Introduction
Achieving a smooth enamel surface after orthodontic bracket debonding is imperative. In this study, we sought to compare the enamel surface roughness values after orthodontic bracket debonding and resin removal using a white stone bur, a tungsten carbide bur, and a tungsten carbide bur under loupe magnification.
Methods
Thirty sound premolars were randomly divided into 3 groups, and their buccal surfaces were subjected to atomic force microscopy to measure initial surface roughness. Brackets were bonded to the buccal surfaces and debonded after 24 hours. Resin remnants were removed using a white stone bur, a tungsten carbide bur, or a tungsten carbide bur under loupe magnification. The teeth were then subjected to atomic force microscopy again. The time required for composite removal was calculated. Data were analyzed using repeated-measures analysis of variance, 1-way analysis of variance, and the Tukey test.
Results
Resin removal increased the enamel surface roughness compared with the initial values ( P <0.001); however, no significant differences were noted among the 3 groups in this respect after resin removal. The mean times required for smoothing by the tungsten carbide bur and the tungsten carbide bur with a dental loupe were similar ( P >0.05): significantly lower than the time with the white stone bur (both, P <0.001).
Conclusions
The tungsten carbide bur is still recommended for composite removal.
Highlights
- •
We compared enamel surface roughness after bracket debonding using 3 methods.
- •
Resin removal led to increased enamel surface roughness.
- •
No significant differences were noted in surface roughness with different burs after resin removal.
- •
Significant difference was observed in the time required for enamel smoothing among various burs.
A major concern when removing orthodontic brackets is restoration of the enamel surface to the pretreatment condition. The quest for an efficient method to remove adhesive resin after debonding of orthodontic brackets has led to the introduction of various techniques and instrumentations. Mechanical removal of composite resin includes scraping with a scaler and various burs, such as ultrafine diamond burs, but some believe that they can cause irreversible damage to the enamel. Other studies have shown that laser energy may be used for resin removal, since it degrades the resin and reduces the force needed to remove orthodontic attachments. However, the Er:YAG laser also has been shown to cause irreversible enamel damage.
Using different burs in conjunction with rubber cups and pumice paste seems to be appropriate for resin removal; however, there is a considerable lack of consensus regarding the most efficient route for this. Tungsten carbide burs in either a low-speed or a high-speed hand piece have been the method of choice for removing resin remnants. Techniques and new composite burs that are less aggressive to the enamel and new instruments such as stone burs, disks, and diamond or silicone coated polishers, also stated to be less aggressive, have been developed. The effect of various rotary instruments on the enamel surface has been assessed qualitatively with scanning electron microscopy. However, using quantitative scales enhances the selection of the most efficient method because of the possibility of better assessing and comparing the damage caused by different instruments.
The atomic force microscope (AFM) is a scanning probe microscope with biologic applications. It uses a flexible cantilever as a type of spring to measure the force between the tip and the sample. The AFM analysis uses several high-resolution scans and is highly recommended for evaluation of the enamel surface. Minimal sample preparation, obtaining 2-dimensional and 3-dimensional images simultaneously and the possibility of reevaluating the sample are among the advantages of this method. It has been stated that the use of a dental loupe by the practitioner may affect the quality of the debonding procedure, causing less enamel damage and better resin removal. To date, multiple modalities have been advocated and used to remove adhesive residues after debonding; a large disparity exists in the literature regarding the most efficient way to remove resin after orthodontic treatment. Therefore, we undertook this study to compare the effect of 3 resin removal methods (tungsten carbide bur, white stone bur, and tungsten carbide bur under loupe magnification) on enamel surface roughness assessed by AFM. The time taken for resin removal after bracket debonding was also evaluated.
Material and methods
In this in-vitro experimental study, 30 freshly extracted (for orthodontic indications) intact premolars were obtained from 10- to 20-year-old patients. The teeth were stored in distilled water before they were sent to the laboratory and cleaned with a low-speed bristle brush. They were then rinsed with water for 10 seconds and dried with oil-free compressed air. The experimental teeth were mounted in acrylic blocks and stored in isotonic saline solution. The teeth were not sterilized (since sterilization could affect the quality of the bond).
The buccal surface roughness of each tooth was determined by AFM (NanoWizard II; JPK Instruments, Berlin, Germany; Fig 1 ), equipped with a scanner with a maximum range of 100 ×100 × 5 μm in the x, y, and z axes, respectively.

