Furlow palatoplasty
Introduction
The Furlow double-opposing palatoplasty (FDOP) was first introduced by Leonard Furlow in 1978 and published formally in 1986 by the Children’s Hospital of Pennsylvania cleft unit . It has gained acceptance by many surgeons as the preferred technique for cleft palate repair. Although conceptually and procedurally a challenge, the FDOP has the distinct advantage of lengthening the soft palate and restoring normal velar anatomy and function. Since its introduction, the FDOP has undergone several modifications, much like other named cleft lip and palate techniques.
The essential components of the FDOP include oral- and nasal-based mucosal and muscle flaps that are designed as Z-plasty flaps on one side and then reversed in configuration on the underlying side. As is commonly understood in reconstruction, a Z-plasty allows lengthening of a tissue limb and resists tension when interdigitated with a corresponding Z-plasty flap. Two Z-plasties allow transposition of the flaps in such a manner that an incision line does not lie on another during closure, resulting in a reconstructed soft palate that is resistant to dehiscence and breakdown of flaps, a particular problem in wider clefts.
Technique
Cleft palate anatomy must first be understood and appreciated before any palatoplasty. The primary objective of palatoplasty is to dissect and mobilize palatal musculature appropriately, specifically the tensor-levator aponeurosis, and to reposition the muscles correctly, such that function is optimally restored to the velar mechanism. Also, it is important to minimize wounding to the hard palate during palatoplasty to reduce scarring and subsequent growth perturbations of the maxilla. This is primarily achieved through reducing the amount of denuded hard palate during initial palatoplasty, which will be discussed later.
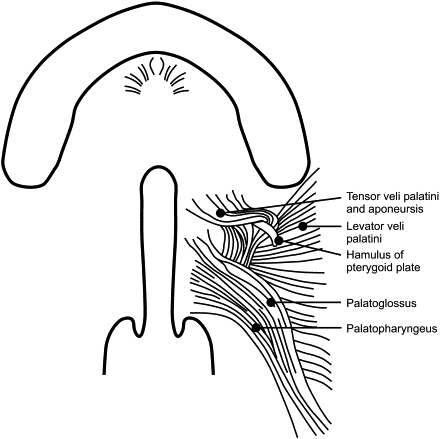
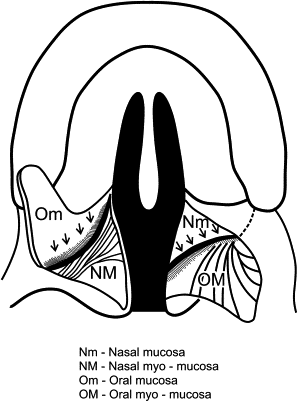
Fig. 1 schematically illustrates the abnormal muscular insertions in the cleft palate condition. The tensor-levator aponeurosis is a confluence of these two principal muscles of the soft palate (the palatal component of the velar mechanism). Note that the muscles are disinserted into the hard palatal margins and the levator is positioned more laterally. Careful dissection of the muscular aponeurosis is paramount in being able to reposition the tensor component (and, to a lesser degree, the levator insertion) across the midline successfully, assuming the correct anatomic position. The FDOP is designed to accomplish this procedural objective.
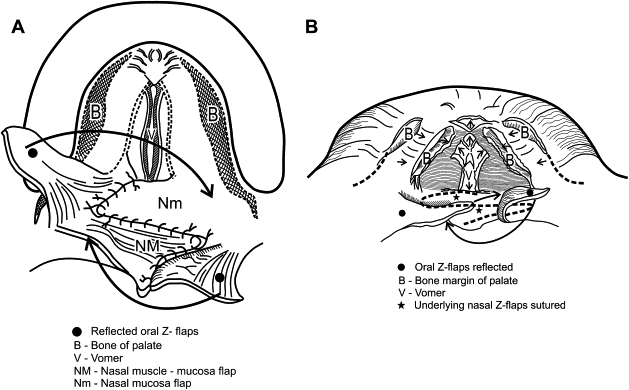
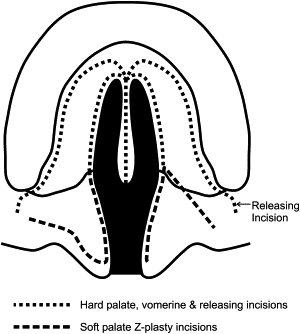
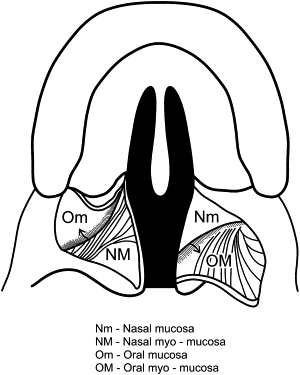
Design of the initial Z-plasties is shown in Fig. 2 . The oral layer is first approached with inscribed Z-incisions incorporating angles of around 60° to 70°. The angles differ according to soft tissue bulk and cleft width. The wider the cleft defect, the less soft tissue there is available, and, generally, the more obtuse the angles must be to achieve dissection and mobilization of the flaps. As the flaps are raised, great care must be taken to keep one oral layer purely mucosal (the author prefers this to be the right side for ease of dissection) and the opposite oral layer a mucosal-muscle flap ( Fig. 3 ). Dissection of the latter flap is signaled by the appearance of muscle, obviously, in this flap. The underlying nasal mucosa also appears “bluish” because it is thin; care must be exercised in this dissection plane not to tear or shred the underlying nasal layer inadvertently. To mobilize the oral flaps further, lateral extension into the space of Ernst (a potential small anatomic space deep and posterior to the hamulus and tensor sling) is often necessary. This is easily achieved by blunt dissection with a small peanut. When adequate lateral dissection is achieved, the uvular portion is divided or simply opened with small opening “snips” from curved tenotomy scissors. The oral flaps are then tagged and retracted laterally to reveal the underlying nasal layer, one side (in the author’s case, the patient’s right side) of which still incorporates the muscular component of the tensor-levator aponeurosis. The Z-flaps are then incised in a reversed configuration from that of the oral flaps, as shown in Fig. 4 . The angled limb of the flap on the patient’s right side, the nasal myomucosal flap, must initially include the tissue inserted at the hard palatal margin to incorporate the attending muscle. After several millimeters, the Z-plasty limb can then be extended with a scissors at an angle of 60° to 70°. The nasal flaps often need to be dissected quite far laterally onto the palatopharyngeal surface to gain adequate mobilization of tissue.
Once the flaps have been adequately mobilized, closure may commence. After ensuring good hemostasis, particularly laterally, where most of the dissection has taken place, the nasal flaps are transposed in a typical Z-plasty manner. The patient’s left-sided nasal flap, composed of mucosa only, is transposed anteromedially to dock at the opposite junction of hard palate and margin of mucosa. A single horizontal mattress suture (the author prefers 3-4 or 4-0 polyglycolic acid suture) is placed at the far corner, the leading edge of the flap, and is sutured to the palatal shelf mucosa ( Fig. 5 A ). The opposite nasal flap of mucosa and muscle is similarly transposed, posterolaterally in this case, and is docked alongside the anterior Z-flap, with the far corner sutured into the lateral recess in the palatopharyngeal tissue, again with a horizontal mattress suture. This places the right-sided musculature into a more horizontally and anatomically correct position (see Fig. 5 B). Closure of the nasal side is commenced along the flap margins with 4-0 or 5-0 polyglycolic acid suture in an interrupted or continuous fashion.