Introduction
Our aim was to assess changes in maxillary incisor exposure, and upper lip and nasal soft tissues with maxillary advancement with or without impaction, accounting for the use of cinch sutures and VY closures.
Methods
This was a prospective study of 41 consecutive patients undergoing maxillary advancement with or without impaction. Lateral cephalometric radiographs and clinical measurements were taken preoperatively and up to 6 months postoperatively by 1 examiner.
Results
Thirty-one patients (19 female, 12 male) with a mean age of 25.5 years (range, 16.9-49.9 years) completed the study. Twenty-six received bimaxillary surgery. Fifteen had simple closures, 6 had cinch sutures, and 10 had alar base cinch and VY closures. The mean amounts of maxillary advancement and impaction were 3.34 and 1.6 mm, respectively. Soft tissues followed increasingly more closely the hard tissue advancement from pronasale to stomion superius. Mean maxillary incisor exposure increased at rest (0.5 mm) and on smiling (1.0 mm). The nasolabial angle increased (1.88°) because of columella upturning. Alar base width (3.09 mm) significantly increased.
Conclusions
Soft to hard tissue horizontal ratios increased progressively from pronasale to stomion superius. Alar base cinch and VY closures increased these further. Maxillary incisor display changes were partly explained by presurgical upper lip thickness and soft tissue manipulation. Nasolabial angle increased, and cinch sutures seemed to increase this further. Alar base width increased significantly, and the cinch sutures did not significantly limit this.
Highlights
- •
We assessed maxillary incisor show, and lip and nasal changes with maxillary advancements.
- •
This was a prospective clinical study on 31 patients up to 6 months postoperatively.
- •
Horizontal soft to hard tissue ratios increased from pronasale to stomion superius.
- •
Incisor show change was partly explained by lip thickness, cinch, and VY closures.
- •
Average nasolabial angle increased; cinch sutures partly explained this.
Contemporary orthognathic surgical planning revolves around the position of the maxillary incisors in relation to the upper lip and the soft tissue envelope of the face to achieve ideal facial esthetic and dental occlusal outcomes. The dynamic relationship of maxillary incisor exposure on smiling is also an important esthetic parameter. An attractive maxillary incisor exposure, as judged by both clinicians and laypeople, was 3 mm at rest and the whole crown with 1 mm or less of gingival display on smiling.
Therefore, because orthognathic surgery is planned around the maxillary incisor position, an understanding of the effect of different surgical movements and adjunctive surgical procedures (cinch sutures, VY closures) on the soft tissues, and in turn the effect of these on incisor exposure, is essential for treatment planning. Generally, a LeFort I maxillary advancement would increase the maxillary incisor exposure, whereas an impaction would tend to decrease it. Interestingly, no previous research has assessed directly the change in incisor exposure with orthognathic surgery or attempted to calculate ratios of hard tissue movement to change in incisor exposure.
Instead, research in this field, which is predominantly retrospective, has focused on calculating soft to hard tissue ratios of several radiographic points on the outlines of the lips and nose on lateral cephalometric radiographs, in both the horizontal and vertical planes. These ratios are in widespread use when using computer software or undertaking hand prediction tracings; the soft tissue changes are predicted using the soft to hard tissue ratios calculated in previous studies. In a systematic review, Kaipatur and Flores-Mir found that although the individual errors between the prediction and the actual measurement were minimal (<2 mm), the addition of these minimal errors could have clinical implications.
The range of the mean horizontal soft to hard tissue ratios from pronasale to stomion superius found in many studies (pronasale, 0.24-0.35; subnasale, 0.26-0.64; labrale superius, 0.36-1.43; stomion superius, 0.31-1.43) reflects a pattern where soft tissues from pronasale to labrale superius increasingly follow more closely the hard tissue movement, with labrale superius and stomion superius moving at similar ratios. Vertical ratios of soft to hard tissue movement are less well documented and demonstrate greater variability among studies. These ratios showed ranges of 0.28 to 0.52 at pronasale, 0.54 to 0.63 at subnasale, and 0.33 to 0.96 at labrale superius relative to maxillary incisor movement. In general, the upper lip soft tissue moves by 25% to 50% of the maxillary vertical movement.
