Introduction
Previous studies have shown that most practitioners plan to maintain intercanine and intermolar widths during orthodontic treatment with fixed appliances. The aim of this study was to determine whether this was put into practice by clinicians during the latter stages of orthodontic treatment with fixed appliances.
Methods
This 2-part investigation was a laboratory-based measurement study at Bristol Dental Hospital, United Kingdom, from 2005 to 2007. Using standardized maxillary and mandibular study models with identical intermolar and intercanine widths but with differing degrees of tooth misalignment, 30 clinicians were asked to fabricate final working archwires according to their normal clinical practice. Then the intercanine and intermolar widths of the archwires were measured. In the second part of the study, the same intra-arch dimensions were measured directly from 50 pretreatment and posttreatment patient study models obtained from a subsample of 10 of the clinicians.
Results
The intercanine and intermolar widths measured on the adapted archwires from the standardized study models showed wide variations in the results, even though the intercanine and intermolar widths of the models were identical. Data from 50 treated patients also showed that, in most, there were wide variations in intercanine and intermolar widths between the patients’ pretreatment and posttreatment study models.
Conclusions
Although most clinicians aim to maintain the pretreatment arch form, this study shows that this is often not transferred to clinical practice.
Changes in tooth position after orthodontic treatment are thought to be caused by either orthodontic relapse as a result of teeth being moved into inherently unstable positions or physiologic changes continuing throughout life. To minimize orthodontic relapse, several treatment conventions have been suggested, including maintenance of the mandibular incisors in their pretreatment position and preservation of the pretreatment arch form.
Arch form is the position and relationship of teeth to each other in all 3 dimensions. Many studies have suggested that, to increase posttreatment stability, the patient’s original arch form should be preserved. No arch form fits all, and although attempts have been made to find a suitable all-encompassing arch form—eg, Bonwill-Hawley arch, catenary curve, and trifocal ellipse —arch forms differ, and therefore customization of archwires is required.
Maintenance of the original intercanine width, intermolar width, and arch length has been found to contribute significantly to a stable posttreatment result. Preservation of the mandibular intercanine width in particular is important because this tends to return, in most patients, to its original value after treatment.
A previous study, with a questionnaire to assess clinicians’ perceptions of the importance of arch form, showed that most clinicians thought it was important to consider and maintain intercanine and intermolar widths when adapting their working archwires. However, when asked what landmarks they routinely used to achieve this—eg, cusp tips or imagined bracket positions—there was no real consensus. Some used only the canines and first molars as landmarks, whereas others used premolars and second molars also when bending their working archwires. There was also considerable inconsistency about the use of study models and symmetry charts. The majority of those who used study models for arch form selection used the mandibular model and later conformed the maxillary archwire to the mandibular archwire (69%). Somewhat surprisingly, others used the maxillary study model to choose the arch form for both archwires (31%).
From the results of the questionnaire study, it was clear that there was no uniformity in how arch form is preserved. So, even if clinicians are carefully adapting their working archwires to preserve arch form, are they actually choosing the correct arch form and dimensions?
The aim of this study was to assess clinicians’ clinical practices when choosing an arch form.
Material and methods
This study was divided into 2 parts, with the first part consisting of a practical component. Instructions consisted of asking clinicians to adjust working archwires as per their normal clinical practice for 3 sets of standardized study models. If they did not normally adjust their archwires, they did not alter them for the study. The resulting archwires were then measured to see whether they corresponded to a predetermined standardized arch form. In the second part of the study, pretreatment and posttreatment study models of a subset of clinicians were measured to see whether they altered the arch forms in routine clinical practice.
The first part of the study, 3 typodonts were set up with acrylic teeth and with Omni arch 0.022-in slot brackets (GAC International, Bohemia, NY) into identical idealized arch forms. To facilitate this, 3 identical sets of maxillary and mandibular 0.018-in Australian stainless steel archwires (A. J. Wilcox, Victoria, Australia) were fabricated and ligated in place on the 3 typodonts. The typodonts were then immersed in warm water to allow the teeth to become aligned by using these same idealized steel archwires; once the teeth were aligned, the typodonts were removed from the water baths and allowed to cool. At this stage, equivalent arch forms and tooth positions were present on each typodont.
