Introduction
Our aim in this study was to compare intermolar widths after alignment of crowded mandibular dental arches in nonextraction adolescent patients between conventional and self-ligating brackets.
Methods
Fifty patients were included in this randomized controlled trial according to the following inclusion criteria: nonextraction treatment in both arches, eruption of all mandibular teeth, no spaces in the mandibular arch, mandibular irregularity index from canine to canine greater than 2 mm, and no therapeutic intervention planned involving intermaxillary or other intraoral or extraoral appliances including elastics before the end of the observation period. The patients were randomized into 2 groups: the first received a conventional appliance, and the other a passive self-ligating appliance, both with a 0.022-in slot. The amount of crowding of the mandibular dentition at baseline was assessed by using the irregularity index. Intermolar width was investigated with statistical methods of linear regression analysis. On an exploratory basis, the effect of appliance type on intercanine width was also assessed. Additionally, the effects of appliance type on time to alignment and crowding on time to alignment were assessed by using the Cox proportional hazards model.
Results
No evidence of difference in intermolar width was found between the 2 bracket systems (β = 0.30; 95% CI, −0.3 to 0.9; P = 0.30). No evidence of difference in intercanine width was observed between the 2 bracket systems (β = 0.33; 95% CI, −0.8 to 0.1; P = 0.15). The time to reach alignment did not differ between appliance systems (hazard ratio, 0.68; 95% CI, 0.4 to 1.2; P = 0.21), whereas the amount of crowding was a significant predictor of the required time to reach alignment (hazard ratio, 0.88; 95% CI, 0.8 to 0.9; P = 0.02).
Conclusions
The use of conventional or self-ligating brackets does not seem to be an important predictor of mandibular intermolar width in nonextractions patients when the same wire sequence is used.
The last decade has witnessed the reemergence of self-ligating appliances with almost every major orthodontic company including in their product line a self-ligating appliance. Passive and active self-ligating appliances with a variety of ligating mechanisms were introduced with their main goals to enable easy clinical handling and allow for efficient sliding mechanics.
It has been proposed that some self-ligating appliances might induce wider intermolar widths. The available evidence on the efficiency of self-ligating brackets derives from a limited number of prospective and randomized clinical trials; some have indicated differences in final molar widths, and some have shown no differences between self-ligating and conventional appliances. However, wire sequences differed between treatment groups, and extraction patients were also included. A recent systematic review, which among other parameters assessed the effect of bracket type on intermolar width by pooling data from previous studies, found no differences between conventional and self-ligating brackets. Because of the limited numbers of studies and because these studies used different protocols with variable quality of the applied methodology, a randomized controlled trial (RCT) was undertaken to further clarify the effect of the type of appliance on intermolar width.
The main purpose of this study was to comparatively evaluate the effect on intermolar width of conventional and self-ligating brackets at the final alignment stages. On an exploratory basis, we intended to assess the effects of type of appliance on intercanine width and days to alignment, and the amount of crowding on time to alignment.
Material and methods
Fifty patients were included in this single-center, 2 parallel-arm (1:1 ratio) RCT. They were selected based on the following inclusion criteria: nonextraction treatment on both arches, eruption of all mandibular teeth, no spaces in the mandibular arch, mandibular irregularity index greater than 2 mm (canine to canine), and no therapeutic intervention planned involving intermaxillary or other intraoral or extraoral appliances including elastics, maxillary expansion appliances, or headgears before the end of the observation period. The amount of crowding of the mandibular anterior dentition was assessed with the irregularity index as described by Little. Measurements were made twice, and the average was taken, on the initial casts by the first author with digital calipers (Digimatic NTD12-6 in C, Mitutoyo, Tokyo, Japan).
The conventional bracket group was bonded with the Roth prescription microarch bracket (GAC, Central Islip, NY), and the self-ligating group received the DamonMX (Ormco, Glendora, Calif), both with a 0.022-in slot size. The trial took place at the private orthodontic office of the first author (N.P.) from June 2009 to October 2010, and all treatments including bracket bonding and archwire placement were performed by him.
The archwire sequence was the same for both treatment groups, as follows: 0.014-in Damon arch form copper-nickel-titanium (35°C, Ormco), followed by a 0.014 × 0.025-in Damon arch form copper-nickel-titanium (35°C, Ormco), and finally a 0.016 × 0.025-in stainless steel. The patients were followed closely on a monthly basis. All maxillary arches were treated with either conventional or Damon appliances in accordance with the mandibular appliance and similar mechanotherapy, starting with 0.014-in copper-nickel-titanium and followed by 0.016 × 0.025-in copper-nickel-titanium, 0.019 × 0.025 beta-titanium alloy, and 0.019 × 0.25-in stainless steel.
The main outcome was intermolar width at the time of the passive placement of the 0.016 × 0.025-in stainless steel wire on the mandibular arch. Alignment was carefully inspected visually; when the 0.016 × 0.025-in wire could be seated passively in the bracket slots, then it was decided that the time for outcome assessment or end of observation had been reached. For the self-ligating bracket, unimpeded closing of the bracket doors and, for the conventional bracket, complete seating at the base of the slot were used as guidelines for placement of the 0.016 × 0.025-in wire. Secondary outcomes included intercanine width and days to reach the time to place the final 0.016 × 0.025-in stainless steel wire. Measurements were made on the mandibular models taken when it was decided that the 0.016 × 0.025-in wire could be placed passively.
The date that each patient was bonded (T1) and the date that alignment was judged to be complete (T2) were entered in a spreadsheet. At that time, mandibular impressions were taken, plaster models were prepared, and the brackets from second premolar to second premolar were scraped off with a curving knife by the laboratory technician to facilitate blind measurements. Each model had an identification number so that the measurements could be correctly entered into the spreadsheet. Intermolar (buccal groove to buccal groove) and intercanine (tip to tip) widths were measured on the dental casts with the digital calipers at T1 and T2. The time to alignment (T2 minus T1) for each patient was calculated in days.
Based on previous research, it was assumed that an intermolar width difference of 2 mm (SD, 2 mm) between the bracket groups would be an important clinical finding. Based on this assumption, the required sample size was 22 participants per group (α = 0.05; power = 90%), and it was decided to round up to 25 subjects per group to make provisions for any losses. Sample size calculations were carried out by using statistical software (version 11, Stata Corp, College Station, Tex) and by implementing the sampsi command.
Fifty patients were randomized to either a conventional or a self-ligating appliance. The statistical software package was used by the first author, and the user-written ralloc command was implemented to generate the random allocation sequence. Randomization was accomplished by generating random permuted blocks of variable size (2 and 4), which assured equal patient distribution between the 2 trial arms. Sequentially numbered, opaque, sealed envelopes were prepared before the trial containing the treatment allocation cards. After patient selection and recording of baseline information, the secretary in the practice was responsible for opening the next envelope in sequence and allocating treatment.
Blinding of either the patient or the orthodontist during delivery of the interventions and assessment of whether the 0.016 × 0.025-in wire could be placed was not possible, but measurements on the models were performed blindly as explained earlier.
Statistical analysis
Demographic and clinical characteristics were investigated with conventional descriptive statistics. The effect of the type of appliance on the intermolar width was investigated by using linear regression modeling. For the univariable analysis, the final intermolar width was the dependent variable and the type of appliance the independent variable. For the multivariable model, the final intermolar width was further adjusted for demographics (sex, age), clinical characteristics (pretreatment crowding from molar to molar, pretreatment crowding from canine to canine, pretreatment molar width, pretreatment intercanine width, and Angle classification), and days to reach the point of passive placement of the 0.016 × 0.025-in stainless steel wire. Residuals analysis was conducted to confirm no violation of the linear regression assumptions.
A similar univariable and multivariable model was used to assess the effect of the demographic and clinical variables on the final intercanine width. The Cox proportional hazard model was used to evaluate the effect of appliance type on the time to reach passive placement of the 0.016 × 0.025-in wire. Hazard ratios (HR) and associated CI values and the Kaplan-Meier survival plot, including numbers at risk at various time points, were calculated. The proportional hazard assumption was not violated, as the Nelson-Aalen plot indicated. A 2-tailed P value of 0.05 was considered statistically significant with a 95% CI for all tests.
On 20 models (20% of the total), the intercanine and intermolar widths were remeasured at 2 times at least a month apart, and the intracluster correlation coefficient was calculated to evaluate the reliability of the measuring method. All analyses were performed by using the Stata software.
Results
Figure 1 is the CONSORT flowchart showing that all patients received the intended treatment with no losses to follow-up.
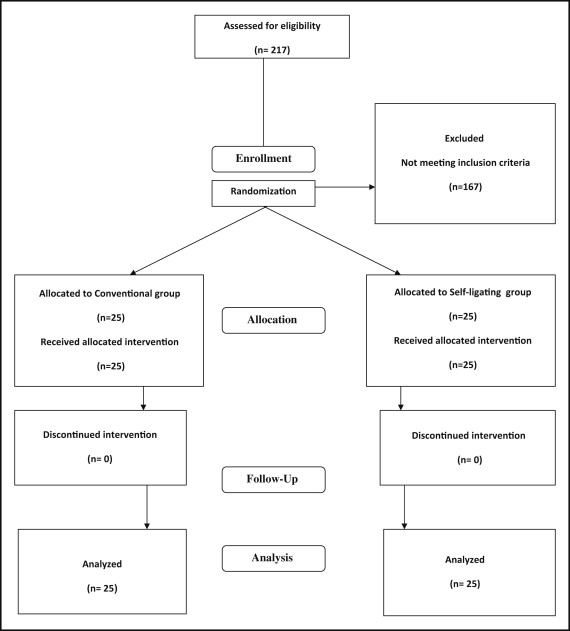
Table I gives the distributions of the demographic and clinical characteristics of the subjects including age, sex, irregularity index, mandibular arch dimensions, and Angle classification. It shows no discrimination with respect to these factors between the 2 groups, thus validating the random assignment of appliances to each group.
| Total (n = 50) | Conventional (n = 25) | Self-ligating (n = 25) | ||||
|---|---|---|---|---|---|---|
| Mean or % | SD | Mean or % | SD | Mean or % | SD | |
| Demographic characteristics | ||||||
| Age (y) | 13.3 | 1.6 | 13.4 | 1.6 | 13.2 | 1.6 |
| Sex | ||||||
| Female | 66.0 | 64.0 | 68.0 | |||
| Male | 34.0 | 36.0 | 32.0 | |||
| Clinical characteristics | ||||||
| Crowding (irregularity index, mm) | ||||||
| Canine to canine | 4.2 | 1.8 | 4.0 | 1.6 | 4.5 | 2.0 |
| First molar to first molar | 10.8 | 3.2 | 10.8 | 2.7 | 10.8 | 3.7 |
| Mandibular arch dimensions (mm) | ||||||
| Intercanine width | 25.3 | 1.8 | 25.0 | 2.0 | 25.6 | 1.4 |
| Intermolar width | 44.6 | 2.2 | 44.7 | 1.9 | 44.5 | 2.4 |
| Angle Class | ||||||
| I | 34.0 | 32.0 | 36.0 | |||
| II | 66.0 | 68.0 | 64.0 | |||
Table II displays the mean intercanine and intermolar widths at T1 and T2, and their mean differences.
| T1 3-3 | T2 3-3 | T2-T1 3-3 | T1 6-6 | T2 6-6 | T2-T1 6-6 | |
|---|---|---|---|---|---|---|
| Mean (SD) | Mean (SD) | Mean (SD) | Mean (SD) | Mean (SD) | Mean (SD) | |
| Appliance | ||||||
| Conventional | 25.0 (2.0) | 27.1 (1.4) | 2.1 (1.2) | 44.7 (1.9) | 46.2 (1.9) | 1.5 (0.9) |
| Self-ligating | 25.6 (1.4) | 27.0 (1.4) | 1.40 (0.8) | 44.5 (2.4) | 46.4 (2.4) | 1.9 (1.3) |
The reliability of the measurement method was high, with an intracluster correlation coefficient value of 0.99.
Table III shows the results of the univariable and multivarible linear regression model derived coefficients (β) and the 95% CI values, indicating the effect on the final intermolar and intercanine widths of type of appliance, adjusted for demographic and clinical characteristics, and days required to reach the point of passive placement of the 0.016 × 0.025-in stainless steel wire. The unadjusted analysis results show that the average increase of intermolar width was 0.17 mm with a range of −1.1 to +1.4 mm for the self-ligating group compared with the conventional group, a nonsignificant finding ( P = 0.79). The adjusted analysis showed a slightly larger increase (β = 0.30; 95% CI, −0.3 to 0.9; P = 0.30) that was also more precise, as expected and as indicated by the narrow width of the CI. The adjusted estimates indicate that the mean difference in intermolar width between the 2 appliances was 0.30 mm after adjusting for the aforementioned variables. The 95% CI indicates that the difference in intermolar width between the 2 bracket systems ranged from −0.3 to +0.9 mm, and it was not a significant finding since it included the value of 0. The only significant predictor of final molar width was pretreatment molar width ( P <0.001), whereas sex (β = 0.65; 95% CI, 0 to 1.3; P = 0.05) and molar-to-molar irregularity (β = 0.1; 95% CI, 0 to 0.2; P = 0.08) were only weak predictors. For intercanine width, the unadjusted estimates were β = 0.0; 95% CI, −0.8 to 0.8; and P = 0.99, and the adjusted estimates were β = 0.33; 95% CI, −0.8 to 0.1; and P = 0.15. The only significant predictor of final intercanine width was pretreatment intercanine width (β = 0.53; 95% CI, 0.6 to 0.7; P <0.001).