Several potential variables may affect the ratio of soft to hard tissue movement after a LeFort I osteotomy: patient factors (sex, age), ethnicity, amount and direction of surgical movement, and lip thickness. Furthermore, a number of surgical adjunctive techniques are available to surgeons to attempt to limit unwanted soft tissue changes as a result of maxillary surgery. The most commonly used include anterior nasal spine (ANS) recontouring to reduce nasal tip upturning, VY closure to limit upper lip shortening, and alar base cinch sutures (AC) to limit alar width broadening. The effects of most of these variables and techniques are not certain, with conflicting results among studies. However, they could affect the upper lip soft tissue response and, in turn, the maxillary incisor exposure change. For example, in a randomized prospective trial, the authors found a statistically significant increase in upper lip height with a VY closure (1.10 ± 0.34 mm) compared with the shortening experienced by the simple closure group (−0.79 ± 0.45 mm). In another study, the authors found that VY closures decreased lip shortening by a factor approaching 2. It would be interesting to identify what effect, if any, these variables have on the soft tissue response, soft to hard tissue ratios, and maxillary incisor exposure to enable improved treatment planning and prediction of surgical outcomes.
Therefore, the primary aim of this study, which has not been tested in any previous study, was to assess the change in maxillary incisor exposure with maxillary LeFort I advancement orthognathic surgery with or without impaction. The secondary aim was to assess whether any adjunctive procedures used in the sample (cinch sutures, VY closures, ANS recontouring) had an impact on the primary aim. The changes in upper lip soft tissues and nasal soft tissues were also measured.
Material and methods
Ethical approval was granted by the South East London Research Ethics Committee (reference: 10/H0807/68) in 2010 for this study, and local research and development approval was granted by St George’s Hospital National Health Service Trust.
Patients were invited to participate by the investigator (L.K.L.), who discussed with them the study, provided information sheets, answered questions, and completed written consent forms. Inclusion criteria included (1) competent adults (>16 years) who provided voluntary, valid informed written consent; (2) undergoing orthodontic-orthognathic treatment involving a maxillary LeFort I osteotomy for advancement with or without impaction (with or without mandibular surgery) with rigid internal fixation; (3) no cleft lip and palate or other congenital deformities; and (4) no history of previous surgical procedures on the maxilla (that could affect the soft tissue response to surgery because of previous scar tissue).
Three experienced surgeons operated on the patients in this sample, using similar techniques for the orthognathic surgeries except for the adjunctive procedures. If patients received any adjunctive surgical techniques—eg, classical AC, ANS recontouring, or VY closure—these were recorded.
Once enrolled, patients were withdrawn if they decided not to go ahead with the surgery or the study, if model surgery showed that surgery had to be delayed (out of the study period), or if they failed to attend follow-ups.
Forty-one consecutive patients (26 female, 15 male) who were within 1 month of receiving orthognathic surgery by the oral and maxillofacial team at St George’s Hospital in London were invited to participate. Of these, 10 did not complete the study. The reasons for noncompletion were declined to participate (1), not ready for surgery (1), excluded because the decision was made to perform mandibular surgery only (1), incomplete data and hence not analyzed, (4) and lost to follow-up (3).
Therefore, the remaining 31 (19 female, 12 male) with a mean age of 25.5 years (SD, 8.6 years; range, 16.9-49.9 years) at the time of surgery constituted the subjects whose measurements are assessed in this study. The characteristics and surgical details of the sample that completed and failed to complete the study are shown on Table I . No statistically significant differences were noted between the 2 groups with regard to the sample characteristics (age, sex, and ethnicity) or the preoperative clinical or radiographic measurements (SNA, SNB, and ANB angles; upper lip thickness; and upper incisor inclination). The continuous quantitative variables were tested using t tests (with means and standard deviations), and the categorical or scored variables using chi-square tests.
