Lasers are currently used to perform a variety of procedures and therapies within the practice of oral and maxillofacial surgery. The laser offers many benefits over traditional surgical procedures performed by traditional techniques of sharp dissection, and the use of the laser continues to expand in conjunction with the advancement of laser technology. The use of lasers within oral and maxillofacial surgery along with potential benefits, drawbacks, and risks with certain procedures will be reviewed along with the discussion of some newer nontraditional applications of laser therapy.
▪
LASER PHYSICS
A brief review of laser physics is essential to understand how lasers work in regard to specific applications of their use for surgical procedures. The physics of lasers is well known as energy is transferred to an electron and then emitted to produce laser energy based on Einstein’s quantum theory of radiation hypothesis that atoms passing from a higher to a lower energy state will emit energy or photons, representing small units or quanta of electromagnetic waves. Electrons are usually in a low energy orbit closest to the atomic nucleus, and electrons can move to a higher energy level orbit by absorbing external energy. Conversely, when the electrons return to the original lower orbital level, the excess energy previously absorbed is released as spontaneous emission in the form of light or photons.
The laser production of energy is accomplished by the transfer of energy to the electron of an atom. Normally the low energy electron is excited through a photon striking the atom and transferring energy to produce excitation of the electron to a higher energy state, causing the electron to enter another excitatory outer electron ring further away from the nucleus of the atom through the absorption of energy. The electron in the unstable higher energy state in an outer orbit returns to the lower energy orbital ring of a resting state and subsequently releases electromagnetic energy through spontaneous emission of radiation in the form of light. The stimulated emission of radiation occurs when external energy of an electrical, chemical, or optical source is used to initiate the atomic photon emission as atoms produce stimulated emission of radiation, which is used to generate laser energy.
Maiman developed the acronym “laser” for light amplified by the stimulated emission of radiation. Lasers are the devices that rely on the stimulated emission of radiation to produce a beam of light. Laser components include an energy source, a resonant chamber, and an active medium. The energy source is usually electrical and flows through the laser medium. The resonant chamber contains the laser medium and reflective mirrors, one of which is highly reflective and another that is only partially reflective, permitting some laser light to exit. The active medium is the atom, molecule, or ion producing the radiation. The type of medium commonly gives the laser its name. Common mediums include the Nd : YAG laser, which is a solid state laser composed of neodymium ions and crystals of yttrium-aluminum-garnet. The CO 2 laser is a gas laser incorporating carbon dioxide, nitrogen, and helium. Dye lasers are liquid lasers with fluorescent organic dyes injected into a tube.
The components and design of a laser permit the efficient production and emission of synchronized light. Initially, atoms within the laser chamber absorb energy from the energy source, in which atoms in the higher energy states spontaneously decay and give up energy. The released energy is absorbed by other atoms and used to enter a higher energy state as a so-called pumping phenomenon. Ultimately, a larger number of atoms exist in a higher energy state called population inversion. More and more atoms reach the higher energy state and spontaneously decay releasing more energy, which results in the emission of additional photons that travel within the laser chamber as amplification of stimulated emission of radiation. As pumping continues to maintain an ample population of inversion with the resonant chamber, a beam of coherent light is produced that is reflected and partially reflected by mirrors, resulting in the emergence of a beam of bright, monochromatic, coherent light, or a laser beam.
Lasers produce energy in the form of light, which is transmitted to an object as the electron in the excited state is bombarded with irradiation by photons of light as the electron is returning to a more stable resting state. Two photons of emitted light energy are produced and transmitted. The light energy is amplified and emitted by radiation of the atom. Emitted laser light is of the same monochromatic wavelength in waves and remains collimated, or parallel, over long distances or coherent versus other light that spreads over distances.
Lasers generate light in a similar manner through the excitation of atoms by photons of light in a resonator or a cavity through the use of a medium, and then the light strikes a fully reflective and a partially reflective mirror, which releases between 5% to 10% of the light. Different mediums will determine the wavelengths of light released. Gas, such as CO 2 , is a common laser medium along with solid mediums, such as garnet or ruby crystals, which release energy as they are electrically charged to produce laser light energy.
