Fig. 1.1
Diagram depicting an endodontically treated tooth restored with a fiber post, a core buildup, and a crown. Co core buildup, Fe ferrule effect, Gp residual gutta-percha, Fp fiber post
Restorative considerations for endodontically treated teeth always include maintaining an effective coronal seal, protection of the remaining tooth, and restoration of both function and esthetics. Rosen (1961) defined the concept of extra-coronal “bracing” as a subgingival collar or apron of gold extending as far as possible beyond the gingival seat of the core and completely surrounding the perimeter of the cervical portion of the tooth, serving to prevent fracturing of the root. Rosen and Partida-Rivera (1996) tested this using 76 extracted maxillary lateral incisors restored with gold cervical collars and coronally threaded with a post until fracture occurred. The collar significantly reduced the incidence of root fracture. Libman and Nicholls (1995) reported that an increased ferrule length increased the resistance to fracture, while an increased post length did not. One significant consideration in the ferrule design is the influence of biologic width. Fugazzotto and Parma-Benfenait (1984) stated a minimum of at least 3 mm should be left between the crown margin and the alveolar bone in order to avoid impingement on the coronal attachment of the periodontal connective tissue. In consideration of the restorative dimension then required, at least 3 mm of supra-alveolar tooth structure, in addition to ferrule height, may be required to provide an effective restorative dimension (Fig. 1.2).
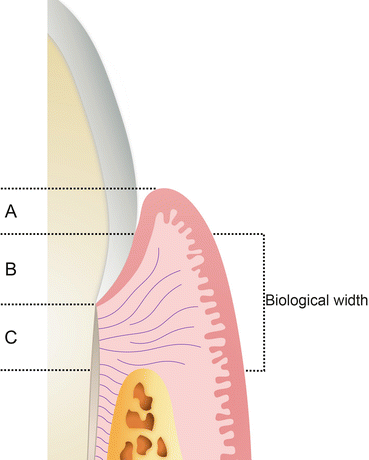

Fig. 1.2
Biological width. A Sulcular epithelium, B junctional epithelium, C connective tissue
Occasionally, the clinician may recommend a crown lengthening procedure on a tooth with inadequate coronal tooth structure for an effective ferrule height and adequate biologic width. In some cases, crown lengthening may compromise the supporting bone of adjacent teeth or the crown to root ratio of the tooth in question. Orthodontic extrusion has been presented as a reasonable alternative to crown lengthening in these situations. However, this procedure may require greater length of treatment. With the potential drawbacks of both crown lengthening and orthodontic extrusion, the clinician may need to decide whether or not to include a ferrule around the entire diameter of the tooth. This clinical alternative was evaluated in a literature review of 62 articles by Juloski et al. (2012). Their findings suggest that if the clinical situation does not allow a 360° ferrule, an incomplete ferrule is considered to be better than the absence of a ferrule. Additionally, including a ferrule lowers the impact of the post and core system, luting agents, and final restoration on the performance of endodontically restored teeth. This study also found that orthodontic extrusion lead to a better prognosis than surgical crown lengthening.
1.4 Alternatives to the Ideal Restoration
1.4.1 Cuspal Coverage Amalgam
Although a full-coverage crown is usually the restoration of choice in posterior teeth, a complex amalgam restoration that covers the cusps has been suggested as a suitable alternative (Starr 1990) (Fig. 1.3). This type of restoration may be indicated in cases in which cost of the crown is prohibitive for the patient or if insufficient tooth structure remains coronal to the crest of bone to maintain biologic width and a crown ferrule. With this type of cuspal coverage restoration, all of the remaining cusps are reduced 2 mm and rebuilt with amalgam. It has also been suggested that, if the pulp chamber height is less than 4 mm, amalgam should be condensed 2–4 mm into each canal to increase the fracture resistance of the amalgam restoration (Nayyar et al. 1980; Kane et al. 1990). Although the long-term prognosis for this type of complex amalgam restoration may not be as favorable as a full-coverage crown (Martin and Bader 1997), Mondelli et al. (1998) found that these cusp-covering amalgam restorations increase the fracture resistance in comparison to endodontically accessed posterior teeth without cuspal coverage. Smales and Hawthorne (1997) also found that complex amalgam restorations had a mean survival rate of 14.6 years. Therefore, this type of restoration can serve as a good intermediate restoration to protect the tooth until the patient can proceed with a crown or crown lengthening if indicated.
