Introduction
The purposes of this study were to determine the incidence of open gingival embrasures after a single mandibular incisor extraction and to investigate whether age, sex, interproximal pretreatment and posttreatment contact location, or the type of mandibular incisor were predictors of the incidence and magnitude of open gingival embrasures.
Methods
Pretreatment and posttreatment intraoral frontal photos of 51 adults who had 1 mandibular incisor extracted were evaluated to determine the incidence and magnitude of open gingival embrasures.
Results
The incidence of open gingival embrasures was 68%; the embrasures were moderately noticeable to very noticeable in 52% of those patients. Age, sex, incisor type, and location of interproximal contact before treatment were not predictors of open gingival embrasures after mandibular incisor extractions. An interproximal contact in the incisal third at the end of treatment was associated with the formation of an open gingival embrasure.
Conclusions
Open gingival embrasures are a common finding after the extraction of a mandibular incisor, and the magnitude of this embrasure is clinically noticeable.
Mandibular incisor extraction therapy has been used as a treatment option since the early 1900s to relieve tooth size-arch length discrepancies in the anterior segment of the mandible. The advantages of this therapy include potential reduction in treatment time, possibility of achieving better long-term stability in the mandibular anterior segment since intercanine width is not increased, and maintenance of the soft-tissue profile because retraction of the mandibular incisors is less compared with mandibular premolar extractions.
These advantages are counterbalanced, however, by some potential disadvantages. The most significant of these is the possibility of the space reopening in the long term, an occlusal result less than ideal because of a significant tooth-mass reduction in the anterior mandibular region. Another potential sequelae of this therapy is the development of an open gingival embrasure.
Open gingival embrasures after orthodontic treatment have been reported in up to 40% of adolescent patients with crowded maxillary central incisors. Some causes attributed to open embrasures are periodontal bone loss, high interproximal contact, triangular shape of the incisors, and divergent root angulations. The interproximal papillae might be sacrificed with the extraction of a mandibular incisor, and an open embrasure can result; yet only anecdotal evidence has pointed to this outcome.
The objective of this study was to quantify the incidence and magnitude of an open gingival embrasure after mandibular incisor extraction. In addition, predictors of this unesthetic outcome were explored.
Material and methods
The study sample comprised 51 patients (22 male, 29 female) in the permanent dentition with a treatment plan involving 1 mandibular incisor extraction. The mean age at the start of treatment was 26.8 years (range, 15-62 years). The majority had Class I crowding (41 patients), followed by Class II (6 patients) and Class III (4 patients) malocclusions. Edgewise appliances were used in treating all the patients, and all had 1 mandibular incisor extracted. The exclusion criteria were (1) evidence of periodontal bone loss or existing open gingival embrasures determined by the clinical and radiographic examinations; (2) mandibular incisors lost to trauma, caries, or periodontal disease; and (3) congenitally missing incisors.
Before and after intraoral frontal photographs were collected from the orthodontic graduate clinic and private offices of alumni and orthodontists in Connecticut ( Fig 1 ). Posttreatment records were taken on average 2 months after appliance removal. Records were obtained as 35-mm slides and digital images. The slides were scanned (Expression 1640XL, Seiko Epson, Nagano, Japan) at a resolution 600 dpi and converted into digital images. Two evaluators (B.H. and M.L) individually viewed and rated each variable in the before and after photographs 3 times, with a 2-week interval between evaluations. There was no limit on the viewing time period; each photograph was projected on a screen (height, 5 ft; width, 6 ft) from a computer projector (Pro Xtrax, Sanyo, Osaka, Japan) for as long as necessary to make a clear determination. All the above criteria were assessed by each evaluator individually, and the scores were established independently; the evaluators did not confer. The protocol was approved by the Institutional Review Board of the University of Connecticut.
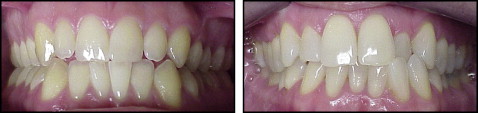
Each pretreatment and posttreatment photograph was evaluated for (1) the initial interproximal contact location (upper, middle, or gingival third), (2) the presence or absence an open gingival embrasure after treatment, and (3) the severity of interdental gingival papillary loss by using an ordinal classification system developed by Nordland and Tarnow. Accordingly, if present, the degree of the open gingival embrasure visible was classified as follows.
-
Normal: interdental papilla fills the embrasure space to the apical extent of the interdental contact point/area.
-
Class I: the tip of the interdental papilla lies between the interdental contact point and the most coronal extent of the interproximal cementoenamel junction (CEJ) (space present but interproximal CEJ not visible).
-
Class II: the tip of the interdental papilla lies at or apical to the interproximal CEJ but coronal to the apical extent of the facial CEJ, and the interproximal CEJ is visible.