| Characteristic | Completed study | Not completed study |
|---|---|---|
| Subjects (n) | 31 | 10 |
| Sex (F:M) | 19:12 | 7:3 |
| Age (y) | 25.5 (SD, 8.6; range, 16.9-49.9) | 22.1 (SD 4.7; range, 17.8-34.8) |
| Ethnicity | 26 white, 3 Asian (Far Eastern), 2 African Caribbean | 9 white, 1 Oriental |
| Malocclusion | 27 Class III, 4 Class II Division 1 | 9 Class III, 1 Class II Division 1 |
| Skeletal pattern | 27 skeletal III, 4 skeletal II | 9 skeletal III, 1 skeletal II |
| Surgeon | Surgeon 1 (13), surgeon 2 (11), surgeon 3 (7) | Surgeon 1 (6), surgeon 3 (4) |
| Type of surgery | 26 bimaxillary | 8 bimaxillary surgery |
| Maxillary advancement ± impaction & BSSO setback (23) advancement (3) | Maxillary advancement ± impaction & BSSO setback (6) advancement (2) | |
| 5 maxillary only | 1 BSSO only (reason for exclusion) | |
| 1 no surgery (reason for exclusion) | ||
| Adjunctive techniques | ACVY (10), AC (6), ANS (3) | ACVY (2), ANS (3) |
| Lip thickness | <12 mm: 12 | <12 mm: 4 |
| 12-15 mm: 10 | 12-15 mm: 3 | |
| ≥15 mm: 9 | ≥15 mm: 0 | |
| Mean preoperative ANB | −1.32° (SD, 4.42°) | −1.3° (SD, 5.09°) |
The completed sample results were tested for differences between sex and ethnicity with 2-sample t tests, and no statistically significant differences were found; hence, all results were pooled and analyzed together.
The sample size calculation before the study indicated that 24 subjects would provide 90% power to show a mean change in maxillary incisor exposure with orthognathic surgery involving a LeFort I osteotomy of 1 mm (SD, 1.5 mm), with an alpha level of 5%. No previous studies were found to have assessed the change in incisor exposure with orthognathic surgery; hence, it was not possible to base the sample size calculation on means and standard deviations of previous research. Based on this, 41 patients were recruited to allow for dropouts.
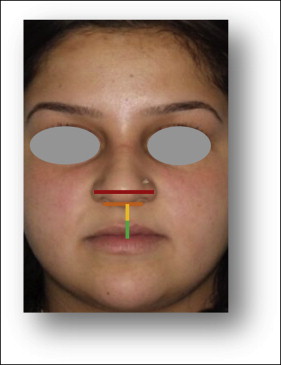
Clinical measurements were taken with sliding digital calipers (Silverline Tools, Yeovil, Somerset, United Kingdom) while the patients were seated upright looking at a distant point at eye level with the head unsupported, the lips at rest, and the teeth in light occlusion ( Fig 1 ). The calipers had a measurement range of 0 to 150 mm with graduations of 0.01 mm and an accuracy of ±0.03 mm. The same examiner (L.K.L.) took the measurements at 4 points: T1 (preoperatively within 1 month), T2 (1-2 weeks postoperatively), T3 (3 months postoperatively), and T4 (6 months postoperatively).
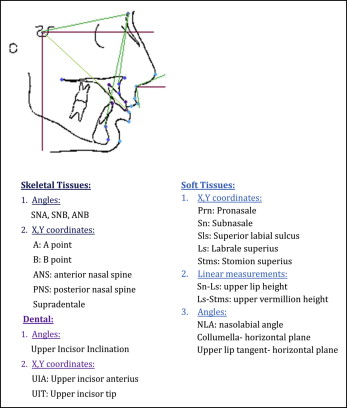
Lateral cephalometric radiographs were taken by the same radiographer in the same cephalostat (Planmeca XC; Planmeca, Helsinki, Finland) with standardized exposure factors (68-70 kV, 10 mA, 0.4 seconds), manual coning to reduce the radiation dose to the patient, and magnification fixed at 1.09. These were taken at time points as advised by the British Association of Oral and Maxillofacial Surgery Orthognathic Minimum Dataset : C1 (preoperatively within 1 month), C2 (within 1-2 weeks postoperatively once the wafer was removed), and C3 (5-6 months postoperatively if justifiable). These were taken in a standardized, reproducible manner by asking patients to look at a distant point at eye level to achieve natural head position while resting their lips and maintaining light occlusion. A plumb line was constructed using radiopaque string (soaked in barium sulphate) with a plumb weight (37.5 g) attached to the cephalostat. This produced a radiopaque “true” vertical reference line on the film ( Fig 2 ). The latter was used as the y-axis (passing through sella), and a perpendicular line to this through sella was used as the horizontal x-axis ( Fig 2 ). Subsequent tracings were superimposed on the sell-nasion line registered at sella, and the reference lines were transferred to ensure that these were the same. The cephalometric points were then measured and recorded as x- and y-coordinates on the preoperative and postoperative radiographs, and the changes in these were calculated. The same examiner (L.K.L.) traced all lateral cephalometric radiographs under the same conditions: in a darkened room without extraneous light. Only 10 radiographs were traced at a time to prevent fatigue. All clinical and radiographic results were transferred to an Excel spreadsheet (Microsoft, Redmond, Wash).