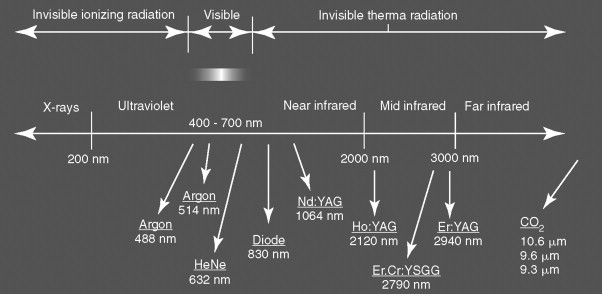
Laser light can be characterized by wavelength. The ultraviolet range is 100 to 400 nm, visible range of 400 to 700 nm, near-infrared range of 700 to 1400 nm, mid-infrared range of 1400 to 20,000 nm, and the far-infrared range of greater than 20,000 nm. Laser light can also be defined by other unique properties. Laser light is monochromatic where all the photons in a laser beam are of the same wavelength, allowing the laser beam to attain a sufficient intensity to interact with tissues based upon wavelength and the absorption, scattering, and reflection properties of the target tissue. Laser light is also coherent with all photons in the beam synchronized in time and space, unlike the random photons of conventional light. The laser beam is collimated with the beams parallel with the ability of the beam to be focused on a small target area and also allowing all the emitted laser energy to be captured and delivered to a target site through a flexible fiber optical system or with the use of mirrors.
A multitude of factors can control the interaction of lasers with tissues. Power density is the amount of power transmitted per area of a cross-section of the laser beam in watts/cm 2 . It also represents the power of the laser striking the targeted tissue per unit area with the power density of a laser inversely proportional to the square diameter of the focal target. The spot size of the beam also determines the energy transmitted by the laser because the spot size reflects the ability of the laser to be focused, delivering more energy, or defocused as the distance of the lens to the tissue is increased by the operator. The vaporization threshold is the amount of energy in watts necessary to vaporize the target tissue.
The wavelength of the laser beam determines factors, such as the degree of scattering, tissue penetration, and the amount of energy absorbed by the tissues. The greater the degree of scattering the less energy focused on the target tissue. Lasers with less scatter are better used as a scalpel because the energy is precisely delivered to a single spot of tissue, whereas a laser with more scatter is better for photocoagulation ( Figure 14-1 ). Fluence is a term that describes the amount of energy applied to a particular area of tissue. The overall delivery of energy can be determined by computer-generated patterns to maximize efficiency and minimize tissue damage.
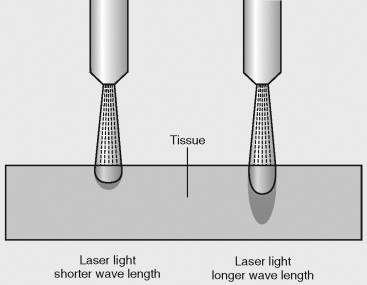
Exposure time is the amount of time the laser energy is directed at the target tissue and can be varied by continuous, pulsated, or other varied modes of delivery. Continuous or nonpulsated delivery provides a continuous wave of laser energy to the tissue over a time period determined by the operator. The ability to pulsate the delivery of laser energy has the effect of modifying the delivery of higher laser energy for very short periods (e.g., 100 microseconds). The pulsation of laser energy prevents deeper tissue penetration of the laser and minimizes tissue heat buildup by allowing the thermal tissue relaxation time for heat dissipation, allowing the tissue to cool. The ability to control the heat buildup of the adjacent tissue with the use of the laser provides the operator with the ability to control the interaction of the laser with the targeted tissue and, ultimately, vary the effects of the laser on the tissue.
The delivery of the energy by the laser can be modified to produce optimal results depending on the desired tissue interaction. The pulsation of a laser provides a noncontinuous delivery of energy to the target tissue. Pulsation rates are measured in number of pulses per second and used to calculate a pulse width, representing the time necessary for the pulse to go from zero energy to maximum energy and return back to zero energy. Superpulsation is another method to minimize adjacent tissue damage by producing higher peak power per pulse at shorter pulse width to allow for the precise cutting or ablation of tissue with a laser. Ultrapulsation of the laser can also be used by increasing the pulse speed, resulting in less adjacent tissue damage. It has been useful in applications, such as skin resurfacing.
The use of flashscanning can also be used to produce less collateral tissue damage by limiting thermal damage. Flashscanning applies the use of a laser at continuous high energy in a circular pattern through the use of rotating mirrors, which limits the energy delivered to any specific area, allowing adequate tissue relaxation. It has been used with skin resurfacing procedures. Quality switching, or Q-switching, is another method to limit damage of adjacent tissue with the use of a laser. Q-switching provides the ability of the laser to produce high-energy pulses of nanoseconds duration through the use of an electromagnetic switch operating a shutter mechanism. Applications of the Q-switched laser have included treatment of certain pigmented skin lesions and removal of tattoos. Ultimately, the laser can be used for selective tissue destruction while limiting the damage or undesirable effects to the adjacent tissue because the tissue relaxation time can be calculated for different tissues, such as skin, blood vessels, and muscle.
