Pediatric dentoalveolar surgery certainly does not make up the bulk of procedures performed in the majority of oral and maxillofacial surgery offices, but it does present the clinician with unique challenges both in patient management and the vast array of problems not encountered in adults. Whether the treatment is as simple as the extraction of a deciduous tooth or as complex as treating a sarcoma, these unique challenges and the long-term effects that our treatments have on these children must always be taken into consideration. A clear understanding of the growth and development of the pediatric patient is necessary to correctly identify abnormalities of the dentition.
The tooth bud is a collection of cells that derive from the ectoderm of the first brachial arch and the ectomesenchyme of the neural crest cells. The formation of primary teeth is evident between 6 to 8 weeks in utero, and the permanent teeth begin to form in the 20th week in utero. The initial calcification of the primary teeth ranges from 14 weeks for the incisors to 19 weeks in utero for the second molars. The permanent teeth calcify between 3 and 4 months for the incisors and 7 to 10 years for the third molars. If the dentition does not develop at these times or there is an event that disrupts the formation, then the teeth will not develop at all.
An anomaly in dental growth and development may be indicative of a more ominous problem, and the clinician must be aware of possible systemic causes including malignancy, endocrine, nutritional, and genetic abnormalities. These can be manifested in a combination of oral and extraoral findings, such as those associated with hereditary ectodermal dysplasia and Gardner’s syndrome. Thus, a comprehensive evaluation may be warranted in some cases.
The ensuing eruption pattern of both the primary and permanent dentition is also of critical importance when evaluating patients with impacted teeth. Table 10-1 shows the eruption patterns for both the deciduous and permanent dentitions.
| Deciduous Dentition | Permanent Dentition | ||||
|---|---|---|---|---|---|
| Tooth | Eruption (Mo) | Root Completion) (Yr) | Tooth | Eruption (Yr) | Root Completion (Yr) |
| Maxillary | Maxillary | ||||
| A | 7 | 1½-2 | 1 | 7–8 | 10 |
| B | 8 | 1½-2 | 2 | 8–9 | 11 |
| C | 16-20 | 2½-3 | 3 | 11–12 | 13-15 |
| D | 12-16 | 2-2½ | 4 | 10–11 | 12-13 |
| E | 21-30 | 3 | 5 | 10–12 | 12-14 |
| 6 | 6–7 | 9-10 | |||
| 7 | 12–13 | 14-16 | |||
| 8 | 17–21 | 18-25 | |||
| Mandibular | Mandibular | ||||
| A | 6½ | 1½-2 | 1 | 6–7 | 9 |
| B | 7 | 1½-2 | 2 | 7–8 | 10 |
| C | 16-20 | 2½-3 | 3 | 9–10 | 12-14 |
| D | 12-16 | 2-2½ | 4 | 10–12 | 12-13 |
| E | 21-30 | 3 | 5 | 11–12 | 13-14 |
| 6 | 6–7 | 9-10 | |||
| 7 | 12–13 | 14-15 | |||
| 8 | 17–21 | 18-25 | |||
If a pediatric patient has a tooth or a number of teeth that have failed to erupt in a timely manner, there can be multiple causes. These include but are not limited to tooth malpositioning, retained primary teeth, arch space/length discrepancies, obstruction by a supernumerary tooth or by a cyst (usually seen in teens, such as keratocysts and dentigerous cysts), or tumors (usually seen in childhood, such as compound/complex odontomas and fibro-osseous lesions). The most commonly impacted permanent teeth after third molars are maxillary canines, mandibular second premolars, and maxillary incisors.
Congenitally missing teeth are observed on a fairly regular basis with the most common, of course, being the third molars followed by the lateral incisors and the mandibular second premolars.
Finally, in 2003 greater than 12 of 1000 children were found to be victims of child abuse and neglect. As medical professionals (and conscientious providers), we are obligated to document and report cases of suspected child abuse and neglect in all 50 states to the appropriate law enforcement agency. It is estimated that more than half of the cases of child abuse involve the head, face, and neck. With these high numbers, it is very likely that as oral and maxillofacial surgeons we will encounter such cases. We have the training and expertise to identify potential victims, and we must have the courage to act in the best interest of the victim who is most often helpless.
▪
IMPACTED TEETH
The management of impacted teeth can pose a significant challenge to both the oral surgeon and orthodontist. An understanding of the cause, treatment options, and outcomes is required when formulating a treatment plan. Open dialogue between the general practitioner, pediatric dentist, oral surgeon, and orthodontist is critical for a successful outcome. This section will review the incidence, causes, diagnosis, and management of impacted teeth other than third molars.
INCIDENCE
Rates of impacted permanent teeth appear to vary among populations and range from 1% to 5%. Thilander and Myrberg performed a study on more than 6000 Swedish school children and found the prevalence of impacted teeth other than third molars to be 5.4%. Although any tooth can become impacted, most studies agree that the maxillary canine has the highest rate of impaction followed by mandibular second premolars, maxillary second premolars, mandibular second molars, and maxillary incisors. Eruption failure of mandibular incisors is relatively rare and is often associated with pathologic conditions when it does occur.
Rates of maxillary canine impaction approach 2% of the general population. Of these, 8% of them show bilateral involvement. This is greater than five times the rate of mandibular canine impactions (0.35%). Females are twice as likely to have an impacted canine as males. Jacoby found the rate of palatally impacted canines to labially impacted canines to be more than 6 : 1.
Relative to the permanent dentition, primary teeth rarely become impacted. When it occurs, it is most often a mandibular molar. It is important to distinguish between an impacted primary molar and one that appears “submerged” relative to the normal eruption of the adjacent permanent teeth. A congenitally missing succedaneous tooth will allow for prolonged retention of the primary tooth and often result in ankylosis. As the adjacent permanent teeth erupt, the retained primary tooth will take on a “submerged” appearance.
ETIOLOGY
Before treatment the cause of an impacted tooth must be ascertained. In general terms, causes of impacted teeth can be categorized into localized mechanical obstruction or systemic abnormalities. Mechanical obstruction can be attributed to arch length deficiency, premature loss of deciduous teeth, prolonged deciduous tooth retention, supernumerary teeth, odontogenic tumors and cysts ( Figure 10-1 ), abnormal eruption path, and cleft lip and palate.
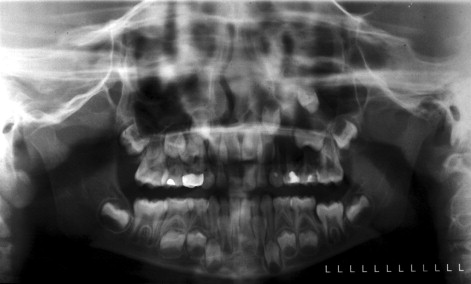
Systemic causes include hereditary conditions, such as cleidocranial dysplasia and Down syndrome. Other systemic causes include endocrine dysfunction, febrile diseases, and irradiation. Radiographs of patients with cleidocranial dysplasia show many retained deciduous teeth with unerupted permanent and supernumerary teeth, frequently with distorted crown and root shapes. Extraction of the retained deciduous teeth does not promote eruption of their permanent successors necessitating surgical exposure and orthodontic traction.
EVALUATION
After determining the cause of an impacted tooth, the clinician must devise a treatment plan in coordination with the patient’s general practitioner and/or orthodontist. Impacted teeth are evaluated by an initial clinical exam followed by a radiographic exam. Clinical signs of abnormal exfoliation and eruption sequences can allow the clinician to act early, circumventing future problems.
The initial radiographic exam should include a panoramic radiograph supplemented with a variety of other modalities that help determine the position of the impacted tooth in three dimensions. Aside from determining horizontal and vertical positions of teeth, panoramic radiographs can aid in determining buccal-lingual positions as well. A tooth that is positioned outside of the radiographic trough will appear out of focus and larger or smaller than the adjacent teeth. If positioned palatal to the adjacent teeth (i.e., further from the x-ray film), a larger image can be expected (see Figure 10-2 ). On the other hand, a smaller image can be expected if the tooth is positioned labial to the focal trough.
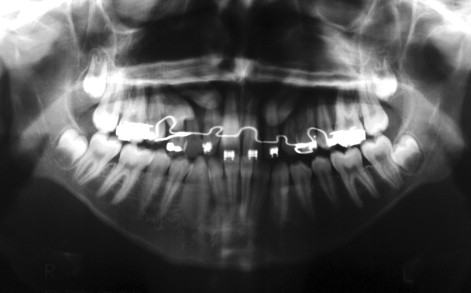
When the location of the impacted tooth is not obvious, a series of periapical radiographs are used to determine tooth position. This technique is commonly referred to as the tube-shift technique or Clark’s rule.
An initial periapical radiograph is taken in the standard fashion. A second radiograph is then taken after moving the beam source mesially or distally. If the impacted tooth appears to move in the same direction as the beam source, it is located lingual or palatal to the adjacent teeth. If it moves in the opposite direction, the tooth is buccal or labial to the adjacent teeth. The common acronym for this is S.L.O.B. (same-lingual, opposite-buccal) ( Figures 10-3, 10-4, and 10-5 ).
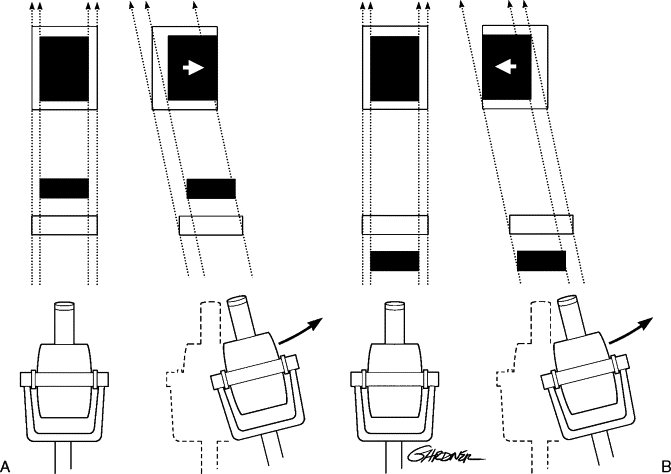
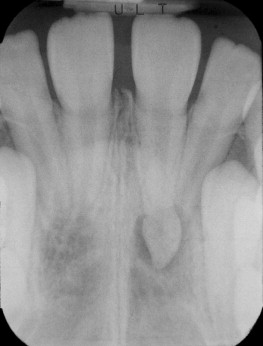
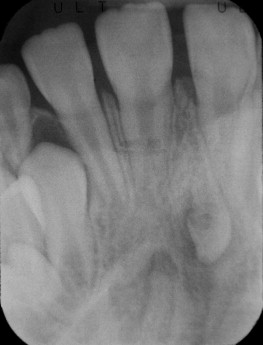
Often impacted teeth can be located in the middle of the alveolus or angulated so that half of the tooth is on the buccal side and half on the palatal. In these circumstances, an occlusal radiograph can be of value in determining tooth angulation.
In 1986 Keur made two improvements on this technique by suggesting the use of the initial panoramic radiograph and a single occlusal radiograph taken at 60° in the vertical plane. Because most panoramic radiographs capture an image at +7° to the occlusal plane, this produces a vertical angulation change of about 53°. This offers two distinct advantages: (1) An occlusal radiograph allows for the capture of the entire impacted tooth while also allowing for a greater change in angulation of the beam source. Thus, the relative change between the impacted tooth and the adjacent teeth is more obvious. (2) Because the panoramic radiograph is usually the initial film obtained, the need for two additional films is decreased to one.
TREATMENT OPTIONS
After determining the location and the cause of the impaction, the clinician should consider the treatment options. Decisions on extraction are based on associated pathologic conditions, tooth position, feasibility of orthodontic alignment, and cooperation of the patient. Studies by Stivaros and Mandall evaluated the radiographic appearance of the tooth and the decision to extract or bring the tooth into the arch. As the angulation of the tooth to the midline increased, it was more likely to be extracted. Palatally impacted teeth were more likely to be retained and brought into the arch than labially positioned teeth. Other treatment options include serial extractions and spontaneous eruption, exposure and spontaneous eruption, exposure with orthodontic traction, autotransplantation, extraction with prosthetic replacement, and no treatment.
MAXILLARY CANINES
To understand the cause of maxillary canine impaction, it is important to consider the timing of its development and the surrounding anatomy. In adolescence the maxillary canine bud is positioned high in the maxilla between the nasal cavity and the orbital rim. Posteriorly, this space is limited by the anterior sinus wall. As root formation progresses, the crown of the cuspid comes in contact with the roots of the lateral incisor mesially, the first bicuspid distally, and the resorbing roots of the deciduous canine. Theoretically, these teeth guide the developing cuspid into its proper position within the arch. When anomalies exist in lateral incisor and bicuspid form and position, the cuspid will waver from its expected eruption path.
In cases of tooth size and arch length discrepancy, the late erupting canine is prevented from taking its normal position in the arch. This will occasionally force the canine labially unless adequate space is made with extractions or orthodontic therapy. This situation only accounts for 13% of all canine impactions and probably does not represent a true impaction because these teeth have been shown to spontaneously erupt if given adequate space.
More commonly an impacted canine is positioned palatal to the arch. Jacoby found this to be true 87% of the time, of which only 15% showed arch length discrepancy. To account for the palatal position of the canine, Jacoby theorized that an excessive amount of palatal space was available for the canine to drift into. This is caused by “(1) excessive bone growth in the canine area, (2) the agenesis or hypodevelopment of the lateral incisor, and (3) stimulated eruption of the lateral incisor or the first premolar.”
Some foretelling signs of maxillary canine impaction include prolonged retention of the deciduous canine beyond 14 years, presence of a palatal bulge, delayed eruption of the permanent canine with abnormal lateral incisor shape or position, and absence of a normal labial canine bulge beyond age 11. Ericson and Kurol found in a study of 505 children between the ages of 10 and 12 that only 5% had nonpalpable canines at age 11.
Treatment
In select cases, prevention of canine impaction can be accomplished by extraction of deciduous canines as early as 8 or 9 years of age. These cases are usually limited to dental class 1 patients without crowding. Ericson and Kurol found that the position of the ectopically erupting canine can be normalized in 91% of cases by removal of the deciduous canine before the age of 11 provided that the canine crown is distal to the midline of the lateral incisor. The success rate decreases to 64% when the canine crown is mesial to the midline of the lateral incisor.
After clinically and radiographically determining a labially positioned cuspid, the clinician has several surgical options to choose from. These include excisional uncovering, an apically positioned flap , and closed eruption techniques . Tooth position and the amount of attached gingiva in the area help determine the correct procedure.
Excisional uncovering is usually done after sufficient space is created for eruption of the permanent cuspid. The procedure is most often reserved for the palatally impacted canine; however, it can be performed on a labially positioned tooth if there is sufficient attached gingiva in the area to provide 2 to 3 mm of gingival cuff after eruption. Without an adequate gingival cuff, the erupting cuspid is predisposed to future periodontal complications. This procedure is easily performed when the majority of the crown is above the mucogingival line and there is little alveolar bone to remove. When the impacted tooth is vertically aligned and there is no obstruction, spontaneous eruption will usually occur. Excisional uncovering should not be attempted if the tooth is positioned within the center of the alveolus or apical to the mucogingival line. In this situation, a closed technique or apically positioned flap is indicated ( Figure 10-6 ).
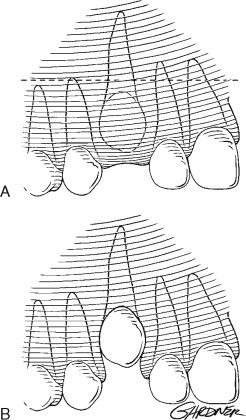
Excisional uncovering can be accomplished if the crown of the tooth is readily palpable. This is ideally performed in the late mixed dentition period to maximize spontaneous eruption; however, orthodontic traction can be used if accomplished later. Local anesthesia is infiltrated over the crown to aid in hemostasis and hydrodissection. A full-thickness mucoperiosteal window is created directly over the tooth, and the soft tissue is removed. The remaining bone overlying the crown is removed with a curette or rotary instrumentation down to the cementoenamel junction, being careful not to damage the root surface. The dental follicle is then removed, and a surgical dressing can be packed in the window for patient comfort. If spontaneous eruption is not anticipated, an orthodontic bracket may be bonded to the crown and secured to the arch wire with a chain or suture. If adequate bone is removed and the tooth is uncovered early enough (late mixed dentition), the tooth will usually spontaneously erupt to the level of the occlusal plane in 6 to 8 months. Orthodontic bracketing can then be accomplished and the tooth brought into correct occlusion.
Exposure of a labially positioned canine is often accomplished using an apically positioned flap. This procedure is indicated if there is insufficient attached gingiva in the edentulous area to provide a 2- to 3-mm cuff around the erupting tooth and should only be performed if the impacted tooth is near the alveolus. In high impaction cases, the use of an apically positioned flap can result in significant reintrusion of the impacted tooth after orthodontic therapy. Before surgery adequate arch space for eruption is usually obtained by the orthodontist. After local anesthesia, vertical releasing incisions are made on either side of the edentulous space with the base wider than the apex. A horizontal incision is made over the edentulous alveolar ridge, connecting the two vertical incisions and incorporating attached gingiva. A full-thickness mucoperiosteal flap is then reflected apically past the level of the impacted tooth. Bone is removed as necessary from around the crown, and an orthodontic bracket and chain can be attached if spontaneous eruption is not anticipated. The flap is then sutured apically to allow for simultaneous descent with the tooth during orthodontic traction ( Figure 10-7 ).
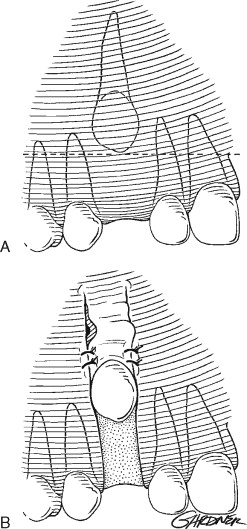
The closed eruption technique is used for high palatal or labially impacted teeth in which excisional uncovering or apically positioned flaps would be difficult or result in periodontal compromise. With the closed eruption technique, the impacted tooth is exposed in the manner described previously, and an attachment is fixated to the tooth and connected to a chain, which is sutured to the archwire for later activation. The flap is replaced with the chain exiting near the alveolar ridge space where the tooth is expected to erupt. The orthodontist then uses the chain to apply traction on the impacted tooth after 2 weeks of healing and forces eruption into the arch ( Figure 10-8 ).
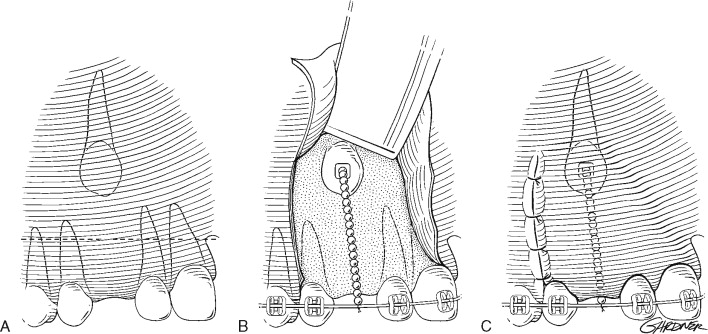
In a 30-patient study comparing labially impacted teeth treated with apically positioned flaps against those treated with the closed eruption technique, Vermette, Kokich, and Kennedy found that more periodontal and aesthetic disadvantages can be expected with the apically positioned flap technique. Those treated with apically positioned flaps were shown to have clinically increased crown lengths, gingival scarring, and intrusive relapse when compared with the closed eruption group.
PREMOLARS
Premolar impactions are more common in the mandible than maxilla and occur more often in the center of the alveolus and lingually than buccally. If the impactions are a result of an arch length discrepancy, extraction should be considered after consultation with the patient’s orthodontist ( Figure 10-9 ).
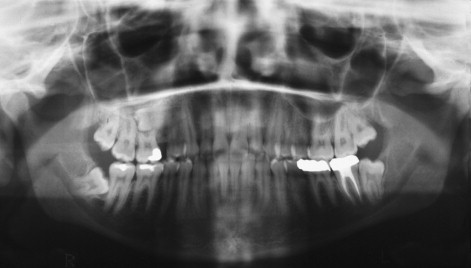
When adequate space exists to accommodate moving the tooth into the arch, the impacted premolar can be treated with the same techniques as described for the impacted canine.
IMPACTED INCISORS
Impacted maxillary incisors are commonly the result of premature loss of the primary incisors or trauma. The impacted tooth is radiographed, as described previously, to both localize the tooth and determine root development. If root development is not complete, soft and hard tissue removal is often adequate to promote spontaneous eruption. If root formation is complete or the inclination of the tooth is expected to prevent normal eruption, exposure should include bonding of an orthodontic bracket and chain to allow for traction.
IMPACTED MOLARS
Impactions of permanent first and second molars are rare, but can have a devastating effect on the dentition. If left untreated, the resulting periodontal defects, caries, and resorption can leave a patient without a functioning posterior dentition. Intervention before complete root formation is paramount to a successful outcome.
Asymmetric first molar eruption patterns should raise suspicion and warrant radiographic exam before age 7. After the age of 7, spontaneous first molar eruption is considered impossible. Treatment options of unerupted molars include surgical exposure and uprighting, extraction with implant replacement, or a combined surgical and orthodontic correction. Orthodontic correction is often complicated from limited access of the impacted tooth and insufficient anchorage, although with the current advances in orthodontic anchorage, this is becoming less of a problem. Patient compliance is also a concern because of the increased treatment time required to correct a problem that often presents itself in the later phases of orthodontic care.
Surgical uprighting of a mesially inclined second molar provides a quick and predictable answer to these problems if performed at the right time. This procedure is best accomplished when two-thirds of root formation have been completed. Before that, stabilization of the second molar in its new position can be compromised. If performed after root development is completed, a restricted blood supply from the constricted apical foramen can result in pulpal necrosis.
The surgical procedure for uprighting a mandibular second molar is described as follows: An incision is made along the external oblique line of the mandible from the anterior border of the ramus to the distal of the first molar and carried anteriorly as an intrasulcular incision to the mesial extent of the first molar. A full-thickness mucoperiosteal flap is reflected, and the developing third molar is removed in a standard fashion being careful to preserve the mesial bone. The remaining bone overlying the mesially inclined second molar is cautiously removed, and a straight elevator is used to apply judicious uprighting force on the second molar, using the buccal bone as a fulcrum. Special attention is directed at not violating the integrity of the second molar root and periodontal ligament. Uprighting is continued until the mesial marginal ridge of the second molar is level with the distal marginal ridge of the first molar. A wedgelike effect is created between the lingual and buccal cortices, and this is usually sufficient to stabilize the second molar in its new position. If stability is still a concern, an orthodontic bracket and archwire may be used to secure the tooth in the immediate postoperative phase. Occlusion is then verified, the incision is irrigated and closed, and a postoperative panoramic radiograph is taken to evaluate the position of the second molar.