Intraexaminer clinical measurement repeatability was assessed by taking these measurements on 30 volunteers (16 female, 14 male) with a mean age of 30 years (range, 20-53 years) who were not participating in the main study and not undergoing any treatment that could affect the position or shape of the soft tissues or the maxillary incisors between the 3 time points; R1, R2 (on the same day 10 minutes apart), and R3 (2 weeks later). Most were of white origin (n = 29), and one was African Caribbean. The measurements were taken by 1 examiner (L.K.L.) with the same sliding digital vernier calipers used for the main study. The repeatability of the tracings and the radiographic measurements was tested by randomly selecting 10 lateral cephalometric radiographs from the participants in the study and tracing these twice 2 weeks apart, by the same examiner under the same conditions.
Statistical analysis
Stata software (version 10; StataCorp, College Station, Tex) was used to perform the statistical analysis. Intraclass correlation coefficients (ICCs) were used to assess intraexaminer repeatability. The means and standard deviations of the measurements and the changes between time points were calculated for the clinical and radiographic results. The statistical significance of the latter was tested with paired t tests. To explore the explanatory effect, if any, of the multiple variables (upper lip thickness, ANS recontouring, cinch sutures, and VY closures) on the results, multiple regression analysis was used. The results tested in this manner included (1) ratios of change in maxillary incisor exposure to maxillary incisor tip and A-point change in the horizontal and vertical planes; (2) clinical measurement changes between T1 and T4; (3) radiographic measurement changes between C1 and C3 in nasolabial angles, angles between the columella and upper lip tangents to the horizontal reference line and upper lip thickness; and (4) soft to hard tissue horizontal and vertical ratios as calculated for the pooled data before.
Results
There was excellent agreement for all values when the clinical measurements were retaken 10 minutes apart (mean ICC, 0.97; SD, 0.02; range, 0.93-0.99) and 2 weeks apart (mean, 0.96; SD, 0.02; range, 0.91-0.98). Similarly, the repeatability for the radiographic measurements showed excellent agreement (mean ICC, 0.97; SD, 0.07; range, 0.64-1.00) for all values except for 2 points, which showed moderate correlations: the maxillary incisor root point in the vertical plane (0.64) and upper lip height (0.78).
The radiographic measurement results showed that the hard tissue maxillary landmarks A-point and maxillary incisor tip moved anteriorly by averages of 3.34 mm (SD, 2.81 mm) and 3.39 mm (SD, 2.81 mm), respectively. The corresponding soft tissue landmarks (pronasale, subnasale, superior labial sulcus, and labrale superius) showed gradual increases in response from a minimum of 0.82 mm at pronasale to 3.02 mm at labrale superius ( Table II ). This trend was also reflected in the soft to hard tissue ratios of these points ( Table III ).
