Introduction
In this study, we evaluated the pain and discomfort experienced by orthodontic patients by comparing how they rated pain associated with had microimplant placement, tooth extraction, and gingival tissue removal in preparation for implant placement.
Methods
Fifty-six microimplants were placed in 28 consecutive orthodontic patients for anchorage reinforcement in the maxilla for en-masse retraction. For all patients, extractions of maxillary, or maxillary and mandibular, premolars had been planned. The recruited patients were randomized into 2 groups according to the timing of the extractions. In group A, at least 1 extraction was performed during the evaluation period; the extractions in group B were after the evaluations. Furthermore, all patients had 2 different surgical procedures for placement. On 1 side, the gingival tissue was removed before placement. On the contralateral side, the implant was placed transgingivally. Each patient’s perception of pain and discomfort was evaluated by a questionnaire before, immediately after, and 1 week after the intervention.
Results
The discomfort experienced during the extractions was described as very painful by 50% of the patients. It was significantly greater than during tissue removal and microimplant placement ( P <0.05). Microimplant placement produced no pain in 30% of the patients and was described as the least painful procedure ( P <0.05). Transgingival microimplant placement was significantly preferred by all patients ( P <0.05).
Conclusions
Microimplant surgery seems to be a well-accepted treatment option in orthodontic patients, with significantly lower pain levels than for tooth extractions. Furthermore, transgingival placement is clearly favored by patients who do not need tissue removed before placement.
The use of microimplants for anchorage purposes is a daily orthodontic routine. They have proven to be efficient and valuable for controlling anchorage and preventing unwanted side effects such as reciprocal tooth movement when maximum anchorage is required. Before the use of implants, orthodontists controlled unwanted tooth movement by choosing the appropriate appliance or technique for the patient’s clinical goals. The treatment objective is dictated by the concepts of ideal occlusion and function. The patient can in general influence the treatment only by cooperation and compliance.
The level of compliance is significantly affected by the patient’s experience of discomfort or pain. Pain has previously been defined as an unpleasant sensory and emotional experience associated with actual or potential tissue damage. Pain and discomfort are frequently experienced during orthodontic treatment, including separation, initial archwire placement, adjustment or change, and debonding. It has also been reported that every tenth orthodontic patient fails to complete treatment because of the pain experienced during care. This also occurs when so-called noncompliance appliances are used.
To address this, it is necessary to consider other techniques including orthodontic microimplants. To date, few data are available with regard to pain associated with microimplants. To understand patient compliance and acceptance, it is not sufficient to only analyze treatment effectiveness, but the extent to which patients can or are willing to tolerate pain during the proposed treatment option must also be determined.
Rating scales are widely accepted and validated tools that are reliable for assessing patients’ discomfort or pain during treatment. They can be continuous (visual analog scale [VAS]), discrete (numerical rating scale [NRS]), or verbal (VRS). All 3 pain-rating scales are valid, reliable, and appropriate for use in clinical practice. Because differences in the VAS score seem to be clinically significant only in the 20% range, a discrete 5-category NRS was chosen for this study.
Previous studies concentrated on comparing pain and discomfort associated with microimplant treatment with other potentially painful procedures including extractions, other interventions, or various anchorage devices. The aim of this study was to compare the pain associated with microimplant placement and various dental procedures routinely accompanying placement. The procedures were microimplant placement, soft-tissue preparation by punch excision, and tooth extractions. Even though these techniques are common in orthodontic practices, the comparative pain associated with them has not been investigated to establish to what extent these techniques are tolerated by patients or how they will be ranked in a comparison.
Material and methods
Twenty-eight consecutive orthodontic patients fulfilling the inclusion criteria were recruited (mean age,14.94 ± .95 years; 14 girls, 14 boys) for this study. The inclusion criteria were that they were in the permanent dentition, were less than 18 years of age, had an orthodontic treatment need that included a treatment plan involving maxillary or maxillary and mandibular premolar extractions, needed en-masse retraction to reduce an excessive overjet, and had maximum anchorage requirements. The sample was taken from patients referred for orthodontic assessment in a private specialist (M.B.) practice.
Information about the treatment and the study was given orally and in writing to all patients and their parents. Also, written consent was obtained from all selected patients and their parents. The patients were randomized and stratified by sex into 2 groups. Group A comprised 7 boys and 7 girls; group B also had 7 boys and 7 girls. In group A, at least 1 extraction was performed before placement of the microimplant. In group B, all extractions were performed after placement of the microimplant ( Table I ).
| A Extraction before placement | B Extraction after placement | ||
|---|---|---|---|
| ia | ib | ia | ib |
| Soft-tissue punch, left side | Transgingival placement, right side | Soft-tissue punch, left side | Transgingival placement, right side |
All microimplants were placed into the interradicular area of the maxillary second premolar and first molar in both maxillary quadrants. For all patients, the Tomas pin (length, 8.0 mm; diameter, 1.6 mm; Dentaurum, Ispringen, Germany) was used.
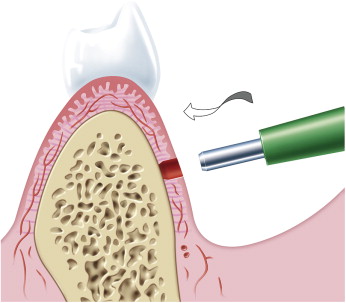
Two placement techniques were used for each patient ( Table I ) in a split-mouth design. On the left side, the Tomas punch (diameter, 2.0 mm; Dentaurum) was used for gingival tissue removal in the placement area ( Figs 1 and 2 ). On the right hand side, the microimplant was transgingivally placed.

Tooth extraction and microimplant placement were performed on consecutive days by different operators. The teeth were extracted by each patient’s local dentist, and all microimplants were placed by 1 orthodontist trained in implant placement.
For anesthesia, a superficial injection was directly applied in the placement area by using 0.2 mL Scandonest (3% mepivacaine hydrochloride; Septodent, Niederkassel, Germany).
The quadrant for the first placement was randomly chosen to prevent bias because of the patient’s anxiety. Also, the patient was not informed which technique was used for which side.
During the interview, the term microimplant was replaced by pin to reduce anxiety in the patients. Before treatment, all patients were asked about their expectations. Immediately after the microimplant placement, they were asked about pain and discomfort during the procedure and to what extent their expectations had been fulfilled. One day after treatment, the preferences in gingival tissue removal and transgingival placement were evaluated. A standardized questionnaire containing 12 items was used for the evaluation ( Fig 3 ). The interviewer was neither involved in nor informed about the clinical procedure to prevent bias.

Statistical analysis
Differences between the groups were tested with the nonparametric Kruskal-Wallis and Mann-Whitney tests for pain and discomfort. The chi-square test was used to determine differences between the procedures. To compare the pain levels of extraction, soft-tissue punch, and transgingival placement, the Wilcoxon test was used.
Differences at P <0.05 were considered statistically significant.
Results
All 28 patients completed the questionnaire, for a response rate of 100%.
The expectations ranked from mild pain to great pain, but, after treatment, most patients described the experience as less painful than expected.
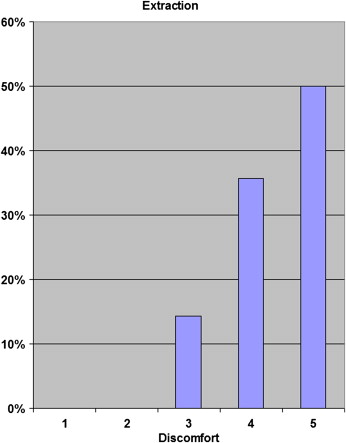
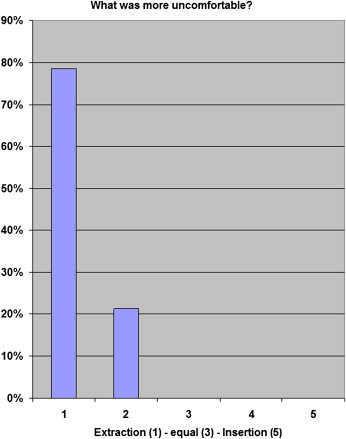
The highest pain values were reached during the extractions, with 50% of the patients describing great discomfort ( Fig 4 ). All patients stated that extractions were more uncomfortable than microimplant placement ( Fig 5 ).
