Nutrition contributes to many of the leading causes of death in the United States, yet less than one-third of dental students feel competent to discuss the relationship of nutrition and systemic disease with their patients. The American Dental Association policy statements acknowledge a need for health professionals and organizations to provide continuing education to professionals and counseling to patients to combat the growing problems of overweight and obesity. Dentists can play a major role in educating patients to adopt a healthier lifestyle, including nutrition and physical activity recommendations. An understanding of the complexity of behavior change may enhance the dentist’s ability to assist their patients in making desired changes.
- •
Nutrition contributes to at least 6 of the 10 leading causes of death in the United States, yet less than one-third of dental students feel competent to discuss the relationship of nutrition and systemic disease with their patients.
- •
The American Dental Association policy statements acknowledge a need for health professionals and organizations to provide continuing education to professionals and counseling to patients to combat the growing problems of overweight and obesity. Dentists can play a major role in educating patients to adopt a healthier lifestyle, including nutrition and physical activity recommendations. In addition, an understanding of the complexity of behavior change may enhance the dentist’s ability to assist their patients in making desired changes.
- •
The interaction of general health and oral health is seen most clearly in the interaction between diabetes and periodontal health, each potentially affecting the other in a downward spiral of worsening general health.
- •
Because the current nutrition and activity behaviors of most Americans is far from optimal, much can be gained as dentists develop a better understanding of the difficulties of sustained behavior change and become proficient in counseling approaches that lead to improved oral health for patients.
Introduction
Nutrition contributes to at least 6 of the 10 leading causes of death in the United States, and less than one-third of dental students feel competent to speak about nutrition with their patients. Cardiovascular disease is the leading cause of death in the United States, accounting for one in three deaths. The American Heart Association has identified seven modifiable health parameters known to reduce the risk of cardiovascular disease, yet only about 2% of adults in the United States engage in the lifestyle behaviors that allow possession of all seven. These health parameters include not smoking; being physically active; having normal blood pressure, blood glucose, total cholesterol levels, and normal weight; and eating a healthy diet. Other articles in this issue deal with smoking, blood pressure, obesity, and diabetes; this article provides the scientific bases of key nutrition and physical activity recommendations. Most of the American Heart Association recommendations are currently not being met, and substantial behavior changes are required to help patients reach desired goals. This represents an important opportunity for dentists to play a role in improving their patients overall health. A brief section describes some of the underlying reasons that patients do not comply with recommendations, even when it is in their own best interests to do so. We also include guidelines in the use of active listening and motivational interviewing (MI), where the practitioner collaborates with the patient to make desired lifestyle changes.
Nutrition and oral health
In young children and adolescents, dentists are very aware of the outcome of constant local exposure of teeth to free sugars, sticky refined carbohydrates, and highly processed foods. Despite 50 years of water fluoridation and decades of nutrition advice, pediatric dentists in the United States are alarmed by caries increase in very young children. Young children are routinely admitted to hospital operating rooms in the United States with the need for general anesthesia to treat multiple decayed and infected teeth. Parents seem disconnected from the relationship of a food environment filled with sweets, constant sipping of fruit juice and sugar-sweetened beverages (SSBs), choosing bottled water over fluoridated tap water, and their lack of reinforcement of brushing of teeth, contributing to their child’s dental caries.
Developing countries adopting the lifestyle and dietary patterns of Western countries have increased caries incidence, with few healthcare resources to treat the pathology. The evolving global food environment is a worldwide public health hazard, replete with a highly processed, inexpensive, ubiquitous supply of high caloric density and low nutrient density foods. The dismal Western dietary pattern, illustrated in Table 1 from the 2010 dietary guidelines on current US consumption patterns, coupled with the sedentary habits of most of the population, has contributed to 66% of adults being overweight and 35.7% of US adults being obese in 2010. Obesity contributes to symptoms of metabolic syndrome with frequent clustering of insulin resistance, ectopic hepatic fat, increased visceral fat, and chronic low-grade inflammation called “metaflammation.” Notably, metaflammation is common to all inflammatory diseases including atherosclerosis, rheumatoid arthritis, inflammatory bowel disease, asthma, diabetes, and periodontitis.
| Rank | Overall, Ages 2+ Years (mean kcal/d; total daily calories = 2157) | Children and Adolescents, Ages 2–18 Years (mean kcal/d; total daily calories = 2027) | Adults and Older Adults, Ages 19+ Years (mean kcal/d; total daily calories = 2199) |
|---|---|---|---|
| 1 | Grain-based desserts b (138 kcal) | Grain-based desserts (138 kcal) | Grain-based desserts (138 kcal) |
| 2 | Yeast breads c (129 kcal) | Pizza (136 kcal) | Yeast breads (134 kcal) |
| 3 | Chicken and chicken mixed dishes d (121 kcal) | Soda/energy/sports drinks (118 kcal) | Chicken and chicken mixed dishes (123 kcal) |
| 4 | Soda/energy/sports drinks e (114 kcal) | Yeast breads (114 kcal) | Soda/energy/sports drinks (112 kcal) |
| 5 | Pizza (98 kcal) | Chicken and chicken mixed dishes (113 kcal) | Alcoholic beverages (106 kcal) |
| 6 | Alcoholic beverages (82 kcal) | Pasta and pasta dishes (91 kcal) | Pizza (86 kcal) |
| 7 | Pasta and pasta dishes f (81 kcal) | Reduced-fat milk (86 kcal) | Tortillas, burritos, tacos (85 kcal) |
| 8 | Tortillas, burritos, tacos g (80 kcal) | Dairy desserts (76 kcal) | Pasta and pasta dishes (78 kcal) |
| 9 | Beef and beef mixed dishes h (64 kcal) | Potato/corn/other chips (70 kcal) | Beef and beef mixed dishes (71 kcal) |
| 10 | Dairy desserts i (62 kcal) | Ready-to-eat cereals (65 kcal) | Dairy desserts (58 kcal) |
| 11 | Potato/corn/other chips (56 kcal) | Tortillas, burritos, tacos (63 kcal) | Burgers (53 kcal) |
| 12 | Burgers (53 kcal) | Whole milk (60 kcal) | Regular cheese (51 kcal) |
| 13 | Reduced-fat milk (51 kcal) | Candy (56 kcal) | Potato/corn/other chips (51 kcal) |
| 14 | Regular cheese (49 kcal) | Fruit drinks (55 kcal) | Sausage, franks, bacon, and ribs (49 kcal) |
| 15 | Ready-to-eat cereals (49 kcal) | Burgers (55 kcal) | Nuts/seeds and nut/seed mixed dishes (47 kcal) |
| 16 | Sausage, franks, bacon, and ribs (49 kcal) | Fried white potatoes (52 kcal) | Fried white potatoes (46 kcal) |
| 17 | Fried white potatoes (48 kcal) | Sausage, franks, bacon, and ribs (47 kcal) | Ready-to-eat cereals (44 kcal) |
| 18 | Candy (47 kcal) | Regular cheese (43 kcal) | Candy (44 kcal) |
| 19 | Nuts/seeds and nut/seed mixed dishes j (42 kcal) | Beef and beef mixed dishes (43 kcal) | Eggs and egg mixed dishes (42 kcal) |
| 20 | Eggs and egg mixed dishes k (39 kcal) | 100% fruit juice, not orange/grapefruit (35 kcal) | Rice and rice mixed dishes (41 kcal) |
| 21 | Rice and rice mixed dishes l (36 kcal) | Eggs and egg mixed dishes (30 kcal) | Reduced-fat milk (39 kcal) |
| 22 | Fruit drinks m (36 kcal) | Pancakes, waffles, and French toast (29 kcal) | Quick breads (36 kcal) |
| 23 | Whole milk (33 kcal) | Crackers (28 kcal) | Other fish and fish mixed dishes n (30 kcal) |
| 24 | Quick breads o (32 kcal) | Nuts/seeds and nut/seed mixed dishes (27 kcal) | Fruit drinks (29 kcal) |
| 25 | Cold cuts (27 kcal) | Cold cuts (24 kcal) | Salad dressing (29 kcal) |
a Data are drawn from analyses of usual dietary intakes conducted by the National Cancer Institute. Foods and beverages consumed were divided into 97 categories and ranked according to calorie contribution to the diet. Table shows each food category and its mean calorie contribution for each age group. Additional information on calorie contribution by age, gender, and race/ethnicity is available at http://riskfactor.cancer.gov/diet/foodsources/ .
b Includes cake, cookies, pie cobbler, sweet rolls pastries, and donuts.
c Includes white bread or rolls, mixed-grain bread, flavored bread, whole-wheat bread, and bagels.
