Distraction osteogenesis is a relatively new surgical technique based on the principle of “tension stress” that allows lengthening of bone and surrounding soft tissues through progressively controlled fracture separation by means of a distraction device.
The first attempt at lengthening a femoral fracture was performed by Alessandro in Bologna, Italy, but it was not until the 1950s that Gavril Ilizarov from Kurgan, Russia, popularized the method to widen or lengthen limbs. Various publications of animal and clinical trials to increase the size and width of the facial bones can be found in the literature; however, the nineties offered a new stage for the growth and development of distraction osteogenesis in the craniofacial skeleton. After our publications in 1990 and 1992 on mandibular widening, on craniofacial microsomia, and later Ortiz-Monasterio and Molina on treatment of the mid-face, this new technology has improved and been widely popularized as a result of better instrumentation, miniaturized distraction appliances, multi-vectorial devices, and use of the intraoral, transconjunctival, and coronal approaches to avoid facial scars. Nevertheless, success in surgery and postoperative follow-up is based on sound biologic and biomechanical principles.
Biologic Principles of Distraction Osteogenesis
Protocol for Distraction
Distraction osteogenesis is indicated for patients with deficiencies or bone discontinuity who have adequate blood supply, sufficient quantity and quality of bone, and ideal surrounding tissues; such patients need to be reliable and intelligent to understand and follow the postoperative instructions.
Osteotomy
The incision and reflection of soft tissues to perform the surgery must be as limited as possible so that the blood supply is not diminished, which is mainly responsible for healing and mineralization. The bone cuts are performed under abundant irrigation, ideally with lactated Ringer solution, and every effort is made to avoid overheating of bone and damage to soft tissues. Once the bone is fractured, the soft tissues are carefully and meticulously closed in layers. The presence of the distraction device under the periosteum would limit bone healing, contract the distraction chamber, and permit saliva and contamination into the distraction area. Ideally, the distraction device should be placed away from the osteotomy site.
Latency Period
After the osteotomy is performed and the soft tissues closed carefully, the distraction device must be activated to open the bone gap 1 or 2 mm. This space will fill with blood, which consolidates, and collagen fibers will advance to bridge the gap; between 6 and 7 days is needed for completion of this process. In addition, undifferentiated cells and morphogenetic proteins accumulate on the sides of the fracture. This interval, during which there is no activation of distraction and the patient is maintained on a liquid diet, is called the latency period.
Activation Period
After 7 days of resting while the collagen fibers develop, activation of the appliance is initiated at a rate of 1 mm/day in one treatment or divided into two or three sessions per day or at a rate of 0.5 mm/day for very small bone fragments, such as for alveolar distraction or patients with compromised blood supply. This is called the rhythm and rate of distraction (i.e., the amount of activation and how often). The collagen fibers are stretched slowly and progressively until the desired movement has been accomplished. The space created within the fractured bony parts is called the distraction chamber, and the chamber box has six walls, two limited by bone and four limited by periosteum. The entire chamber is filled with collagen fibers, and nutrients for mineralization are obtained from neighboring tissues. The patient is maintained on a liquid diet until the end of the activation period, at which time acrylic is applied to the distractor to make it rigid, and the diet is advanced to soft foods.
Consolidation
The time between the end of the activation period and complete bone mineralization of the chamber is the consolidation period. Obviously, many variables are involved in this critical period: the quality and quantity of the original bone, the amount of movement, the age of the patient, the rigidity of the appliance, and the surgical site. The new instrumentation and miniaturized distractors allow the surgical devices to be kept in place for much longer periods, which permits mineralization to become advanced before considering removal of the appliance. The basic rule is to remove the distractors once adequate radiopacity is observed on radiographs. Because extraoral appliances were used in the initial period of distraction osteogenesis, there was a tendency to remove the appliances before proper mineralization to avoid the psychological impact and reduce scar formation around the surgical facial pins; major relapse and the need for secondary surgeries were common. Other surgeons suggested that the bone fragments be rigidly fixated once distraction was accomplished, and thus two major surgical interventions were needed.
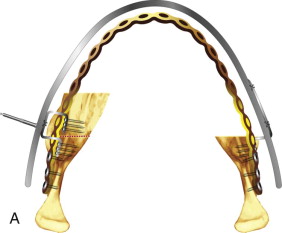
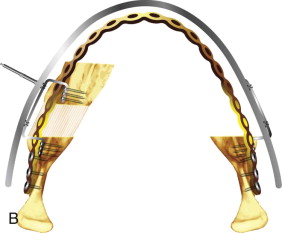
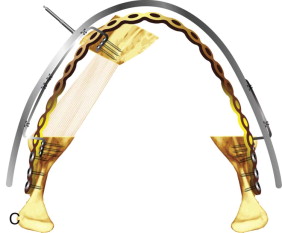
Intraoral, transconjunctival, and coronal approaches permit surgeons to perform distraction osteogenesis without facial scars and, by using the new miniaturized distraction devices, allow prolongation of the consolidation period without considering removal of the appliances. Once activation is completed, mineralization starts at the two bony walls, with major contributions from the periosteum. Deposition of minerals begin at either end of the chamber ( Fig. 11-1, A ) and advances into the mid-chamber, with a fibrous island called the fibrous interzone ( Fig. 11-1, B ) left in the middle. The fibrous interzone reduces slowly and progressively until complete disappearance, after which the consolidation period is completed and the patient is advised to have the distractors removed.


