The treatment of skeletal anterior open-bite malocclusion requires complex orthodontic planning that considers its multifactorial etiology, treatment limitations, and high relapse rates. This case report illustrates a successful treatment approach for a skeletal high-angle Class II malocclusion in an adult with a severe open bite. The treatment consisted of a high-pull headgear therapy after mini-implants failure during fixed orthodontic therapy. Adequate esthetics and function were achieved. Despite its low probability, the unexpected event of mini-implant loosening during complex treatments should be considered. Therefore, classic orthodontic mechanics should be established, especially when treating patients for whom invasive procedures such as miniplates or orthognathic surgery are not available options.
Highlights
- •
A dentoalveolar orthodontic camouflage of a severe open bite in an adult patient is described.
- •
A high-pull headgear was implemented due to subsequent mini-implants loosening episodes.
- •
Adequate esthetics and function were achieved.
- •
The 23-month follow-up showed the stability of this treatment modality.
Skeletal anterior open-bite malocclusions require a complex orthodontic therapy that considers their multifactorial etiology, treatment limitations, and high relapse rates. A rigorous investigation of the open-bite etiology is the first step toward the treatment plan. The classical factors associated with this condition include functional factors (inappropriate muscle growth or activity, neurologic and respiratory disabilities), habitual factors, and dental and skeletal components. High-pull headgear, vertical chincups, posterior bite-blocks, habit-breaking appliances, fixed appliances, and orthognathic surgery are some traditional treatment modalities reported. The patient’s age is a determinant for treatment once, in the early stages, it is possible to control the vertical growth of the alveolar process and the consequences of oral habits. The main limitation of conventional orthodontics in nongrowing patients is the establishment of a rigid anchorage for molar intrusion, which normally calls for a surgical-orthodontic approach to intrude the posterior maxillary arch segments, reducing the lower facial height.
Skeletal anchorage systems provide an alternative for less invasive treatment of patients with severe anterior open-bite malocclusions because of the possibility of occlusal and mandibular plane alterations upon the intrusion of posterior teeth. With this system, it is possible to control the anterior tooth extrusion, which is more susceptible to root resorption and relapse. Successful outcomes have been reported concerning the treatment of anterior open-bites with mini-implants and miniplates.
This case report illustrates a 23-month follow-up of a nonsurgical approach for a patient with a high-angle skeletal Class II open-bite malocclusion. She was treated with premolar extractions and posterior tooth intrusion with mini-implants that failed during maxillary incisor leveling and were replaced by a hyrax expander associated with high-pull headgear.
Diagnosis and etiology
A young woman, aged 18 years and 11 months, sought treatment in the Department of Orthodontics at the Federal University of Rio de Janeiro in Brazil, with an anterior open bite and symptoms of temporomandibular disorders; she reported occasional pain in the temporomandibular joints (TMJ) during mastication. During the TMJ clinical examination, bilateral crepitation and pain upon masseter muscle palpation were observed. There was history of a pacifier sucking habit until the age of 7 years. At initial orthodontic appointment, she did not report any medical intercurrence, and she was not taking any medication. However, 1 year later, she underwent medical treatment for a nutritional deficiency. She weighed 43 kg and was 1.61 m tall.
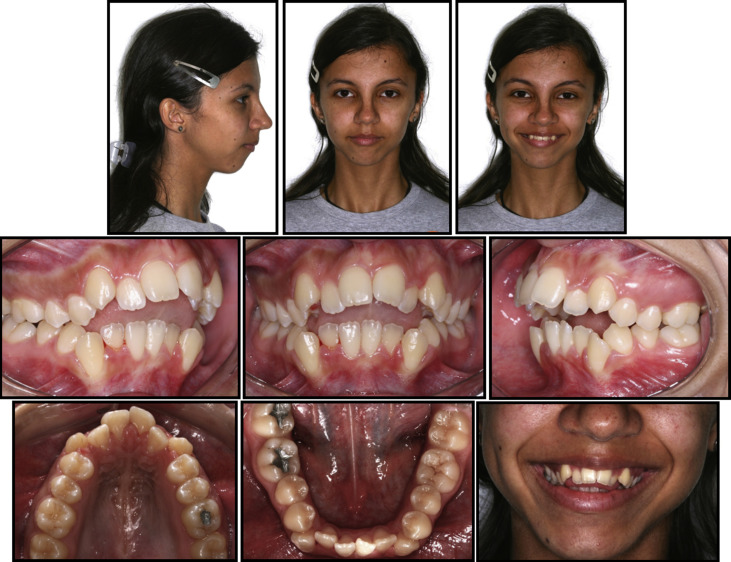
Initial facial analysis indicated vertical growth with mild facial asymmetry toward the right side, a convex profile, increased lower facial third, and the absence of passive lip sealing with increased mentalis muscle activity with closed lips ( Fig 1 ). As for the functional aspects, there was improper tongue posture with atypical speech and swallowing. The intraoral clinical examination and analysis of the initial cast models showed an Angle Class II Division 1 malocclusion, maxillary and mandibular anterior crowding (9 mm), V-shaped maxillary and quadratic mandibular dental arches, overjet of 9 mm, and anterior open bite of 5 mm. The maxillary and mandibular dental midlines were deviated 0.5 mm to the left and 2 mm to the right from the facial midline, respectively ( Figs 1 and 2 ; see Video 1 , available at www.ajodo.org ).