Orthodontic Assessment and Treatment Planning Strategies
This chapter reviews the steps involved in an orthodontic assessment and briefly evaluates the principles of treatment planning. Diagnosis and treatment planning in an orthodontic practice is solely the responsibility of an orthodontist. Oral health therapists and dental hygienists carry out necessary examinations and clinical procedures within their scope of practice under the supervision of an orthodontist. Nevertheless, it is crucial to have a thorough knowledge and understanding of the processes involved in an orthodontic assessment and treatment planning.
This process commences with a patient interview to address the patient’s concerns, identifying the issues and developing a list of problems. Patient interviews provide valuable information that is critical in planning for successful treatment outcomes. Accurate analysis of all gathered records, including photographs, radiographs and study models of the teeth, leads to an accurate diagnosis and thus a successful treatment outcome.
Risks and benefits of the chosen treatment plan should be discussed with the patient and parent (if the patient is under the legal age of consent) to gain an informed consent, which is the final stage prior to commencement of the chosen treatment. It is critical that explanations are given in a simple manner with the use of terminology that is easy for parents and patients to understand.
Data Collection
Gathering an accurate and detailed patient history aids in diagnosis and treatment planning. Comprehensive records are extremely valuable as they reveal vital information regarding the general health, oral health and social and family history of the patient. During the patient and parent interview, several factors may be revealed that could compromise the treatment plan. Accurate and thorough data collection and history taking are therefore extremely important.
Clinicians must obtain a medical and dental history at initial appointments, and should review the information at subsequent visits, and update this information every six months for better patient management.
The initial appointments in an orthodontic practice are dedicated to patient interviews and consultations. This allows the dental team to get to know the patient better, to gain a better understanding of their attitude and assess their level of understanding of their orthodontic condition. These interviews are essential for better patient management, as the lifestyle of the patient is considered when treatment planning to ensure that they benefit from their orthodontic treatment.
Medical History
The objective behind taking a detailed medical history is to provide a beneficial orthodontic treatment without the patient suffering from any medical complications and to avoid medical emergencies. This can be achieved by considering the medical contraindications when treatment planning (examples of these contraindications and modified treatment planning are summarised in Table 3.1). Growth is another aspect that requires specific attention as it facilitates orthodontic treatment. Beyond the growth spurt peak, orthodontists may need to alter the treatment plan to accommodate for changes in the facial structures to prevent the treatment outcome being compromised. Box 3.1 highlights some areas covered in a medical history form. The growth assessment and the record of onset of puberty is essential in children and young adults.
Table 3.1 Medical conditions and orthodontic implications for treatment.
| Medical Alert | Concerns | Modifications for Orthodontic Treatment |
| Infective endocarditis | Risk of bacteraemia in the inner tissues of the heart causing infection and inflammation. | Separators, impressions and surgical tooth exposures may require antibiotic prophylaxis. Bonding is a better option than banding. Always maintain oral hygiene and monitor plaque control. Avoid mucosal cuts during rewire replacements. Always confirm treatment with patient’s cardiologist or physician. |
| Hypertension | High blood pressure can put the patient at risk of cardiovascular disease, renal failure and stroke. The major concern is gingival hyperplasia due to calcium channel blockers. Therefore, any signs of gingival overgrowth requires immediate attention. | To reduce stress levels, the appointments should be kept to less than one hour. Regular oral hygiene advice is necessary to ensure that plaque control is achieved. If calcium channel blockers cause gingival hyperplasia, refer to physician for new prescriptions. Delay treatment for uncontrolled hypertension until the physician confirms the condition is under control. |
| Diabetes | Hyperglycaemia causes delayed healing and patients are at higher risk of periodontal disease. This is due to reduced leucocyte function, low collagen metabolism and reduced polymorphonuclear leucocyte. Periodic periodontal assessment is necessary in patients with both type I (insulin dependent) and type II (insulin resistant) diabetes. |
Owing to periodontal breakdown, avoid treatment in patients with uncontrolled diabetes. Always confirm with the physician before starting treatment. Reduce local factors such as calculus by stressing the importance of immaculate oral hygiene. Appointments are best to be scheduled after breakfast. |
| Epilepsy | Gingival hypertrophy is associated with anticonvulsants causing red, swollen and sore gums. Studies have shown high doses of antiepileptic medications during early growth and development can affect the child’s skull development, position of teeth and periodontal structures. Other oral findings associated with antiepileptic medication include hypercementosis, root shortenings, gingival bleeding, xerostomia, ulceration and delayed eruption. It is essential to record history of seizures, related traumas and details of medication. Patients are also at risk of inhaling or swallowing fragments of appliances during seizures; nevertheless, it is important to advise patients and parents/carers to seek medical advice immediately |
Gingival contouring may be needed prior to bracket positioning in cases of severe gingival hypertrophy. Minimize stress levels during treatment. Cease procedure immediately if seizure occurs during treatment, retrieve all instruments from the mouth and lower the chair in a supine position as low as possible. If the seizure does not cease within a few minutes, seek help immediately. |
| Pregnancy | There are generally no contraindications associated with pregnancy. However, increased levels of progesterone and estrogen can cause an exaggerated response to plaque. It is essential to assess periodontal health frequently. | Monitor oral health and review oral hygiene each visit. Keep appointments short and avoid x‐rays. |
| Thyroid disorders | The hormones produced by the thyroid gland are responsible for growth, development and metabolism in the body. Common oral findings in hypothyroidism include delayed wound healing, macroglossia, delayed eruption and periodontal disease. Patients with hyperthyroidism can suffer from stress and anxiety. | Reduce stress levels throughout treatment and avoid the use of adrenaline. Cease treatment in the case of thyrotoxic crisis. Ensure that the patient visits their physician regularly. A thyroid collar is critical for taking radiographs for protection against radiation. |
| Infectious diseases | The major concern for patients with infectious diseases such as hepatitis and HIV would be maintaining good oral hygiene and high standard infection control as per guidelines. | Follow universal precaution guidelines. Good oral hygiene. Check treatment with haematologist for any medical contraindications. |
Dental History
The dental history provides valuable information regarding the motivation and cooperation of the patient in a dental setting. Gaining a better understanding of previous dental treatments and oral hygiene habits determines the level of motivation. Attending regular dental check‐ups is a good indication that the patient will comply with their orthodontic appointments as well. The dental history must be thorough, including details of any previous treatments, attitude and behaviour towards previous treatments and records of any dental trauma. One of the main contraindications of orthodontic treatment is poor oral hygiene, as the patient will be at high risk of caries and periodontal disease. It is important to record the oral hygiene regimen, such as the type of toothbrush and toothpaste used, as well as the technique and frequency of brushing. Box 3.2 highlights some areas covered in a dental history form.
Patient Concerns
Chief complaints reveal the patient’s perception of their concern, whether it be aesthetics or functional. This may or may not be the same reason as the initial referral by other colleagues. Addressing the chief complaint is key to reaching a successful treatment outcome. It is vital for practitioners to understand the patient’s concern and it is just as critical to ensure that the patient understands their orthodontic problem and in what ways it can be treated. For example, a patient might request treatment in the upper jaw because of excessive protrusion, yet the underlying problem may indicate a mandible that is retrusive and requires a more complicated treatment than the patient anticipated. Before treatment starts, the patient needs to have a thorough understanding of their functional and aesthetic orthodontic problem and accept the procedures and steps involved in their chosen treatment. Addressing the chief complaint also increases patient compliance.
Aetiology of Malocclusion
Investigating the cause of any underlying dental discrepancy is necessary. If the aetiology is unknown, a successful treatment outcome may not be guaranteed. Hereditary factors or environmental factors may contribute to the cause of the malocclusion. Eliminating environmental causes will allow better interception and enhances treatment stability. For example, if a child presents with normal craniofacial growth and an anterior open bite caused by a thumb sucking habit, it is critical to plan habit breakers as part of the treatment to cease the habit and to reduce the chances of relapse upon completion of treatment. The aetiology of malocclusion is multifactorial in nature and may be due to skeletal discrepancies, dentoalveolar issues and habits. Skeletal discrepancies can be the most difficult to treat because of their widespread effect and it may require a combination of orthodontic treatment and orthopaedic appliances or surgical correction. Dentoalveolar factors may have localised effects on the occlusion. Examples include anomalies in the position of teeth, the number of teeth, eruption patterns, crowding, spacing or pathological abnormalities such as cysts and odontogenic tumours.
Clinical Examination
The clinical dental examination is an essential part of dentistry and guides every treatment plan. A thorough orthodontic examination begins with a systematic extra‐ and intraoral examination.
Extraoral Examination
The findings of a thorough extraoral examination greatly aids in treatment planning. The extraoral examination includes a general assessment of the patient’s awareness, posture, temporomandibular joint, head, neck, skeletal pattern and soft tissues. It is important to observe the patient at rest and in function, without their awareness. This approach increases the accuracy of the assessment. The extraoral examination commences in the waiting room or consultation room by observing:
- posture
- awareness
- compliance
- level of comprehension and communication.
Facial Type and Skeletal Pattern
A valuable aspect of the extraoral examination is identifying the facial type (Figure 3.1) and skeletal pattern (Figure 3.2). The patient must be in a neutral position, sitting upright or standing, looking at a distant object straight ahead. Ensure that the Frankfort plane is horizontal and parallel to the floor by imagining a line from the upper border of the external auditory meatus to the lower border of the orbit (McDonald, 1998). It is important to ensure that the teeth are in centric relation and biting in maximum interdigitation, as these factors affect the accuracy of the examination. Some patients tend to posture the mandible forward and a false diagnosis can be recorded. The frontal view allows an evaluation of the facial type. The sagittal view allows an assessment of the skeletal pattern. On the lateral profile of the patient imagine two lines:
- From the bridge of the nose to the base of the upper lip.
- Extending from the base of the upper lip to the base of the chin.

