To provide the ultimate in surgical care, the surgeon must be intricately intoned with the complex risks wrought by anesthesia and surgery in concurrence with the patients preexisting medical conditions. It is the surgeon’s responsibility to investigate each patient’s unique risk factors and assemble the appropriate plan to maximize surgical outcome.
Oral and maxillofacial surgeons have the unique privilege of providing an array of various anesthetic methods. As such we must be dually prepared to identify and deal with the risks associated with performing the surgery and anesthesia in concert. Therefore given this task, one must be keenly aware of the tools available to fully evaluate the patient before a surgical procedure. Complete and detailed history and physical examination, previous anesthetic and surgical history, appropriate family and social history, laboratory and radiographic tests, proper involvement of a specialist, prophylactic measures, and behavioral modification each provide an invaluable method to prepare the patient for successful surgery. In combination with complete mastery of the anesthesia and surgical techniques, the practitioner is well prepared to deliver a custom designed and well-planned surgical treatment.
The course of preoperative evaluation provides an opportunity for the practitioner to declare a genuine care and interest for the patient, which in turn allows for further global success and satisfaction. It allows for involvement of the patient and their support team, thus gaining tangible insight into the surgical procedure and obtaining realistic expectations. This can be invaluable for the patient because the amount of satisfaction with the surgical treatment is maximized when the patient’s expectations are close to reality.
A complete immersion into the preoperative evaluation process is conducted in this chapter to provide the reader with a clear understanding of current methods and the reason for their use.
▪
HISTORY AND PHYSICAL EXAMINATION
A complete history and physical examination is an integral part of the preoperative evaluation. It is the practitioner’s first opportunity to identify any abnormalities or dysfunctions that could require further evaluation or planning before the operative procedure. To streamline this process and allow the patient adequate anonymity to disclose important health information that one can then further explore, a health questionnaire is valuable. This form and also any history and physical examinations performed by other admitting house staff, should not in any way become the preoperative history and physical examination required. The form should only be used as an aid to identify the most critical risk factors and guide one to further scrutinize them. For example, if the form identifies a patient as an asthmatic, one needs to further understand the extent of this dysfunction by conducting a detailed interview with the patient regarding their disease. (When was the diagnosis made? How often do the attacks occur and under what circumstances? How do they control their asthma? How often are medication(s) used? How often do they visit the emergency department for their asthma?, etc.)
A patient’s medication(s) can have a large effect on anesthesia and surgical planning. The general rule is to continue most medications as prior; however, there are unique situations that require altered dosing, change to shorter acting preparations, and even discontinuing the medication temporarily ( Table 1-1 ). Furthermore, the patient’s current medication(s) can require the modification of postoperative medications used for the treatment of pain, swelling, infection, and so forth.
| Medications | Anesthetic Implications | Recommended Management |
|---|---|---|
| Aminoglycosides | Can potentiate nondepolarizing relaxants | Monitor neuromuscular relaxants carefully |
| Aspirin | Platelet dysfunction, bleeding potential | Consider preoperative discontinuation for at least 10-14 days; discuss with prescribing physician regarding risk of stroke, myocardial infarction (MI), or thrombosis with discontinuation |
| Clonidine | Acute withdrawal can cause hypertensive crisis; decrease anesthetic requirements | Continue therapy the day of surgery; can use dermal delivery perioperatively; decrease anesthetic requirements intraoperatively |
| Insulin | Hypoglycemia if not monitored | Depends on time of surgery and serum glucose range; recommend to continue partial dose (one-half or one-third) of long-acting insulin and delete short-acting insulin the day of surgery; monitor serum glucose closely perioperatively; watch for combined long- and short- acting preparations |
| Lithium | Potentiate neuromuscular blockers, induce hypothyroidism in some patients; lithium concentrations increase with decreased serum sodium | Monitor neuromuscular blockade carefully; obtain thyroid function tests preoperatively if indicated; monitor serum sodium and avoid sodium wasting diuretics |
| Monoamine oxidase inhibitors (isocarboxazid, pargyline, phenelzine, tranylcypromine) | Increased catecholamine stores; hepatotoxicity; rare but potentially fatal reactions with opioids, especially meperidine | Avoid indirect-acting sympathomimetics and use reduced doses of direct-acting agents; serum liver function tests if not done; avoid opioids, especially meperidine; for elective surgery, request psychiatrist to discontinue for 14-21 days unless suicide risk; less time needed for pargyline and tranylcypromine because reversibly |
| Warfarin | Excessive intraoperative bleeding | Manage with prescribing physician; withdrawal in advance; substitute with heparin; heparin may be stopped immediately preoperatively and restarted postoperatively |
Allergies and reactions to medication(s) are important to identify. It is of further importance to explore the circumstances and extent of such reaction (from a mild rash to an anaphylactic reaction). The offending drugs are obviously avoided, unless formal immunologic treatment has been performed or pretreatment with antihistamines or steroids is conducted.