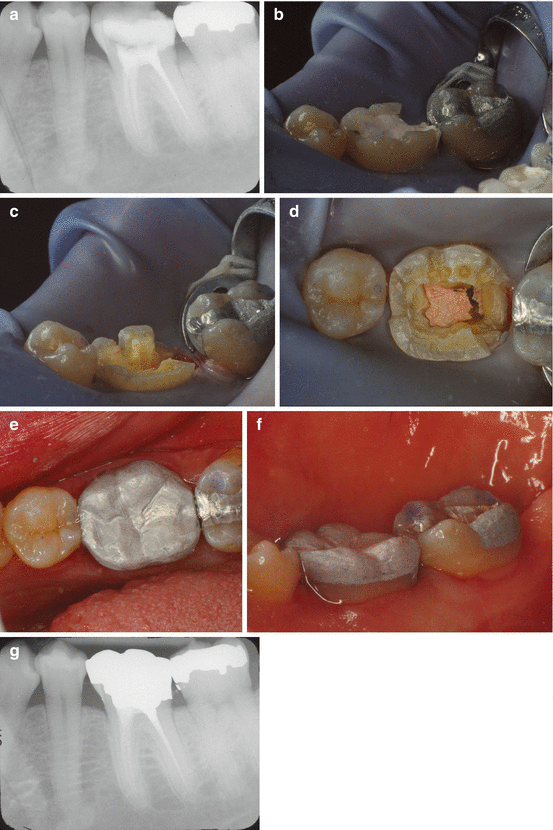

Fig. 1.3
Cuspal coverage amalgam (Courtesy of Dr. Scott B. McClanahan, University of Minnesota School of Dentistry). (a) Radiographic image showing tooth #19 root canal completed and coronal temporary restoration in place. (b) Clinical image showing tooth #19 root canal completed and coronal temporary restoration in place. (c) Temporary restoration is removed, occlusal tooth structure is reduced 2 mm, and mesial and distal box preparations are created. (d) Occlusal view of tooth preparation for amalgam cuspal coverage. (e) Completed amalgam cuspal coverage restoration (occlusal). (f) Completed amalgam cuspal coverage restoration (lingual). (f) Radiographic image showing amalgam cuspal coverage in place. Note amalgam condensed into distal canal for retention
1.4.2 Cuspal Coverage Composite
Like the cuspal coverage amalgam restoration, a composite restoration covering the cusps has also been suggested as an alternative to a crown for endodontically treated posterior teeth. In a laboratory study examining the fracture resistance of endodontically treated molars with direct or indirect cuspal coverage composite restorations, Plotino et al. (2008) selectively covered the mesial cusps and restored the mesial marginal ridges. They found that selectively covering cusps did not restore the strength of the cusps to their preoperative state. However, in an ex vivo study on endodontically treated premolars, Mondelli et al. found that restoring all cusps with composite significantly increased the fracture resistance (Mondelli et al. 2009). Therefore, reducing the entire occlusal surface and all cusps 2 mm and restoring the tooth in composite may offer a suitable option for restoring endodontically posterior teeth especially in the premolar region where a metallic restoration may not be as esthetically acceptable. However, a review of the literature indicates that amalgam is superior to composite for posterior tooth restorations in terms of long-term survivability of the restoration (Kovarik 2009). This may again indicate that a cuspal coverage composite may reinforce the strength of the tooth and serve as a good transitional restoration until a crown can ultimately be placed to protect the tooth long term.
1.5 What Are the Guidelines and Techniques for Post Preparations?
Once it is decided that a post is indicated, the practitioner must consider the timing of the post placement, the design (length, width, taper, etc.), and the best location to place the post within the tooth in question.
