Underweight
BMI less than 18.5
Normal weight
BMI 18.5–24.9
Over weight
BMI 25–29.9
Obesity
BMI equal to or greater than 30
Class I obesity
BMI 30–34.9
Class II obesity
BMI 35–39.9
Class III obesity
BMI equal to or greater than 40
Table 4.2
Waist circumference values for risk of chronic disease [10]
|
Men
|
Greater than 40 inches (102 cm)
|
|
Women
|
Greater than 35 inches (88 cm)
|
This chapter will address the associations between overweight, obesity and oral health, some environmental factors that may impact oral health and disease, and, suggest roles for OHCPs in weight status screening, provision of education relative to oral health, and appropriate and timely referral of patients to other health care providers for counseling.
Associations Between Overweight/Obesity and Oral Health
While obesity is of concern for overall systemic health and risk of chronic diseases, it is important for OHCPs to be concerned with the associations between obesity and dental and oral health. The possible role of oral bacteria as a contributor to obesity has been investigated via measures of salivary bacterial populations in overweight and normal weight subjects [11]. Composition of salivary bacterial changes in overweight subjects was evident when compared to healthy weight subjects; the results suggested that oral bacteria may contribute to development of obesity via several hypothetical propositions that need further investigation before stating definitive tenets. When 15,538 subjects in Sweden were assessed and followed from birth for 19 years to explore risk factors for caries development, the investigators found that overweight during pregnancy, as well as smoking habits, were risk factors for development of proximal caries in their offspring in their teen years [12]. Analysis of three cycles of National Health and Nutrition Examination Survey (NHANES) data collected between 2001 and 2006 noted a significant and positive association between obesity and timing of tooth eruption [12]. Teeth erupted earlier in obese children who on average had 1.44 more erupted teeth than non-obese children by 11 years of age [12]. The implications suggest that early and periodic oral health evaluation and preventive measures including dietary guidance may be needed as early as possible because, on average, obese children compared to non-obese children had significantly more erupted teeth for a more extended length of time exposure in the oral cavity, subsequently increasing risk for dental caries [13]. A meta-analysis of 14 studies examining the relationship between obesity and dental caries in children reported mixed and inconclusive results in general, but did indicate a significant relationship between obesity in children with permanent dentition and dental caries when parameters were standardized [14]. For example, Ziegler et al. noted an association between obesity and the sum total of bacterial cells (23 bacterial species derived from subgingival biofilm), in approximately threefold higher amounts, on average, in obese adolescents compared with normal weight controls, thus indicating a possible link between increases in oral microbiota indicative of caries risk and obesity in adolescents [15].
Suvan et al. conducted a systematic review to explore associations between overweight/obesity and periodontitis in adults [16]. The investigators concluded that there was an obesity-periodontal disease relationship mediated by chemicals (cyctokines and hormones resulting in low-grade inflammation and insulin resistance) secreted by adipose tissue and implicated in periodontal disease. This finding supports an association between BMI, overweight and obesity [16]. Dental plaque and infection were associated with a high BMI and obesity, independent of dietary patterns and insulin resistance, when investigators analyzed associations between number of teeth, periodontal status, and plaque index (15). A systematic review of 41 epidemiologic studies examining the evidence of an obesity-periodontal disease relationship supported by the National Institutes of Health suggested greater mean clinical attachment loss among obese individuals and an increase in periodontal disease with increasing BMI [16]. However, the magnitude of these associations remains unclear in cross-sectional studies due to confounders that have not been categorically defined. Thus, clinicians should continue to stress the importance of maintaining a healthy weight [17] for overall health and disease risk reduction.
Environmental Factors Related to Obesity and Oral Health
While there is controversial evidence regarding the associations between obesity and dental caries and periodontal disease [14, 18], there is an association between incidence of caries and increased sugar-sweetened beverage (SSB) intake and greater levels of inflammation, larger WC, and decreased HDL cholesterol in children age 3–11 years of age [19]. The authors reported associations between SSB and cardiometabolic markers in children, and suggest that prospective studies are warranted to determine if SSB may be one of the food and nutrition targets leading to deleterious systemic health effects. According to the CDC, SSBs include sodas, soft drinks, fruit drinks/ades, sports drinks, tea, coffee, energy drinks and milk drinks that contain caloric sweeteners or syrups [20]. These beverages are also a source of fermentable carbohydrates associated with caries risk. Similarly, Skinner et al. [21] reported significant associations between inflammatory markers and increasing weight in a cross-sectional study among children age 1–17 years old. While the identified association cannot be assumed to be causal, SSB may be independently associated with obesity, obesity-related chronic diseases, and dental caries. As part of health promotion and treatment efforts, OHCPs can advise patients on the impact of cariogenic foods and beverages, including SSB, on oral, nutritional and systemic health and healthful approaches to reducing risk of oral and systemic diseases and maximizing health.