▪
LASERS AND TISSUE INTERACTIONS
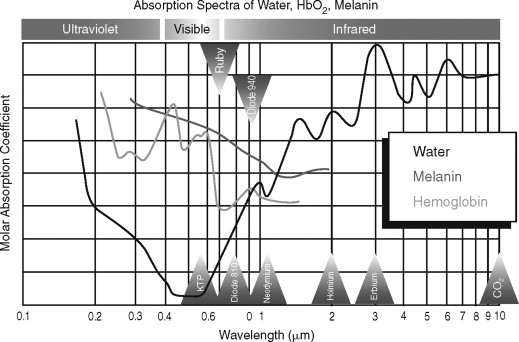
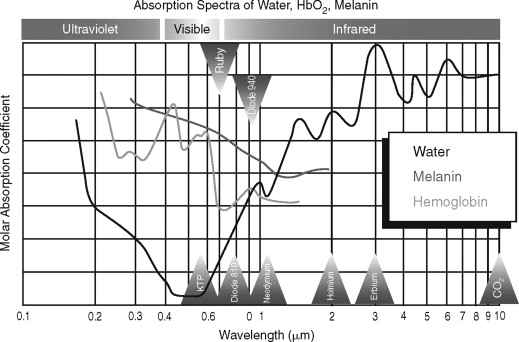
The effects of lasers on tissues can result in the energy of the laser being reflected, transmitted, or absorbed. Energy absorbed within the tissue can be dissipated or converted to other forms of energy, such as heat, shock waves, or chemical reactions. The conversion of laser energy into heat by the tissue is common with medical lasers interacting with molecular compounds, such as water, melanin, or hemoglobin, within the tissue called chromophores ( Figure 14-2 ). The amount of energy absorbed by the tissues is determined by the amount of chromophores within the tissue. The tissue reaction with the use of a laser is determined by the type of tissue exposed to the laser energy and the wavelength of the laser light ( Table 14-1 ).
| Temperature °F | Tissue effect |
|---|---|
| 37-60 °F | Tissue retraction and conformational protein changes |
| >60 °F | Protein denaturation and protein coagulation |
| 90-100 °F | Tissue carbonization and tissue char |
| >100 °F | Tissue ablation |
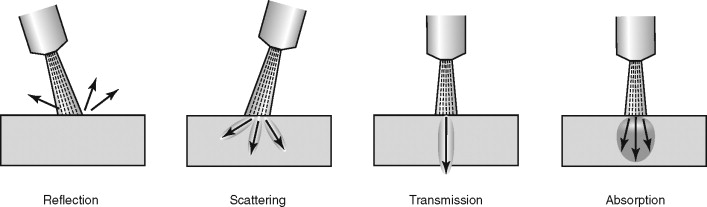
Laser light results in one of four basic tissue reactions to the energy. The reactions include reflection off the tissue, scattering to the surrounding tissue, transmission through the tissue, and absorption of the energy into tissue chromophores ( Figure 14-3 ). Immediate reactions and delayed reactions take place once the laser reacts with the tissue through photochemical, photothermal, and photoablation reactions. Photochemical reactions can occur after lasers interact with a photosensitizer, causing tissue necrosis.
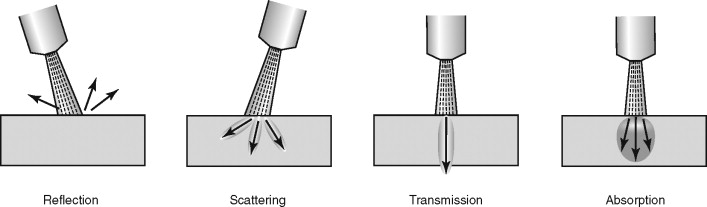
Photothermal reactions result as the laser causes denaturing of enzymes, coagulation, tissue necrosis, and vaporization. Photoablation reactions of lasers can cause tissue disruption by thermal explosion or mechanical shock waves, causing tissue disruption.