1.5.1 Timing of Post Space Preparation
Sequencing of the restoration of endodontically treated teeth may seem straightforward until one considers implementing provisional treatment steps, all while maintaining the integrity of the coronal and apical seals established during endodontic treatment. One such challenge exists with post space preparation. When a post space is determined to be necessary for restoration of the tooth (Goerig and Mueninghoff 1983), there is considerable debate regarding the timing of post space preparation with respect to coronal microleakage and apical seal. Immediate removal of the coronal sections of the root canal filling may be accomplished using heated pluggers or an electronic thermal tip. Delayed post space preparation, however, may require the use of rotary instrumentation in combination with solvent softeners. Earlier studies by Dickey et al. (1982) suggest that immediate post space preparation significantly increased apical leakage due to inadequate sealer setting time. Portell et al. (1982), however, reported that the removal of gutta-percha was more difficult with delayed post space preparation. They hypothesized that this may have contributed to greater apical leakage with delayed post space preparation than with immediate post space preparation in their study. More recent studies have indicated less apical leakage associated with immediate post space preparation, as well as immediate post and core placement (Demarchi and Sato 2002; Solano et al. 2005). With increased acceptance of contemporary obturation techniques, such as continuous warm gutta-percha backfill and the use of resin sealers, it seems prudent for the restoring clinician to consider immediate post space preparation, rather than delayed, given the convenience and timeliness afforded by these material and techniques.
1.5.2 Post Length
The length of the post space preparation is determined by both the mechanical retention requirements and the need to maintain an adequate root canal filling dimension for an apical seal. In vitro studies using pressurized dye leakage systems have suggested caution is advised when making the assumption that a minimal apical obturation dimension is equivalent to the apical seal obtained with the intact root canal filling (Abramovitz et al. 2001). The authors of these studies reported that a retained apical filling dimension of 5 mm was inferior to that of the intact root canal filling. Additionally, reduction of the fillings to 3 mm resulted in an unpredictable seal. Portell et al. (1982) found that 7 mm of remaining gutta-percha in the apical fill resulted in less leakage than 3 mm, reaffirming the need to maintain an adequate apical dimension of root canal filling material.
Occasionally, one is confronted with the dilemma of a short crown-root ratio potentially limiting the apical filling dimension as a compromise to maximizing post length retention form. A novel approach presented by Mavec et al. (2006) incorporates the use of an intracanal glass ionomer barrier to assist in the resistance to microleakage resulting from an inadequate dimension of apical filling material. In this in vitro study, for teeth requiring a post and core that allowed for only 3 mm of remaining gutta-percha, a 1 mm glass ionomer barrier placed over the remaining gutta-percha reduced the risk of recontamination of the apical filling material (Fig. 1.4).
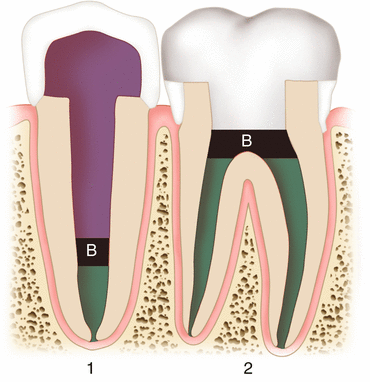

Fig. 1.4
Illustration of intracanal and orifice barriers. (1) Represents an endodontically treated tooth restored with a full-coverage crown, post and core, and use of an intracanal barrier (B); (2) Represents an endodontically treated tooth restored with a cuspal coverage restoration and an orifice barrier (B) (Illustration adapted from Mavec et al. (2006))
In addition to maintaining adequate apical canal filling dimensions, another post length consideration relates to the influence of post fit or “form-congruence” as presented by Schmage et al. (2005). This concept of form-congruence aims to maximize adaptation of the post to the surrounding root canal walls, in order to facilitate stress distribution along the canal wall. This effect was observed in studies by Sorensen and Engelman (1990) with tapered cast post and cores and crowns luted with zinc phosphate cement. This was not, however, observed with parallel-sided posts and post space preparations. There may be an effect of destabilization by creating a post space that transforms a naturally conical canal space into a cylindrical form. Kishen et al. (2004) have suggested that not only the thickness of the dentin wall stabilizes the root but also the presence of inner dentin with a lower elastic modulus than the more mineralized outer dentin. This is particularly important when large diameter post space preparations are created to transform an oval canal into a cylindrical form for the purpose of circumferential post fit, thereby removing critical dimensions of inner dentin. Selecting a post that closely approximates the existing canal form preserves the inner dentin and elastic modulus but may be associated with poor form-congruence. Büttel et al. (2009) reported that the fracture resistance of teeth restored with fiber-reinforced composite posts and direct resin composite crowns without ferrules was not influenced by post fit within the root canal, irrespective of the post length. This implies that excessive post space preparation aimed at producing an optimal circumferential post fit is not required to improve fracture resistance of the root.
1.5.3 Post Placement Complications and Management
Although posts may be indicated in certain clinical situations, the creation of the post space adds a certain degree of risk to the restorative procedure. These risks include contamination of the root canal system, root perforation, and weakening of root dentin leading to vertical root fracture, all of which can affect the long-term prognosis for the tooth.
An important factor in root fracture subsequent to post placement is the reduction of root dentin thickness during post space preparation (Hunter et al. 1989). In a clinical study, Cohen et al. (2003) found that 91 % of diagnosed vertical root fractures were due to inadequately designed posts (either too wide or too long), indicating that the thickness of root dentin had been overly reduced. Therefore, it is important that when creating a post space, the practitioner is as conservative as possible with the removal of dentin to prevent the root weakening due to canal overenlargement (Tjan and Whang 1985). Using solvents, such as chloroform or heat to remove gutta-percha, will facilitate creating a post space without removing additional dentin or affecting the apical seal as compared to rotary removal techniques (Grecca et al. 2009). However, there is evidence that chloroform, and other solvents used to soften gutta-percha (halothane or xylene), may decrease the microhardness of dentin (Rotstein et al. 1999). Therefore, heat may be the safest way to remove gutta-percha for post space preparation, as long as the practitioner is mindful of the possible damage heat can produce on the supporting tissues if the temperature on the external root surface is significantly raised (Eriksson and Albrektsson 1983). Generally, however, electronic heat sources are safe to use within the canal at temperatures of around 200 °C (Silver et al. 1999) and with short (4 s) intervals of heating (Buchanan 2007).
When the canal space has already been subject to overenlargement either by iatrogenic error or by a previous provider, it may be possible to reinforce the root dentin by using a resin-reinforced dowel system (Saupe et al. 1996). By this method, a smooth light transilluminating post is placed into the overenlarged canal space, and resin is compacted around it against the canal walls. The resin is cured by transmitting light through the post pattern. The post pattern is then removed, the post space is refined within the cured resin, and a permanent post is cemented. Saupe et al. (1996) found this technique to increase fracture resistance in endodontically treated thin-walled teeth. There is evidence, though that this strengthening effect may be reduced over time with occlusal forces and as the bond between the dentin and the resin weakens (Heydecke et al. 2001). For more on this technique and concept, see Chap. 5.
When post-preparation burs are misdirected away from the canal space or when large post drills are used in areas of thin root dentin, there is risk that the post drill can perforate the root dentin and create a communication between the canal space and the external surface of the root (Fig. 1.5). In a radiographic study, Kvinnsland et al. (1989) observed that more than half of the perforations noted in their cases were attributed to post-preparation procedures. The main complication that arises from perforations is the potential for secondary inflammatory periodontal involvement and loss of attachment, eventually causing tooth loss (Wong and Cho 1997). Bacterial infection originating either from the root canal or the periodontal tissues, or both, prevents healing and brings about inflammatory reactions in the tooth-supporting tissues. Conditions such as suppurations, abscesses, sinus tracts, and bone resorptive processes may follow (Tsesis and Fuss 2006). It follows that the goal of repairing a perforation is to achieve a tight and permanent seal that will prevent bacteria and their by-products in the root canal from entering the surrounding periodontal tissues. As far as prognosis for the repair of perforations, the chance of healing of the supporting tissues is improved if the perforation is small, if it occurs below the level of the bone, and if it is repaired immediately under aseptic conditions, preventing bacterial contamination (Fuss and Trope 1996).
