Key points
- •
Upper facial rejuvenation is an important component of complete facial rejuvenation and has an overall low complication rate.
- •
Most complications of upper facial procedures are avoided with proper preoperative work-up, patient selection, diagnoses, and fundamental knowledge of relevant anatomy.
- •
With the advances in brow procedures, in particular the endoscopic forehead and brow lift, a more youthful appearance is achieved with avoiding an open procedure with unsightly scars.
Introduction
Patients who seek upper facial rejuvenation often present with complaints of excessive wrinkling, tired-appearing eyes, and excess eyelid skin. The goal of the cosmetic surgeon should be to restore the aesthetic balance and a youthful three-dimensional facial topography. The cosmetic surgeon should take time to discuss the patient’s goals and realistic outcomes including complications that may arise from the planned procedures. The conversation should include aging changes that occur in the upper facial region caused by
- •
Sun damage
- •
Gravity
- •
Bone resorption
- •
Decreased tissue elasticity
- •
Facial volume loss (deflation)
- •
Genetics
The facial aging process begins with surface and subsurface structural changes in multiple facial tissue layers, including skin, fat, muscle, and bone. These facial tissue layers age interdependently and contribute to the overall facial appearance. The skin undergoes several changes including thinning, dryness, loss of elasticity, reduction in collagen, and increased likeliness to wrinkle or sag. The collagen loss is a key factor and decreases the skin’s ability to retain elasticity (elastin) and moisture (hyaluronic acid). The aging face has redistribution, accumulation, and atrophy of fat that leads to an overall facial volume loss. There is also loss of craniofacial bone with age and without this structural support there are perceptible changes in the overlying layers.
Upper facial rejuvenation procedures rank at the top of facial cosmetics with more than 206,000 blepharoplasties performed in 2014 (number two of all facial cosmetic surgical procedures) and 42,000 forehead lifts in 2014 (number five of all facial cosmetic surgical procedures). The top minimally invasive cosmetic procedures for 2014 were botulinum toxin type A (6.7 million) and soft tissue fillers (2.3 million). A thorough preoperative evaluation, knowledge of pertinent anatomy, and meticulous surgical planning allow cosmetic surgeons to prevent and understand the management of complications ( Fig. 1 ).
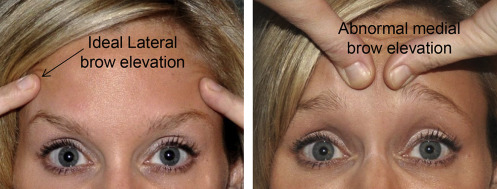
Introduction
Patients who seek upper facial rejuvenation often present with complaints of excessive wrinkling, tired-appearing eyes, and excess eyelid skin. The goal of the cosmetic surgeon should be to restore the aesthetic balance and a youthful three-dimensional facial topography. The cosmetic surgeon should take time to discuss the patient’s goals and realistic outcomes including complications that may arise from the planned procedures. The conversation should include aging changes that occur in the upper facial region caused by
- •
Sun damage
- •
Gravity
- •
Bone resorption
- •
Decreased tissue elasticity
- •
Facial volume loss (deflation)
- •
Genetics
The facial aging process begins with surface and subsurface structural changes in multiple facial tissue layers, including skin, fat, muscle, and bone. These facial tissue layers age interdependently and contribute to the overall facial appearance. The skin undergoes several changes including thinning, dryness, loss of elasticity, reduction in collagen, and increased likeliness to wrinkle or sag. The collagen loss is a key factor and decreases the skin’s ability to retain elasticity (elastin) and moisture (hyaluronic acid). The aging face has redistribution, accumulation, and atrophy of fat that leads to an overall facial volume loss. There is also loss of craniofacial bone with age and without this structural support there are perceptible changes in the overlying layers.
Upper facial rejuvenation procedures rank at the top of facial cosmetics with more than 206,000 blepharoplasties performed in 2014 (number two of all facial cosmetic surgical procedures) and 42,000 forehead lifts in 2014 (number five of all facial cosmetic surgical procedures). The top minimally invasive cosmetic procedures for 2014 were botulinum toxin type A (6.7 million) and soft tissue fillers (2.3 million). A thorough preoperative evaluation, knowledge of pertinent anatomy, and meticulous surgical planning allow cosmetic surgeons to prevent and understand the management of complications ( Fig. 1 ).
