Fixation of implant-supported restorations
In this chapter:
■ Cemented implant restorations
■ Screw-retained implant restorations
■ Screw-retained versus cemented
Fixed implant-supported restorations like single crowns, multiple-unit partial, and full-arch fixed dental prostheses (FDPs) are well documented in the literature and nowadays fully accepted as a treatment option for the replacement of single or multiple missing teeth1–6. The detailed outcomes of different types of implant-supported fixed restorations are given in Part III of this book.
Fixation of implant-supported restorations can be done in several ways. Restorations that are cast-on to prefabricated metal-abutments (Fig 1-10-1) and restorations that are cemented extraorally onto standard (titanium base) or customized abutments can be directly screw-retained onto the implants (Fig 1-10-2). For other screw-retained restorations, a standard abutment is screw retained into the implant and the restoration is then screw-retained onto the abutment. This is sometimes referred to as a screw in a screw in a screw type of restoration (Fig 1-10-3). Today, cemented restorations usually refer only to restorations that are cemented intraorally onto a standard or customized abutment. Single-unit restorations are either screw-retained or cemented, but multiple-unit restorations can be a combination of screw- and cement-retention. When combining the two types of retention in a single restoration it has been proposed to use temporary cement to maintain the retrievability of the restoration (Fig 1-10-4) 7.



Figs 1-10-1a to 1-10-1c Cast-on metal-ceramic implantsupported single crowns in a lateral position that can be directly screw-retained into the implants without any cementation.

Fig 1-10-2 Three-unit monolithic microveneered zirconia restoration cemented extraorally on titanium-base abutments and screw-retained directly into the two implants.
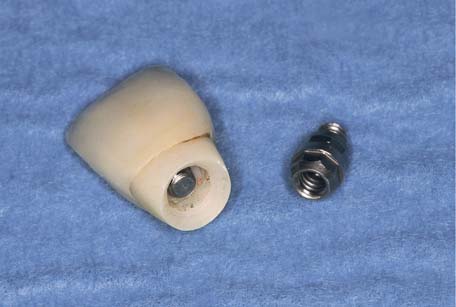
Fig 1-10-3 Implant-supported ceramic screw-retained crown with a prosthetic screw onto an abutment that was screw-retained into the implant with the abutment screw. This combination is sometimes referred to as a screw in a screw in a screw.

Fig 1-10-4 Two three-unit implant-supported restorations that were cemented intraorally with provisional cement on the anterior abutments and screw-retained on the more deeply placed posterior implants.
1.10.2 Cemented implant restorations
Initially, screw retention was only used for full-arch implant-supported FDPs in edentulous patients (Fig 1-10-5)8–10 and single-unit restorations were generally cemented on standard prefabricated cementable abutments (Fig 1-10-6)11. Both types of restorations exhibited satisfactory long-term outcomes9,12. However, due to the need for customized prosthetic components to improve esthetic outcomes or correct possible malangulations of the implant, new components like the cast-on UCLA abutment were developed13,14. These cast-on abutments could be used to fabricate both screw-retained and cement-retained single-unit restorations.

Fig 1-10-5 Full-arch implant-supported FDPs are usually screw-retained, allowing for retrievability in case of biological or technical complications.

Fig 1-10-6 Cementable implant abutment for intraoral cementation of a single molar crown.
Cemented implant-supported restorations clinically and technically resemble the procedures used for tooth-supported restorations. They might, therefore, be easier to fabricate and to manipulate in the patients’ mouths than screw-retained restorations. There are basically two ways to design a cemented implant-supported restoration. For implants with a neck configuration (soft tissue level implants), the implant shoulder represents the margin of the restoration and the abutment gives the retention (Fig 1-10-7). For such implants, a thorough evaluation of the implant site and correct three-dimensional implant position is required. Otherwise, the cementation margin might be situated too deep submucosally not allowing for an adequate removal of the excess cement15. For implants without a neck configuration (bone level implants) the restoration margin is situated on the abutment. To avoid having the cementation margin too deep submucosally, standard cementable abutments with different mucosal height and customized abutments with the cementation margin located slightly (0.5–1 mm) submucosally, can be utilized. Nowadays, the CAD/CAM manufacturing procedures enable a broad application of customized abutments and, as a consequence, the cemented restorations have become the restoration of choice in some clinical situations (Fig 1-10-8).

Fig 1-10-7 Two soft tissue-level implants with solid abutments. The implant shoulders represent the margin of the restorations and the abutments give retention for the intraoral cemented restorations.

Fig 1-10-8 The implants were placed lingually angulated due to anatomical limitations. Customized CAD/CAM abutments were used to correct the angulation and two intraorally cemented implant-supported crowns were made.
The main advantage of cemented restorations is that the implant angulations are less critical than for screw-retained restoration. Hence, one of the indications for cemented restorations are situations where it is difficult to achieve correct implant angulations due to the bone anatomy or the position of the neighboring teeth (Fig 1-10-9a, b). On the other hand, the vertical, the facio-oral, and the mesiodistal positions of the implant are equally critical for cemented and screw-retained restorations. Moreover, for cemented restorations there is no need for access holes, which increases the strength of the restoration and decreases the possible niches for ceramic fractures. The main disadvantage of the cemented restorations is that, in case of problems such as technical complications, they are difficult or impossible to remove without destruction. Furthermore, there is difficulty with the removal of the excess cement. In-vitro investigations have shown that some excess cement always remained at the tested specimens, irrespective of submucosal position of the crown margin16,17. Soft tissue complications due to excess cement have been reported in several clinical studies on cemented restorations18,19. Excess cement was also shown, in clinical studies, to be one of the major reasons for peri-implantitis20. Fortunately, in that recent clinical investigation, the signs of peri-implant disease disappeared as soon as the cement excess was successfully removed20. Nevertheless, considering a deep submucosal position of the restoration margin, the removal of the cement excess may be very difficult or even impossible15,21. Surgical interventions are often necessary to remove any remnants of the cement (Fig 1-10-10). With multiple-unit implant restorations, access to the cement remnants can be impaired due to the shape and size of the framework. As a consequence, a higher incidence of excess cement may be expected, which may cause higher rates of peri-implantitis and bone loss. This assumption is supported by the findings of systematic reviews (see Part III)22,23.


Figs 1-10-9a and 1-10-9b Three implants were inserted in the posterior mandible in combination with a bone augmentation procedure. Customized CAD/CAM abutments and intraorally cemented crowns were used to compensate for semi-optimal implant angulations.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