A complete list of previous surgical procedures along with the mode of anesthesia used should be obtained. Moreover, detailed exploration of each surgical and anesthesia experience to identify any complications, effective pain control, and patient’s social and emotional experience is invaluable. The anesthetic plan can be fine-tuned based on such previous experience. For example, ease or difficulty of airway intubation, reaction to anesthetic(s) used, and other detailed history are vastly important to reduce anesthetic risks. Past surgical dictations pertinent to the surgical procedure planned should also be obtained and reviewed to gain insight into pitfalls and success of previous techniques.
Identifying a family history of malignant hyperthermia, pseudocholinesterase abnormalities, or glucose-6-phosphate dehydrogenase (G6PD) deficiency can be lifesaving for the patient. History of smoking, drug use, and alcohol abuse should be further explored with detailed cardiovascular, pulmonary, and hepatic evaluation. Women of child-bearing age should be questioned in regards to the possibility of being pregnant, and if any doubt proper testing should be conducted.
The physical exam should both be global and targeted. An organized evaluation including vital signs, height, weight, airway evaluation, head and neck, cardiac, pulmonary, gastrointestinal (GI), renal, neurologic, musculoskeletal, and other physical markers pertinent to the history is essential. A more scrupulous examination of the surgical site is immensely valuable, to identify possible complicating factors and plan for them.
With the above complete, the practitioner can further submerge into the specific review of systems to uncover any dysfunctions that would require possible laboratory or radiographic testing along with proper specialist consultation. Once all the above information has been amassed, the practitioner can use a risk stratification scheme to more globally expose the level of risk and allow for better communication of such risks amongst the medical staff. The American Society of Anesthesiologists Physical Status Classification System (ASA) has provided a simple and effective means of communicating the severity of patient’s illness since 1940. However, there has been no proven direct correlation between the ASA classification and surgical and anesthesia risk. Therefore certain modifications have been implemented to safeguard the simplicity of this design and yet add more true risk stratification. Such modifications have been put forth by Natalie F. Holt et al at the Yale University Department of Anesthesiology that take into account the physical status modified for individual system, surgical invasiveness and risk, anesthetic risk and complexity, and other special “risk indicators.” This information is then communicated in a simple integrated system to facilitate categorization and communication of large amounts of information, highlight potentially high-risk situations, guide perioperative planning, and provide a means by which to analyze outcomes.
▪
SYSTEM APPROACH TO PREOPERATIVE SURGERY
CARDIOVASCULAR
It is widespread knowledge that cardiovascular disease is extremely common in the industrialized world. As such, cardiovascular complications are the most common cause of perioperative mortality. Of the 27 million patients undergoing surgery in the United States every year, 8 million have significant coronary artery disease or other cardiac comorbidities. One million of these patients will go on to have perioperative cardiac complications with substantial morbidity, mortality, and cost. Given these facts, meticulous assessment of the cardiovascular system is intensely important in determining a patient’s surgical candidacy, preoperative planning, and anesthesia planning.