d Includes fried or baked chicken parts and chicken strips/patties, chicken stir-fries, chicken casseroles, chicken sandwiches, chicken salads, stewed chicken, and other chicken mixed dishes.
e Sodas, energy drinks, sports drinks, and sweetened bottled water including vitamin water.
f Includes macaroni and cheese, spaghetti, other pasta with or without sauces, filled pasta (eg, lasagna and ravioli), and noodles.
g Also includes nachos, quesadillas, and other Mexican mixed dishes.
h Includes steak, meatloaf, beef with noodles, and beef stew.
i Includes ice cream, frozen yogurt, sherbet, milk shakes, and pudding.
j Includes peanut butter, peanuts, and mixed nuts.
k Includes scrambled eggs, omelets, fried eggs, egg breakfast sandwiches/biscuits, boiled and poached eggs, egg salad, deviled eggs, quiche, and egg substitutes.
l Includes white rice, Spanish rice, and fried rice.
m Includes fruit-flavored drinks, fruit juice drinks, and fruit punch.
The dentist may be less aware of how lifestyle interventions beyond smoking cessation, such as physical activity and diet, mitigate chronic illness. The same child presenting with rampant dental caries who is overweight or obese becomes an adolescent at risk for nonalcoholic fatty liver disease, atherosclerotic cardiovascular disease, and type 2 diabetes mellitus.
The American Dental Association (ADA) policy statements acknowledge a need for health professionals and organizations to provide continuing education to professionals and counseling to patients to combat the growing problems of overweight and obesity. Information defining the relationships between oral health and nutrition, and systemic and oral health are to be incorporated into documents and educational materials.
The 2010 dietary guidelines provide a focal point of what every dentist should know to meet ADA policy guidelines and global public health challenges of oral and systemic health interactions. The 2010 Guidelines center on unprocessed whole foods that are nutrient dense but energy poor per kilocalorie consumed. This eating style features minimally processed foods and avoids manufactured food products. It emphasizes whole grains, fruits, vegetables, and foods high in long-chain omega 3 polyunsaturated fat. It stresses reducing saturated fats, moderate alcohol intake, decreasing SSBs, reducing refined grains, and avoidance of trans fat. The whole grains, fruits, and vegetables provide fiber and promote satiety. Protein sources and consumption are adequate in the United States and there is a recommendation to seek lean sources of protein and add vegetable protein sources, such as nuts and legumes.
Ludwig emphasizes that traditional diets, such as the “Mediterranean diet,” incorporate most of the protective aspects of the guidelines, such as minimal processing with little refined carbohydrates, and have low added sugar content. Traditional diets from such countries as Japan and China exemplify the dietary guidelines with frequency and variety of fruits and vegetables as the cornerstones of healthy food choices. They are easy to follow for those ethnic groups accustomed to them.
In comparison, the food consumed in the Western diet, built on fast food, partially hydrogenated added fats, refined carbohydrates, and added sugars has high caloric density with dismal nutritional value. The number one food category is grain-based desserts, which are refined grain foods with added fats, including cakes, cookies, pie, cobbler, sweet rolls, pastries, and donuts (see Table 1 ).
The most relevant points in the guidelines for dentists include:
- •
Increase intake of whole grains, vegetables, and fruits : A diet high in whole grains, fruits, and vegetables has a great deal of volume and provides satiety. This contributes to what is described in the guidelines as “moderate” scientific evidence that adults who eat more whole grains, particularly those higher in dietary fiber, have a lower body weight compared with adults who eat very few whole grains.
- •
Reduce intake of SSBs : This recommendation stresses that SSBs provide calories and little nutrients, displace foods of nutrient density, and should be considered only after nutrient needs have been fulfilled but calorie limits have not been met. Given the universal availability of these beverages, emphasis that constant exposure to these liquids increases caries risk, and the calories increase obesity risk, should be part of preventive care.
- •
Monitor intake of 100% fruit juice for children and adolescents, especially those who are overweight or obese : Natural sugars are as cariogenic as free or added sugars. Patients may have difficulty distinguishing 100% real fruit juice from juice drink. Food manufacturers place juice content in small print on the back of the nutrition label. Front labels often show the product provides 100% of a nutrient, such as “provides 100% Daily Value for vitamin C” in larger print. This is confusing for patients with limited English language skills and makes a wise purchase more challenging. Unless the package also states it is “100% juice,” it is not 100% juice. Sweetened juice products are considerably cheaper but are SSBs rather than fruit juice, and should be avoided.
- •
Monitor calorie intake from alcoholic beverages for adults : Moderate consumption of alcohol, thought to be cardioprotective, is defined as one glass of wine per day (5 oz) for women and two glasses (10 oz) for men. Greater amounts than this are associated with weight gain.
- •
Milk and milk products : Dentists are familiar with recommendations for calcium and vitamin D intakes for healthy teeth, periodontium, and bones, and recommend milk, cheese, and yogurt to patients as sources of calcium. However, evidence in adults and children indicates that consumption of milk and milk products does not play a special role in weight management. Added fats, sugars, and excessive portion sizes remain embedded in the Western diet and patients should be mindful of portion size and fat content when choosing calcium-rich foods.
The Dietary Approaches to Stop Hypertension (DASH) Diet and the Therapeutic Lifestyle Changes (TLC) diets are specialized, but in many ways similar, to the 2010 guidelines. DASH is formulated to reduce hypertension, and TLC focuses on reducing low-density lipoprotein to ease metabolic syndrome and coronary heart disease. A summary and description of DASH and TLC are found in Table 2 and Table 3 .
| Fruits and vegetables | 4.5 cups per day |
| Fiber-rich whole grains | 3 1-oz-equivalent servings per day |
| Sodium | <1500 mg per day |
| Sugar sweetened beverages | <450 kcal (36 oz) per wk |
| Supplemented with: | |
| Nuts/legumes/seeds | >4 1-oz servings per wk |
| Saturated fat | <7% of total energy intake |
| Processed meats | None or <2 servings per wk |
| Limits | |
| Saturated fat | <7% of calories |
| Total fat | <25%–35% of daily calories from total fat (including saturated fat calories) |
| Other low-density lipoprotein lowering strategies: | |
| 2 g per day of plant stanols or sterols | |
| 10–25 g per day of soluble fiber | |
| Consume enough calories to reach or maintain a healthy weight | |
| 30 min of a moderate-intensity physical activity, such as brisk walking, on most and preferably all days of the wk |
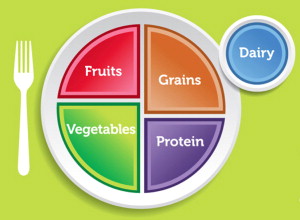
MyPlate.gov ( Fig. 1 ) and My Plate Planner ( Fig. 2 ) are visual tools that reflect the message of what consumers should place on their plates. A 9-in plate replaces an 11-in plate to encourage smaller portion selection and promotes increasing the amount, and frequency, of fruit and vegetable consumption. My Plate Planner, from the New York City Department of Health, may be more effective in encouraging compliance because a full half of each lunch and dinner plate is filled with low starch (low glycemic load) and low caloric density vegetables. The average US consumer adopting this practice would greatly improve their consumption patterns. No whole fruit or a single vegetable, except fried potatoes, are noted in the top 25 foods most frequently consumed in the United States from the 2005 to 2006 NHANES Data (see Table 1 ). Smaller areas, one-quarter of the plate for protein and one-quarter of the plate for carbohydrate, comprise the other half of plate contents.

Caution, Controversy, and Lack of Consensus
There are some points of concern and disagreement.
- •
The DASH and TLC diets : These diets have recommended fruit servings of four to five 4-oz servings (DASH) and four 4-oz servings (TLC), respectively, of fruit or fruit juice, with several such servings allotted per day. A total of 20 oz (DASH) or 16 oz (TLC) of fruit juice could be consumed each day while still complying with guidelines. Dietary guidelines suggest whole fruit as better choices than fruit juice for those who are caries prone, diabetic, or obese because they provide more fiber and more satiety. Those choosing fruit juices instead of whole fruit on the DASH and TLC diet could be consuming 2 to 2.5 8-oz servings per day. Basch and coworkers caution that not more than one fruit serving should be fruit juice and that juice quality differs in nutrient density. Constant between-meal sipping of juice is not one of the “five-a-day” recommendations. Using the Nurses’ Health Study data, Bazzano and coworkers discovered that with each increase of one serving per day of fruit juice (again defined as an 8-oz serving), the multivariate-adjusted relative risk of diabetes was 1.18.