There were no statistically significant differences between groups A and B in the comparison of the pain levels of gingival tissue removal and microimplant placement. No differences were observed between extractions before or after placement of the implants.
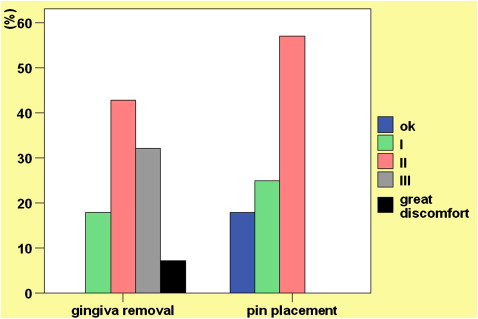
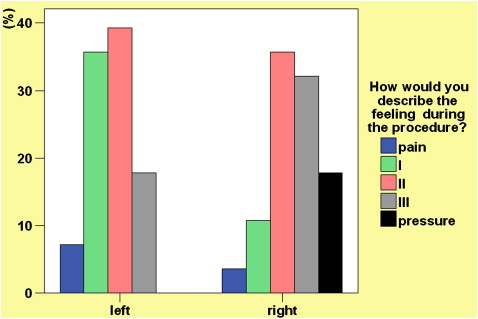
The soft-tissue punch caused significantly higher discomfort levels compared with transgingival placement ( P = 0.002; Fig 6 ). Also, the feeling of the soft-tissue punch side (left) was significantly more often described as painful, but the feeling on the right (transgingival placement) was described as pressure rather than pain ( P = 0.036; Fig 7 ).
This led to a significant preference for the transgingival procedure ( P = 0.002; Fig 8 ).
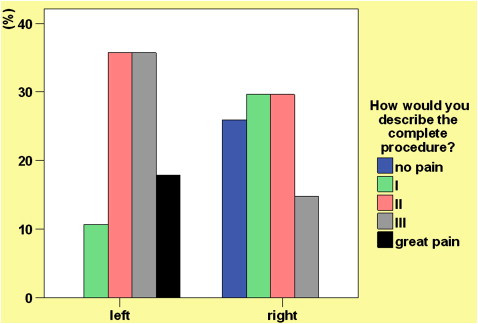
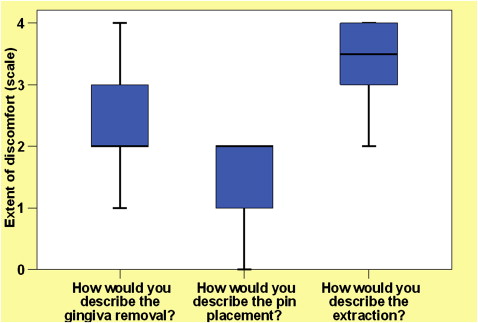
When the 3 interventions were compared, extractions caused the greatest discomfort, followed by the soft-tissue punch. Transgingival placement produced the least discomfort. These results were also statistically significant ( Table II ; Fig 9 ).
| 3. How would you describe the gingiva removal? | 4. How would you describe the pin placement? | 5. How would you describe the extraction? | |
|---|---|---|---|
| Valid (n) | 28 | 28 | 14 |
| Missing (n) | 0 | 0 | 14 |
| Mean | 2.29 | 1.39 | 3.36 |
| Median | 2.00 | 2.00 | 3.50 |
| SD | 0.85 | 0.79 | 0.75 |
| Minimum | 1 | 0 | 2 |
| Maximum | 4 | 2 | 4 |
| 4. How would you describe the pin placement? 3. How would you describe the gingiva removal? | 5. How would you describe the extraction? 3. How would you describe the gingiva removal? | 5. How would you describe the extraction? 4. How would you describe the pin placement? | |
|---|---|---|---|
| Asymptotic significance (2-sided) | 0.001 | 0.003 | 0.002 |