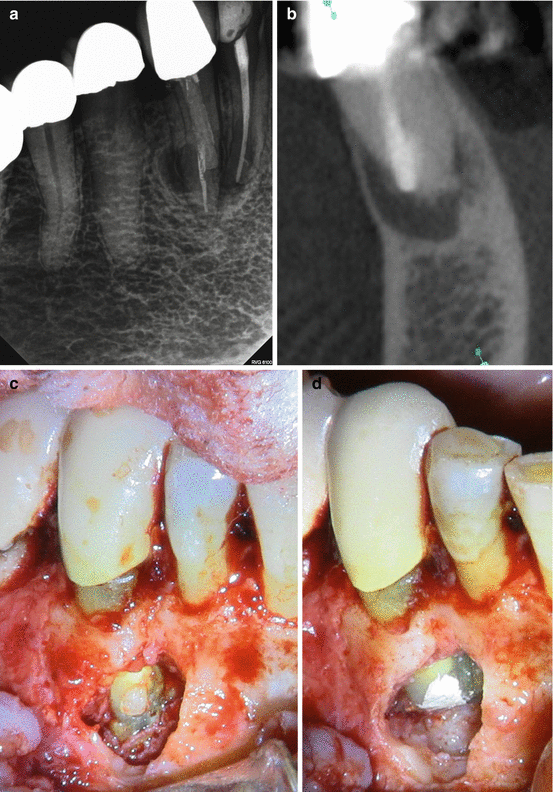

Fig. 1.5
(a) Digital radiographic image of tooth #27 showing fiber post placement mesial to canal space. (b) Cone beam CT image showing post perforating facial aspect of root. (c) Surgical clinical image showing fiber post perforating mesial-facial aspect of root. (d) Surgical clinical image showing root end resection and repair of perforation (Clinical photos attributed to Dr. Cynthia Tyler, University of Minnesota Division of Endodontics)
Materials that have been used to repair perforations include amalgam (Benenati et al. 1986; Balla et al. 1991), gutta-percha (Petersson et al. 1985; Benenati et al. 1986; Kvinnsland et al. 1989), tricalcium phosphate (Sinai et al. 1989; Balla et al. 1991), zinc oxide eugenol (Bramante and Berbert 1987), Super EBA (Bogaerts 1997), dentin chips (Petersson et al. 1985), Cavit (Sinai et al. 1989), hydroxyapatite (Balla et al. 1991), glass ionomer cement (Fuss et al. 2000), and mineral trioxide aggregate (MTA) (Holland et al. 2001). Currently MTA is widely used as a perforation repair material due to results of in vitro studies demonstrating its sealing ability (Nakata et al. 1998; Daoudi and Saunders 2002) and biocompatibility (Hakki et al. 2012) and case reports demonstrating its clinical success in these types of repairs (Arens and Torabinejad 1996; Main et al. 2004; Mente et al. 2010). Biodentine (Septodont, USA) is a calcium silicate-based material that has been recently advocated as another root perforation repair material. Although in vitro studies have shown Biodentine to exhibit biocompatibility (Mori et al. 2014), there is a lack of evidence supporting its clinical success as a perforation repair material at this time (Malkondu et al. 2014). Another recently introduced perforation repair material is Endosequence Root Repair Material (ERRM). Initial investigations have suggested that ERRM may offer a seal superior to that created by MTA (Jeevani et al. 2014) and provide a similar biocompatibility (AlAnezi et al. 2010). Yet again, there are few clinical cases or long-term clinical studies that have been published using this material as a perforation repair material. Therefore, clinical success and long-term prognosis associated with ERRM are unknown at this time.
In some cases, especially in large perforations, it may be difficult to avoid pushing repair materials beyond the root and into the periodontal ligament space, possibly changing the architecture of the supporting structures and impairing the healing process. In these cases, the use of an internal matrix using a biocompatible material has been advocated to help maintain repair materials inside the tooth and preserve the health and structure of the supporting bone and periodontal ligament. This technique, as described by Bargholz (2005), involves placing pieces of resorbable collagen membrane through the perforation and into the defect in bone. The collagen serves to recreate the outer surface of the root. MTA or another perforation repair material can then be layered against the collagen barrier without great risk of extruding the repair material beyond the root surface. After the perforation is repaired, the collagen membrane will be resorbed within a few weeks.
In the case of a large perforation, a perforation as a result of resorption, a perforation that does not heal after nonsurgical repair, or a perforation that is inaccessible from an orthograde approach, surgical repair of the root perforation may be an option (Tsesis and Fuss 2006). Generally this surgical repair consists of a reflecting the gingival tissue, accessing the area of the perforation via osteotomy if necessary, removing any inflammatory tissue around the site of perforation, and repairing the perforation with a perforation repair material, such as MTA, to create a permanent seal. It has also been suggested that guided tissue regeneration, by the use of a bone allograft and a membrane, may promote healing in surgical perforation repair sites where a significant amount of bone was lost due either to the inflammatory process or the osteotomy created to access the perforation area (Dean et al. 1997).