| Landmark | Horizontal | Vertical | ||
|---|---|---|---|---|
| Mean | SD | Mean | SD | |
| Hard tissue (mm) | ||||
| A | 3.34 ‡ | 2.81 | −1.81 † | 3.40 |
| ANS | 2.22 † | 3.61 | −0.84 | 2.19 |
| PNS | 4.56 ‡ | 4.10 | −2.48 ‡ | 2.15 |
| UIT | 3.39 ‡ | 2.81 | −1.37 ∗ | 2.99 |
| B | −1.84 † | 5.61 | −3.03 | 4.08 |
| Soft tissue (mm) | ||||
| Prn | 0.82 | 2.66 | −1.06 ∗ | 2.56 |
| Sn | 1.78 ‡ | 1.94 | −1.01 † | 1.75 |
| Sls | 3.38 ‡ | 2.36 | −0.35 | 2.56 |
| Ls | 3.02 ‡ | 2.28 | −0.56 | 2.21 |
| Stms | 2.22 ‡ | 2.33 | −0.14 | 2.86 |
| Upper lip thickness (at Ls) | −0.05 | 2.77 | ||
| Sn-Ls | 0.67 | 2.01 | ||
| Ls-Stms | 0.94 † | 1.27 | ||
| Angular measurements (°) | ||||
| ANB | 3.9 ‡ | 3.25 | ||
| Maxillary incisor inclination to sella-nasion | −0.62 | 4.80 | ||
| Soft tissue (S) | Hard tissue (H) | S:H ratio | Pearson correlation coefficient (r) | R 2 |
|---|---|---|---|---|
| Horizontal | ||||
| Prn | A | 0.32 | 0.23 | 0.05 |
| Sn | A | 0.70 | 0.35 | 0.12 |
| Sls | A | 0.83 | 0.40 ∗ | 0.16 |
| Ls | UIT | 2.16 | 0.66 † | 0.44 |
| Stms | UIT | 1.14 | 0.72 † | 0.52 |
| Vertical | ||||
| Prn | A | 0.14 | 0.20 | 0.04 |
| Sn | A | 0.18 | 0.49 ∗ | 0.24 |
| Sls | A | −0.24 | 0.40 ∗ | 0.16 |
| Ls | UIT | 0.48 | 0.70 † | 0.49 |
| Stms | UIT | −0.09 | 0.68 † | 0.46 |
A slight average posterior differential impaction occurred as reflected by the average change at postnasal spine of −2.48 mm compared with that at A-point of −1.81 mm. The corresponding labial soft tissue landmarks followed more closely the vertical changes at pronasale and subnasale with −1-mm changes, and lesser rates at superior labial sulcus (−0.35 mm), labrale superius (−0.56 mm), and stomion superius (−0.14 mm). A mean increase in upper vermilion height was noted radiographically between C1 and C3 of 0.94 mm (SD, 1.3 mm; P = 0.001). This was also reflected in the clinical measurements between T1 and T4 of 0.87 mm (SD, 0.90 mm; P <0.001).
The upper lip soft tissue demonstrated similar correlations in the vertical and horizontal planes relative to maxillary incisor movement ( Table III ). Maxillary incisor tip change accounted for 52% and 46% of the horizontal and vertical changes at stomion superius, respectively.
The nasolabial angle increased by a mean of 1.88°, primarily due to the increased angle between the columella and the horizontal reference line: ie, upturning of the columella ( Fig 2 ). The latter increased by a mean of 5.68° (SD, 6.2°; P <0.001), whereas the angle made by the tangent to the upper lip-horizontal reference line decreased by a mean of −3.2° (SD, 6.5°; P <0.05). The increase in the nasolabial angle was moderately correlated to the maxillary advancement at A-point (r = 0.45; P <0.01). The angle between the upper lip tangent-horizontal reference line decreased by 1.45° (SD, 5.1°) for a 1-mm maxillary incisor tip advancement (r = −0.54; P <0.01). The angle made by the columella-horizontal reference line increased by 2.74° (SD, 11.6°) for a 1-mm advancement of the maxillary incisor (r = 0.42; P <0.05).
The clinical measurements showed highly statistically significant mean increases in both interalar (2.62; SD, 1.4 mm) and alar (3.09 mm; SD, 3.5 mm) base widths, albeit with large variation in the pooled sample ( Table IV ). The mean changes between the third and sixth months postoperatively on all clinical measurements undertaken were not statistically significant.
| Measurement | Mean change T1−T4 | SD | Mean change T3−T4 | SD |
|---|---|---|---|---|
| Interalar width | 2.62 † | 1.41 | −0.32 | 1.06 |
| Alar base width | 3.09 † | 3.49 | −0.20 | 0.85 |
| Upper cutaneous lip height (Sn-Ls) | 0.68 † | 0.94 | 0.22 | 0.49 |
| Upper vermilion height (Ls-Stms) | 0.87 † | 0.90 | 0.01 | 0.38 |
| Maxillary incisor display: rest | 0.46 | 1.55 | −0.19 | 0.67 |
| Maxillary incisor display: posed smile | 1.03 ∗ | 1.71 | 0.44 | 1.11 |
| Maxillary incisor display: spontaneous smile | 0.18 | 1.71 | 0.05 | 0.94 |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


