4 Clinical Case Presentations Based on Different Loading Protocols
Posterior Multi-Tooth Gaps and Free-End Situations in the Maxilla or Mandible
4.1 Replacement of Multiple Teeth in a Partially Dentate Posterior Mandible with a Fixed Dental Prosthesis Using an Early Loading Protocol
Y. Nakajima
A 55-year-old female patient was referred for consultation and treatment. Her chief complaint was pain associated with the mandibular right second premolar (tooth 45). The patient denied systemic or oral diseases capable of compromising dental care. She had a history of adult periodontitis, for which she continued to be treated. Her response to therapy and motivation towards dental health were considered excellent.
Intraoral examination revealed a cantilever fixed dental prosthesis in the mandibular right quadrant, with retainers on teeth 45 and 47, and pontics at sites 44 and 46. The retainer on tooth 45 was loose, and the tooth was carious. Radiographic evaluation confirmed the extent of the caries and the maintenance of bone around tooth 45 and in the pontic region 46 (Fig 1).
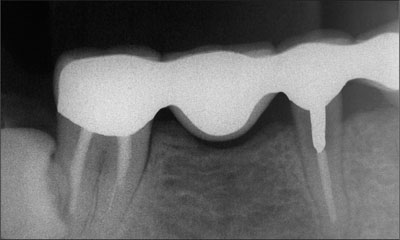
Fig 1 Pretreatment radiograph, illustrating the degree of carious destruction involvment on tooth 45 and the bone height around tooth 45 and under the pontic at site 46.
Removal of the fixed dental prosthesis revealed the extent of the destruction of tooth 45, which was considered to be non-restorable (Fig 2).
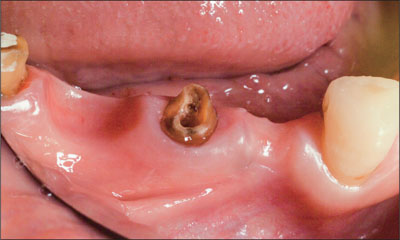
Fig 2 Pretreatment lateral view subsequent to the removal of the existing fixed dental prosthesis.
The patient was given several treatment options. These included:
-
Option 1: Bone augmentation at site 44, to be followed by implant placement in sites 44, 45, and 46. This would allow for single-tooth implant-supported crowns in sites 44, 45, and 46, and a metal-ceramic crown on tooth 47.
-
Option 2: Bone augmentation at site 44, to be followed by implant placement in sites 44 and 46. This would facilitate restoration with an implant-supported fixed dental prosthesis (44-46), and a metal ceramic crown on tooth 47.
-
Option 3: Placement of dental implants in sites 45 and 46. This would allow for the fabrication of a fixed dental prosthesis (44-46) with a cantilevered unit (44). A metal-ceramic crown would be provided on tooth 47.
-
Option 4: The fabrication of a conventional removable partial denture.
The patient chose not to augment site 44, and she preferred a fixed restoration. After considering all the treatment options, the patient elected and consented to pursue treatment option 3 (two implants and a cantilevered fixed dental prosthesis). Immediate (type 1) implant placement in site 45 was to be undertaken, should hard and soft tissue volume be considered adequate after the extraction of the tooth.
Tooth 45 was extracted with periotomes and elevators without incident. Trauma to surrounding soft tissues and bone was minimized and the site was considered appropriate for the immediate placement of a dental implant. A full thickness mucoperiosteal flap was elevated, and two Straumann Standard Plus implants were positioned in sites 45 (endosteal diameter, 4.1 mm; length, 10 mm; Regular Neck prosthetic platform, 4.8 mm) and 46 (endosteal diameter, 4.8 mm; length, 10 mm; Wide Neck prosthetic platform, 6.5 mm) according to a restoration-driven protocol, using appropriate templates. Both implants were considered stable, and the dimension of the horizontal defect surrounding the implant in site 45 was less than 1 mm (Fig 3).
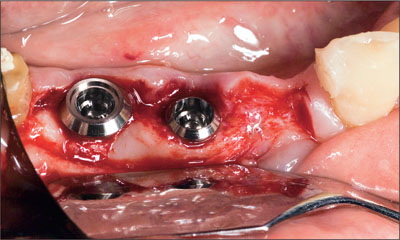
Fig 3 After implant placement. Note the restorative margins at the height of the buccal bone crests and the limited horizontal defect.
Healing caps were then positioned to ensure transmucosal healing, and the wound was sutured closed (Fig 4).
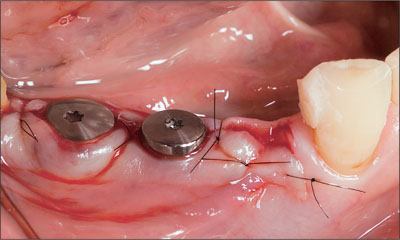
Fig 4 The implants with the healing caps and wound closure.
After 6 weeks of healing, the patient was evaluated and the soft tissue response was considered excellent (Fig 5).
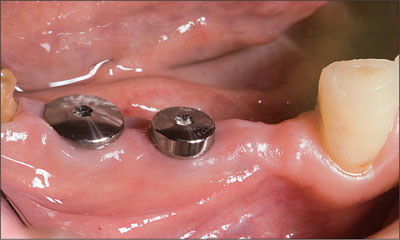
Fig 5 The healing caps and soft tissue healing 6 weeks after implant placement.