-
Class III: the tip of the interdental papilla is level or apical to the facial CEJ.
Additionally, the severity of each open gingival embrasure was measured on a 4-point scale (1, not noticeable; 2, barely noticeable; 3, moderately noticeable; and 4, very noticeable) ( Fig 2 ). Photographs of patients where the contact and papillary height could not be visualized were excluded.
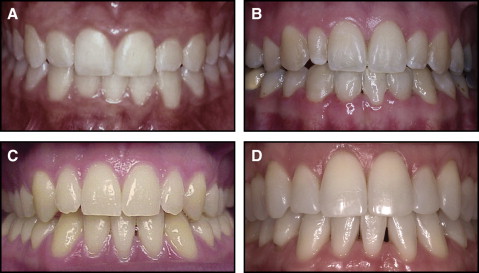
Statistical analysis
Intrarater and interrater reliability was analyzed by using Pearson and intraclass correlation coefficients. Descriptive statistics of the frequencies for the categorical variables were calculated. A point-biserial correlation coefficient was used to evaluate the relationship between age and presence and magnitude of an open gingival embrasure. A chi-square analysis was used to evaluate the relationship of the presence and magnitude of an open gingival embrasure, with sex, contact location before and after treatment, and the incisor extracted as the variables. The level of significance was set at P <0.05.
Results
More than 100 patients were screened, with 51 patients (22 male, 29 female) satisfying the inclusion and exclusion criteria. The measurements were made by 2 raters on 3 occasions. As a result, intrarater and interrater reliability analyses were conducted. Interrater reliabilities ranged from 0.9 to 0.98 for rater 1 and from 0.81 to 0.97 for rater 2 for the different measurements and time points. Interrater reliability was evaluated by using an average across the 3 measurement occasions and was calculated for each rater for each item measured. The correlations between the 2 raters ranged from 0.54 to 0.98. The raters strongly agreed on all but 2 items; contact before and contact after treatment had acceptable, although lower, reliability.
Descriptive statistics for the sample on the categorical measurements obtained in the study are shown in Table I . Frequencies are based on measurements obtained by the first evaluator on the first measurement occasion.
| Clinical variable | Percentage |
|---|---|
| Tooth extracted | |
| Central incisor | 52.9 |
| Lateral incisor | 47.1 |
| Incidence of open gingival embrasure | |
| Absent | 31.4 |
| Present | 68.6 |
| Magnitude of open gingival embrasure | |
| Normal | 31.4 |
| Class II | 68.6 |
| Contact before treatment | |
| Not determined | 17.6 |
| Incisal third | 2 |
| Middle third | 76.5 |
| Gingival third | 3.9 |
| Contact after treatment | |
| Not determined | 2 |
| Incisal third | 13.7 |
| Middle third | 82.4 |
| Gingival third | 2 |
| Level of open gingival triangle | |
| Not noticeable | 31.4 |
| Barely noticeable | 33.3 |
| Moderately noticeable | 13.7 |
| Very noticeable | 21.6 |
The variables for the magnitude and level of open gingival embrasure were significantly correlated (r = 0.76, P <0.001), indicating good correlation between the index of Nordland and Tarnow and a clinical appraisal index of the open gingival embrasure.
A point-biserial correlation failed to find a significant correlation between age and presence or absence of an open gingival embrasure (r = 0.034, P = 0.81). A chi-square analysis was conducted to examine whether there was a relationship between which incisor was extracted (lateral vs central) and presence or absence of an open gingival embrasure ( Table II ).
| Open gingival embrasure (%) | ||
|---|---|---|
| Tooth extracted | Absent | Present |
| Central incisor | 11.8 | 41.2 |
| Lateral incisor | 19.6 | 27.5 |
The data suggested that more patients who had the central incisor extracted were likely to have an open gingival embrasure than those whose lateral incisor was extracted (41% vs 27%). However, the analysis yielded a nonsignificant result, showing no association between these 2 variables (χ 2 (1) = 2.23, P = 0.13).
A chi-square analysis was also conducted to examine the association between contact before treatment (incisal third, middle third, gingival third) and presence of an open gingival embrasure. The analysis excluded patients whose contact before treatment could not be determined to reduce error in the analysis. Nine patients were excluded in this analysis.
Table III shows that most patients (93%) had contact at the middle third at the beginning of treatment. Of those, 71.4% ended with an open gingival embrasure. Few patients had a pretreatment contact location in the incisal or gingival third. The data were not significant (χ 2 (2) = 1.08, P = 0.58), suggesting that the contact location at the beginning of treatment is not associated with an open gingival embrasure.
| Open gingival embrasure (%) | ||
|---|---|---|
| Contact location | Absent | Present |
| Incisal third | 0 | 2.4 |
| Middle third | 21.4 | 71.4 |
| Gingival third | 2.4 | 2.4 |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