Figure 3.1 Facial types. A) Mesofacial: well‐balanced facial features with average cranial width. B) Brachyfacial: square‐shaped faces with a prominent chin and a broad forehead, giving the appearance of a short, wide face. C) Dolichofacial: long narrow face with a small cranial width.

Figure 3.2 Skeletal patterns and facial profiles.
These lines are an indication of the facial profile and a straight line is considered to be the norm (class I). In a skeletal class II, a convex profile is evident, owing to prominence of the maxilla. In a skeletal class III, concavity in the profile is evident, owing to prominence of the mandible.
Facial appearance is evaluated in three planes of space: anteroposterior, vertical and transverse.
Anteroposterior
This is the assessment of the relative position of the maxilla and the mandible. It is classified as:
- Class I skeletal pattern: the mandible is about 2–3 mm posterior to the maxilla. The patient presents with a straight profile, known as a mesognathic profile. The harmony between the maxilla and the mandible creates this straight profile.
- Class II skeletal pattern: the mandible is too far posterior in relation to the maxilla. The patient presents with a convex profile, known as a retrognathic profile. This discrepancy may be due to a protrusive maxilla or a retrusive mandible:
- Protrusive maxilla: the mandible is in a normal position but the maxilla is positioned too far forward.
- Retrusive mandible: the maxilla is in the normal position but the mandible is positioned too far posterior in relation to the maxilla.
- Class III skeletal pattern: the mandible is positioned anterior to the maxilla. The patient presents with a concave profile, known as a prognathic profile due to the overgrowth of the mandible.
The dental base supports the alveolar process without the presence of a distinct barrier. Protrusion of both maxillary and mandibular alveolar processes is known as a bimaxillary protrusion (Figure 3.3). This protrusion of the alveolar process in the upper and lower arches can occur concomitantly with class I, class II or class III skeletal bases. Clinically, this is presented by protrusive and everted lips that are separated at rest; hence, incompetent lips. If both the upper and lower alveolar processes are retruded regardless of the skeletal base characteristics, this is termed bimaxillary retrusion.

Figure 3.3 A) The lateral cephalometric radiograph confirms the bimaxillary protrusion of the anterior segment. B) Intraoral photograph shows the protruded upper and lower incisors.
Vertical
Assessment of the lower facial height (Figure 3.4) provides a good indication of any vertical discrepancies:
- Upper third: the forehead.
- Middle third: supraorbital ridge to the base of the nose.
- Lower third: base of the nose to the base of the chin. The lower portion is further classified as:
- The lower one‐third is from the base of the nose to the base of the upper lip.
- The lower two‐thirds consists of the lower lip and chin.

Figure 3.4 Facial height.
The height of the middle third should equal to height of the lower third. An increase lower facial height is commonly seen in patients with a class III skeletal base owing to the prominence of the chin. A decreased lower facial height is seen in patients with class II skeletal base with a retrusive mandible.
Transverse
A mild asymmetry can be considered to be normal. However, any asymmetry must be noted clearly as part of the extra oral examination. This may be due to discrepancies in the transverse sizes of the maxilla and/or the mandible.
Assessment of Lymph Nodes and the Temporomandibular Joint
The head and neck regions are examined for any alerts that may indicate an underlying condition, which may require specific attention prior to starting the treatment. The head and neck must be palpated to ensure that the lymph nodes are of normal size and no abnormalities can be detected.
The temporomandibular joint and the surrounding muscles must be checked for anomalies such as tenderness, crepitus (clicking sound that occurs due to friction between cartilage and bone) and deviations that can affect the orthodontist’s therapeutic approach and appliance design. If the patient presents with one or more signs of irregularities, a referral to an oral maxillofacial surgeon may be indicated for further investigations.
Soft Tissue Analysis
This part of the examination is most effectively and accurately achieved by assessing the patient in function and at rest, without their awareness. It is important to note the following as part of the soft tissue analysis:
- Lip morphology: fullness, tone and form of the lips.
- Lip competency and anterior oral seal: determine how well the upper and lower lips can meet without muscular effort. Lip incompetency may be due to a bimaxillary protrusion, short resting lip length, increased lower anterior face height or protruded upper incisors due to a severe class II. If the lips are incompetent, a normal anterior oral seal will not be achieved.
- Smile framework: the dental midline will set a starting point for achieving an aesthetically pleasing smile. Ideally, the dental midline needs to be parallel and in the same direction as the facial midline. The degree of incisor display and smile symmetry are important aesthetic parameters.
- The lip line: the position of the upper lip is pivotal to the degree of upper incisor display. This exposure of the height of the incisors is called the lip line. Reduced incisor display may be an indication of aging. The lip line must reach the gingival margin, displaying upper incisal edges and the interdental gingiva. A ‘gummy smile’ is the term given to a higher than average lip line, which exposes excessive gingiva.
- The golden proportion: the golden proportion of the width of the upper teeth displayed on a frontal view upon smiling is a recurrent 62% proportion – the width of the upper lateral incisor displayed should be 62% of the upper central incisor, the apparent width of the upper canine must be 62% of the upper lateral incisor and the first upper premolar apparent width should be 62% of the upper canine.
- Black triangles: these are the gingival embrasures contour around the interproximal contacts in an aesthetically pleasing smile. Short interdental papillae fail to contour the interproximal contacts, so black triangles develop. Black triangles may occur as a result of periodontal disease and are commonly seen after correction of severely crowded or rotated teeth.
- Buccal corridors: the smile width can be assessed by checking the degree of the first upper premolar exposure. The buccal corridor is the space formed between the inner buccal surfaces and the maxillary molars upon smiling. An aesthetically pleasing smile has reduced buccal corridors (Moore, 2005). The anteroposterior position of the maxilla and the inclination of the upper molars influence the width of the buccal corridor. Increased arch width results in reduced buccal corridor. Palatally inclined molars results in increased buccal corridor width.
- Smile arc: There are three types of smile arcs:
- Consonant: the border of the lower lip follows a curvature along the upper incisal edges. This is considered an ideal smile arc.
- Flat: the superior boarder of the lower lip is parallel to the upper incisal edges.
- Non‐consonant: the top border of the lower lip forms a reverse curve with the upper incisal edges.
- Tongue: check for tongue thrust during speech or swallowing. Tongue thrust is protrusion of the tongue between the incisors due to musculature imbalance.
Intraoral Examination
The purpose of this part of the examination is:
- to address chief compliant
- to determine clinical signs of malocclusion or dentoalveolar discrepancies
- to check periodontal health
- to assess the patient’s oral health and hygiene status.
A systematic approach is needed to prevent omission. The intraoral examination commences with an assessment of the soft and hard tissue for any lesions, congenital abnormalities and evaluation of the occlusal relationships. Orthodontists assess four areas to make a diagnosis of the malocclusion:
- Upper jaw
- Upper dentoalveolar
- Lower dentoalveolar
- Lower jaw
The anteroposterior, vertical and transverse relationships of the alveolar bone, dentition and the underlying basal bone forms the final diagnosis.
Soft Tissues
In a logical approach, all the soft tissues in the mouth must be assessed for any abnormalities. Using a good source of light, dental mirror and a probe, examine:
- the oral mucosa and vestibules
- the glands
- the fraenum
- the health status of the gingiva
- the gingival margins
- the soft and hard palate
- the tongue.
A periodontal chart is also recommended for patients presenting with signs of poor periodontal health. In cases of any form of periodontal disease, orthodontic treatment is contraindicated until the disease is under control, regardless of the age of the patient.
Hard Tissues
Teeth must be charted carefully and all findings must be recorded thoroughly. The clinical examination must have a systematic routine to ensure that nothing is missed. It is recommended to begin the examination from one quadrant and move across to the next, assessing and recording:
- the presence of pathology
- detected caries
- erupted teeth
- enamel morphology
- missing teeth and reason for tooth loos
- previous dental treatment
- previous or current trauma.
It is extremely important to note the pattern of eruption to assess the dental age. Delayed eruptions, particularly asymmetrical delayed eruptions, may indicate an underlying problem such as a supernumerary teeth, ectopic eruption or impaction (see Chapter 6). The area must be palpated for permanent successors both palatally, lingually and labially. Radiographs are necessary if the permanent successor is not palpable. However, further data collection may be required in patients with a history of trauma, as the tooth may be dilacerated (bent roots), resulting in a delayed eruption.
Occlusion
Occlusion is the relationship between the upper and lower jaws. Various terminologies are given to the occlusion depending on how the jaws meet. When the teeth meet during a function, such as speech or eating, the occlusion is termed ‘dynamic occlusion’. The centric relation is critical during an intraoral examination. The centric relation is the most posterior position of the mandible. In centric relation, the mandibular condyle is in the most superior and posterior position in the glenoid fossa. The centric relation is considered the orthodontic problem. The centric occlusion refers to the habitual bite or bite of comfort. Centric occlusion is also known as intercuspation position, because of the maximum interdigitation as the cusps of both arches lock in completely.
Dentoalveolar Compensations
When noting malocclusion and skeletal patterns, attention must be paid to dentoalveolar compensations. The dentoalveolar compensatory mechanism is when discrepancies are camouflaged or disguised due to dentoalveolar modifications; for example, protrusive upper anterior incisors camouflaging the severity of a skeletal class III malocclusion.
Midline Shift
Check the path of mandibular closure to assess the midline when the patient bites into maximum interdigitation. Any displacement or deviation upon closure is best examined from behind, looking directly down from above the patient. The patient must therefore be in a supine position.
Occlusal Curvature
Another critical aspect to be noted is the curvature of the occlusion. An ideal occlusion contains a flat occlusal plane. The various types of occlusal curvature are:
- the curve of Spee: a curvature in the mandible caused by extrusion of the anterior teeth and intrusion of the molar teeth. It is typically seen in deep bites (Figure 3.5a).
- the curve of Wilson: a curvature in the occlusion resulting from inward tipping of the molars (Figure 3.5b).

Figure 3.5 Types of occlusal curvature: A) Curve of Spee. B) Curve of Wilson.
Occlusal Relationships
The canine and molar occlusal relationships are best assessed using Angle’s classification and the incisor relationships examined on the basis of the British standards incisor classification (Table 3.2). In an ideal occlusion, all lower teeth are about half a unit anterior to the upper teeth (Figure 3.6). This is because of the size differences between the upper and lower incisors; the lower anterior teeth are narrower than the upper anterior teeth.
Table 3.2 Assessment of canine and molar occlusal relationships: Angle’s classification and the British standard classification of incisor relationships.
| Classification | Class I Neutrocclusion |
Class II Distocclusion |
Class III Mesiocclusion |
| Angle’s Classification | |||
| Molar relationship | The mesiobuccal cusp of the upper first molar occludes on the mesiobuccal groove of the lower first molar. | The lower first molar is positioned distal to the upper first molar. | The lower first molar is positioned mesial to the upper first molar. |
| Canine relationship | Upper canine occludes on the mesial half of the lower first premolar and the distal half of the lower canine. | Upper canine occludes anteriorly to the lower first premolar. Thus, the distal surface of the lower canine lies posteriorly to the mesial surface of the upper canine by width of a premolar. If it is less than width of a premolar it is given the term ‘tendency towards class II’. | The distal surface of the lower canine lies anteriorly to the mesial surface of the upper canine by width of a premolar. If it is less than width of a premolar it is given the term ‘tendency towards class III’. |
| British Standard Classification of Incisor Relationship | |||
| Relationship | The lower incisor edges occlude with or lie immediately below the cingulum of the upper central incisors. | The lower incisor edges lie posterior to the cingulum of the upper incisors. There are two subdivisions to this classification. The first division is protrusion of the incisors resulting in an overjet and the second division results in a deep bite as the upper central incisors are retroclined. | The lower incisors lie anterior to the upper central incisors. There is reduced or reverse overjet. |

Figure 3.6 Normal occlusion.
Source: Illustration by Professor Ali Darendeliler.
Class I Malocclusion
Class I represents the ideal occlusion. Orthodontists aim to achieve class I molar, canine and incisor relationships when planning any treatment (Figure 3.7). However, a class I malocclusion can present with normal molar, canine or incisor relationship but discrepancies within the arches may be evident. The common problems are dental‐related issues rather than skeletal abnormalities, with the exception of bimaxillary cases. The list below covers some of the most common findings in class I malocclusion that require significant attention during examination. These findings can be evident in combination with class II and class III malocclusions and are not confined to class I malocclusion.
- Crowding and spacing.: the lack of space results in crowding and occurs as the maxilla and/or the mandible fail to accommodate for any size discrepancies between the dental arches and the teeth. Extra spacing can be related to microdontia (teeth smaller than the normal size), tooth loss or hypodontia (congenitally missing teeth).
- Rotations: teeth that are rotated in the socket.
- Ankylosis: this is the term used to describe fusion of roots to the alveolar bone. Ankylosis is commonly seen in overretained deciduous teeth with missing permanent successors.
- Cross bite (Figure 3.8A): this is commonly seen in patients with a narrow maxilla. Cross bite occurs when maxillary teeth are positioned lingually in relation to the mandibular teeth. It can occur anteriorly or posteriorly and may involve one tooth or a group of teeth.
- Scissor bite (Figure 3.8B): the maxillary teeth rest completely outside or inside the mandibular teeth.
- Impacted teeth: blockage of an erupting tooth is called impaction. The most commonly impacted teeth are the third permanent molars and canines.
- Ectopic teeth (Figure 3.9): teeth erupting or located in an unusual position.


Figure 3.7 Class I: A) molar and canine relationship. B) Class I Incisor relationship.
Source: Courtesy of professor Ali Darendeliler.

Figure 3.8 Class I malocclusions: A) Cross bite. B) Scissor bite.

Figure 3.9 Ectopic central incisor.
Class II Malocclusion
Class II malocclusion is shown in Figure 3.10. Within class II, a division 1 malocclusion is an increased overjet with proclined upper central incisors (Figure 3.10B). A division 2 malocclusion is an increased overbite with retroclined upper central incisors (Figure 3.10C). The upper lateral incisors overlap the central incisors in some cases (Figure 3.11).

Figure 3.10 Class II: A) Molar and canine relationship. B) Incisor relationship, division 1. C) Incisor relationship, division 2.

Figure 3.11 Class II division 2; retroclined upper central incisors with proclined lateral incisors.
Patients with class II skeletal patterns tend to position the mandible forwards to reduce the degree of overjet and to disguise the underlying problem. This false bite is known as a Sunday bite. When assessing the profile and examining the occlusion, check that the mandible is not positioned too far forward.
Overjet is the horizontal discrepancy between the upper and lower incisors measured in millimetres (Figure 3.12B). In cases of severe overjet, the lower incisal edges will bite in the soft tissue of the maxillary anterior region (Figure 3.13). This traumatic bite will lead to gingival ulceration and recession if left untreated. Overbite is the vertical discrepancy between the upper and lower incisors measured in percentages (Figure 3.12A).

Figure 3.12 A) 100% overbite. B) Overjet.

Figure 3.13 Traumatic bite.
Class III Malocclusion
Class III malocclusion is shown in Figure 3.14. In some cases, the patients can achieve an edge‐to‐edge bite but, once at rest, the lower incisors can slip forwards, resulting in a reverse jet. This bite is called pseudo class III, as the patient does not have a true class III malocclusion, meaning the centric relation is edge to edge as the mandible is in its most posterior position (Figure 3.15). However, the centric occlusion as the habitual bite of the patient slips into a class III, as the mandible protrudes forward to achieve maximum interdigitation.

Figure 3.14 Class III malocclusion: A) Molar and canine relationship. B) Incisor relationship.

Figure 3.15 Pseudo class III: A) Centric relation: edge to edge bite. B) Centric occlusion.
Primary Dentition
The permanent and primary dentition share the same classification for incisor and canine relationships but the molar classification is assessed on the terminal plane, based on the relative position of the upper and lower second primary molars in a vertical plane (Figure 3.16).
- Flush terminal plane: the distal of the primary mandibular second molar lies in line with the distal of the primary upper second molar (same vertical plane). This can lead to a class I or a class II molar relationship in the permanent dentition.
- Distal step: the distal of the primary mandibular second molar lies distal to the primary upper second molar. A class II molar relationship is predictable in the permanent dentition.
- Mesial step: the distal surface of the primary mandibular second molar lies mesial to the primary upper second molar. Studies reveal that this type of occlusion typically results in a class I molar relationship in the permanent dentition. However, if the mesial step is greater than 2 mm, a class III molar relationship is inevitable.