Dietary patterns refer to food choices, portion control, and frequency of food intake that includes meals and snacks. Snacking among Western populations has resulted in a nearly doubled intake of energy-dense, low-nutrient-dense snack foods in the past two decades [22, 23]. In the US, potato chips, fried potatoes, whole milk and fruit drinks were identified as snack preferences among individuals with incomes below the poverty level; high-income groups prefer grain-based salty snacks, fruits, skim milk, soft drinks, coffee and tea [22]. Among 44,754 adults aged 19 years and older, the five most common sources of snack foods were desserts, salty snacks, sweetened beverages and fruit juices [23]. In either case, one can identify available fermentable carbohydrates in these foods that may contribute to caries risk. Caries development in children and adults has become significantly associated with the increasing role that snacking plays in dietary patterns [24]. Additionally, a prominent dietary trend has been the increasing frequency with which meals are consumed outside of the home in fast food establishments, restaurants, from street vendors, convenience stores and vending, all of which have implications for diet quality, obesity and chronic disease risk including oral diseases [25]. Both dietary food and beverage choices and patterns of consumption including frequent intake of energy dense low nutrient quality options can contribute to risk of overweight and obesity [24, 26].
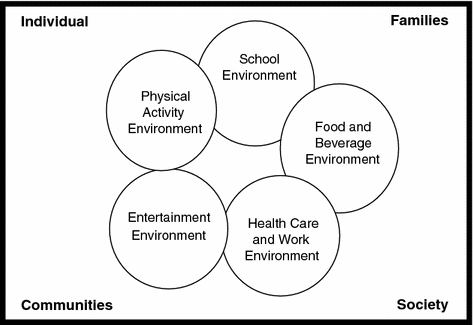
The environment includes both food and physical activity factors responsible for modulating behavioral decisions associated with the prevalence of overweight and obesity in both children and adults. Figure 4.1 illustrates a synergistic environmental model that identifies primary influences on individuals, families, communities, and societies that may impact access to and availability of a spectrum of food choices. Larson et al. surveyed 2,793 adolescents and concluded that infrequent family meals, a higher proportion of friends who were overweight, television viewing, and lower physical activity among female friends were associated with higher BMI z-scores [27]. Inequitable access to healthy foods is one mechanism by which socioeconomic factors influence the diet and health of a population where obesity may follow a social gradient [28]. As income declines, energy-dense, nutrient-poor foods provide daily calories at an affordable cost whereas nutrient-rich foods and high-quality diets may cost more and be consumed by more affluent groups [28]. School children in rural areas have been reported to have a higher prevalence of obesity as compared to children in urban schools due to socioeconomic distress where parents are single, possibly unemployed and have lower educational attainment [29]. Associations between overweight and obesity and longer work hours and shift hours have been identified among adults. Much of this has been attributed to the environmental shifts in employment from agriculture and physical labor to automated, labor-saving environments and to after-work hours spent on social networks [30].
Interprofessional Practice
Obesity is a disease that is prevalent globally. This disease is associated with increased risk for several chronic diseases with oral health implications. Although there is no causal evidence of the impact of obesity on oral disease, studies cited throughout this chapter speak to associations between obesity and oral diseases. Collaboration across disciplines including networking with physicians, pediatricians, and registered dietitians (RD) to foster health promotion and disease prevention and intervention through weight screening, education and referral may help reduce the prevalence of obesity [31, 32]. The American Dental Association’s “Call to Action for Oral Health” aims to reduce oral health disparities while “advocating for healthier lives, through guidelines on healthy nutrition…” and that to make an impact OHCPs must identify the needs of the patient populations and remove barriers that may impede action [33, p. 96]. This section addresses approaches for OHCPs in weight screening, education and referral. Although weight loss counseling is outside of the scope of practice for OHCPs, awareness with scientifically sound approaches may be valuable in directing patients for care. Weight management resources and strategies are presented in an effort to familiarize OHCPs with recommended approaches to patient care in the context of interdisciplinary collaboration to reduce obesity prevalence.
Role of OHCPs in Weight Screening
Oral health affects overall health and wellness [34]; OHCPs have a role like other health professionals in screening patients for overweight and obesity, providing basic health promotion and disease prevention education and referring accordingly to other health professionals [32, 35, 36].