To measure roughness values, the tip of a silicon probe (with a radius of less than 10 nm, height of 4-6 μm, and spring constant of 0.046 N/m) was moved across the middle third of the buccal surface of the samples in the contact mode with 10 −6 N force. In the contact mode, the tip never left the surface. After obtaining 2 to 3 initial images (20 × 20 × 5 μm), 5 images of each specimen (5 × 5 × 5 μm) were extracted from the initial images via blind randomization. Then the teeth were etched for 30 seconds using 37% phosphoric acid gel, rinsed with water, and air dried. The brackets were bonded to the prepared enamel (Reliance Orthodontic Products, Itasca, Ill), excess adhesive was removed, and the resin was light-cured for 40 seconds ( Fig 2 ). All samples were stored in isotonic saline solution at room temperature for 24 hours, and the brackets were debonded with a fine cutter using the peeling method. The teeth were randomly assigned to 3 equal groups with 10 teeth in each group. In the first group, removal of resin remnants was performed with a 12-bladed tungsten carbide bur (0197; D & Z, Frankfurt, Germany) and a low-speed hand piece.

In the second group, a dome-shaped white stone bur (Arkansas 661 DEF; D & Z) in a low-speed hand piece was used for resin removal.
In the third group, removal of resin remnants was performed with a 12-bladed tungsten carbide bur as in the first group, but during the debonding process the operator used a dental loupe (binocular loupe, HR 2.5 × 420 mm; Heine, Dover, NH). All bonding and debonding processes were done by the same operator. Composite resin remnants were completely removed and verified by visual inspection by the operator under a dental operating light.
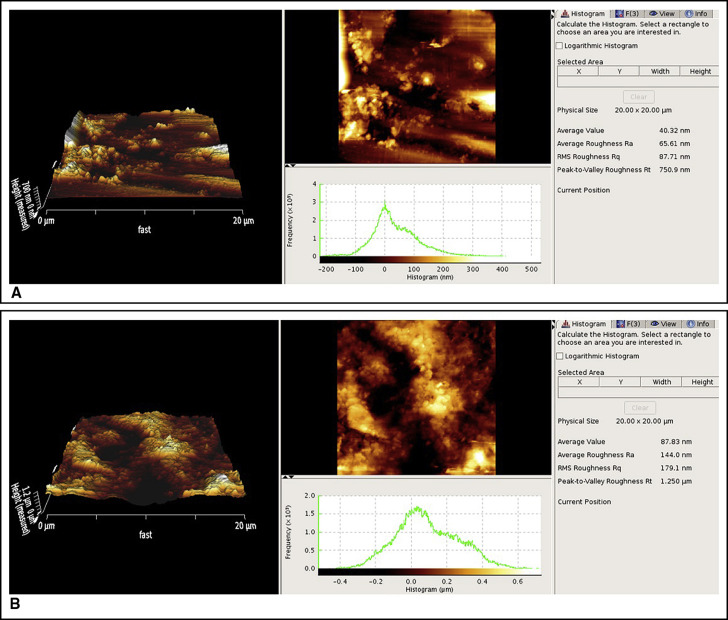
Different parameters of enamel roughness were determined by AFM ( Fig 3 ): (1) average roughness value (Ra), the arithmetic mean of the height of peaks and the depths of valleys from a mean line in nanometers; (2) root mean square roughness (Rq), the height distribution relative to the mean line in nanometers; and (3) maximum roughness height (Rt), representing the isolated profile features on the surface.
The duration of composite removal was also calculated and statistically analyzed by 1-way analysis of variance (ANOVA) and the Tukey post hoc test. The level of significance was set at 0.05. Roughness parameters were statistically analyzed by repeated-measures ANOVA. If we had only 1 group in a before-and-after design, we would analyze the data using paired-samples t tests. But in this study, we had 2 independent variables including times (before, after) and groups (tungsten carbide, white stone, and tungsten carbide under loupe magnification). To control the type I error of statistical tests, we used repeated-measures ANOVA.
Results
Composite resin removal increased enamel surface roughness compared with the initial values in all 3 methods. The Ra, Rq, and Rt values showed significant changes after composite removal in all 3 groups compared with the baseline values ( P <0.0001).
No significant differences were noted among the different burs regarding Ra ( P 0.9), Rq ( P = 0.14), and Rt ( P = 0.29) after composite resin removal ( Figs 4-6 , respectively). Number 1 ( blue line ) in Figures 4 through 6 represents the values before debonding, and number 2 ( green line ) shows the values after debonding. According to the Tukey post hoc test, the mean values of time required for resin removal with the tungsten carbide bur and tungsten carbide bur under loupe magnification were similar (34.2 and 33.6 seconds, respectively) and were significantly lower than the time for the white stone bur (56.6 seconds; both, P <0.0001; Table ). The difference between the tungsten carbide bur and the tungsten carbide bur under loupe magnification was not statistically significant ( P >0.05).