Complications from surgically uprighting molars can include pulpal necrosis, root fracture, dilacerations, internal and external resorption, and periodontal complications. However, in Dessner’s retrospective study of 34 patients treated by surgical uprighting of mandibular second molars, 31 showed complete bony fill of the space previously occupied by the crown of the uprighted tooth. Only 12 of the 34 teeth showed pulpal changes, and there was no incidence of a periapical pathologic condition.
AUTOTRANSPLANTATION VERSUS EXTRACTION
Autotransplantation of impacted teeth is an acceptable alternative for patients who will not tolerate extensive orthodontic treatment. The need to minimize orthodontic treatment for patients with periodontally compromised teeth or poor dental hygiene is also a valid reason to perform autotransplantation. Sagne and Thailander were able to successfully transplant 54 of 56 canines. The technique involves ensuring adequate arch space at the recipient site before surgery. Wide exposure of the impacted tooth is accomplished followed by careful luxation from its crypt. Care is directed at not disrupting the periodontal ligament. The alveolar bone at the recipient site is conservatively contoured, and the tooth is moved into position and stabilized with a segmental orthodontic appliance. Endodontic treatment is advocated at 6 to 8 weeks beginning with calcium hydroxide paste. Conventional root canal filling is performed at 1 year following surgery. Complications associated with autotransplanted teeth are devitalization, decreased root length, periodontal compromise, and root resorption.
The decision to surgically remove an impacted tooth is considered when no other treatment is feasible. Many factors should be considered including the age of the patient, associated pathologic conditions, severity of the impaction, and the morbidity associated with a given procedure. Radiographic localization should be accomplished before removal. Anterior teeth are approached from the surface of the maxilla, with which they are most closely associated. Labially impacted teeth can usually be removed with judicious force from a dental elevator. Care is taken to avoid excessive force on developing tooth buds or adjacent roots. A full-thickness flap without release is used to expose impacted teeth on the palate. If wide access is anticipated, a palatal stent can be fabricated before surgery and placed after closure to prevent hematoma formation. Conservative bone removal with crown and root sectioning is accomplished. Longitudinal sectioning of the root can often be helpful to minimize the amount of bone removal.
Extraction of impacted premolars can be challenging because of limited access, adjacent roots, the maxillary sinus, or the mental nerve in the mandible. Extraction of maxillary bicuspids is accomplished in a similar fashion to anterior maxillary teeth. Mandibular bicuspids are usually approached from the buccal surface. When mandibular premolars are located on the buccal aspect, a buccal flap is used to gain access, the mental nerve is identified and protected, and the tooth is sectioned and delivered. When access is limited as a result of a lingually impacted premolar, buccal and lingual flaps are used, and once again the mental nerve is identified and protected. Bone is conservatively removed from the buccal surface of the mandible, and the tooth is sectioned and removed from the lingual aspect. A blunt osteotome or straight elevator can sometimes be used to “push” the premolar out the lingual cortex from the buccal. Care must be taken not to damage adjacent roots or the neurovascular bundle.
ADVANCES IN ORTHODONTIC ANCHORAGE
Orthodontic treatment is a complex process that involves the transmission of constant force to teeth to move them into proper alignment within the alveolus. Anchorage control to counteract these forces is the cornerstone of treatment and is often the limiting factor when deciding to treat a case with orthodontics alone or in combination with surgery. In particular intrusion of posterior teeth to correct an anterior open bite and distal movement of posterior teeth to correct a class 2 or 3 malocclusion presents significant anchorage challenges.
To supplement orthodontic anchorage, various intraoral and extraoral appliances have been used with varying degrees of success. Headgear, lip bumpers, Herbst appliances, magnets, and multiloop edgewise archwires have been used to maximize orthodontic anchorage. Unfortunately, these devices are cumbersome and become ineffective when patient cooperation fades. Surgical correction of skeletal malocclusions is often indicated for these patients, but declined for various social and economic reasons. Advances in skeletal orthodontic anchorage over the past 25 years have revealed other options for these patients.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


