these factors might account for the high interindividual variability in perception of pain or discomfort observed in orthodontic patients during treatment [64, 65]. As a consequence, orthodontic practitioners should be aware of the psychological characteristics of their patients, and they should try to recognize those individuals who may represent yellow flags for irreversible dental treatments. This is especially true when patients report having multiple bad experiences with previous orthodontists, but now they have selected you to solve their problems.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses