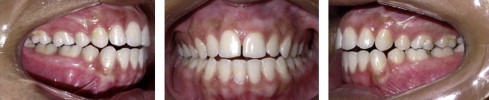
Introduction
In this study, we aimed to evaluate the long-term stability of anterior open-bite treatment with occlusal adjustment and the dentinal sensitivity caused by this procedure in the long term.
Methods
The sample comprised 17 open-bite patients who experienced relapse of the negative vertical overbite after orthodontic treatment and were retreated with occlusal adjustment. The cephalometric changes were evaluated on lateral cephalograms obtained before and after the occlusal adjustment and in the long term (mean, 3.4 years after occlusal adjustment). Dentinal sensitivity was also evaluated before the occlusal adjustment, and 1.35 months, 4.61 months, and 3.4 years later. The cephalometric statuses between the 3 evaluations were compared with analysis of variance (ANOVA) and Tukey tests. The percentages of clinically significant relapse were calculated. To compare dentinal sensitivity at the several stages, nonparametric Friedman and Wilcoxon tests were performed.
Results
Statistically significant relapse of anterior open bite occurred in 33.3% of the patients. Those who had the procedure before 21 years of age were most likely to experience relapse. Dentinal sensitivity remained within the normal range in the long term.
Conclusions
Despite the statistically significant relapse of anterior open bite, clinically significant stability was found in 66.7% of the patients.
Editor’s comment
An open-bite malocclusion in the permanent dentition can be difficult to correct, and patients often have significant relapse after treatment. What do you do when an adult patient returns 4 years later with mild relapse? Do you propose the fixed-appliance approach again, do you schedule a surgical consultation, or do you look for an alternative approach, such as occlusal equilibration? Let’s say you recommend the occlusal adjustment and the patient asks, “What are the chances that this process will be successful and my teeth will still fit together a year from now?” Do you know?
This report presents long-term data from a study that initially included 20 patients who experienced mild relapse 4 years or more after treatment for closure of anterior open bite. The first article reporting data from this study was published online in July 2008 (Janson G, Crepaldi MV, Freitas KMS, Freitas MR, Janson W. Evaluation of anterior open-bite treatment with occlusal adjustment. Am J Orthod Dentofacial Orthop 2008;134:10.e1-9). In that study, all the patients were retreated with occlusal adjustment until a positive overbite was established. At the time, these researchers planned to follow them in the long term to evaluate the success of this approach. Three years later, 17 of the same patients returned for additional posttreatment evaluation. A sample of this size can be considered satisfactory because of the unusual procedure used to correct the open bite.
What did these Brazilian clinicians see when they examined the same patients in the long term? First, they noted “clinically significant” stability in 66.7% of the patients treated with occlusal adjustment, and the dentinal sensitivity remained within the normal range. They found a statistically significant relapse of anterior open bite in the entire sample. Growth seemed to have contributed to a significant amount of the relapse. The primary factor contributing to the relapse was the increase in posterior molar height, consequent to compensatory posterior tooth eruption. It seems to me that these researchers believe that open-bite malocclusions are destined to relapse in many patients. An interesting approach would be to associate the procedures to reduce the clinically significant relapse. For example, nonextraction and extraction orthodontic treatments have 38.1% and 25.8% of clinically significant relapses, respectively. If these relapsed patients can be retreated with occlusal adjustment, and, knowing that this procedure has a clinically significant relapse rate of 33.3%, after the 2 procedures, the amount of clinically significant relapse would be significantly reduced. For now, we can only look forward to additional studies with larger sample sizes.