Figure 3.16 Terminal planes: 1) Flush terminal plane. 2) Distal step. 3) Mesial step.
Leeway and Primate Spaces
The difference in the mesiodistal width between the primary teeth and their permanent successors is known as the leeway spaces (Figures 3.17). The total width of primary canines, first and second primary molars is greater than the total width of permanent canines, first and second premolars. In the upper arch, there is an average of 1–1.5 mm excess space per quadrant and in the lower arch there is an average of 2–2.5 mm of excessive space per quadrant. These space discrepancies can be used in relieving minor crowding to a degree in the permanent dentition.

Figure 3.17 Leeway spaces: the differences in the mesiodistal width between the primary teeth and their permanent successors.
Source: Courtesy of Professor Ali Darendeliler.
Spacing in the primary dentition is common and expected. Space is commonly detected mesial to the maxillary canine and distal to the mandibular canines. These spaces are known as primate spaces (Figure 3.18). Generally, crowding is expected in the permanent dentition if spacing is not evident once the primary dentition is established.

Figure 3.18 A) Primate spaces. B) Example of leeway spaces; the mesiodistal width of the deciduous molars is larger than the width of the permanent premolars.
Mixed dentition
The term ‘mixed dentition’ is given to a dentition where the both permanent and primary teeth are present. Early detection of malocclusion aids in prevention of complex orthodontic treatment in the later stages of growth and development. The eruption of permanent teeth should be monitored to detect any signs of abnormalities in the pattern of eruption during the early mixed dentition stage.
The early mixed dentition stage begins with eruption of the first permanent molars and lower incisors around the age of six years. Several factors influence this stage of development and affect the direction of eruption of the lower incisors:
- rotation of growth
- soft tissue
- habits.
The late mixed dentition stage commences with the eruption of the lower canines and the upper and lower first premolars at the age of eleven years.
Between the ages of 7 and 12 years, children may undergo a phase known as the ‘ugly duckling’ stage (also known as the Broadbent phenomenon, after B. H. Broadbent, who first described it in 1937). A median diastema (space in the midline) occurs, with protrusion and lateral spacing of the upper incisors preceding the eruption of the maxillary canines. As the upper canines erupt, the incisors mesialise and the closure of the diastema becomes evident. This can be monitored and active orthodontic treatment is generally not indicated unless it is accompanied by an underlying skeletal discrepancy.
From the ages of 8–10 years of age, the presence of canine successors should be palpable in the sulcus of both upper and lower arches. Radiographs are indicated if delayed eruption is noticed or the permanent successors are not palpable. Negligence in monitoring the pattern of eruption leads to irrevocable consequences. In Figure 3.19, an ectopic canine was not detected at an early stage. The ectopic upper left canine resorbed the root of the upper left central incisor (Figure 3.20). Saving the incisor became impossible for the orthodontist as more than one‐third of the root was resorbed and a significant degree of mobility was evident clinically. Extraction of the upper left central incisor and the overretained deciduous canines was indicated to create space for the eruption of the canine into the central incisor space. This technique is known as transposition.

Figure 3.19 Ectopic canine not detected at an early stage; initial records.
Source: Case by Dr Jim Bokas.

Figure 3.20 Three‐dimensional scan of the ectopic canine reveals the damage that it has caused to the upper left central incisor.
Source: Courtesy of Dr. Jim Bokas.
Once the canine was erupted and aligned into position, cosmetic restorations were used to alter the shape of the canine to resemble the central incisor and final alignment and space closure was achieved (Figure 3.21–3.23).

Figure 3.21 Space was created using fixed appliances to allow eruption of the upper left canine in the central incisor position. This is termed transposition.
Source: Courtesy of Dr. Jim Bokas.

Figure 3.22 Composite resin restoration of the canine was indicated to resemble the central incisor.

Figure 3.23 End of treatment records.
Source: Courtesy of DR. Jim Bokas.
Records
Dental photographs and models of teeth are valuable diagnostic tools in orthodontics. In this section, the essentials for quality photographs and dental impressions are discussed.
Photographs
Dental photographs are essential medico‐legal documents and have other major benefits such as marketing, communication among practitioners and patient education. Thus, the quality of the photographs must be of a high standard. These photographs not only provide valuable baseline data in practices but also create a visual record of the orthodontic problem of the patient and aid in the acceptance of treatment.
To document accurate pre‐ and post‐treatment photographs of a high standard, the clinician must learn to control and standardise the variables. These variables include technique, patient positioning and selection of camera, lens and flash. Photographs within the oral cavity are termed intraoral photographs and photographs of the head and neck are extra oral photographs (Figure 3.24).