The healing caps were removed, and the sulcus depth on both implants was considered to be less than 3 mm in all areas. Impression caps were positioned to allow for the registration of the implant shoulders, and appropriate positioning cylinders were then placed without incident. A polyvinyl siloxane impression was made to facilitate the indirect fabrication of the provisional restoration. The screw-retained provisional restoration was fabricated in acrylic resin incorporating titanium provisional cylinders for bridges, and it was delivered 8 weeks after implant placement without incident (Fig 6). The cantilevered unit was kept out of occlusion in centric relation and all excursions. Transient blanching (less than 10 minutes) was observed in the region of the ovate pontic.
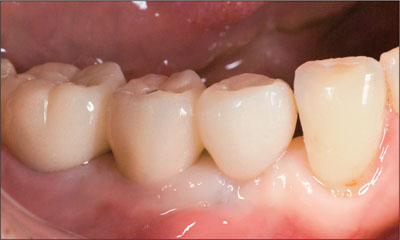
Fig 6 The screw-retained provisional fixed dental prosthesis.
The soft tissues adjacent to the provisional restoration were allowed to mature for an additional 6 weeks (Fig 7). The health of all tissues was confirmed subsequent to removal of the provisional restoration (Fig 8).
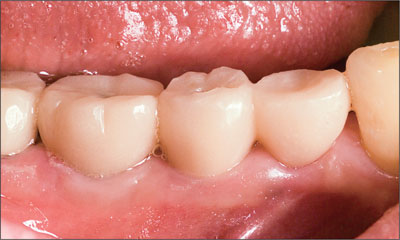
Fig 7 The screw-retained provisional fixed dental prosthesis 6 weeks after placement.
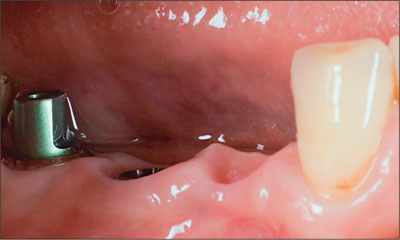
Fig 8 Soft-tissue condition after 6 weeks of provisional restoration.
A customized impression cap, duplicating the emergence of the restoration at site 45, and the ovate site 44, was then fabricated (Fig 9) and positioned (Fig 10). A final impression was then taken in polyvinyl siloxane and a cast poured.
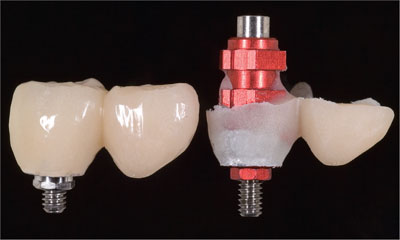
Fig 9 The customized screw-retained synOcta impression cap and duplicated ovate pontic.
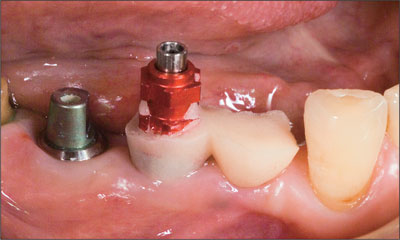
Fig 10 The customized impression cap in position.
A high-strength, biocompatible cementable zirconium oxide framework (Zeno-Tec) was fabricated on the customized master cast, utilizing 2-piece cementable synOcta abutments (Fig 11). Attention to tooth position, room for veneering ceramic, and connector dimension was required to provide adequate resistance to fracture, particularly in the cantilever region. Feldspathic ceramic was then applied to the framework (Fig 12). The emergence profile of the restoration was carefully controlled to prevent inappropriate contouring and to improve the esthetic outcome (Fig 13).
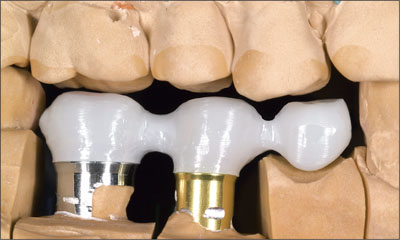
Fig 11 High-strength biocompatible zirconium oxide framework, illustrating adequate room for feldspathic ceramic and connector dimensions.
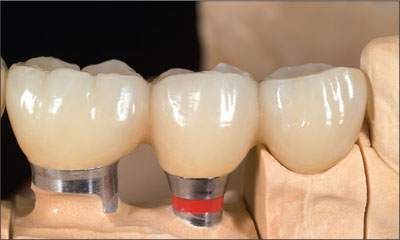
Fig 12 The final fixed dental prosthesis on the master cast.
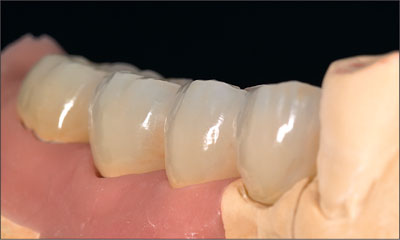
Fig 13 Buccal view of the final fixed dental prosthesis, illustrating an appropriate emergence profile.