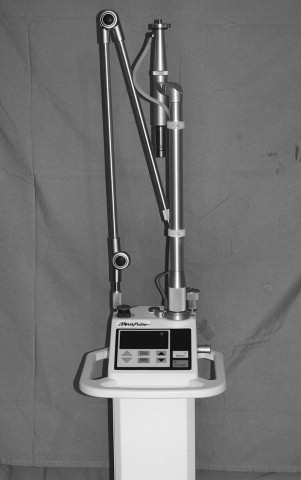
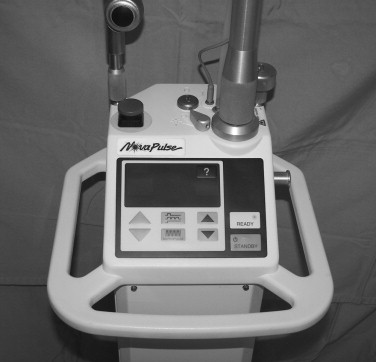
Currently, there are multiple lasers for biomedical use, such as the CO 2 , Nd : YAG, erbium : YAG, argon ion, and diode lasers ( Figure 14-4 ). The CO 2 laser was developed in 1964 by Patel at Bell Laboratories. CO 2 lasers use a gas medium composed primarily of CO 2, which produces a laser beam with wavelengths in the mid-infrared region of 10,600 nm. The CO 2 laser is commonly used in oral and maxillofacial surgery and otolaryngology. The benefits of the CO 2 laser include minimal scatter, excellent water absorption, rapid soft tissue vaporization, and negligible surrounding tissue damage. The CO 2 laser functions as an excellent scalpel and can focus precisely onto the target tissue, thus avoiding adjacent tissue damage for hemostatic cutting as vessels below 0.5 mm are coagulated. The CO 2 laser previously had to be delivered down an articulated arm by a series of mirrors, but is now delivered through a flexible fiber, making the delivery more versatile ( Figures 14-5, 14-6, 14-7 ).
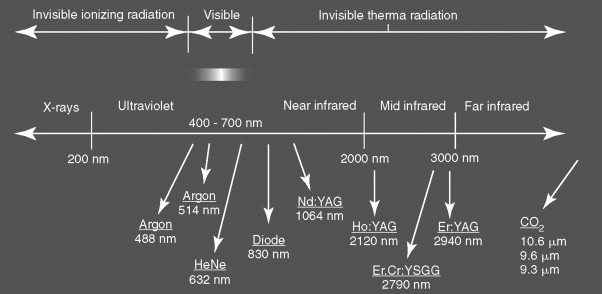

The Nd : YAG laser was also developed in 1960 at Bell Laboratories by Geusic et al. The Nd : YAG laser is a solid state laser and was the first laser developed. The Nd : YAG laser produces a laser beam with wavelengths between 1064 and 1320 nm, and the beam itself is invisible requiring the use of a helium-neon guide beam. The Nd : YAG laser is minimally absorbed, but can deeply penetrate tissue up to depths of 10 mm for deep tissue vasoconstriction of even vessels up to 2 to 3 mm in diameter. There is also a greater amount of adjacent tissue damage than the CO 2 laser. Common maxillofacial applications include coagulation of angiomas, vascular tumor resections, and arthroscopic surgery of the temporomandibular joint (TMJ).
The erbium : YAG laser produces a wavelength of 2940 nm and is another laser that has excellent energy absorption by water, making it an ideal laser for intraoral use and for superficial skin resurfacing as a result of the limited depth of penetration through skin with less adjacent tissue damage, resulting in decreased erythema, edema, and pain. The erbium : YAG laser can also cut hard tissue, including both bone and enamel, which makes it an obvious choice for oral and maxillofacial surgical procedures where a combination surgery is performed on both hard and soft tissue, such as crown elongation, tooth exposure, and implant uncovering procedures. The erbium : YAG laser is used for operative dentistry and the cutting of tooth structure.
The argon ion laser is a low wavelength laser of 488 to 514 nm that produces a blue-green color beam. The argon ion laser is primarily used for photocoagulation of small vessels in dermatology and ophthalmology.
The Nd : YAGKTP laser is another available laser with a wavelength of 0.32 μm through the use of a frequencydoubling potassium titanyl phosphate (KTP) crystal in the green spectrum of light similar to the argon laser. The KTP crystal halves or “doubles” the wavelength. Diode lasers are another development that rely on the use of non-solid state semiconductor technology. Diode lasers can attain higher power around 0.81 μm with a power of 20 W, which has applications similar to the Nd : YAG laser. Benefits of the diode laser include a reduced size, reduced cost, and greater versatility through the use of frequency-doubling crystals to allow a variety of output wavelengths for applications ranging from tissue excision, coagulation, periodontal surgery, or use at lower wavelengths for the treatment of pain or to modulate healing. There are also a multitude of low-level lasers produced that are used for a variety of nonsurgical therapeutic treatments, which will be discussed in further detail later.
▪
LASERS AND TISSUE INTERACTIONS
The effects of lasers on tissues can result in the energy of the laser being reflected, transmitted, or absorbed. Energy absorbed within the tissue can be dissipated or converted to other forms of energy, such as heat, shock waves, or chemical reactions. The conversion of laser energy into heat by the tissue is common with medical lasers interacting with molecular compounds, such as water, melanin, or hemoglobin, within the tissue called chromophores ( Figure 14-2 ). The amount of energy absorbed by the tissues is determined by the amount of chromophores within the tissue. The tissue reaction with the use of a laser is determined by the type of tissue exposed to the laser energy and the wavelength of the laser light ( Table 14-1 ).
| Temperature °F | Tissue effect |
|---|---|
| 37-60 °F | Tissue retraction and conformational protein changes |
| >60 °F | Protein denaturation and protein coagulation |
| 90-100 °F | Tissue carbonization and tissue char |
| >100 °F | Tissue ablation |
Laser light results in one of four basic tissue reactions to the energy. The reactions include reflection off the tissue, scattering to the surrounding tissue, transmission through the tissue, and absorption of the energy into tissue chromophores ( Figure 14-3 ). Immediate reactions and delayed reactions take place once the laser reacts with the tissue through photochemical, photothermal, and photoablation reactions. Photochemical reactions can occur after lasers interact with a photosensitizer, causing tissue necrosis.
Photothermal reactions result as the laser causes denaturing of enzymes, coagulation, tissue necrosis, and vaporization. Photoablation reactions of lasers can cause tissue disruption by thermal explosion or mechanical shock waves, causing tissue disruption.
Currently, there are multiple lasers for biomedical use, such as the CO 2 , Nd : YAG, erbium : YAG, argon ion, and diode lasers ( Figure 14-4 ). The CO 2 laser was developed in 1964 by Patel at Bell Laboratories. CO 2 lasers use a gas medium composed primarily of CO 2, which produces a laser beam with wavelengths in the mid-infrared region of 10,600 nm. The CO 2 laser is commonly used in oral and maxillofacial surgery and otolaryngology. The benefits of the CO 2 laser include minimal scatter, excellent water absorption, rapid soft tissue vaporization, and negligible surrounding tissue damage. The CO 2 laser functions as an excellent scalpel and can focus precisely onto the target tissue, thus avoiding adjacent tissue damage for hemostatic cutting as vessels below 0.5 mm are coagulated. The CO 2 laser previously had to be delivered down an articulated arm by a series of mirrors, but is now delivered through a flexible fiber, making the delivery more versatile ( Figures 14-5, 14-6, 14-7 ).

The Nd : YAG laser was also developed in 1960 at Bell Laboratories by Geusic et al. The Nd : YAG laser is a solid state laser and was the first laser developed. The Nd : YAG laser produces a laser beam with wavelengths between 1064 and 1320 nm, and the beam itself is invisible requiring the use of a helium-neon guide beam. The Nd : YAG laser is minimally absorbed, but can deeply penetrate tissue up to depths of 10 mm for deep tissue vasoconstriction of even vessels up to 2 to 3 mm in diameter. There is also a greater amount of adjacent tissue damage than the CO 2 laser. Common maxillofacial applications include coagulation of angiomas, vascular tumor resections, and arthroscopic surgery of the temporomandibular joint (TMJ).
The erbium : YAG laser produces a wavelength of 2940 nm and is another laser that has excellent energy absorption by water, making it an ideal laser for intraoral use and for superficial skin resurfacing as a result of the limited depth of penetration through skin with less adjacent tissue damage, resulting in decreased erythema, edema, and pain. The erbium : YAG laser can also cut hard tissue, including both bone and enamel, which makes it an obvious choice for oral and maxillofacial surgical procedures where a combination surgery is performed on both hard and soft tissue, such as crown elongation, tooth exposure, and implant uncovering procedures. The erbium : YAG laser is used for operative dentistry and the cutting of tooth structure.
The argon ion laser is a low wavelength laser of 488 to 514 nm that produces a blue-green color beam. The argon ion laser is primarily used for photocoagulation of small vessels in dermatology and ophthalmology.
The Nd : YAGKTP laser is another available laser with a wavelength of 0.32 μm through the use of a frequencydoubling potassium titanyl phosphate (KTP) crystal in the green spectrum of light similar to the argon laser. The KTP crystal halves or “doubles” the wavelength. Diode lasers are another development that rely on the use of non-solid state semiconductor technology. Diode lasers can attain higher power around 0.81 μm with a power of 20 W, which has applications similar to the Nd : YAG laser. Benefits of the diode laser include a reduced size, reduced cost, and greater versatility through the use of frequency-doubling crystals to allow a variety of output wavelengths for applications ranging from tissue excision, coagulation, periodontal surgery, or use at lower wavelengths for the treatment of pain or to modulate healing. There are also a multitude of low-level lasers produced that are used for a variety of nonsurgical therapeutic treatments, which will be discussed in further detail later.
▪
LASER EQUIPMENT REVIEW
The purchase of a laser represents a significant expense. Before purchasing a laser, a review of available lasers should compare certain practical characteristics of the laser unit. Primary consideration should be given to the specific laser application or intended function and the functional treatment range of the laser along with the specifics of operation and considerations of return on equity. Lasers are useful for a variety of procedures for soft and hard tissue applications. Many practitioners want a multifunctional laser with the ability to perform a variety of surgical procedures. Therefore, any present and future applications of lasers should be considered before purchase. There are also a number of lasers with multiple mediums available.
The length of service of a laser generally indicates that the laser may be more reliable and has minimal operational breakdowns. Lasers that have been in service for extended periods of time can indicate the laser has the ability to be used with many diverse procedures and a greater professional acceptance, popularity, and reliability. Lasers with FDA clearance for use on humans is paramount, although it is noted many lasers and cosmetic procedures do not require FDA approval when used for so called “nonsurgical treatments.”
The laser medium is usually crystal or gas and generates a specific wavelength of laser energy for the desired application. The name of the laser will often incorporate the type of medium used. The type of medium will also dictate the overall price of the laser. How long the laser medium will last is related to the number of times the lasing medium expands itself over time. Often the laser medium will require replacement after a certain range of hours of use. The lifespan of the laser medium should be considered in the purchase of a laser.
Laser wavelength will dictate the tissues’ response to the absorption of the laser energy and the applicable use of the laser. The emission mode of the laser will also vary from continuous to a pulsed mode. Continuous lasers will work more rapidly, but also generate more heat and pain. Pulsed lasers can provide less pain during the surgical procedure. Maximum power as watts will determine the energy levels to affect different tissues, and the energy should be able to be modulated depending on the application.
The laser delivery system should be versatile with easy access in the oral cavity. Laser delivery systems can include the hollow fiber, fiber with diffuser tips, bare fibers, and articulating arm and hand piece. Hollow fiber delivery systems have a perforated metal tip and require cooling by a nonflammable gas, such as CO 2 , and are useful for coagulation in a noncontact manner. Fibers with a diffuser tip are usually made of sapphire and are used in a contact mode for cutting tissue. Bare fibers are useful for use in confined cavities, such as the TMJ, because of the small diameter and can coagulate or cut tissue. The articulated arm and handpiece uses reflective mirrors with the beam exiting through a handpiece to allow both coagulation and cutting of tissue ( Figure 14-8 ). Lasers with hollow fibers or fibers alone will need periodic replacement and result in higher operating costs than those with articulating arms and hand pieces.
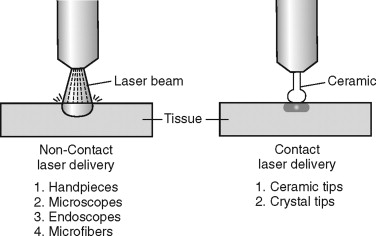
Optional features of some lasers can include a cooling system, such as a water spray, to protect the adjacent tissue and remove debris during use of the laser. The beam and fiber diameter is also important depending on the laser application. Some lasers will require contact with the tissue, whereas others operate in a noncontact mode at a variable distance from the tissue. The noncontact lasers have a hand piece with a lens along with a pointing blade or a HeNe target beam as a visible guide. The sterilization cycle of the laser is also important and may dictate the need for additional laser hand pieces. Most lasers operate on 120 V power, although some models require 220 V power and a separate electrical supply within the office.
Other factors to be considered in laser selection can include size and portability of the laser unit. Appropriate training from the manufacturer should be provided as part of the package and should include training of the office staff. The laser warranty should be evaluated because lasers can break down. Consideration should be given to the time frame of the warranty and if parts and labor are covered and if the laser can be repaired on-site or has to be returned to the manufacturer. Thorough research is advisable before obtaining a laser because of the many available options, specific use limitations, and large cost variations of available lasers.
▪
LASER SAFETY
Laser safety is paramount to the use of lasers for oral and maxillofacial surgical procedures. All laser equipment should be thoroughly inspected and tested on an inert object, such as a moistened tongue blade, before use to confirm proper energy levels and safe operation of the laser. Adequate precautions must be taken to prevent inadvertent exposure of operating room personnel and the patient to unintentional laser energy not directed toward the therapeutic target tissue ( Box 14-1 ). The laser should be inactivated before moving the laser upon completion of the energy delivery to the operative site to prevent inadvertent laser burns to the patient or operatory personnel. The operatory room door must be closed during the procedure, and warning signs indicating the use of the laser and requiring additional eyewear must be placed on the operatory doors while the laser is being used ( Figures. 14-9 and 14-10 ).
-
Electrical source injury
-
Laser-ignited contact fire
-
Laser-ignited airway fire
-
Eye exposure injury
-
Laser plume inhalational injury
-
Inadvertent mucosal and skin burns
-
Enamel injury


Problems of inadvertent laser exposure can include corneal or scleral scarring by direct exposure, making the use of safety glasses with side shields mandatory. If the patient is receiving laser therapy in the region of the eye, the use of metal corneal shields with topical anesthetic and lubrication must be used, otherwise the patient should have their eyes completely covered with laser glasses or moistened towels ( Figure 14-11 ). Proper evacuation of the resultant laser plume via laser vacuums with HEPA filters held near the operative field should be used along with the use of viral filtering face masks to prevent possible contamination of operating room personnel with bacteria or viruses during laser procedures ( Figures 14-12 and 14-13 ).



The use of nonflammable surgical skin preparations containing no alcohol, such as Betadine or hexachlorophene, should be followed by wiping with sterile water to prevent skin color changes. The use of isopropyl alcohol or chlorhexidine preparations containing alcohol should be avoided because of potential flammability with pooling in facial crevices or potential flammability with vaporization of the alcohol after the facial application. Nonflammable patient drapes for use with lasers or moistened towels should also be used. The teeth must also be protected with moistened gauze or commercial silicone teeth protectors when using the laser around the mouth or intraorally because enamel can be damaged by absorbed laser energy along with possible thermal damage to pulpal tissue from heat conduction. The need to protect adjacent oral tissue from damage is also required, such as the use of wet sponges, moistened tongue blades, and nonreflective ebonized instruments, to prevent unintentional tissue damage.
The use of lasers in the presence of supplemental oxygen requires the use of precautions to prevent inadvertent fires. Patients under general anesthesia should use a commercial metal-covered endotracheal tube specific for laser use or have the tube wrapped with nonreflective foil to prevent a possible fire in the endotracheal tube, with pressurized oxygen creating a torchlike effect. The cuff should be inflated with normal saline versus air, and the tube should additionally be protected with wet sponges if exposed intraorally. If the patient is being sedated and supplemental oxygen is used via a nasal cannula or face mask, care must be used, and the oxygen delivery cannula or mask can be wrapped in foil to prevent an airway fire. The oxygen can be delivered through a nasopharyngeal airway under low flow while packing off the posterior pharynx with moistened gauze. The supplemental oxygen should be used at a low flow or can be turned off while the laser is being used. The use of facial drapes that can cause a high oxygen concentration to accumulate under the drapes, possibly leading to a fire, should be avoided. Saline or sterile water should also be readily available to extinguish an airway fire if needed.
▪
LASER USE FOR ORAL AND MAXILLOFACIAL SURGERY
The use of a laser to perform oral and maxillofacial surgical procedures has continued to evolve over the last 35 years. Lasers have commonly been used to treat a variety of pathologic conditions, and the use of lasers for other modalities has continued to grow. The laser has proven to be a useful tool within the practice of oral and maxillofacial surgery for procedures, such as implant uncovering, gingival recontouring, surgical exposure of teeth, laser-assisted arthroscopic TMJ surgery, and treatment of oral pathologic conditions, such as vascular lesions, and many other applications. The use of the laser within oral and maxillofacial surgery continues to progress, especially with the newer low-level diode and other lasers for newer applications to aid in bone healing, treatment of periimplantitis, therapy for temporomandibular disorders (TMD), and novel applications, such as navigational surgery ( Figure 14-14 ). Today, lasers are a common part of the armamentarium of the oral and maxillofacial surgeon because the laser equipment is readily available for office procedures with the development of lasers that are multiversatile in use, easier to operate, and more affordable in cost.
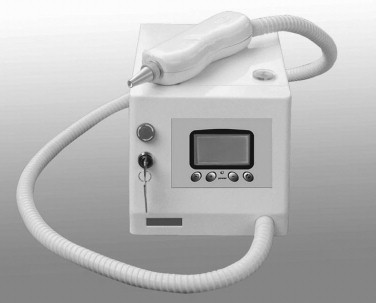
The use of lasers for oral and maxillofacial surgery was initiated in 1970 by Polanyi with the use of a CO 2 laser to incise living tissue. Polanyi also developed a hand-held laser delivery system. The CO 2 laser remains the most commonly used laser for intraoral surgery as a result of the excellent absorption of the infrared laser wavelengths of 10,600 nm by tissues with high water content. A multitude of other lasers, such as argon, holmium : YAG, and erbium : YAG, are also used for selected applications in oral and maxillofacial surgery.
The use of the CO 2 laser for the surgical treatment of oral mucosa stems from the excellent energy absorption because oral mucosa has a 90% water composition making it ideal for absorption of infrared energy. The laser energy results in cellular disruption and vaporization of the oral mucosal tissue by the CO 2 laser. CO 2 lasers also provide excellent coagulation and hemostasis and decreased wound contraction and scarring as a result of decreased fibrosis with healing. Other benefits include decreased postoperative pain and edema with intraoral surgery. The laser is also able to be used in areas of limited exposure within the oral cavity where access with conventional surgical scalpel blades or other means of dissection can be difficult, such as areas of moveable mucosa (e.g., the floor of the mouth, posterior pharynx, or soft palate). Lasers do have some disadvantages, such as delayed wound healing, possibly up to a 2- to 3-week period, versus conventional surgical dissection techniques, which generally heal in 7 to 10 days because laser wounds are slow to epithelialize.
▪
INCISIONAL AND EXCISIONAL LASER SOFT TISSUE PROCEDURES
Laser soft tissue surgery is another common area where the treatment can be well controlled with minimal adjacent tissue damage and also provides excellent wound hemostasis. The benefits of the CO 2 laser are well documented for a variety of intraoral soft tissue procedures because the procedures can be completed with excellent hemostasis and less pain during the procedure and postoperatively. The reduction of the associated bacteria is another benefit that results in improved wound healing with a decrease in the rate of infection with surgery. The CO 2 laser is set on a continuous wave in a range of 2 to 10 W for most excisional procedures with the smallest spot size at the focal point of the laser to produce an incision of a controlled depth and thin width. The laser can also be defocused to permit coagulation of blood vessels to aid in hemostasis.
A common example of a laser excision procedure would be the excision of a labial or lingual frenum. The mucosa and the underlying muscle are easily excised with the use of the laser. Following the administration of local anesthesia, the frenum attachments are separated and the surrounding tissue is preserved. The wound demonstrates complete hemostasis, and suturing is usually not required. Following laser frenectomy procedures, the wound heals slower than those done with sharp dissection with a blade or scissors, although the patient will usually experience less postoperative pain than with a sharp dissection.
The laser-assisted excision of common benign mucosal lesions is also commonly performed. For example, the laser can be used to excise a fibroma of the lip or buccal mucosa by excising the lesion in an elliptical manner with adequate soft tissue margins usually extending 0.5 mm beyond the normal margin for a scalpel excision to allow for a zone of lateral necrosis within the specimen from the laser, which can be difficult to interpret histologically. The specimen is sent for routine histopathologic examination, and the subsequent wound can be closed with sutures or left to granulate. Lesions that can be excised with the laser include epulis fissurata, mucoceles, or other mucus retention phenomenon with the use of the CO 2 laser on a continuous mode of 4 to 10 W depending on the tissue to be incised and spot sizes of 0.1 to 0.5 mm. The entire mucocele lesion is outlined, excised, and undermined. A ranula is treated with the laser by excising the covering layer of mucosa at the periphery for marsupialization. The laser will provide excellent hemostasis of the surgical site, and the need for countertraction is negated as normally needed for a scalpel blade excision with the use of the laser in the floor of the mouth region. Suturing is generally not needed with the use of the laser. Laser-assisted sialolith excision in the floor of the mouth can also be performed by incision through the mucosa and duct to the area of the stone with a flash of light noted once the stone is encountered. The sialolith is then removed, and the wound is left to granulate without suturing to prevent stricture or obstruction of the underlying duct.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