Figure 3.24 A series of ideal extra‐ and intraoral photographs.
The Camera
Camera selection plays an important role in achieving a high standard of photographic record. A digital single lens reflex (DSLR) camera is an ideal choice. Other cameras may require extra equipment to adapt them to be appropriate for dental photography. Lens and flash selection also require specific attention. Macro lenses allow close distance photographs taken without affecting the quality of the image.
The following must be considered for capturing clinical photographs:
- Focus: all images must clearly show the required detail. If an image is blurred, it is out of focus. By turning the focus ring, the image will sharpen.
- Exposure: the images must have sufficient light. The exposure is determined by luminesce of the area, shutter speed, ISO setting and lens aperture. Shutter speed is the exposure duration, controlling the amount of time the sensor is exposed to light. ISO settings control the sensitivity of the sensor to the light. Sensitivity is reduced with lower ISO. If sensitivity is high due to an increased ISO, images will have grains or ‘noise’ added to it. Generally, ISO is increased in low luminesce areas. Aperture controls the amount of light passing through the lens and it is known as the f‐stop value. The depth of field is dependent on the aperture. The lower the aperture, the shallower the depth of field as more light will pass through the lens.
- Framing: capturing the subject only. Capturing the top of the head up to the shoulders is sufficient for the extra oral photographs. Intraoral photographs must clearly show all the hard and soft tissues.
Settings
The DSLR camera offers several settings. All exposure settings will be preselected if the camera is set to automatic. In the manual mode, all three variables of shutter speed, ISO setting and aperture must be set as required for the image being captured. The author recommends the following for quality photographs on a manual setting:
- ISO – 1/60 seconds
- extraoral – lower aperture (f); e.g., 5.6
- intraoral – higher aperture (f); e.g., 22.
The setting can greatly vary, depending on the type of camera used. Every specialist will have their own preferred setting for capturing clinical photographs.
Technique
Extraoral Photographs
Extraoral photographs should be obtained against a plain background with the camera held at 90 degrees (Figure 3.25A). The posture of the patient plays a major role in the accuracy of the photographs. The patient should be in a relaxed neutral position, with the chin parallel to the floor and the eyes focused on the lens. The top of the head, forehead, ears and base of the neck must clearly be visible, excluding the shoulders. Hair should be tied back and any items covering the face and neck must be removed, such as glasses, scarf or hat. One photograph should be taken with the patient in a resting position with relaxed facial muscles and a second with the patient smiling and biting in maximum interdigitation. Some orthodontists may also request a close‐up of the smile for further assessment of the smile. Another photograph is needed of the lateral profile of the patient in a relaxed position, for assessment of the skeletal pattern and facial profile. To assess the social smile framework, the patient can be asked to slightly turn from the profile position to capture a 45‐degree profile, also known as three‐quarter profile.
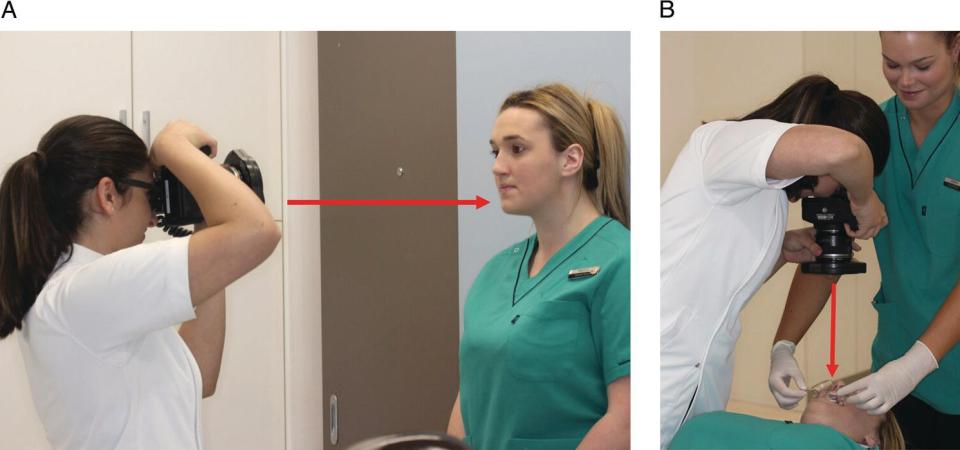
Figure 3.25 Camera position for: A) Extraoral photographs. B) Intraoral photographs.
Intraoral Photographs
The patient must be seated comfortably in a supine or semi‐supine position for intraoral photographs (Figure 3.25B). It is crucial that the camera is positioned directly above the patient. Cheek retractors are used to retract the cheeks and lips, allowing a better field of view of the occlusion. Three photographs are taken:
- centre occlusion
- left occlusion
- right occlusion.
It is extremely important that the first molars are visible in photographs showing molar relationships. Lip retractors move the upper or lower lip away from the teeth as intraoral mirrors are placed posterior to the last erupted molar (Figures 3.26 and 3.27). A photograph of the reflection provides upper and lower occlusal views. To prevent the dental mirrors from becoming foggy, ask the patient to breathe through their nose and the mirror must be kept in warm water before insertion into the mouth. To avoid trauma and burn to the intraoral tissues, ensure that the mirror is cooled down before inserting it into the mouth. It is also important to notify the patient of all the steps involved for better patient management. Guiding the patient also enhances patient cooperation.

Figure 3.26 Intraoral photography accessories: cheek retractors (top), lip retractor and occlusal mirror (bottom).

Figure 3.27 Intraoral photography accessories.
In extraoral photographs, common errors include:
- Poor patient posture – the patient should not slouch.
- Incorrect head and neck position – the head must be in a neutral position. Care must be given the head and neck are not positioned too far back, too low or tilted.
- The chin and forehead must be relaxed in all the photographs.
- Hair covering the forehead and face – hair must be tied back to make the face, ears and neck visible.
- Not capturing the base of the neck.
- Out of focus images.
- Incorrect framing.
In intraoral photographs, common errors include:
- Not capturing all the critical intraoral structures.
- Poor cheek and lip retraction results in coverage of the roots and the mucogingival areas by the lips.
- Incorrectly sized intraoral mirrors and retractors can be uncomfortable for the patient and can cause insufficient retraction.
- Incorrect camera angulation – the image will not be accurate.
- Incorrect patient positioning – the angulation of the image is affected if the patient’s head is positioned too far upwards or downwards.
- Out of focus images.
Impressions and Digital Scanners
Dental impressions provide an imprint of the teeth, gingiva and surrounding tissues. A positive model is created once the alginate impressions are poured with plaster to achieve a replica of the oral tissues. Cast models are used as a diagnostic tool and fabrication of appliances. Therefore, the quality and accuracy of the impressions are critical (Figure 3.28).