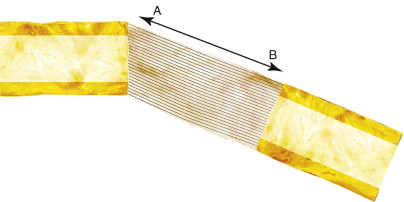
This healing process of mineralization and bone maturation starts after activation is completed, and depending on certain variables, especially the amount of movement and the age of the patient, 2 to 24 months is needed. Creation of a curve or molding of the regenerate bone is not possible because according to the biomechanical concept of lengthening the bone from point A to point B, there is no other bone shape possible but a straight line between the two separated points ( Fig. 11-2 ). In addition, the more extensive the bone movement, the narrower the mid-chamber because the periosteal layer contracts as the distraction device is activated further; this phenomenon is called the “hourglass deformity” ( Fig. 11-3 ) and is particularly important since this is the weakest point in the bone and the place where post-treatment fractures occur.

Remodeling Period
Once the distractors are removed, patients progress to normal living and daily activities, the healed bone undergoes regular tension from the muscles and normal biting forces, and the soft tissues surrounding the bones exert regular tension over the tissues; this process will transform the bone and allow definitive healing and final reshaping.
The healing process of distraction osteogenesis is variable and depends on the tissues involved in maxillary or mandibular lengthening.
Biology
Bone Lengthening
Once the osteotomy has been performed and the latency and activation periods completed, the distraction chamber, filled with collagen fibers, will undergo cell differentiation. Mesenchymal cells situated in the periphery of the osteotomy gap will invade the chamber and turn into osteoblasts, chondroblasts, or fibroblasts, depending on the magnitude of strain, rigidity of the callus, and movement ( Fig. 11-4 ). Different histologic patterns can be observed in the various stages of bone healing ( Figs. 11-5 and 11-6 ).

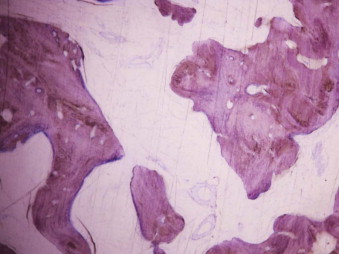
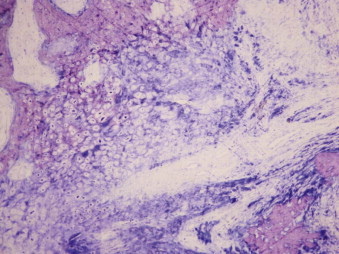
The histologic pattern within the distraction chamber is uniform, and bone differentiation and metabolism depend on mechanical loading. Bone healing is achieved by maturation of the collagen template and deposition of osteoid by osteoblast proliferation, and levels of osteocalcin and osteonectin are increased as woven and lamellar bone develops. Even though both the endosteum (both bony walls) and periosteum make contributions to osteoid deposition, the periosteum is more important and justifies a non-invasive surgical technique to keep the periosteal layer intact ( Fig. 11-7 ).

