Introduction
The most frequent adverse effect of canine impaction is resorption of the adjacent incisors. The subjective image quality and the radiographic diagnostic accuracy for detection of simulated canine-induced external root resorption lesions in maxillary lateral incisors were compared among 6 cone-beam computed tomography (CBCT) systems in vitro.
Methods
A child cadaver skull in the early mixed dentition was obtained. This skull had an impacted maxillary left canine and allowed a reliable simulation. Simulated root resorption cavities were created in 8 extracted maxillary left lateral incisors by the sequential use of 0.16-mm diameter round burs in the distopalatal root surface. Cavities of varying depths were drilled in the middle or apical thirds of each tooth root according to 3 setups: slight (0.15, 0.20, and 0.30 mm), moderate (0.60 and 1.00 mm), and severe (1.50, 2.00, and 3.00 mm) resorption. The lateral incisors, including 2 intact teeth, were repositioned individually in the alveolus with approximal contacts to the impacted maxillary left canine. Six sets of radiographic images were obtained with 3D Accuitomo-XYZ Slice View Tomograph (J. Morita, Kyoto, Japan), Scanora 3D CBCT (Soredex, Tuusula, Finland), Galileos 3D Comfort (Sirona Dental Systems, Bensheim, Germany), Picasso Trio (E-WOO Technology, Giheung-gu, Republic of Korea), ProMax 3D (Planmeca OY, Helsinki, Finland), and Kodak 9000 3D (Trophy, Croissy-Beaubourg, France) for each tooth setup. The CBCT images were acquired and subsequently analyzed by 12 observers. Linear models for repeated measures were used to compare the CBCT systems for the image quality and the degree of agreement between the diagnosed severity of root resorption and the true severity.
Results
The differences in the image quality between CBCT systems were statistically significant ( P <0.001). The root resorption scores between CBCT systems showed a significantly higher score for the ProMax when compared with the Galileos and the Kodak. However, the differences in agreement between the diagnosed severity of root resorption and the true severity for all resorption sizes were not significantly different ( P >0.05) among the different CBCT systems.
Conclusions
High image quality is important when detecting root resorption. The CBCT systems used in this study had high accuracy with no significant differences between them in the detection of the severity of root resorption.
Maxillary lateral incisor root resorption is the most common adverse effect associated with an impacted maxillary canine. This process is progressive and irreversible. The degree of resorption depends on the nature and strength of the pressure produced by the impacted canine; it often remains asymptomatic. Resorption defects can be challenging to correctly diagnose and difficult to accurately assess. Root resorption is mostly found close to the maxillary canine or the dental follicle. Root resorption usually starts mildly in a specific area. Yet in time, it can extend in all directions and invade the entire root, making the prognosis of the tooth poor. The exact diagnosis of root resorption entails an essential stage to determine the treatment plan. The selection of an effective therapeutic protocol for orthodontic patients is necessary to ensure correct treatment and better treatment outcomes. Radiographic investigation is an essential part of the early diagnostic process for root resorption because a clinical examination without radiographic information is insufficient for treatment decisions.
In the past, conventional 2-dimensional (2D) radiographic imaging was the first choice and most commonly used clinical method for obtaining a primary diagnostic radiograph for the detection of root resorption in routine patients. Several 2D techniques have been widely used for the differential diagnosis of root resorption. Previous studies have shown that root resorption less than 0.60 mm in diameter and 0.30 mm in depth cannot be detected with 2D radiography. In addition, buccal or lingual resorption is less detectable in 2D radiographs. The use of conventional 2D radiography has been found to be inaccurate for the detection of mild resorption. Furthermore, 2D radiography is also inadequate for representing the resorption lesions and their dimensions, which depend on the severity of the root resorption. A comparative study found that digital radiography is more sensitive in detecting external root resorption than conventional radiography. In contrast, other studies have found that the performance of digital systems is equal to that of conventional systems. Digital subtraction radiography has been shown to be superior to conventional radiography for detection of simulated external root resorption by eliminating anatomic noise.
There is a great need for a more accurate diagnostic method for root resorption. The use of computed tomography (CT) has been suggested in the assessment of root resorption. CT offers 3-dimensional (3D) imaging and increases the detection rate of incisor root resorption caused by impacted canines. However, CT has some limitations in the detection of mild resorptions in the apical third.
Cone-beam CT (CBCT) is a promising alternative because it provides 3D imaging of dental structures with submillimeter resolution images of high diagnostic quality. CBCT also has a short scanning time, reduced radiation exposure, and low cost compared with conventional CT. The diagnostic tasks for which these CBCT systems were mostly used in orthodontics included impacted teeth, temporomandibular joints, root proximity and resorption, tooth movement, cephalometric analysis, cleft lip and palate, planning for miniscrews, and orthodontic treatment planning. CBCT has been found to be useful for diagnosing root resorption caused by ectopically erupting teeth. Recent studies have compared conventional radiography with CBCT for the detection of root resorption. It was shown that the detection of root resorption was higher when using CBCT than with conventional radiography, and it was suggested that CBCT imaging is a reliable tool for the localization and detection of root resorption. Although these systems have rapidly developed while improving their overall image quality, all CBCT systems mainly vary according to their field of volume (FOV) and the detector type, with either image intensifier tube and charge-coupled device or flat-panel detector. It has been reported that detector type influenced image quality such as IIT/CCD has more artifacts and produces more noise compared with flat-panel detector systems. Moreover, FOV was found to be correlated to spatial resolution and contrast. The radiation dose varies substantially between CBCT systems depending on FOV and parameters. The size of voxels plays a role in determining image resolution, quality, and scanning and reconstruction times of CBCT images. Previous studies have only compared the effect of voxel size in 1 or 2 CBCT systems. It was found that the 3 voxel sizes did not affect the diagnostic performance for detection of external root resorption. The best option is to work with dose optimization and full justification to apply a low-dose CBCT technique that offers reasonable to excellent diagnostic accuracy.
The diagnostic ability of different CBCT systems in detecting root resorption caused by an impacted canine has not been sufficiently studied.
The purpose of this in-vitro study was to compare subjective image quality and radiographic diagnostic accuracy for detection of simulated external root resorption lesions caused by an impacted canine with 6 CBCT systems.
Material and methods
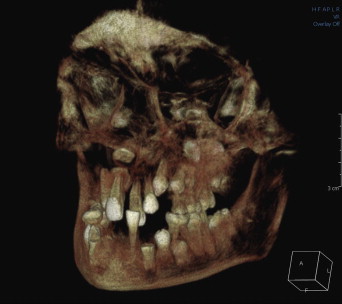
A child cadaver skull in the early mixed dentition phase was used; this skull had an impacted left maxillary canine ( Fig 1 ). CBCT radiographs of the dry skull were taken in specific in-vitro conditions as described by Alqerban et al. Briefly, 8 setups were examined, each with a different maxillary left lateral incisor placed into the extraction site of the maxillary left lateral incisor. Each of the 8 selected lateral incisors was specifically modified to simulate the resorption process according to slight (0.15, 0.20, and 0.30 mm), moderate (0.60 and 1.00 mm), and severe (1.50, 2.00, and 3.00 mm) resorption. In total, 8 cavities ranging in depth from 0.15 to 3.00 mm were created on the distopalatal surface of the root in the middle or apical third. In addition, 2 setups with intact lateral incisors were used (control group). Each tooth was then consecutively repositioned in the alveolus of the pediatric skull.
The samples were scanned according to the protocols recommended by the manufacturers. The CBCT systems were 3D Accuitomo-XYZ Slice View Tomograph (J. Morita, Kyoto, Japan), Scanora 3D CBCT (Soredex, Tuusula, Finland), Galileos 3D Comfort (Sirona Dental Systems, Bensheim, Germany), Picasso Trio (E-WOO Technology, Giheung-gu, Republic of Korea), ProMax 3D (Planmeca OY, Helsinki, Finland), and Kodak 9000 3D (Trophy, Croissy-Beaubourg, France). The machine specifications, scanning protocols, and the FOVs for each CBCT are shown in Table I . After image acquisition, all scans were exported as digital imaging and communications in medicine (DICOM) files and saved to a portable hard disk for later reconstruction. Images were exported and viewed with OnDemand3D software (version 1, CyberMed, Seoul, South Korea) that provided slices in the axial, coronal, and sagittal planes and 3D models. All exposures were made by the same operator (A.A.).
| Accuitomo 3D CBCT | Scanora 3D CBCT | Galileos 3D | Picasso Trio | ProMax 3D | Kodak 9000 3D | |
|---|---|---|---|---|---|---|
| Gray scale (bit) | 8 | 12 | 12 | 12 | 12 | 14 |
| Potential (kV) | 80 | 85 | 85 | 85 | 84 | 85 |
| Current (mA) | 3 | 8–15 | 7 | 5 | 12 | 10 |
| Exposure type | Continuous | Pulsed | Pulsed | Pulsed | Pulsed | Pulsed |
| Scan time (s) | 18 | 2.25–4.5 | 3.4–14 | 15 | 18 | 10 |
| Reconstruction time (min) | 5 | 1–2 | 7 | 4–6 | 3 | 2 |
| Voxel size (mm) | 0.125 | 0.133–0.350 | 0.29 | 0.2 | 0.16 | 0.076–0.2 |
| Field of volume (FOV) (mm) | 30 × 40 | 75 × 100 | 120 × 150 | 70 × 120 | 80 × 80 | 3.7 × 50 |
| Detector type | Image intensifier | Flat panel | Image intensifier | Flat panel | Flat panel | Flat panel |
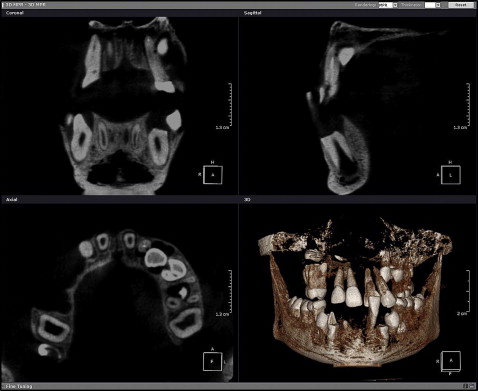
Ten images from 5 CBCT systems (Accuitomo, Scanora, Galileos, Promax, and Kodak) were produced. These were the images of the 8 lateral incisors with simulated resorption cavities and 2 sound lateral incisors (control teeth). However, for the Picasso CBCT system, only 6 teeth were scanned: 4 lateral incisors with resorption cavities (0.15, 0.20, 0.30, and 0.60 mm) and 2 sound lateral incisors. In total, 56 CBCT images were acquired and subsequently analyzed in 2 sessions. The first evaluation session was by 8 postgraduate orthodontic residents, 2 orthodontic instructors, and 2 dental radiologists. All images were viewed by each observer as screen shots. The slice that best showed root resorption in the axial, coronal, and sagittal views was used. The images for all CBCT systems were standardized based on identifying identical anatomic structures at the same location. To standardize viewing conditions, image brightness and contrast were calibrated by a light meter (PeakTech 5025, Dürr Dental, Bietigheim, Germany). The 12 observers were not allowed to adjust the brightness and contrast settings or the reconstruction views, thus ensuring standardized comparisons. All images were viewed on a 20-in flat panel screen (2007 FP 1600 × 1200, Brilliance 200WP, Philips, Brussels, Belgium). The acquired images in the first evaluation session were presented to the observers under the same conditions to prevent differences between observers while scoring the 6 CBCT systems. Observers used the screen shot and standardized contrast to decrease the role of other variables such as computer and viewing software experience and to become more user-friendly and efficient ( Fig 2 ).
The second evaluation session was performed by the 2 dental radiologists, who reviewed the 56 DICOM data sets again 4 weeks after the first session. The radiologists in the second session were allowed to individually reconstruct the images with OnDemand3D and to adjust the brightness and contrast settings with software enhancement tools. They also were able to scroll through the CBCT slices using their own preferences for the optimal display of root resorption in the 3 planes (axial, coronal, and sagittal). This observation design was used to mimic the routine diagnostic approach in which clinicians can adjust image display settings.
All observers were blinded to the type of CBCT machine used and to the purpose of the study. The examiners were trained to use CBCT images for the detection of root resorption, and they assessed the images independently in the same random order. The observers were aware that not all images had root resorption, and they were encouraged to score only resorption in the root of the lateral incisor close to the impacted canine. The observation time was also not limited. The evaluation process of the 2 sessions included a questionnaire on the subjective diagnostic image quality on a 5-point rating scale (very poor, poor, acceptable, good, and excellent). This scale was used to assess the visibility of the following structures: pulp, dentin, and enamel; lamina dura; and overall image noise (brightness, contrast, and intensity). Excellent images were scored as those with clear visibility and distinguishable structures rather than esthetics of the image or the background.
After assessing the image quality, the observers were asked to assess the presence of a resorptive defect in the lateral incisor. The identification of root resorption was done by using a 5-step confidence scale: 1, definitely no resorption; 2, maybe no resorption; 3, unsure; 4, maybe resorption; 5, definitely resorption. If resorption was diagnosed, the examiners were asked to score the degree of resorption according to the criteria of Ericson and Kurol : slight (resorption up to half of the dentin thickness toward the pulp), moderate (resorption of half of the dentin thickness or more, with an unbroken pulp lining), or severe (pulp is exposed because of resorption). The examiners were then asked to classify the location of the diagnosed resorptive defect as apical, midapical (halfway between the apical and middle thirds), or middle third of the root.
Statistical analysis
In the first evaluation session, linear regression models for repeated measurements were used to analyze the relationships between the types of CBCT systems and various indexes of image quality (pulp, enamel, and dentin; lamina dura; overall image noise). Ordinal scores were treated as continuous variables in these analyses. An overall index of image quality was constructed by summing the scores of the 4 indexes. Tukey adjustments for multiple testing were used for pairwise comparisons between CBCT systems in the evaluation of image quality.
The observers’ scores for root resorption were categorized so that scores of definitely resorption or maybe resorption were considered as “yes,” and scores of unsure, maybe no resorption, or definitely no resorption were considered to be “no.” With the actual presence of resorption used as the gold standard, the percentages of correct identification of resorption (sensitivity) and the percentages of correct identification of lack of resorption (specificity) were calculated. Sensitivity and specificity were compared among systems by using the McNemar test. A correction for multiple testing (false discovery rate) was applied on the set of pairwise comparisons between CBCT systems.
The linear regression model was used to compare the 8 setups with resorption for root resorption and to compare all 10 setups for agreement between the diagnosed severity of the resorption and the true severity. The agreement scores were calculated based on Table II . Perfect agreement was given a score of 3, and most severe disagreement was given a score of 0. Moreover, the linear regression model was also used for lesions of 0.6 mm or less to obtain a fair comparison with the Picasso CBCT systems.
| Resorption | Score for severity of diagnosed lateral incisor resorption | |||
|---|---|---|---|---|
| No resorption | Slight resorption | Moderate resorption | Severe resorption | |
| True status | ||||
| None | 3 | 2 | 1 | 0 |
| Slight | 2 | 3 | 2 | 1 |
| Moderate | 1 | 2 | 3 | 2 |
| Severe | 0 | 1 | 2 | 3 |
All analyses were performed with SAS software (version 9.2, SAS System for Windows, SAS Institute, Cary, NC).
Results
The image quality scores of pulp, dentin, and enamel; lamina dura; and overall image noise scored by 12 observers (first evaluation session) of each CBCT system are shown in Figure 3 , A . The results of the second evaluation session of the image quality of dental structures by the 2 radiologists are shown in Figure 3 , B . Figure 4 shows the sum of the image quality scores for each CBCT system. The differences in the image quality scores between CBCT systems were statistically significant ( P <0.001) for all indexes including the sum of all quality scores ( Fig 4 , A ). ProMax images had the best quality, with significantly higher scores than the other systems ( P <0.0001). The Galileos CBCT ranked as the second best system ( P <0.01). Moreover, the differences in scores between the CBCT systems followed a similar pattern in the second evaluation by the 2 radiologists ( Fig 4 , B ).
The radiologists rated image quality of the different CBCT systems higher than did the orthodontic observers ( Table III ). The second evaluation session of the radiologists was better than the first evaluation session, thus indicating that freely using the software improved their ratings of the image quality ( Table III , Fig 5 ).
| First evaluation | Second evaluation | ||||
|---|---|---|---|---|---|
| Scale | Orthodontic residents (n = 8) | Orthodontic instructors (n = 2) | Radiologists (n = 2) | Radiologists (n = 2) | |
| Pulp | Very poor | 13.17 | 3.57 | 0.89 | 0.00 |
| Poor | 33.48 | 29.46 | 17.86 | 7.14 | |
| Acceptable | 37.50 | 40.18 | 47.32 | 34.82 | |
| Good | 14.29 | 25.89 | 27.68 | 44.64 | |
| Excellent | 1.56 | 0.89 | 6.25 | 13.39 | |
| Enamel and dentin | Very poor | 18.75 | 15.18 | 10.71 | 4.46 |
| Poor | 34.15 | 33.93 | 29.46 | 10.71 | |
| Acceptable | 28.35 | 30.36 | 33.04 | 40.18 | |
| Good | 16.74 | 18.75 | 17.86 | 33.04 | |
| Excellent | 2.01 | 1.79 | 8.93 | 11.61 | |
| Lamina dura | Very poor | 12.50 | 12.50 | 0.89 | 0.89 |
| Poor | 38.17 | 37.50 | 34.82 | 16.07 | |
| Acceptable | 36.16 | 22.32 | 31.25 | 32.14 | |
| Good | 11.83 | 25.89 | 27.68 | 36.61 | |
| Excellent | 1.34 | 1.79 | 5.36 | 14.29 | |
| Overall structure identification on the image quality | Very poor | 12.28 | 8.93 | 8.04 | 2.68 |
| Poor | 38.62 | 37.50 | 38.39 | 15.18 | |
| Acceptable | 37.95 | 26.79 | 32.14 | 29.46 | |
| Good | 10.94 | 25.89 | 14.29 | 44.64 | |
| Excellent | 0.22 | 0.89 | 7.14 | 8.04 | |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