Figure 3.28 Ideal impression on the left side, showing sufficient detail of hard and soft tissue coverage. On the right side, there is dragging of the posterior region, sufficient details are not captured and the impression material mix was of a poor quality as it was set prior to insertion so the teeth are not fully captured.
Impression Trays
Choosing a correct impression tray size is the first step to a great impression. The trays are either plastic or metal (autoclavable). Perforations in the trays enhance the adhesion of the alginate to the tray. To increase the retention and prevent separation of the material from the tray, adhesives are brushed on the inner surfaces of the tray before loading the alginate material.
Impression Materials
The impression materials are classified as non‐elastic and elastic. Non‐elastic materials are plaster and wax. Elastic materials are further categorised as synthetic elastomers and hydrocolloids.
Elastomers
Polysulfide, silicone and polyether are three different types of synthetic elastomers. These are manufactured in three different viscosities of light body with low viscosity, medium/regular body and heavy body, which has the highest viscosity. Silicone is classified based on its polymerisation method. Type I is condensation curing and type II is addition curing. Putty materials are a type of silicone that are extremely viscous and consist of a much higher filler content than the heavy‐body silicone. Putty was invented to reduce the shrinkage effect upon polymerisation of the material due to its higher filler content. Typically, putty is used in combination with a low‐viscosity silicone in a putty wash technique (discussed in the technique section). Polysulfide and condensation‐cured silicone have comparable physical properties, although polyether and addition‐cured silicone similarly present better dimensional stabilities. The maximum storage time for synthetic elastomers is around 48 hours.
Hydrocolloids
There are two types of hydrocolloid dental impressions: agar and alginate. Agar can repeatedly reverse between high‐viscosity gel and low‐viscosity solution with temperature changes. Agar is not commonly used in the dental setting, as it requires complex set‐up and armamentarium. Alginate is irreversible, as it will not convert back into solution after gelation. Alginate is non‐toxic, non‐irritant and inexpensive. It is therefore widely used in dental practice. Hydrocolloids are hydrophilic with insufficient tear resistance and poor dimensional stability (Walls, 2002). Over the years, manufacturers have produced dust‐free alginate materials with improved formulas that provide better physical properties to enhance the accuracy and stability of the material.
Alginate Setting Reaction
Alginate is in a form of a powder composed of sodium alginate, calcium sulphate, trisodium phosphate, diatomaceous earth, zinc oxide and potassium titanium fluoride (Nandini, 2008). Once mixed with water, a chemical reaction between the soluble alginate and the calcium sulphate occurs, resulting in the production of a gel gel‐like insoluble calcium alginate. The setting rate of this reaction can be controlled by water temperature. The higher the temperature of the water, the faster the material sets. Trisodium phosphate is incorporated into the material to slow down the chemical reaction and increase working time. Some alginate materials are manufactured with a colour change setting indicator, meaning it will change colour upon setting.
Mixing and Loading Alginate
The powder to water ratio can vary, depending on the manufacturer’s guidelines.
Using a flat spatula, the content must be mixed rapidly. To prevent air bubbles becoming trapped in the material, smear the mix against the mixing bowl. The aim is to achieve an alginate mix that is smooth and viscose. The alginate mix becomes runny with excessive water or dry and hard to mix with insufficient water. The impression trays must be loaded with adequate material. The excess is to be removed from the edges of the tray and over the surface.
Technique
The initial step is to decide on the correct tray size for the dental arch, regardless of the type of material used. In the upper arch, the trays must cover the hard palate, maxillary tuberosity and the vestibular areas. In the lower arch, the tray must cover the mandibular retromolar area, lingual fraenum, tongue space, vestibular area and the mylohyoid ridge. Anteriorly, there must be about a 5 mm space for the material to fill in the vestibular areas. The edges of the trays are usually covered with peripheral wax for better patient comfort and act as an extension to the tray. Prior to loading the material on to the impression trays, an adhesive is brushed over the inner surfaces to prevent separation of the material upon removal.
Alginate impressions
Its best to take the lower impression first, as the upper impression induces a gagging reflex in many patients. There are two ways in which impressions can be taken:
- Keeping the patient in a supine position.
- Keeping the patient sitting upright.
Both positions can have advantages for the patient and the practitioner. Keeping the patient in a supine position provides a better field of vision for the practitioner and thus better placement of the impression tray, particularly in the upper. Sitting upright position can be more comfortable for the patient, particularly those with a strong gag reflex.
For a better field of vision and positioning of the trays, it is best to stand behind the patient for the upper impression (Figure 3.29A) and in front of the patient to take the lower impression (Figure 3.29B). Use a dental mirror to retract the cheek and lip. Always insert the trays in sideways first to avoid overstretching the labial commissures. Always seat the impression on the posterior teeth first and slowly seat the anterior, with no movement once the tray is positioned. Any movement after the tray is seated will cause distortion to the impression.

Figure 3.29 Taking an impression: A) Standing behind the patient for the upper. B) Standing in front of the patient for the lower impression for a better field of vision.
Ensure that teeth are not desiccated, as the radicals from the chemical reactions in the material tend to bond with enamel hydroxyapatite. Thus, removal of the impression will be difficult or may result in tear of the material. If the impressions are required on patients with braces, it is important to cover it with dental wax to prevent tear of the alginate upon removal.
Impressions are not pleasant for patients and cause a gagging reflex, particularly if the impression reaches the soft palate. It may also be psychologically induced, particularly in anxious patients. The best strategy for managing patients during this procedure is to help patients control their breathing pattern. Slow deep breaths through the nose can aid in managing anxious patients and are an expedient distraction.
Putty wash
The putty‐wash technique can be obtained in three methods:
- Laminate technique – this is a one‐stage impression technique, as both putty and wash are recorded instantaneously. This technique is also termed twin mix.
- Two‐stage unspaced – putty is loaded in the dental tray and seated on the mouth. A thin layer of wash is lined over the set putty and reinserted in the mouth.
- Two‐staged spaced – once the putty is recorded and set, a space is created for the wash with either polyethylene spacer over the teeth before the putty impression is taken or making indentations in the putty to create channels for outflow of the wash.
Bite Registration
Bite registration is essential, particularly for study models. Diagnosis becomes difficult for orthodontists if an incorrect bite is registered. Fabrication of some appliances also requires bite registration; thus, incorrect technique will lead to poor fit of the appliance. A non‐elastic impression material such as wax is typically used for bite registration. The wax is trimmed into small rectangles and softened in warm water before insertion in the mouth. Polyvinyl siloxane (PVS) can also be used to obtain bite registration. Monitor the patient closely to ensure that the correct bite is captured. It is best to position the wax posteriorly on the occlusal table for better vision of the incisal relationships. If the wax covers too much of the anterior region, it will be difficult to check for the correct occlusion. Capturing the molars and canines is usually sufficient for a quality bite registration.
Disinfection and Storage
All dental impressions must be disinfected prior to any laboratory preparations to prevent cross contamination without causing distortions to the impressions. Once removed from the mouth, impressions must thoroughly be rinsed under cold running water to remove saliva, debris and blood. Studies suggest that all impressions should be immersed in 1% sodium hypochlorite for a minimum of ten minutes.
Inappropriate storage can cause distortion to the material, so it is recommended that the impressions are poured with plaster immediately or stored in cool temperatures in damp tissues to prevent dehydration of the material. The impression dries out and shrinks if left in open air for a prolonged period of time. Evaporation of moisture from the impression is termed syneresis. If the material is left in excessive water, it swells and expands, which is known as imbibition.
Cast Models
The impressions are poured with a non‐elastic impression material such as plaster of Paris to achieve a positive of the impressions (Figure 3.30). These casts are used as records, study models or fabrication of appliances. The plaster is mixed with water similarly to alginate. The water and plaster ratio can vary depending on the manufacturing guidelines. To avoid air bubbles in the final cast models, a dental plaster vibrator machine is used in laboratories. The impression trays are placed over the machine and plaster is poured from one end of the impression until all teeth are covered with the material. The base of the material should have a thicker consistency, so a higher powder to water ratio is needed to create the base. These are left to set over time and trimmed once hardened (Figure 3.31).
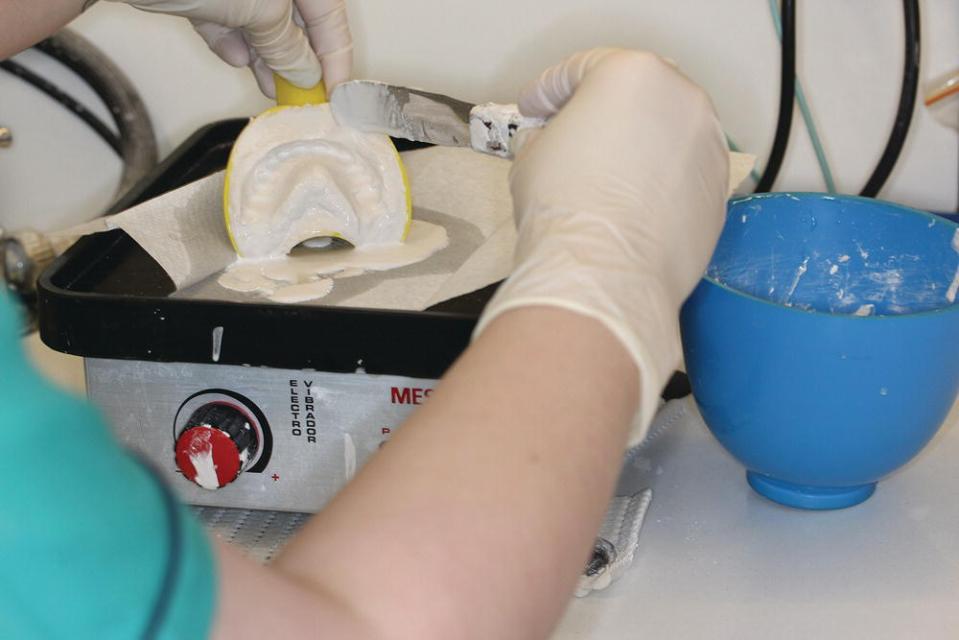
Figure 3.30 Pouring impressions with plaster of Paris.