As mentioned earlier, one of the early risk stratification methods was the ASA classification, which lacked accuracy in predicting risk and was not easily reproducible among physicians. Recent methods rely more on easily defined and measured parameters and were enhanced by multivariate statistical methodology. An exemplary example is the Goldman’s criteria, which is reliant on multivariate analysis and assigns points to easily reproducible characteristics. Once tallied the point total correlates well with the cardiac risk ( Table 1-2 ).
| Criteria | Points |
|---|---|
| HISTORY | |
| Age >70 yr | 5 |
| Myocardial infarction <6 mo | 10 |
| PHYSICAL EXAMINATION | |
| S 3 gallop or jugular venous distention | 11 |
| Aortic valvular stenosis | 3 |
| ELECTROCARDIOGRAM (ECG) | |
| Rhythm other than sinus or premature atrial | 7 |
| contraction | |
| >5 Premature ventricular contractions/min | 7 |
| GENERAL STATUS | |
| PO 2 <60 or PCO 2 >50 | 3 |
| K <3.0 or HCO 3 <20 mEq/L | 3 |
| BUN >50 or creatinine >3.0 mg/dL | 3 |
| Abnormal SGOT or chronic liver disease | 3 |
| Bedridden | 3 |
| OPERATION | |
| Intraperitoneal, intrathoracic, or aortic operation | 3 |
| Emergency operation | 4 |
| TOTAL | Possible 53 points |
| Class I | (0 to 5 points) | has a 0.9% risk of serious cardiac event or death |
| Class II | (6 to 12 points) | has a 7.1% risk |
| Class III | (13 to 25 points) | has a 16.0% risk |
| Class IV | (greater than 26 points) | has a 63.6% risk |
A major advancement in the above method of risk stratification is the inclusion of the patient’s functional capacity, clinical signs and symptoms, and operative risk assessment to estimate overall risk and plan preoperative intervention.
The American College of Cardiology and the American Heart Association (ACC/AHA) guidelines first introduced in 1996, and then updated in 2002 and 2006, further enhance the assessment and cardiac risk evaluation of patients under-going noncardiac surgery. The ACC/AHA guidelines further take into account patients’ functional capacity and surgery types to determine risk and then counsel properly based on an easy-to-follow flowchart ( Figure 1-1 ).
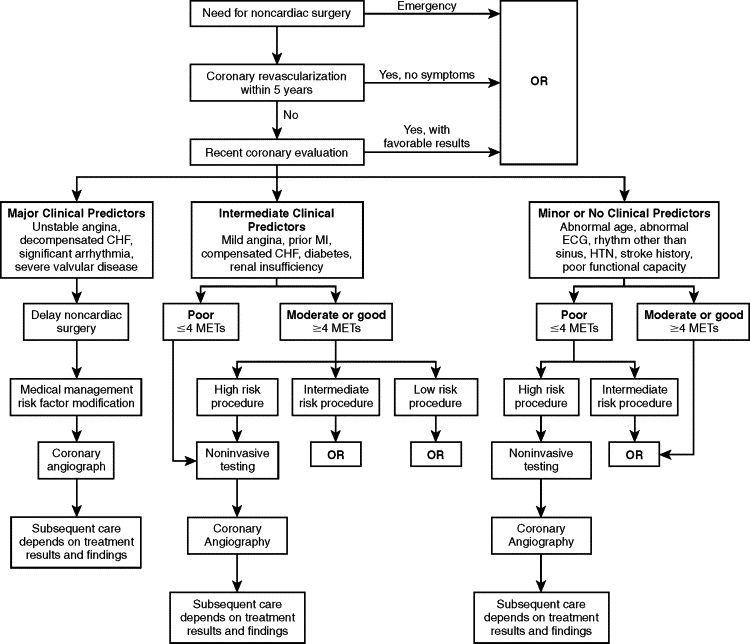
Once the risk assessment process is complete, the practitioners, along with consultants (if appropriate), need to consider perioperative interventions, which can include coronary revascularization (bypass, percutaneous transluminal coronary angioplasty), modification of anesthetic technique, and use of invasive monitoring.
Current general recommendations regarding the optimal timing of elective surgery after a myocardial infarction (MI) is 4 to 6 weeks. This is mildly different than the 3-month delay previously recommended through the evidence presented by Tarhan et al and Steen et al. Today this decision is based on assessment of ischemic risk either by clinical or noninvasive studies. The infarction event is considered a major clinical predictor in the context of ongoing ischemic risk.
