Chapter 4
Evidence-based Guidelines
Aim
The aim of this chapter is to define guidelines, highlight key guideline resources and introduce questions for the appraisal of guidelines.
Outcomes
After completing this chapter readers will be able to define guidelines, be aware of a number of resources to find guidelines and have eight simple questions to help them decide whether to trust a guideline.
Understanding Guidelines
“Guidelines are systematically developed statements which assist in decision making about appropriate health care for specific clinical conditions” (Field and Lohr, 1990).
Well-developed guidelines will have gone through at least the first three stages of the five-stage evidence-based process (Ask, Acquire, Appraise, Apply and Assess). Some will even provide information on when they should be applied and how you assess your outcomes. In this chapter we take you through where to look for them and how to decide if they can be trusted.
Let us consider the first two scenarios outlined in Chapter 3, and apply the evidence-based method.
Scenario A
A mother with two older children who have had experience of dental decay resulting in fillings and extraction wants to know how the same can be prevented in her newborn (Fig 4-1)?
Fig 4-1 Scenario A, prevention of decay.
Scenario B
It is Friday afternoon. An adult patient who is an irregular attender presents with history of a dull throbbing pain in a filled tooth that is tender to percussion. The patient is keen to retain the tooth and is going away for the weekend (Fig 4-2).
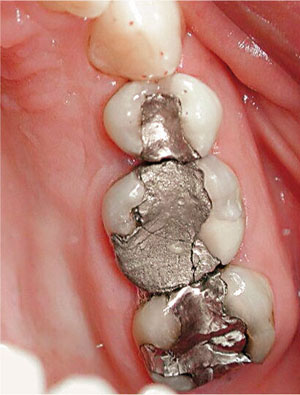
Fig 4-2 Scenario B, pain in a filled tooth.
First we need to confirm what the question is – the ASK stage.
While the question in scenario A may seem obvious to the experienced practitioner, it may not necessarily be the question to which the patient actually needs an answer. For example, in this case the questions the mother might want answered are:
-
When should I start brushing my child’s teeth?
-
When should children start brushing their own teeth?
-
Should I use fluoridated toothpaste?
-
How much toothpaste should I use?
-
Should I use fluoride tablets?
-
What about fluorosis?
-
Can my child have sweets?
-
What foods and drinks should I avoid giving my child?
-
Is there anything the dentist can do to help?
-
What about my older children?
PICO (PECO)
A useful method of clarifying the question is to use the PICO format (Richardson et al., 1995). PICO is a useful acronym that describes the elements of a well-formed clinical question about therapy. The letters stand for:
-
Population, patient or problem
-
Intervention or treatment, or Exposure or potential risk factor
-
Comparison
-
Outcome
Population is really a general description of the group to which your patient belongs, and may include age, gender, race, ethnicity and stage of disease. The description should be specific enough to be helpful, but not overly specific. You are unlikely to find studies of “Asian 63-year-old women” (too specific); describing the population as “post-menopausal women” is much more likely to be helpful. When reading or searching for clinical evidence, this term helps you determine whether you can apply the evidence you find to the group of patients you deal with on a regular basis.
Intervention/exposure is a description of the test or treatment (or exposure to a potential risk factor) that you are considering. This is the most useful term to use when searching databases or websites for the best available evidence.
Comparison is the alternative intervention or exposure. It may be the current gold standard treatment, a placebo or watchful waiting (i.e. monitoring, no treatment). Not all questions need a comparison but, in terms of treatment, the only way we can be certain that a new method or material is better than what we are currently using (or than nothing at all) is to use a comparison group.
Outcome refers to what we are expecting to find as a result of the treatment or exposure. Are you looking to see an improvement in the quality of life, a reduction in dental caries, an association between a potential cause and effect, or whether a new diagnostic test adds to the confidence of your diagnosis?
Most research studies deal with clinical outcomes like millimetres of probing depth or bond strength, but the outcome should be something that not only matters to you but matters to the patient too. (Do patients really care if you can reduce their probing pocket depths by 0.68 mm? Or are they more interested in how long they can keep their teeth?)
Defining the outcome is not necessarily helpful in searching for the answers, but once you find some studies that look at this question, you can eliminate (not have to read!) the ones that don’t deal with the outcome of interest.
Scenario A
| A mother with two older children who have had experience of dental decay resulting in fillings and extraction wants to know how the same can be prevented in her newborn. | |||
| Population | Intervention | Comparison | Outcomes |
| Pre-school children | Caries prevention methods
|
||
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