The risk of creating thin root dentin or root perforation is higher in certain teeth or roots where anatomic considerations, such as dentin thickness, canal shape and size, and external root shape are a factor (Sathorn et al. 2005). Mandibular incisors generally have a ribbon-shaped root, with more thickness of dentin in the buccal lingual dimension and very thin dentin in the mesial-distal dimension. With a round post space preparation, therefore, there is risk of thinning or even perforating the mesial or distal root dentin (Gluskin et al. 1995). Maxillary premolars with two roots also present an area of thin dentin on the furcal aspect of the buccal root (Lammertyn et al. 2009), making the palatal root the more ideal location for a post. Similarly, when a post is necessary in a maxillary molar, it is suggested that it be placed in the palatal root due to greater bulk of tooth structure in that root (Schwartz and Robbins 2004); however, the operator must also take into consideration the apical curvature of the palatal root (Bone and Moule 1986). Rigid post drills and posts will not follow root curvatures, so there is risk of perforating at the inner aspect of the curvature if the post drill used beyond the point of curvature. In the mandibular molar, the “danger zone” for perforation is on the distal aspect of the mesial root, just below the furcation (Berutti and Fedon 1992). Therefore, it is generally recommended to place posts in the distal root in these teeth (Schwartz and Robbins 2004). However, recent studies have shown that the furcal aspect of both the mesial and distal roots in the mandibular first molar can present areas of extremely thin dentin (Harris et al. 2013), so again it is advisable to remove as little tooth structure as possible when creating post space in this tooth, even in the distal root.
Additionally, post design can contribute to the risk for root fracture. Active threaded posts induce more stress into the dentin and carry with them a higher risk of root fracture (Felton et al. 1991). Threaded posts, therefore, should only be used in teeth with substantial remaining root thickness (Schwartz and Robbins 2004).
1.6 Coronal Microleakage
1.6.1 Orifice Barriers
Due to time constraints or patient scheduling conflicts, it may not always be possible to place a permanent coronal restoration immediately after root canal obturation. However, in order to provide an environment conducive to healing following root canal therapy, great care must be taken to ensure adequate sealing of coronal and apical structures. If the canal space is not sealed adequately, then microbial organisms, or their toxins, may induce an inflammatory response and lead to persistent disease. Obturated root canal systems may be recontaminated with microbes, or toxins, in various ways. A delay in placing a permanent coronal restoration following root canal treatment may allow coronal microleakage of the temporary filling material to occur. While oxide eugenol materials, such as Cavit (3M ESPE), have good sealing properties, there is a limit to the duration of their effectiveness. Fracturing of the coronal restoration, or tooth, resulting in exposure of the endodontic filling material and preparation of a post space in which the resulting dimension of apical filling material is less than adequate to maintain a seal are additional means of microleakage. The factor that the clinician has the most control over in regard to preventing recontamination of the root canal system is the use of a rubber dam during post space fabrication and coronal restoration. In a recent retrospective study by Goldfein et al. (2013), it was reported that when no rubber dam was used during post placement, 73.6 % of cases were considered successful at follow-up. 93.3 % of cases were considered successful when a rubber dam was used, and this difference was found to be statistically significant.
The impact of coronal microleakage as it relates to clinical outcome is not new. Allison et al. (1979) suggested the possibility that a poor coronal seal might contribute to clinical failure. In the following years, in vitro dye leakage studies by Swanson and Madison (1987) suggested that a significant amount of coronal microleakage is evident after only 3 days of exposure of gutta-percha to artificial saliva. The extent of microleakage in that study was similar at 3 days and 8 weeks, implying that coronal microleakage may be a rapid and significant event. Further studies have reinforced the significance of coronal microleakage. Torabinejad et al. (1990) found that 50 % of single-rooted teeth were contaminated with bacteria along the whole length of the root after 19 days or 42 days, depending on the contaminating microbial species introduced. In another study, Magura et al. (1991) assessed salivary penetration through obturated root canals and found that gutta-percha exposed coronally for up to 3 months should be retreated prior to placement of the definitive restoration. So, while the critical timeframe of coronal microleakage may be debated, the significant impact of adequate coronal seal in preventing microleakage is clearly evident.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