Recent ACC/AHA update (2006) focuses on the perioperative use of beta-blockers to reduce cardiovascular morbidity and mortality in the noncardiac surgery patient. The perioperative risk of cardiovascular morbidity and mortality was decreased by 67% and 55%, respectively, in patients receiving beta-blockade in the perioperative period versus those receiving placebo. The general philosophy behind beta-blockade and aspirin use perioperatively is to reduce the effects of adrenergic surge and halt platelet activation and microvascular thrombosis. The specific perioperative beta-blocker recommendations for each patient class (based on size of treatment effect and estimate of certainty of treatment effect) are well illustrated in the 2006 update and are beyond the scope of this chapter.
Prevention of endocarditis through appropriate prophylactic measures is a vital part of the preoperative evaluation of a cardiac patient. The American Heart Association recommendations have been illustrated in Tables 1-3, 1-4, and 1-5 .
|
* Except for the conditions listed above, antibiotic prophylaxis is no longer recommended for any other form of CHD.
† Prophylaxis is recommended because endothelialization of prosthetic material occurs within 6 mo after the procedure.
| All dental procedures that involve manipulation of gingival tissue or the periapical region of teeth or perforation of the oral mucosa * |
* The following procedures and events do not need prophylaxis: routine anesthetic injections through noninfected tissue, taking dental radiographs, placement of removable prosthodontic or orthodontic appliances, adjustment of orthodontic appliances, placement of orthodontic brackets, shedding of deciduous teeth, and bleeding from trauma to the lips or oral mucosa.
| Regimen: Single Dose 30 to 60 Min before Procedure | |||
|---|---|---|---|
| Situation | Agent | Adults | Children |
| Oral | Amoxicillin | 2 g | 50 mg/kg |
| Unable to take oral medication | Ampicillin | 2 g IM or IV | 50 mg/kg IM or IV |
| OR | |||
| Cefazolin or ceftriaxone | 1 g IM or IV | 50 mg/kg IM or IV | |
| Allergic to penicillins or ampicillin—oral | Cephalexin * † | 2 g | 50 mg/kg |
| OR | |||
| Clindamycin | 600 mg | 20 mg/kg | |
| OR | |||
| Azithromycin or clarithromycin | 500 mg | 15 mg/kg | |
| Allergic to penicillins or ampicillin and unable | Cefazolin or ceftriaxone † | 1 g IM or IV | 50 mg/kg IM or IV |
| to take oral medication | OR | ||
| Clindamycin | 600 mg IM or IV | 20 mg/kg IM or IV | |
* Or other first- or second-generation oral cephalosporin in equivalent adult or pediatric dosage.
† Cephalosporins should not be used in an individual with a history of anaphylaxis, angioedema, or urticaria with penicillins or ampicillin.
In summary, it is extremely important to have a consistent and reliable way to stratify cardiac risk in a noncardiac surgical patient. Furthermore the practitioner needs to be completely clear on the steps required for each patient to decrease cardiac risk and to safely plan a surgical and anesthetic treatment. Appropriate and clear communication with the anesthesia and cardiac specialists regarding the patient’s cardiovascular risk will also increase the patient’s confidence before an invasive procedure.
▪
SYSTEM APPROACH TO PREOPERATIVE SURGERY
CARDIOVASCULAR
It is widespread knowledge that cardiovascular disease is extremely common in the industrialized world. As such, cardiovascular complications are the most common cause of perioperative mortality. Of the 27 million patients undergoing surgery in the United States every year, 8 million have significant coronary artery disease or other cardiac comorbidities. One million of these patients will go on to have perioperative cardiac complications with substantial morbidity, mortality, and cost. Given these facts, meticulous assessment of the cardiovascular system is intensely important in determining a patient’s surgical candidacy, preoperative planning, and anesthesia planning.
As mentioned earlier, one of the early risk stratification methods was the ASA classification, which lacked accuracy in predicting risk and was not easily reproducible among physicians. Recent methods rely more on easily defined and measured parameters and were enhanced by multivariate statistical methodology. An exemplary example is the Goldman’s criteria, which is reliant on multivariate analysis and assigns points to easily reproducible characteristics. Once tallied the point total correlates well with the cardiac risk ( Table 1-2 ).
| Criteria | Points |
|---|---|
| HISTORY | |
| Age >70 yr | 5 |
| Myocardial infarction <6 mo | 10 |
| PHYSICAL EXAMINATION | |
| S 3 gallop or jugular venous distention | 11 |
| Aortic valvular stenosis | 3 |
| ELECTROCARDIOGRAM (ECG) | |
| Rhythm other than sinus or premature atrial | 7 |
| contraction | |
| >5 Premature ventricular contractions/min | 7 |
| GENERAL STATUS | |
| PO 2 <60 or PCO 2 >50 | 3 |
| K <3.0 or HCO 3 <20 mEq/L | 3 |
| BUN >50 or creatinine >3.0 mg/dL | 3 |
| Abnormal SGOT or chronic liver disease | 3 |
| Bedridden | 3 |
| OPERATION | |
| Intraperitoneal, intrathoracic, or aortic operation | 3 |
| Emergency operation | 4 |
| TOTAL | Possible 53 points |
| Class I | (0 to 5 points) | has a 0.9% risk of serious cardiac event or death |
| Class II | (6 to 12 points) | has a 7.1% risk |
| Class III | (13 to 25 points) | has a 16.0% risk |
| Class IV | (greater than 26 points) | has a 63.6% risk |
A major advancement in the above method of risk stratification is the inclusion of the patient’s functional capacity, clinical signs and symptoms, and operative risk assessment to estimate overall risk and plan preoperative intervention.
The American College of Cardiology and the American Heart Association (ACC/AHA) guidelines first introduced in 1996, and then updated in 2002 and 2006, further enhance the assessment and cardiac risk evaluation of patients under-going noncardiac surgery. The ACC/AHA guidelines further take into account patients’ functional capacity and surgery types to determine risk and then counsel properly based on an easy-to-follow flowchart ( Figure 1-1 ).
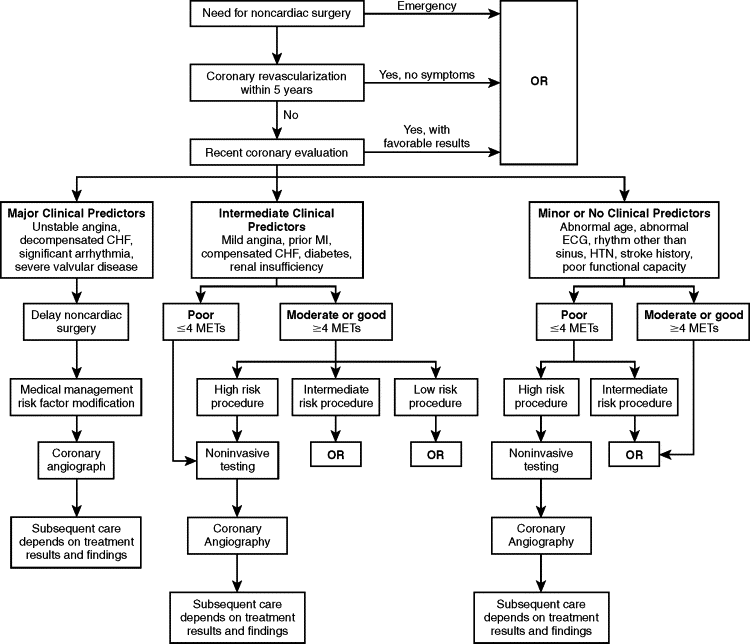
Once the risk assessment process is complete, the practitioners, along with consultants (if appropriate), need to consider perioperative interventions, which can include coronary revascularization (bypass, percutaneous transluminal coronary angioplasty), modification of anesthetic technique, and use of invasive monitoring.
Current general recommendations regarding the optimal timing of elective surgery after a myocardial infarction (MI) is 4 to 6 weeks. This is mildly different than the 3-month delay previously recommended through the evidence presented by Tarhan et al and Steen et al. Today this decision is based on assessment of ischemic risk either by clinical or noninvasive studies. The infarction event is considered a major clinical predictor in the context of ongoing ischemic risk.
Recent ACC/AHA update (2006) focuses on the perioperative use of beta-blockers to reduce cardiovascular morbidity and mortality in the noncardiac surgery patient. The perioperative risk of cardiovascular morbidity and mortality was decreased by 67% and 55%, respectively, in patients receiving beta-blockade in the perioperative period versus those receiving placebo. The general philosophy behind beta-blockade and aspirin use perioperatively is to reduce the effects of adrenergic surge and halt platelet activation and microvascular thrombosis. The specific perioperative beta-blocker recommendations for each patient class (based on size of treatment effect and estimate of certainty of treatment effect) are well illustrated in the 2006 update and are beyond the scope of this chapter.
Prevention of endocarditis through appropriate prophylactic measures is a vital part of the preoperative evaluation of a cardiac patient. The American Heart Association recommendations have been illustrated in Tables 1-3, 1-4, and 1-5 .
|
* Except for the conditions listed above, antibiotic prophylaxis is no longer recommended for any other form of CHD.
† Prophylaxis is recommended because endothelialization of prosthetic material occurs within 6 mo after the procedure.
| All dental procedures that involve manipulation of gingival tissue or the periapical region of teeth or perforation of the oral mucosa * |
* The following procedures and events do not need prophylaxis: routine anesthetic injections through noninfected tissue, taking dental radiographs, placement of removable prosthodontic or orthodontic appliances, adjustment of orthodontic appliances, placement of orthodontic brackets, shedding of deciduous teeth, and bleeding from trauma to the lips or oral mucosa.
| Regimen: Single Dose 30 to 60 Min before Procedure | |||
|---|---|---|---|
| Situation | Agent | Adults | Children |
| Oral | Amoxicillin | 2 g | 50 mg/kg |
| Unable to take oral medication | Ampicillin | 2 g IM or IV | 50 mg/kg IM or IV |
| OR | |||
| Cefazolin or ceftriaxone | 1 g IM or IV | 50 mg/kg IM or IV | |
| Allergic to penicillins or ampicillin—oral | Cephalexin * † | 2 g | 50 mg/kg |
| OR | |||
| Clindamycin | 600 mg | 20 mg/kg | |
| OR | |||
| Azithromycin or clarithromycin | 500 mg | 15 mg/kg | |
| Allergic to penicillins or ampicillin and unable | Cefazolin or ceftriaxone † | 1 g IM or IV | 50 mg/kg IM or IV |
| to take oral medication | OR | ||
| Clindamycin | 600 mg IM or IV | 20 mg/kg IM or IV | |
* Or other first- or second-generation oral cephalosporin in equivalent adult or pediatric dosage.
† Cephalosporins should not be used in an individual with a history of anaphylaxis, angioedema, or urticaria with penicillins or ampicillin.
In summary, it is extremely important to have a consistent and reliable way to stratify cardiac risk in a noncardiac surgical patient. Furthermore the practitioner needs to be completely clear on the steps required for each patient to decrease cardiac risk and to safely plan a surgical and anesthetic treatment. Appropriate and clear communication with the anesthesia and cardiac specialists regarding the patient’s cardiovascular risk will also increase the patient’s confidence before an invasive procedure.
▪
PULMONARY
Postoperative lung complications are a significant source of overall perioperative morbidity and mortality. In some review articles, pulmonary complications have proven to be as common as or more common than cardiac complications. Some of the most common pulmonary problems, such as chronic obstructive pulmonary diseases (asthma, bronchitis, emphysema, bronchiectasis), pulmonary infections, and cystic fibrosis, should be easily identifiable through a thorough preoperative history and physical examination ( Table 1-6 ). Once identified, the extent of the disease process needs to be revealed through further testing and consultation with the pulmonary specialist. Amongst the tools available to extract further tangible evidence of the severity of the pulmonary disease, chest radiograph, arterial blood gas analysis, and pulmonary function test are worth mentioning.
| Dyspnea | Tachypnea |
| Decrease breath sounds | Rhonchi |
| Wheezing | Prolonged expiratory phase |
| Cyanosis | Barrel chest |
By obtaining such detailed information regarding the patient’s pulmonary dysfunction, one can then properly stratify the risk of perioperative pulmonary complication and make the necessary actions to optimize results.
The pulmonary risk factors can be best illustrated by dividing them into two categories: patient-related risk factors and surgery-related risk factors.