- •
De novo lipogenesis : Frequent SSB consumption is thought to lead to high dietary glycemic load, inflammation, insulin resistance, and impaired pancreatic β-cell function. Fructose from any sugar or high fructose corn syrup may promote the accumulation of visceral fat and ectopic hepatic fat deposition because of increased hepatic de novo lipogenesis (de novo lipogenesis [DNL]).
- •
Uric acid pathway : The association of SSBs and elevated blood pressure is consistent with the hypothesized effect of the uric acid pathway. The uric acid pathway contributes to raised serum uric acid, which may influence blood pressure by reducing levels of nitric oxide, a potent vasodilator. SSBs are the fourth most common source of calories in the United States and a clinician may find an immigrant adopting a Western diet with new complaints of abdominal/visceral fat, even in the absence of a change in weight. The clinician may see an increase in blood pressure over successive routine examinations. Asian populations are considered obese at lower body mass indexes than whites, so initially, their risk may not be apparent to the clinician. Nakagawa and coworkers provide a thorough review of the mechanisms underlying the physiologic changes leading to these elevations in blood pressure.
- •
Human studies : Human studies have pointed to differences in visceral fat accumulation when 25% of calories were provided with either glucose- or fructose-sweetened beverages. In 32 obese men visceral fat increased by 14% in the fructose-consuming group compared with about 5% in the control group, with no significant change in body weight or subcutaneous fat. De novo lipogenesis, a liver-mediated path of fructose metabolism, was increased and postprandial triglycerides increased, particularly at night. In one small 10-week prospective study in humans, consuming either fructose or glucose, fasting plasma glucose and insulin levels increased and insulin sensitivity decreased in subjects consuming fructose, but not in those consuming glucose. The fructose consumption again increased DNL. Clinicians should be aware that visceral fat is metabolically active and intertwined in metabolic perturbance and metaflammation. Fructose is hypothesized to uniquely increase DNL, promote dyslipidemia, decrease insulin sensitivity, and increases visceral fat in adults who are overweight or obese.
- •
Satiety : In some studies, very specific macronutrient choices contributed to weight gain or weight loss. Mozaffarian and colleagues argue: “Strong positive associations with weight change were seen for starches, refined grains, and processed foods. These findings are consistent with results in limited short-term trials: consumption of starches and refined grains may be less satiating, increasing subsequent hunger signals, and total caloric intake, as compared with equivalent numbers of calories obtained from less processed, higher-fiber foods that also contain healthy fats and protein.”
Summary and Future Directions Regarding Nutrition and Oral Health
Historically, individual foods have not been linked to periodontal disease in the same manner that sugars act locally to affect caries. However, periodontal disease management is bidirectional : metabolic syndrome, obesity, and type 2 diabetes mellitus exacerbate periodontal disease severity, and periodontal conditions contribute to and worsen systemic illness. Taylor and Susanto and coworkers direct all clinicians to their crucial role in improving chronic disease biomarkers, such as blood pressure, fasting blood glucose, and triglycerides, through the aforementioned changes in nutrition. This is an urgently needed step toward mitigation of the pandemic of chronic debilitating disease across the globe. The next section describes promotion of physical activity to enhance primary and secondary prevention of disease.
Nutrition and oral health
In young children and adolescents, dentists are very aware of the outcome of constant local exposure of teeth to free sugars, sticky refined carbohydrates, and highly processed foods. Despite 50 years of water fluoridation and decades of nutrition advice, pediatric dentists in the United States are alarmed by caries increase in very young children. Young children are routinely admitted to hospital operating rooms in the United States with the need for general anesthesia to treat multiple decayed and infected teeth. Parents seem disconnected from the relationship of a food environment filled with sweets, constant sipping of fruit juice and sugar-sweetened beverages (SSBs), choosing bottled water over fluoridated tap water, and their lack of reinforcement of brushing of teeth, contributing to their child’s dental caries.