At delivery, the occlusal, esthetic, and hygienic results were confirmed and modified as required (Fig 14). The cementable synOcta abutments were torqued to 35 Ncm without incident and the final prosthesis permanently luted using glass- ionomer cement (Fig 15). The patient was placed on a 3-month recall schedule and was completely satisfied with the outcome.
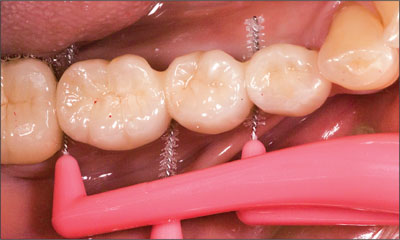
Fig 14 The try-in and confirmation of hygiene capacity.
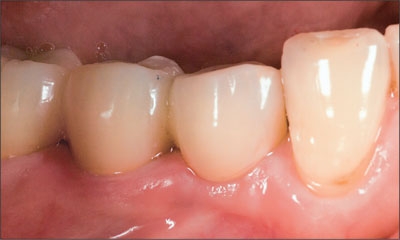
Fig 15 The fixed dental prosthesis immediately subsequent to cementation.
At the 18-month recall visit, oral hygiene maintenance was considered excellent and the fixed dental prosthesis was free of complications (Fig 16).
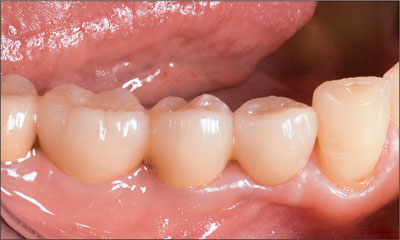
Fig 16 The fixed dental prosthesis at the 18-month follow-up appointment.
The periapical radiograph 18 months after implant restoration confirmed excellent bone maintenance (Fig 17).
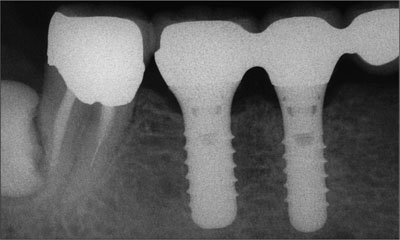
Fig 17 Periapical radiograph 18 months after placement of the prosthesis. Bone levels adjacent to the implants and in the ovate pontic region appear excellent.
Acknowledgments
Laboratory Procedures
Isamu Saitou – CDT, IS Dental, Tokyo, Japan.
Oral Hygienist
Yuki Seki – DH, Nakajima Dental Clinic.
4.2 Replacement of Multiple Teeth in a Partially Dentate Posterior Mandible with a Fixed Dental Prosthesis Using an Early Loading Protocol
W. C. Martin, J. Ruskin
In 2002, a 27-year-old female patient was referred to our clinic for the treatment of her failing dentition. The patient’s medical history revealed no significant findings that would preclude routine dental procedures. She reported no drug allergies and was currently taking no medications. Her dental history was restricted to operative dentistry that addressed several areas of recurrent decay. The patient was on a periodontal recall and home care program that continually fell short of maintaining a healthy dentition. The patient’s chief complaint was: “My teeth often break, and they are sensitive when I eat and drink.”
An intraoral examination revealed several areas of recurrent decay around restorations that were placed within a 3-year period. The majority of the teeth in quadrants 1 to 3 were restorable without the need for endodontic or periodontal intervention. Teeth 33-36 exhibited gross recurrent decay with severe gingival inflammation (Fig 1). Tooth 36 had circumferential decay extending from the distolingual surface to the distofacial, with occlusal involvement. In addition, the decay extended approximately 3 mm subgingivally Tooth 35 exhibited facial and subgingival recurrent decay with occlusal caries. Tooth 34 exhibited facial re-current decay extending 2 mm subgingivally with occlusal caries. Tooth 33 exhibited facial recurrent decay extending 1 mm subgingivally.
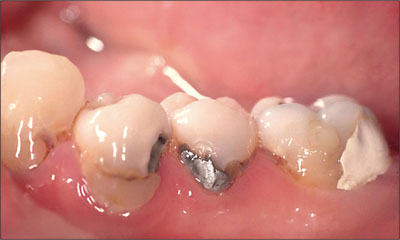
Fig 1 Lateral view of teeth 33-36.
The radiographic analysis of teeth 34-36 confirmed the findings of recurrent decay (Fig 2). There were no radiographic signs of bone loss or of the widening of the periodontal ligament space. The pulp chambers and canals were visible and there were no signs of periapical radiolucencies. The teeth tested vital to an electric pulp test.
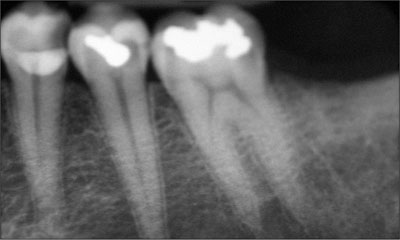
Fig 2 Periapical radiograph of teeth 34-36.
Several treatment plans were considered and discussed in detail with the patient. A conventional approach was offered that addressed the patient’s needs through caries control, periodontal therapy, endodontic therapy, crown lengthening, and restorative procedures, including dowel and core foundations restored with full coverage restorations. This approach, in addition to being costly, was met with concerns by the patient based upon her restorative history. A second treatment option was given to extract teeth 34-36, maintain the osseous structure, and place two dental implants in sites 34 and 36 and restore them with a three-unit fixed dental prosthesis. While this may be viewed as an aggressive approach, the treatment was believed to have the best long-term prognosis, given the patient’s dental history. When the cost was reviewed, the second option was also more feasible for the patient. Other conservative treatment options were also discussed and subsequently declined by the patient.
In the laboratory, the existing teeth were utilized to plan for implant positioning. A surgical template was fabricated to assist the surgeon in placing two immediate implants in sites 34 and 36 in an ideal restorative position, utilizing the available bone upon the extraction of the teeth (Higginbottom and coworkers, 1996).
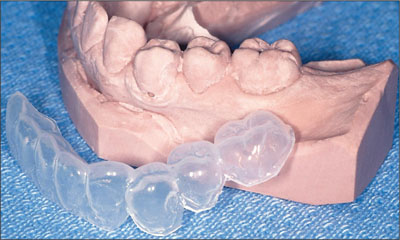
Fig 3a A vacuform template (6 mm) of the existing teeth was fabricated.
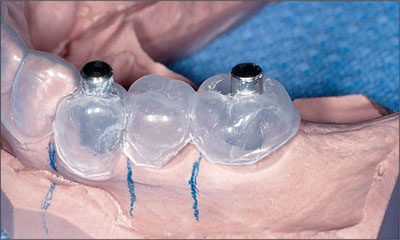
Fig 3b The cast was adjusted to remove the teeth, and guide pins (3.5 mm) were placed in ideal restorative positions based upon the planned restoration and existing ridge shape.
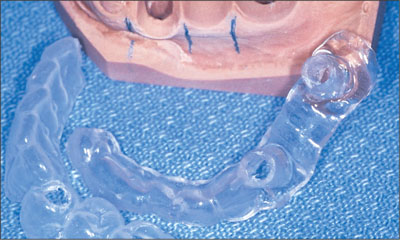
Fig 3c A vacuform template (2 mm) was fabricated over the pins to create a surgical template to assist the surgeon with the placement of the dental implants.
At the surgical visit, teeth 34-36 were extracted, utilizing periotomes and forceps in an attempt to preserve osseous structure. Upon the removal of the teeth, the sockets were debrided with a curette and irrigated with NaCl solution. The proposed implant sites were examined to confirm that the cortical plates were intact. A surgical template was utilized to place implants in sites 34-36. Because the implants were to be positioned immediately, tapered effect implants (Straumann AG) were selected to maximize primary stability (Fig 4). Two healing caps were placed and a postoperative radiograph was taken (Figs 5-6). Postoperative instructions were given to the patient, and a one-week follow-up appointment was scheduled.
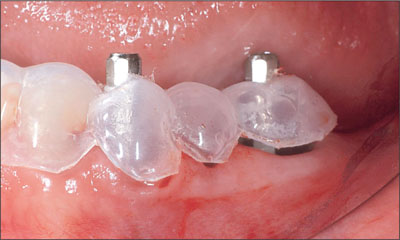
Fig 4 The surgical template in place, confirming the final position of the dental implants prior to the removal of the implant mount.
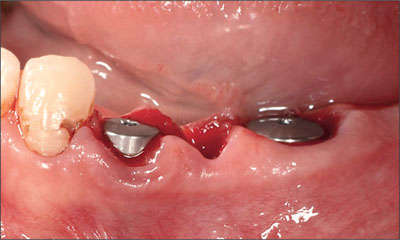
Fig 5 The dental implants with the healing caps in place.
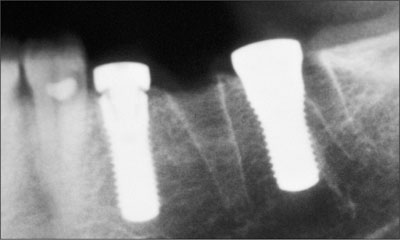
Fig 6 The postoperative periapical radiograph. Site 34: 4.1 x 12 mm RN, site 36: 4.8 x 12 mm WN.
At the one-week follow-up visit, the healing cap on the implant in site 34 was loose and was subsequently tightened with the SCS screwdriver. Six weeks after the placement of the dental implants, the patient returned for the final impression. A periapical radiograph was taken to view the extent of the socket healing (Fig 7). Prior to the final impression, a shade selection was made and photographed for laboratory communication. The healing caps were removed and impression caps and synOcta positioning cylinders were placed (Figs 8-9). A polyvinyl siloxane impression was made in addition to a jaw relation record. In clinical situations where implants are not bound by natural tooth stops distal to the most posterior implant, a second impression cap is captured within the jaw relation record to function as a third reference point for cast articulation (Fig 10). The healing caps were placed and the patient was scheduled for a delivery appointment.
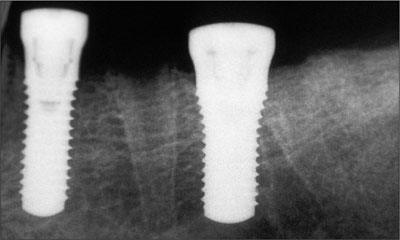
Fig 7 Periapical radiograph 6 weeks after implant placement.
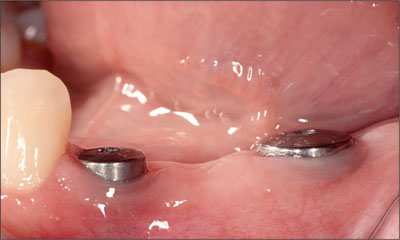
Fig 8 The lateral view of the implants 6 weeks after placement.
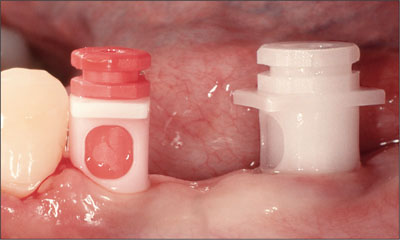
Fig 9 Lateral view of the impression caps and synOcta positioning cylinders in place.
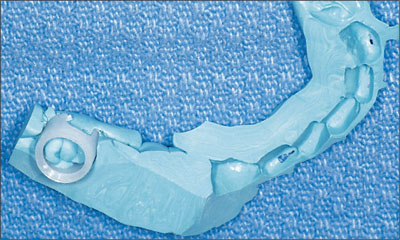
Fig 10 Jaw relation record with the impression cap in place.
In the laboratory, synOcta analogs were carefully snapped into the impression caps. A soft-tissue analog material was positioned around their collars and allowed to set (Fig 11). Excess tissue analog material was removed prior to pouring the impression in a low-expansion die stone. The master casts were articulated and definitive synOcta abutments were selected. The implants were placed in a parallel position that allowed cementable synOcta abutments to be utilized (Fig 12). The abutments were prepared with a twelve-fluted carbide bur to allow for a common path of insertion and adequate reduction for a metal-ceramic fixed dental prosthesis. A full-contour wax-up was created (Fig 13). The wax-up was cut back to allow for a uniform ceramic thickness (Fig 14). The wax pattern was sprued, invested, and cast in a high-noble ceramic alloy (Fig 15). Ceramic material was applied, and the prosthesis was completed (Figs 16-17).
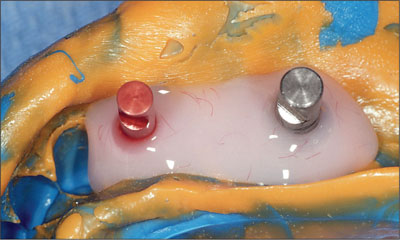
Fig 11 Intaglio surface of the final impression with synOcta analogs.
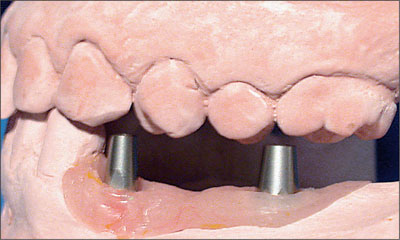
Fig 12 Lateral view of the cementable synOcta abutments in place prior to reduction.
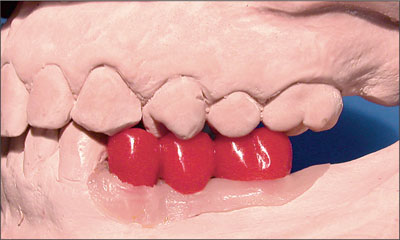
Fig 13 Lateral view of the full-contour wax-up.
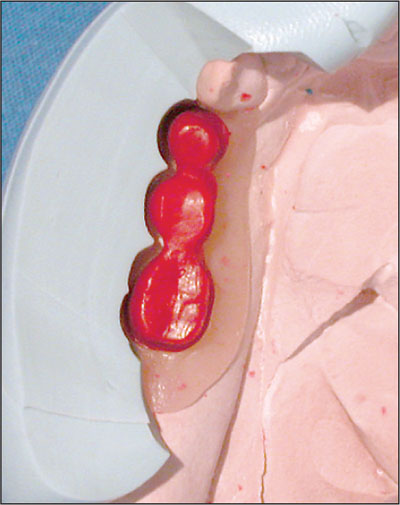
Fig 14 Occlusal view of the cutback with a putty matrix of the full-contour wax-up.
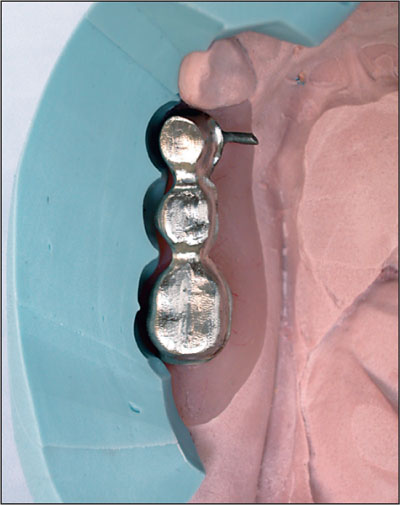
Fig 15 Occlusal view of the framework on the master cast with the matrix in place.
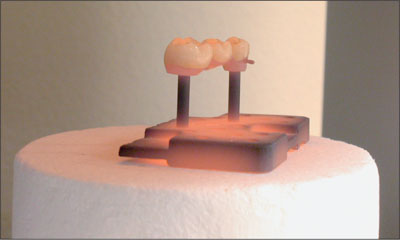
Fig 16 Ceramic firing.
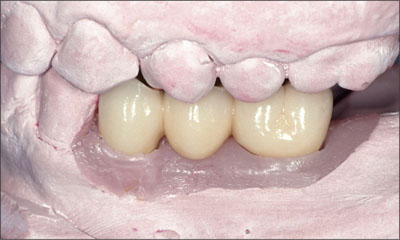
Fig 17 Fixed dental prosthesis on the master cast.
Prior to returning the implant-supported fixed dental prosthesis, an abutment positioning or transfer index was fabricated to allow for the accurate placement of the synOcta abutments into the dental implants. In general, when multiple abutments that support a fixed dental prosthesis are prepared, their accurate placement into the implants may be difficult due to the multiple orientations that could occur. The fabrication of an acrylic resin transfer index that captures their orientation on the master cast allows for an accurate placement of the abutments into the oral cavity (Figs 18-19).
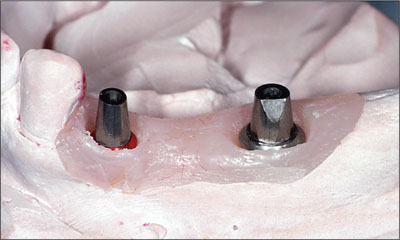
Fig 18 Prepared synOcta abutments on the master cast.
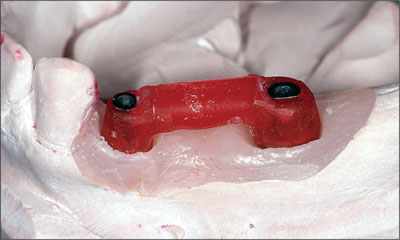
Fig 19 Acrylic resin index fabricated over the definitive synOcta abutments.
At the delivery appointment, the healing caps were removed and the implants cleansed with the air/water syringe. The transfer index (with the synOcta abutments in place) was placed into the implants (Fig 20). The abutments were hand-tightened and the fixed dental prosthesis was placed onto the implants. The fixed dental prosthesis was examined for accurate shade, passivity, and interproximal and occlusal contacts. Once the color and fit were confirmed, the synOcta abutments were tightened to 35 Ncm and sealed with cotton and cavit (Fig 21).
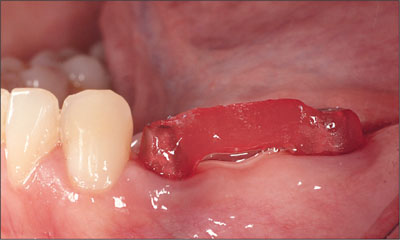
Fig 20 The transfer index placed on the dental implants.
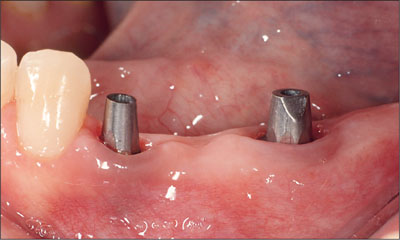
Fig 21 The definitive synOcta abutments prior to sealing with cotton and cavit.
A definitive resin-modified cement was utilized to seat the restoration. Occlusion was refined and polished with diamond-impregnated burs (Figs 22-23). A periapical radiograph was taken, and the patient was scheduled for a follow-up appointment (Fig 24).
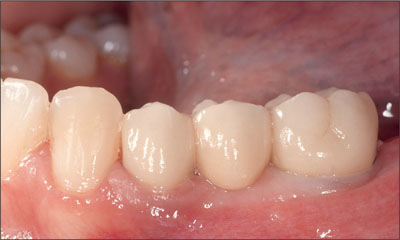
Fig 22 Lateral view of the fixed dental prosthesis.
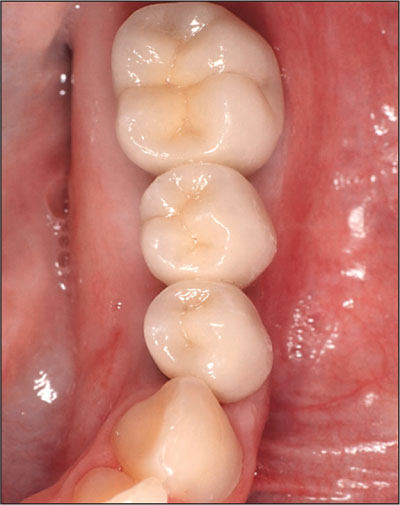
Fig 23 Occlusal view of the fixed dental prosthesis.
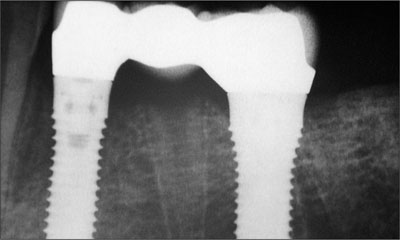
Fig 24 Periapical radiograph of the fixed dental prosthesis at the time of delivery.
The patient was placed on a strict recall program and therapy was continued for other areas of concern. Follow-up pictures and radiographs were taken at four years (Figs 25-26).
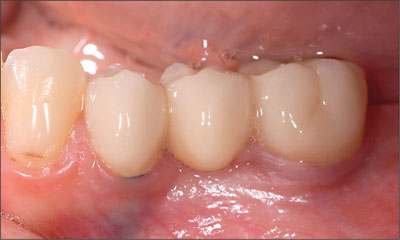
Fig 25 Lateral view of the fixed dental prosthesis at 4 years after implant placement.
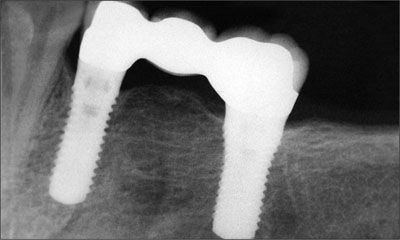
Fig 26 A periapical radiograph of the fixed dental prosthesis at four years.
Acknowledgments
Laboratory Procedures
Todd A. Fridrich – Definitive Dental Arts, Coralville, Iowa, USA.
4.3 Replacement of Multiple Teeth in a Partially Dentate Posterior Maxilla and Mandible with Fixed Dental Prostheses Using a Conventional Loading Protocol
G.O. Gallucci
In the summer of 2002, a 42-year-old female patient was referred to the University of Geneva for the replacement of posterior maxillary and mandibular missing or non-restorable teeth. The patient’s medical history revealed no significant findings, and she was in good general health. Her dental history included recurrent decay that led to the loss of several posterior teeth. The patient showed no history of periodontal disease.
At the extraoral examination, the patient presented normal physiognomy with normal facial and lip support and homogenous distribution of the facial thirds. At full smiling, the patient displayed an average lip line, and a tooth gap was slightly visible in the left maxilla. Small diastemas were present between the anterior maxillary teeth (Fig 1).
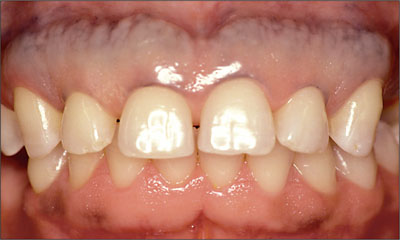
Fig 1 Frontal view in occlusion. The vertical dimension is consistently maintained by the remaining posterior and anterior teeth.
The patient’s chief complaint was “discomfort when chewing and speaking,” which called for the replacement of the posterior missing teeth. The patient had no esthetic concerns regarding her current dental status. The patient ruled out a removable solution and requested a fixed restoration.
At the intraoral evaluation, the patient presented with multi-tooth gaps in the posterior maxilla and the right posterior mandible. The missing teeth were recorded as follows: 17, 16, 15, 24, 25, 26, 37, 45, 46, and 47. In the area of tooth 16, a residual root fragment resulting from an incomplete tooth extraction was clinically visible (Fig 2).
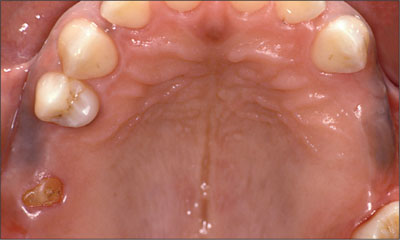
Fig 2 Maxillary occlusal view. The root fragment is clinically visible in the area of tooth 16.
Radiographic analysis revealed the recent extraction of tooth 45. This finding became important to the treatment planning for implant placement.
Radiographically, the residual root fragment appeared to be small and sequestered within the edentulous mucosa without any signs of acute inflammation. The radiological aspect of the partial dentition displayed three similar multi-tooth gaps. The maxillary ridges presented adequate coronoapical dimension for implant placement. A similar situation was observed in the mandible, where the inferior alveolar nerve was located rather apically, leaving enough space for a straightforward implant placement (Fig 3). Since the clinical evaluation revealed good orofacial dimension, the orthopanoramic radiograph and mounted diagnostic casts were judged to be sufficient for diagnostic and treatment-planning purposes.
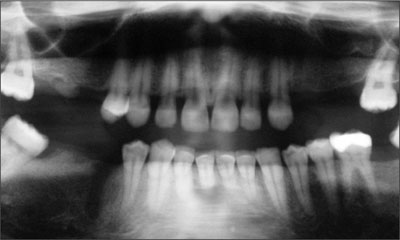
Fig 3 Panoramic radiograph displaying enough bone height. The residual root fragment and the post-extraction area 45 were issues to be considered for the treatment planning.
The treatment plan considered 3 three-unit implant-supported restorations to restore the maxillary right and left posterior sectors, as well as the mandibular right posterior zone. The vertical dimension of occlusion and occlusal contacts were stable at centric relation. The dimensions of the multi-tooth gaps were homogenous and presented a correct mesiodistal dimension for the allocation of three prosthetic units. Based on these diagnostic elements, implant placement was performed with two implants per multi-tooth gap (Fig 4).