Preoperative evaluation
Preoperative risk assessment should take into account the patient’s overall health status (American Society of Anesthesiologists [ASA] physical status); fortunately most patient’s presenting for facial cosmetic surgery are healthy (ASA I) or have a mild, controlled systemic disease (ASA II). Preexisting cardiovascular disease, particularly systemic hypertension, should be well controlled because it may predispose the patient to hematoma formation. Facial cosmetic surgical procedures carry a low (<1%) risk of major cardiac complications, such as cardiac death or nonfatal myocardial infarction. Preoperative 12-lead electrocardiogram and routine preoperative laboratory testing should be performed as indicated. Pulmonary status of patients with chronic obstructive pulmonary disease should be evaluated and optimized to decrease the chance of postoperative pulmonary complications. In particular, cigarette smoking is associated with a 12- to 20-fold increase in flap slough and excessive coughing postoperatively caused by abnormal airway reactivity can increase the risk of postoperative bleeding. Patients should be instructed to discontinue smoking and nicotine products for a minimum 3 weeks before and after surgery. Patients with diabetes mellitus and rheumatologic disease should be medically optimized before surgery because they are prone to bruising, infection, and delayed healing ( Fig. 2 ). A personal or family history of blood dyscrasias should be noted. The use of the following should be stopped at least 2 weeks before surgery to avoid the risk of excessive bleeding:
- •
Nonsteroidal anti-inflammatory drugs
- •
Aspirin
- •
Fish oil
- •
Herbal supplements, such as ginkgo, Echinacea , and St. John’s wort
- •
Certain vitamins (eg, vitamin E)
Patients with obesity and history of a difficult airway should be evaluated for sleep-disordered breathing. Obstructive sleep apnea is screened for using a simple STOP-BANG questionnaire.
Complications in browlift
Procedures to lift the ptotic brow were initially described by Hunt in 1926 and later in 1930, Passot discussed the direct browlift with an excision of an ellipse of tissue above the brow. The endoscopic brow lifting was first introduced in 1991 by Keller. The overall complication rate for any forehead procedure is low. De Cordier and coworkers retrospectively reviewed 393 patients who underwent endoscopic forehead lift from 1994 to 2000. The review reported alopecia in one occurrence (0.3%), transient scalp numbness in most patients, 2% with prolonged dysesthesia, and seven patients (2.3%) with a temporary frontal nerve weakness. Forehead hematoma requiring in-office drainage occurred in 3.5% of patients. Seven percent of their patients experienced lagophthalmos, 8% with upper eyelid asymmetry, and 3% with brow malposition. There was also one patient who had wound dehiscence and one who had a suture abscess.
Brow malposition
For successful rejuvenation the surgeon must have a fundamental knowledge of forehead anatomy. In the forehead, the layers are.
- •
Skin
- •
Subcutaneous tissue
- •
Muscle
- •
Fibrous galea
- •
Loose areolar tissue
- •
Pericranium
The superficial musculoaponeurotic system in the lower two-thirds of the face continues as the superficial temporoparietal fascia over the zygoma and then merges with the fibrous galea in the forehead. The temporal line is formed by the convergence of the deep and superficial layers of the deep temporal fascia. The deep temporal fascia is thicker and has a white glistening appearance. Inferior to the zygomatic arch, the deep temporal fascia splits into two layers called the intermediate temporal and deep temporal fasciae. Another important landmark in brow lifting procedures is the adherent arcus marginalis along the supraorbital rim, this is where the periosteum of the frontal bone fuses with the galea. Release of these dense fibrous attachments in forehead rejuvenation is important to produce the desired elevation and stabilization of the brow. Preoperative evaluation of the patient with photographic documentation noting asymmetries helps minimize the risk of patient dissatisfaction. Careful patient selection, release of arcus marginalis, and symmetric suspension should decrease the risk of poor patient satisfaction.
Malposition of the brow may occur with any approach to forehead rejuvenation. Too much resection of skin in any open approach or excessive suspension with any procedure may results in possible lagophthalmos and brow malposition ( Fig. 3 ). The risk is increased when simultaneously blepharoplasty is performed. To avoid excessive skin resection during the blepharoplasty the forehead lift should be completed before the eyelid surgery. When lagophthalmos is limited to less than 2 mm there is a decreased risk of dry eye syndrome. If a patient develops symptoms of irritation or dryness this should be treated with lubricating eye drops and ointments. In one study of 600 patients who underwent combined upper blepharoplasty and open coronal browlift there was no dry eye syndrome, blindness, or globe exposure, and there were only two cases of brow asymmetry. In a retrospective study comparing 140 (121 coronal and 19 endoscopic) patients who had either the endoscopic-assisted approach or the open approach there was no significant difference in brow elevation with either approach alone or in combination with blepharoplasty at the 1-year evaluation.