The new tissue forms in a direction parallel to the vector of traction, spindle-shaped fibroblasts appear in the distraction gap, the peripheral vascular supply extends into the chamber and starts the process of mineralization, and osteoblasts proliferate within the collagen matrix and initiate osteoid deposition with the creation of bone spicules. In addition, chondroblasts start depositing chondroid, but to a minor degree, depending on the rigidity and stability of the distraction frame; if excess movement is present, more fibrous tissue and cartilage production will be seen. These islands of cartilage will become encased in the bone matrix and are of no clinical significance unless they are abundant. Mineralization occurs from either end of the bony walls and from the periosteal layer in the periphery and finally bridges the center to eliminate the fibrous interzone, the last area to consolidate. Haversian remodeling is the final stage of cortical healing and results in maturity and mechanical stability ( Fig. 11-8 ).
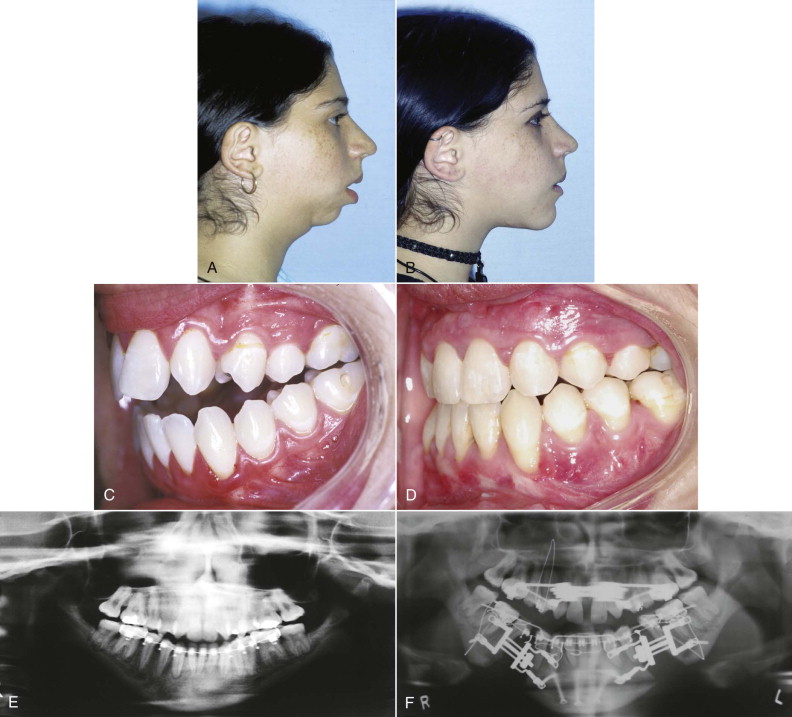
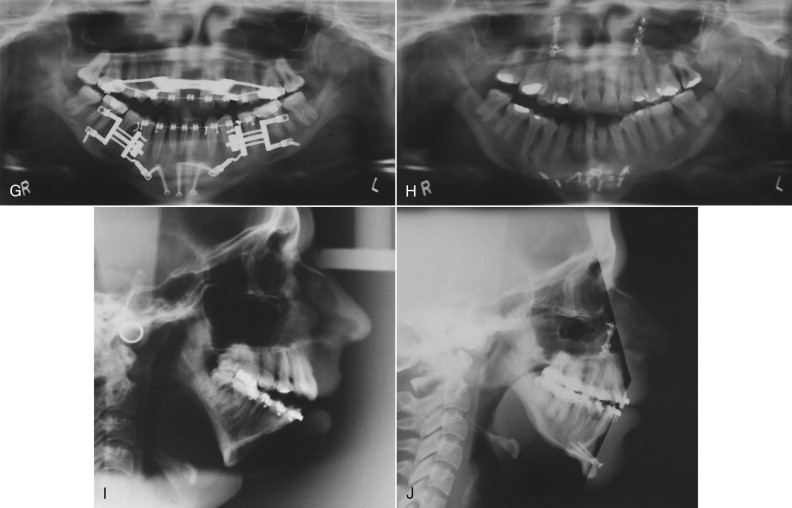
Muscle Lengthening
Most surgeons consider distraction osteogenesis as merely bone lengthening and think that the surrounding tissues should “just” accommodate; however, there are important issues regarding function and relapse that are related to the fact that as muscles lengthen, different healing processes become relevant to the health and position of the bone.
The distraction movement will lengthen striated muscle, and the adaptation is usually well tolerated when the direction is parallel to the distraction. The areas M and Z ( Fig. 11-9, A ) are stretched initially, and this will create pressure at the origin and insertion of the muscle and stimulate the creation of new sarcomeres at either end of the myotendinous junction, or new ones could be created within the muscle mass, called intercalary new sarcomeres. As distraction activation continues, the inner pressure of the muscle increases and induces fibers to rupture ( Fig. 11-9, B and C ); these fibers may heal by muscle regeneration or by sclerosis and fibrosis ( Fig. 11-9, D ). Staged activations decrease muscle damage since DNA synthesis is higher with multiple small activations, such as four 0.25-mm activations in 24 hours.




After lengthening, mandibular hypomobility develops in some patients secondary to muscle edema and spasm, as well as muscle widening when forces are applied in a plane perpendicular to the insertion of the muscle. Active physiotherapy is mandatory for all patients to achieve the goals of mouth opening and mandibular translation in the early postoperative phase. In any event, there will be situations in which distraction osteogenesis should be performed in different surgical stages to avoid the functional complications and relapse associated with large movements; for any lengthening of more than 25% of the original bone size, several stages should be considered. It is also important to measure the different muscles involved in a predetermined direction. For example, a 20-mm mandibular anteroposterior advancement in the mandibular angle in a 80-mm-long mandible corresponds to bone lengthening of 20%, but the geniohyoid muscle undergoes 35% lengthening and the masseter muscle is widened 40%; both muscles will be very susceptible to contraction, relapse, and diminished functionally postoperatively, and hypomobility usually occurs.
The muscles will increase in length via different mechanisms: increasing numbers of sarcomeres either at the insertion and origin or within the muscle mass. If tolerance is exceeded, fibrous tissue invades the ruptured areas and produces fibrosis and mandibular hypomobility. The ideal rhythm and rate need to be followed and the limit of 25% of the original muscle length not be surpassed.
Nerve Lengthening
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