All health care providers are encouraged to serve as role models and advocate for health. The Patient Promise is an initiative aimed at health professionals to encourage them to partner with patients and clients in adapting healthy lifestyle examples. It encourages health professionals to “lead by example” by practicing healthy behaviors for diet, physical activity and stress management to reduce risk of and manage chronic diseases including obesity, CVD, hypertension and diabetes (http://www.thepatientpromise.org/index.html). Students and clinicians can adopt the Patient Promise to make a commitment to their patients to practice the same healthy behaviors that they espouse (http://www.thepatientpromise.org/index.html).
Awareness of the associations between overweight/obesity and systemic and oral health, can prepare OHCPs to screen and provide pertinent education on the role of diet and oral health and disease, and as necessary provide referrals to RD for weight management counseling, or other health care providers for chronic disease management.
Screening for Overweight and Obesity
Knowledge and confidence have been identified as barriers to screening and counseling on dietary intake and obesity [37, 38] and diabetes and oral health [39] among OHCPs. OHCPs are increasingly adopting screening practices for chronic diseases including diabetes and CVD [35, 36, 40]. They may also recognize their role in weight screening and questioning patients about their use of weight control diets, dietary intake patterns, and dietary supplements in the context of the dental office as part of routine care for patients of all ages [41, 42]. Since overweight and obesity increase risk and associated comorbid conditions of both CVD and diabetes hence the integration of weight screening would expand their screening practices in a comprehensive manner. Both future and currently practicing OHCPs may benefit by continuing professional education and accessing resources to confidently screen for overweight and obesity and provide referrals to their patients for best possible outcomes. Chapters 11 and 19 on diabetes and approaches to oral nutrition health risk assessment respectively provide additional insight into screening strategies.
However, while excess body weight carries social stigma in the US [43], OHCPs and other healthcare providers may feel uncomfortable and uncertain in their approach to screen and discuss the topic with their patients and the caregivers of pediatric patients, especially if the provider is overweight or obese himself/herself [44, 45]. The Weight Control Information Network recommends addressing the patient’s primary concern first and then having an open discussion regarding weight control, and encourages using terms such as “excess weight” or reference to BMI, rather than using the terms “overweight” and “obese” (Table 4.3) [46]. Volger et al’s research findings further emphasized avoiding undesirable terms such as “heaviness”, “fatness” and “large size” [47]. Tseng et al. [31] offer practical guidelines for addressing obesity in the dental practice, and they emphasize that the context of the discussion should relate obesity to oral health and disease. The messages should be delivered in a culturally appropriate manner and sensitive to the wellbeing of the patient or caregiver. Explaining the rationale behind recommendations may increase the likelihood of attaining change.
Table 4.3
Weight screening, sample questions, and resources for clinicians [46]
|
Purpose
|
Question/action
|
Resources/outcome
|
|---|---|---|
|
Screen for overweight and obesity by measuring height and weight. If a scale (to measure weight) and stadiometer (to measure height) are not available, screen based on patient recall
|
Calculate BMI (note different tools for adults and children/adolescents)
|
http://www.cdc.gov/healthyweight/assessing/bmi/index.html or download the smartphone app
|
|
Start the discussion in a respectful, culturally-sensitive manner; be aware of body language of both the clinician and patient
|
“Ms. Brown, your BMI is above the healthy range. Excess weight could increase your risk for some health problems. Would you mind if we talked about it?”
|
If the patient is receptive to the conversation then continue to ask about dietary intake and physical activity. If the patient is resistant to a discussion then emphasize the importance of weight management in context of reduced risk of chronic disease and impact on oral health
|
|
Find out what a patient’s eating habits are like on a typical day
|
“What kinds of foods do you eat on a typical day?”
“What does ‘healthy eating’ mean to you?”
|
www.choosemyplate.gov offers resources for weight management that a OHCPs and patients may access and use http://myplate.gov/weight-management-calories/weight-management.html
|
|
Find out what a patient’s physical activity habits are like in a typical day/week
|
“How much time do you spend sitting down each day?”
“Do you know how much physical activity you should do each week to stay healthy?”
|
Aim for 150 minutes of moderate intensity physical activity a week. http://myplate.gov/weight-management-calories/weight-management/better-choices/increase-physical-activity.html
|
|
If a patient is ready to adopt a healthier lifestyle, refer them to a registered dietitian for weight management counseling or to a primary care clinician with expertise in treating patients with overweight and obesity
|
Refer to www.eatright.org
|
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses