Fig. 7.1
(a, b) Esthetically pleasing smile with papilla that fills the entire embrasure
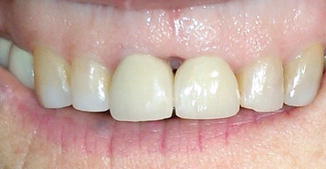
Fig. 7.2
A “black triangle” between maxillary central incisors
Pretreatment periodontal evaluation and accompanying strategic operative planning is essential to avoid postoperative esthetic complications. Specific periodontal parameters should be recorded and include the following:
1.
Signs of periodontal inflammation at the surgical site in terms of pocket depths, bleeding upon probing, color, and contour of gingival tissue.
2.
Attachment loss.
3.
The location and measurement of the mucogingival junction along with measurement of the width of attached gingiva.
4.
The position and inclination of the root and thickness of bone over the root.
5.
Patient biotype: generally speaking, a thin gingival biotype has greater potential for gingival recession when compared to a thicker gingival biotype.
For the patient that exhibits periodontal disease (Fig. 7.3), treatment of the periodontium should be completed before endodontic surgery [2]. With these periodontal parameters in mind, the endodontic surgeon must consider the patient’s esthetic demands along with an evaluation of the quality and type of restoration particularly as it relates to the position of the margin to the gingiva. This represents a critical component of treatment planning especially as it relates to a good esthetic outcome. Finally, these clinical findings must also be considered in the context of location and extent of the existing periradicular pathosis before incision and selection of surgical flap design.
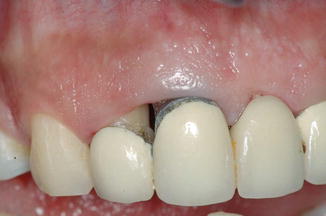

Fig. 7.3
Pretreament presentation of periodontal disease
Even with careful consideration of the pretreatment periodontal condition, it has been shown that an ongoing endodontic infection represents a contributing factor for marginal attachment loss after endodontic surgery [2].
Application of Microsurgical Techniques for Prevention of Esthetic Complications
Endodontic microsurgery fundamentally represents the refinement of established and recognized surgical principles by incorporating technology to improve visualization. This is accomplished primarily with the utilization of the operating microscope along with the development and use of microsurgical instrumentation. There are three important principles that are incorporated in endodontic microsurgery [9, 10]:
1.
The improvement of motor skills which translates into the enhancement of surgical ability
2.
Wound closure by exact primary apposition of the wound edge
3.
The adjunctive development and utilization of microsurgical instrumentation
The goal of the endodontic surgeon is to cause minimal tissue damage and provide the environment for primary healing which contemplates gentle handling of both hard and soft tissue with accurate wound closure. Understanding, training, and experience in endodontic microsurgery will allow the surgeon to achieve both excellent treatment outcomes with highly esthetic clinical results.
For the surgeon who practices without an operating microscope, a willingness to adapt this level of magnification is necessary. Surgical magnification will tremendously enhance motor skills which will translate into the enhancement of surgical ability [11]. In addition, greater attention to surgical esthetics, microanatomy, and tissue handling are critical. While tissue handling and microsurgical instrumentation are discussed in other chapters of this text, the incorporation of endodontic microsurgery requires the discussion of some aspects of hand function.
Hand Support and Control
It is well understood that unsupported finger movements in extension or flexion are relatively unstable and not suited for endodontic microsurgery [10, 12]. Therefore, wrist stabilization on a fixed surface with a 20° angulation in dorsiflexion decreases muscle tremor and mitigates unsupported finger flexion and extension thereby providing finely controlled finger movements [10, 12].
Physiologic hand tremor is not unusual and a manifestation of intentional and unintentional actions causing hand and finger movement [13]. The realization of a surgeon’s tremor becomes more obvious with visual enhancement of magnification. It typically is associated with tension generated by poor postural control, unsupported hand, and unstable instrument holding position, but several other factors have been associated with hand tremor such as cigarette smoking, alcohol withdrawal, caffeine, hypoglycemia, hyperparathyroidism, pheochromocytoma, and Wilson’s disease. Drug-induced hand tremor is a nervous system and muscle response to certain medications which include valproic acid, albuterol, cyclosporine, lithium carbonate, tricyclic antidepressants, antivirals such as acyclovir, and certain blood pressure drugs [14]. To perform endodontic surgery with microsurgical techniques and to minimize hand tremors, the surgeon must be in a relaxed and proper mind-set. To perform highly esthetic results, the endodontic surgeon must consider his/her attitude with mental focus and patience in order to maintain precise motor skills [10, 11].
Hand: Instrument Grips
It is interesting to consider that with the rapid expansion and utilization of technological advances of computers and even text messaging on handheld mobile devices, there is very little emphasis on handwriting or penmanship. In an academic setting or for the contemporary specialist dentist trainee, this lack of emphasis provides little background for good ergonomic habits during training [11, 15].
The three-digit pen or internal precision grip is the most commonly utilized in microsurgery and provides excellent stability particularly when compared to other hand grips [9, 16]. As its name suggests this grip mimics a three-digit pen grip with the thumb, index finger, and middle finger creating an effective tripod [9]. The surgeon’s hand should rest on an immovable flat surface with support of the ulnar surface of the wrist and forearm. With this tripod in place, the instrument is supported by the middle finger with the thumb and index finger placed in contact with the instrument. Opening and closing of an instrument requires very fine movements, and any possible tremor is minimized. By utilizing the pen or internal precision grip, the flexor and extensor muscles of the hand remain relaxed facilitating accurate movement. Finally, proper surgical ergonomics not only helps prevent back and neck problems; it provides the functional environment to properly perform endodontic microsurgery and prevent esthetic complications. The patient and chair position should be adjusted to the surgeon and microscope with the surgeon seated in an upright position with thighs approximately at a right angle to the knees [17].
Microsurgical instrumentation, accurate hand movement with precision hand grip, and correct posture and position of the endodontic surgeon (Fig. 7.4) are critical factors in avoiding esthetic complications.
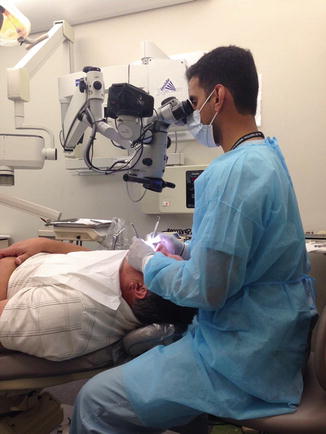

Fig. 7.4
Posture and position of the endodontic surgeon
Tissue Management and Esthetic Considerations
Surgical access has been cited as a major point of concern in endodontic surgery [18]. Appropriate selection of flap design enables proper access reducing the time needed in surgery and thus reducing postoperative morbidity. Poor flap design may lead to failure in treating the pathology or to unsightly hard and soft tissue defects leading to unhappy patients (Fig. 7.5). With the introduction of the surgical operating microscope, microsurgical techniques have evolved to improve the handling of soft tissues and reduce the incidence of defects [19].
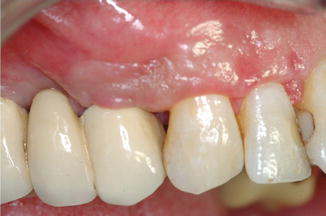

Fig. 7.5
Esthetic consequences of poor flap design and incision
Incisions should be made in smooth continuous motions pressing the blade to the bone in order to follow the topography of the hard tissue maintaining a full thickness cut. Discontinuous motions lead to jagged irregular edges more likely to leave noticeable scarring [20]. Full thickness flaps are desirable in endodontic surgery as it is essential to have direct access to the bone in order to gain access to the root in question. A full thickness mucoperiosteal flap consists of the marginal, interdental, and attached gingiva, alveolar mucosa, and periosteum [20–22]. This flap reduces the risk of tears and perforations, and upon closure, the periosteum immediately begins to reattach [22]. Furthermore, incisions should be long enough to provide adequate tissue to reflect so that unnecessary tension is not placed on the soft tissue. Tears of the tissue heal more slowly and leave greater scars as approximating the margins becomes more difficult, and associated healing occurs by secondary rather than primary intention [21, 22].
Intrasulcular releasing incisions are full thickness cuts directed toward the crestal bone. This incision is used in full mucoperiosteal flaps such as triangular-, rectangular-, trapezoidal-, and in papilla-base flap designs. The contraindication of this approach is the presence of a dehiscence [23]. A full thickness incision at a point of dehiscence may damage root attachment fibers leading to localized chronic periodontal disease [23]. This is one indication for a split thickness design to preserve gingiva in the compromised location. A split thickness flap will provide a suitable surface for reattachment of the flap, but this is a technically challenging approach. The split thickness flap is contraindicated in areas of normal bone as the incision has a greater likelihood of damaging the supraperiosteal vessels [7]. A simpler alternative is the use of limited mucoperiosteal flaps such as the Luebke-Ochsenbein flaps that place right-angle incisions apically to the dehiscence. But remember, horizontal incisions should always be made leaving at least 2 mm and more ideally 3–4 mm of attached gingiva [24–26
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