Developing countries adopting the lifestyle and dietary patterns of Western countries have increased caries incidence, with few healthcare resources to treat the pathology. The evolving global food environment is a worldwide public health hazard, replete with a highly processed, inexpensive, ubiquitous supply of high caloric density and low nutrient density foods. The dismal Western dietary pattern, illustrated in Table 1 from the 2010 dietary guidelines on current US consumption patterns, coupled with the sedentary habits of most of the population, has contributed to 66% of adults being overweight and 35.7% of US adults being obese in 2010. Obesity contributes to symptoms of metabolic syndrome with frequent clustering of insulin resistance, ectopic hepatic fat, increased visceral fat, and chronic low-grade inflammation called “metaflammation.” Notably, metaflammation is common to all inflammatory diseases including atherosclerosis, rheumatoid arthritis, inflammatory bowel disease, asthma, diabetes, and periodontitis.
| Rank | Overall, Ages 2+ Years (mean kcal/d; total daily calories = 2157) | Children and Adolescents, Ages 2–18 Years (mean kcal/d; total daily calories = 2027) | Adults and Older Adults, Ages 19+ Years (mean kcal/d; total daily calories = 2199) |
|---|---|---|---|
| 1 | Grain-based desserts b (138 kcal) | Grain-based desserts (138 kcal) | Grain-based desserts (138 kcal) |
| 2 | Yeast breads c (129 kcal) | Pizza (136 kcal) | Yeast breads (134 kcal) |
| 3 | Chicken and chicken mixed dishes d (121 kcal) | Soda/energy/sports drinks (118 kcal) | Chicken and chicken mixed dishes (123 kcal) |
| 4 | Soda/energy/sports drinks e (114 kcal) | Yeast breads (114 kcal) | Soda/energy/sports drinks (112 kcal) |
| 5 | Pizza (98 kcal) | Chicken and chicken mixed dishes (113 kcal) | Alcoholic beverages (106 kcal) |
| 6 | Alcoholic beverages (82 kcal) | Pasta and pasta dishes (91 kcal) | Pizza (86 kcal) |
| 7 | Pasta and pasta dishes f (81 kcal) | Reduced-fat milk (86 kcal) | Tortillas, burritos, tacos (85 kcal) |
| 8 | Tortillas, burritos, tacos g (80 kcal) | Dairy desserts (76 kcal) | Pasta and pasta dishes (78 kcal) |
| 9 | Beef and beef mixed dishes h (64 kcal) | Potato/corn/other chips (70 kcal) | Beef and beef mixed dishes (71 kcal) |
| 10 | Dairy desserts i (62 kcal) | Ready-to-eat cereals (65 kcal) | Dairy desserts (58 kcal) |
| 11 | Potato/corn/other chips (56 kcal) | Tortillas, burritos, tacos (63 kcal) | Burgers (53 kcal) |
| 12 | Burgers (53 kcal) | Whole milk (60 kcal) | Regular cheese (51 kcal) |
| 13 | Reduced-fat milk (51 kcal) | Candy (56 kcal) | Potato/corn/other chips (51 kcal) |
| 14 | Regular cheese (49 kcal) | Fruit drinks (55 kcal) | Sausage, franks, bacon, and ribs (49 kcal) |
| 15 | Ready-to-eat cereals (49 kcal) | Burgers (55 kcal) | Nuts/seeds and nut/seed mixed dishes (47 kcal) |
| 16 | Sausage, franks, bacon, and ribs (49 kcal) | Fried white potatoes (52 kcal) | Fried white potatoes (46 kcal) |
| 17 | Fried white potatoes (48 kcal) | Sausage, franks, bacon, and ribs (47 kcal) | Ready-to-eat cereals (44 kcal) |
| 18 | Candy (47 kcal) | Regular cheese (43 kcal) | Candy (44 kcal) |
| 19 | Nuts/seeds and nut/seed mixed dishes j (42 kcal) | Beef and beef mixed dishes (43 kcal) | Eggs and egg mixed dishes (42 kcal) |
| 20 | Eggs and egg mixed dishes k (39 kcal) | 100% fruit juice, not orange/grapefruit (35 kcal) | Rice and rice mixed dishes (41 kcal) |
| 21 | Rice and rice mixed dishes l (36 kcal) | Eggs and egg mixed dishes (30 kcal) | Reduced-fat milk (39 kcal) |
| 22 | Fruit drinks m (36 kcal) | Pancakes, waffles, and French toast (29 kcal) | Quick breads (36 kcal) |
| 23 | Whole milk (33 kcal) | Crackers (28 kcal) | Other fish and fish mixed dishes n (30 kcal) |
| 24 | Quick breads o (32 kcal) | Nuts/seeds and nut/seed mixed dishes (27 kcal) | Fruit drinks (29 kcal) |
| 25 | Cold cuts (27 kcal) | Cold cuts (24 kcal) | Salad dressing (29 kcal) |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