▪
PATIENT-RELATED RISK FACTORS
SMOKING
Smoking is a well-established risk factor as proven by numerous studies since Morton’s pioneering work in 1944. Regardless of other pulmonary dysfunction, smoking will increase the risk of perioperative pulmonary complications. The relative risk of perioperative pulmonary complication in smokers compared with nonsmokers range from 1.4 to 4.3. According to Warner et al, the previously mentioned relative risk decreases only after 8 weeks of smoking cessation. It is surprising to note that those who stopped smoking less than 8 weeks had a higher risk compared with those who continued smoking. Significant effort should be made by the practitioner and staff to relay such risk to the patients during the preoperative course and equip them with practical measures to achieve smoking cessation.
ACUTE RESPIRATORY TRACT INFECTIONS
Different general advice has been provided regarding the postponement of elective surgery in the face of acute respiratory tract infections. One thing is clear, that enough time needs to be permitted to allow for the acute treatment of the infection and symptoms followed by a period of recovery of the tracheobronchial mucosa. In general this can range from 2 weeks to 6 weeks. One must be cautious to further evaluate the patient following respiratory tract infection recuperation to ensure complete recovery, thus avoiding undue risk. In cases of mild viral upper respiratory infections in adults who are undergoing planned elective surgery of a site besides the chest or abdomen, it is acceptable to proceed because there is little evidence of increased risk.
ASTHMA
Having a complete understanding of the extent and severity of asthma in a patient is critical in their operative and anesthesia planning. Information, such as number of hospitalizations and emergency department visits secondary to asthma attacks in the past 2 years, amount of inhaler usage in a day, history of steroid and other medications used, and scenarios that may aggravate symptoms, is vital in planning for an asthmatic patient. It is known that well-controlled asthmatics with peak flow greater than 80% of that predicted can proceed to surgery with an average risk. Continued use of inhalers as per patient routine (well-controlled asthmatic) all the way up to the surgical procedure is advisable. Poorly controlled asthmatics require immediate and aggressive treatment before elective surgery. Such measures as stress dose steroids, avoidance of anesthetics with bronchospastic potential, use of bronchodilating anesthetics (ketamine), and meticulous intubation technique and planning (airway management) are important for the practitioner to consider during the planning of surgery and anesthetic technique.
CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)
Relative risk of pulmonary complication in this disease group ranges from 2.7 to 4.7. This variation is explained by the degree of severity of the disease state in each individual. As previously discussed, the preoperative evaluation should reveal the extent of the dysfunction through an excellent history and physical examination along with information obtained from appropriate laboratory and radiographic tests and consultants. Those with poor symptomatology, significant airflow obstruction, and poor exercise capacity require aggressive treatment before any consideration of elective surgery. Treatment modalities, such as bronchodilators, steroids, and antibiotics, along with smoking cessation and aggressive physical therapy can significantly reduce perioperative risk in this patient population.
OBESITY
Recent evidence suggests that there is absolutely no difference in the risk of pulmonary complications between obese and nonobese patients.
AGE
Age alone, based on numerous studies, is not a factor in increasing risk of pulmonary complications. Such complications are very much dependant on coexisting conditions rather than age.
SURGERY-RELATED FACTORS
The most important factor in determining the risk of pulmonary complication is the site of surgery ( Table 1-7 ). The risk increases as the incision site approaches the diaphragm. Therefore thoracic and upper abdominal surgery ranks highest in postoperative pulmonary complications. Complications are rare in operations outside the thoracic and abdominal cavities.
| Type of Surgery % of Cases with Complications (Total No. of Cases) | ||||||
|---|---|---|---|---|---|---|
| Study | Yr | Upper Abdominal | Lower Abdominal | Laparoscopic Cholecystectomy | Thoracic | All Others |
| Pooler | 1949 | 19 (331) | 11 (1334) | 0.7 (4204] | ||
| Wightman | 1968 | 19 (130) | 6 (323) | 0.6 (330) | ||
| Tarhan et al * | 1973 | 13 (75) | 7 (45) | 10 (112) | 3 (396) | |
| Gracey et al † | 1979 | 25 (57) | 0 (7) | 19 (21) | 17 (72) | |
| Garibaldi et al ‡ | 1981 | 17 (201) | 5 (208) | 40 (102) | ||
| Pedersen et al | 1990 | 33 (419) | 16 (200) | 3 (6687) | ||
| Southern surgeons club | 1991 | 0.3 (1518) | ||||
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