Figure 3.31 Trimmed plaster models.
Common Errors
To guarantee high standards, practitioners must examine each impression thoroughly prior to disinfection and storage. Some of the common errors include:
- separation of the material from the tray
- voids or drags
- air bubbles in the impression
- syneresis or imbibition due to improper storage
- removal of impression from the mouth prior to setting results in an inaccurate impression
- air bubbles in cast models due to incorrect technique
- breakage of models during separation of the impression trays from the models (the models are prone to breakage if the material is still soft if it is not set).
Digital Scanners
Over the years, there has been a paradigm shift in taking dental impressions and cast models in dentistry. In many practices, digital scanners have replaced dental impressions (Figures 3.32 and 3.33). The digital scans are sent to digital laboratories to produce three‐dimensional models of the digital data. This innovative technology has several advantages in comparison with conventional impressions and plaster models. Advantages are:
- greater accuracy
- better patient comfort
- digital storage of models
- eliminates the risk of cross contamination.

Figure 3.32 Digital scanner; the iTero machine uses a powder‐free technology for accurate scanning; a gentle stream of air disperses from the wand.

Figure 3.33 The TRIOS POD is another example of a digital scanner. This innovative technology is a much smaller scanner with dramatically reduced chair time and provides more patient comfort. This scanner can easily be connected to multiple laptops or computers and the pod solution allows the scanner to easily be relocated and shared among various treatment rooms.
There are four types of imaging technology (Kravitz, 2014):
- Triangulation uses laser light to measure angles and distances used in CEREC (Chairside Economical Restoration of aEsthetic Ceramics, or CEramic REConstruction).
- Parallel confocal imaging uses laser and optical scanning to capture intraoral structures.
- Accordion fringe interferometry.
- Three‐dimensional in‐motion video.
Some digital scanners may require the application of a layer of powder to eliminate any inconsistencies caused by tooth and restorative surfaces dispersing light at an impulsive angle. The powder is commonly composed of titanium oxide or zirconium oxide with amorphous silica and aluminium hydroxide. This technique is termed dusting or accent frosting.
Analysis of Study Models
The diagnostic models retrieved either from dental impressions or digital scanners are analysed for occlusal symmetry and space. The symmetry of each dental arch is assessed carefully by the orthodontist. An assessment of space is made during this part of the examination. Crowding is classified as mild, moderate or severe. The categories are:
- mild: 1–2 mm of crowding per quadrant
- moderate: up to 4 mm of crowding per quadrant
- severe: more than 4 mm of crowding per quadrant.
Space analysis allows a better comparison of the degree of space available in the dental arches with the space necessary for alignment of the dentition. The space available is calculated by a linear measurement of all four segments. The total sum of the mesiodistal width of every tooth in the arch is needed, including an estimation of the size of permanent teeth that have not yet erupted. There is a space deficiency in the arch if the total sum of the space required is higher than the space available in the arch.
Radiographs
One of the most valuable diagnostic tools in orthodontics are radiographs. The two most important radiographs indicated for an accurate orthodontic diagnosis are orthopantomogram and lateral cephalometric radiograph.
Orthopantomogram
The orthopantomogram, also known as a dental panoramic tomogram, is a critical diagnostic tool, as it shows upper and lower arches with surrounding structures (Figure 3.34). This type of extraoral radiograph is commonly taken prior to treatment to aid in accurate diagnosis and at the end of treatment to ensure that the crown and root positioning are ideal. This radiograph must be examined in a systematic approach, working from one side to the other assessing:
- the position and size of the permanent and primary teeth
- tooth development (dental age)
- missing (hypodontia) and extra (hyperdontia) teeth
- alveolar bone density and height
- root inclinations
- impacted or ectopic teeth
- presence of pathology.

Figure 3.34 Example of an orthopantomogram.
Cephalometric Radiographs
The cephalostat is an x‐ray machine invented after the First World War by B. Holly Broadbent to take cephalometric radiographs (Mitchell, 2001). This type of radiograph allows an assessment of the growth, balance and harmony of the dentofacial structures in various planes. Indications of lateral cephalometric radiographs and the different analyses are discussed briefly in this section. The objective of this section is to create a better understanding of the anatomical landmarks on lateral cephalometric radiographs and how it can aid an orthodontic diagnosis. However, as mentioned previously orthodontic diagnosis is solely the scope of an orthodontist.
This type of radiograph is not indicated for every orthodontic patient; however, it provides a valuable baseline record, particularly in patients with severe overjet. Lateral cephalometric radiographs at various stages of treatment allow a better assessment of the progress of treatment over time. It is important to examine airway patency, root length and any pathology on the radiograph prior to analysis of the skeletal discrepancies. Anatomical points and planes are used in the analysis (Figures 3.35, 3.36, 3.37 and Table 3.3). The relationship between the anatomical landmarks and points aid a radiographic diagnosis of any discrepancies.

Figure 3.35 Some commonly known anatomical landmarks and points; the same anatomical points are not used for all analyses. A, A‐point (subspinale); ANS, anterior nasal spine; Ar, articular; B, B‐point (supramentale); Ba, basion; Co, condylion; G, glabella; Gn, gnathion; Go, gonion; Me, menton; N, nasion; Or, orbitale; PNS, posterior nasal spine; Po, porion; Pog, pogonion; Pr, prosthion.

Figure 3.36 Commonly used horizontal planes:

VIDEdental - Online dental courses