The archwires were then removed, and the typodonts were again placed in warm water to allow the positions of the teeth to be altered. In each case, the canines and the molars were left unchanged, whereas the remaining teeth were moved to simulate different arch forms. The intercanine and intermolar widths were measured by using digital calipers (Fowler, Newton, Mass) to ensure that these widths remained unaltered and were comparable among the 3 typodonts.
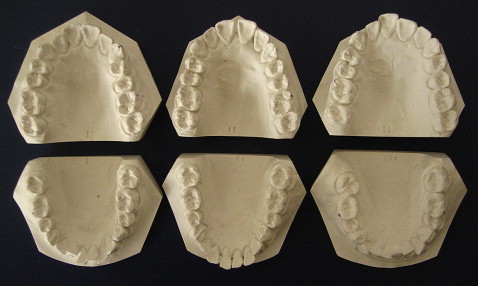
The typodonts were then cooled in cold water, and alginate impressions were taken of each. The impressions were then cast in white stone, trimmed, and lettered (A, B, or C) to mimic pretreatment study models ( Fig 1 ). These study models were presented to 30 clinicians, and it was stated that these patients were nearing the end of treatment. The clinicians were asked to conform 0.019 × 0.025-in stainless steel working archwires using the 3 sets of study models (6 archwires in total), per their usual clinical practice. They were then asked to mark the expected positions of the midpoint of the canines and the mesiobuccal cusps of the first molars on the archwires.
The clinicians could choose from a selection of 0.019 × 0.025-in stainless steel archwires and modify them or not according to their normal clinical practices using the simulated pretreatment plaster models. Both maxillary and mandibular archwires were provided: Orthoform I Tapered, Orthoform II Square, and Orthoform III Ovoid (3M Unitek, St Paul, Minn); and Ideal Form and Accuform (GAC International, Bohemia, NY).
If clinicians did not normally conform their archwires to the study models, they were asked to choose an appropriate arch form and mark the expected positions of the midpoint of the canines and the mesiobuccal cusps of the first molars on this archwire.
Then the intercanine and intermolar widths of the archwires fabricated by the clinicians were measured with digital calipers. This was carried out independently by 2 operators and repeated 1 week later to assess interoperator and intraoperator reliability. In total, 90 maxillary and 90 mandibular archwires were fabricated or adapted and then measured.
The second part of this study was a retrospective analysis of arch dimensions. The intercanine and intermolar widths of 50 pretreatment and posttreatment study models of 50 Class I patients treated without extractions with fixed appliances by a subset of 10 clinicians from a previous trial were measured. Each clinician was asked to submit 5 pretreatment and 5 posttreatment study models for measurement (50 pretreatment and 50 posttreatment models).
The criteria for inclusion of the subjects were Class I incisor relationship, nonextraction treatment, no active expansion, no previous functional treatment, and no headgear. Patients treated with self-ligating brackets were excluded.
Measurements of intercanine and intermolar widths were made on both maxillary and mandibular models at pretreatment and posttreatment. Intercanine width was measured between the canine cusp tips or the expected cusp tips in case of wear. Intermolar width was taken between the mesiobuccal cusp tips of the first molars. In each case, the measurements were made with digital calipers by 2 clinicians on 2 occasions a week apart to assess intraoperator and interoperator reliability. The reported accuracy of the calipers from the manufacturer’s product data sheet was 0.02 mm.
Statistical analysis
The data were analyzed by using Stata software (version 8.2, Stata, College Station, Tex) with a predetermined level of significance of α = 0.05.
For the intercanine and intermolar width measurements with the fabricated or adapted archwires, the data were tested for normality by using the Shapiro-Francia W′ test and, in most instances, were normally distributed. The data were subsequently analyzed and interpreted by using 1-way analysis of variance (ANOVA), means, and 95% confidence intervals (CI) of the mean. Repeatability of measurements, by using intercanine width, was good with the Bland-Altman test, where the mean difference in measurements over the 2 time periods was −0.014 mm, and the 95% CI was −0.09 to 0.06 mm. This good agreement was confirmed by using paired t tests ( P = 0.71).
Summary statistics are given in Table I . The key to the codes is shown in Table II . Means and 95% confidence intervals for the three typodonts with regard to each of the dimensions, upper and lower intercanine and intermolar width are shown in Figures 2 to 5.
| Code | n | Mean (mm) | Median (mm) |
Maximum (mm) |
Minimum (mm) |
SD | 95% CI of mean | Shapiro-Francia W′ |
|---|---|---|---|---|---|---|---|---|
| 1 | 30 | 29.12 | 29.01 | 34.00 | 24.23 | 2.11 | 28.33-29.92 | 0.769 |
| 2 | 30 | 49.63 | 49.53 | 52.24 | 46.70 | 1.32 | 49.14-50.13 | 0.874 |
| 3 | 30 | 37.90 | 37.91 | 40.63 | 32.89 | 1.49 | 37.35-38.46 | 0.013 |
| 4 | 30 | 54.90 | 54.98 | 60.76 | 52.30 | 1.56 | 54.32-55.48 | 0.001 |
| 5 | 30 | 30.92 | 30.92 | 34.40 | 25.29 | 2.03 | 30.16-31.68 | 0.400 |
| 6 | 30 | 49.69 | 49.48 | 53.54 | 46.09 | 1.94 | 48.96-50.41 | 0.960 |
| 7 | 30 | 39.65 | 39.54 | 42.73 | 37.32 | 1.49 | 39.09-40.21 | 0.399 |
| 8 | 30 | 55.23 | 55.15 | 58.00 | 50.70 | 1.53 | 54.66-55.80 | 0.129 |
| 9 | 30 | 28.76 | 28.68 | 33.09 | 25.05 | 1.93 | 28.04-29.48 | 0.943 |
| 10 | 30 | 48.42 | 48.08 | 51.54 | 45.75 | 1.44 | 47.88-48.96 | 0.427 |
| 11 | 30 | 38.97 | 38.82 | 42.48 | 34.41 | 1.62 | 38.37-39.58 | 0.326 |
| 12 | 30 | 55.32 | 55.23 | 60.84 | 52.21 | 1.63 | 54.71-55.93 | 0.020 |
| Code | Model set | Measurement |
|---|---|---|
| 1 | A | Mandibular intercanine width |
| 2 | A | Mandibular intermolar width |
| 3 | A | Maxillary intercanine width |
| 4 | A | Maxillary intermolar width |
| 5 | B | Mandibular intercanine width |
| 6 | B | Mandibular intermolar width |
| 7 | B | Maxillary intercanine width |
| 8 | B | Maxillary intermolar width |
| 9 | C | Mandibular intercanine width |
| 10 | C | Mandibular intermolar width |
| 11 | C | Maxillary intercanine width |
| 12 | C | Maxillary intermolar width |
In the second part of the study with the 50 treated patients, the data for most were not normally distributed, and therefore nonparametric statistics were used. The differences between the pretreatment and posttreatment intercanine and intermolar widths were plotted as box and whisker plots ( Figs 6 to 9 ), and the summary data are presented in Tables III to VI .
| Operator | n | Mean (mm) | Median (mm) | SD | Maximum (mm) | Minimum (mm) | Interquartile range |
|---|---|---|---|---|---|---|---|
| 1 | 5 | −1.54 | −0.81 | 1.31 | −0.31 | −3.4 | −2.40 to −0.77 |
| 2 | 5 | 0.58 | −0.31 | 3.12 | −2.26 | 5.87 | −0.75 to 0.33 |
| 3 | 5 | −1.12 | −0.82 | 0.95 | −2.66 | −0.36 | −1.33 to −0.41 |
| 4 | 5 | −1.46 | −1.15 | 1.92 | −3.84 | 0.64 | −2.98 to 0.05 |
| 5 | 5 | −0.09 | −0.2 | 1.59 | −1.63 | 2.51 | −1.05 to −0.10 |
| 6 | 5 | −1.01 | −1.15 | 1.21 | −2.38 | 0.66 | −1.85 to −0.32 |
| 7 | 5 | −1.56 | −0.79 | 1.73 | −4.25 | −0.22 | −2.33 to −0.23 |
| 8 | 5 | −0.71 | −0.73 | 0.58 | −1.4 | −0.01 | −1.14 to −0.29 |
| 9 | 5 | −0.75 | −0.75 | 0.79 | −1.79 | 0.1 | −1.23 to −0.08 |
| 10 | 5 | 0.20 | 0.42 | 1.29 | −1.79 | 1.51 | −0.22 to 1.06 |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