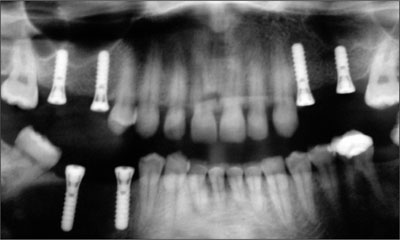
Fig 4 Post-surgical radiograph. The prosthetics-driven implant allocation and distribution ensured the fabrication of 3 three-unit fixed dental prostheses.
Six Straumann Standard Plus implants (endosteal diameter, 4.1 mm; length, 12 mm (sites 15, 24, 45, 47) and 10 mm (sites 17, 26); Regular Neck prosthetic platform, 4.8 mm) were placed. Primary stability was achieved with all implants, and flaps were repositioned in a non-submerged surgical approach. In order to enhance the esthetic appearance of the edentulous ridge, a lateral bone augmentation was performed simultaneously to the implant placement. During the healing phase, the patient was given a soft toothbrush and instructions for implant maintenance with chlorhexidine mouthwash during the first week.
After a healing period of 4 months, the healing caps were removed and the soft tissue status was assessed (Figs 5-8).
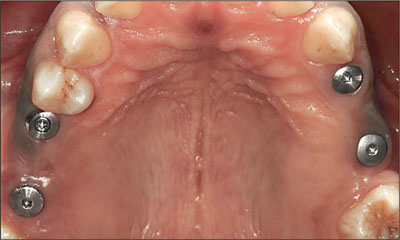
Fig 5 Clinical status of maxillary implants after 4 months of non-functional healing.
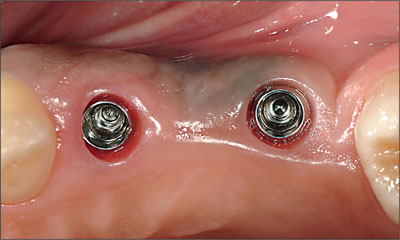
Fig 6 Close-up view of implants at sites 24 and 26, showing the healing status of the maxillary peri-implant mucosa.
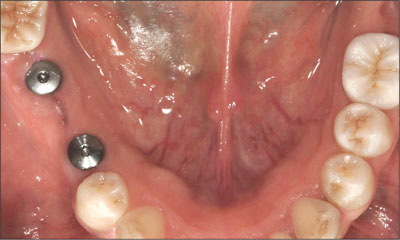
Fig 7 Clinical condition of the implants in the mandible after 4 months of undisturbed healing.
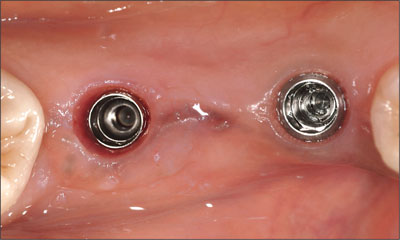
Fig 8 Close-up view of the implants in sites 45 and 47, showing the healing status of the mandibular peri-implant soft tissue after the removal of the healing caps.
A provisional phase was considered to be not essential in this particular case. The overall esthetic appearance was not compromised, and the vertical dimension of the occlusion was stable. Based on these parameters, the decision was made to proceed with the final restoration and to shorten the total treatment time.
Therefore, final impressions were made. Final upper and lower impressions were made at the implant level using two different kinds of impression copings. In the maxilla, screw-on impression copings were used due to the slightly deeper placement of the implants (Fig 9). In the mandible, the snap-on impression approach was selected according to a more superficial implant placement and a slightly thinner peri-implant mucosa (Fig 10).
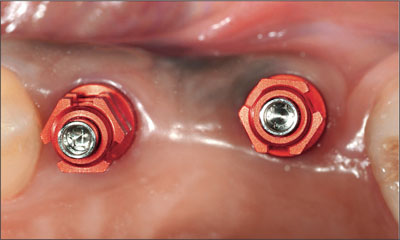
Fig 9 Prior to taking the implant-level impression at sites 24 and 26. Screw-on impression caps were selected for the maxillary open-tray final impression.
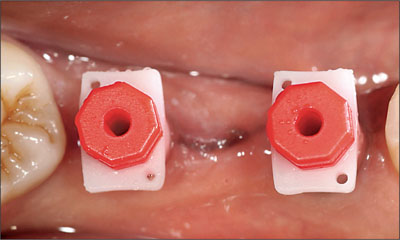
Fig 10 Prior to taking the implant-level impression of the implants in the mandible. Snap-on impression caps were selected for the closed-tray final impression.
After the interarch relationship was recorded, healing caps were tightened back onto the implants and the patient was rescheduled for the frameworks try-in one week later.
The different synOcta impression copings offered the same versatility at the time of fabricating the master cast (Figs 11-12). In the retrieved impression trays, the copings provided a stable fit for the implant analogs. Once the analogs were connected to the impression copings, the implant location was reproduced along with the position of the antirotational internal octagon (Figs 13-14).
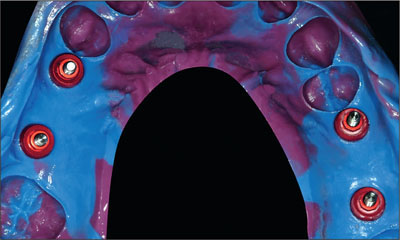
Fig 11 Impression with screw-on synOcta impression copings. Final maxillary open-tray impression.
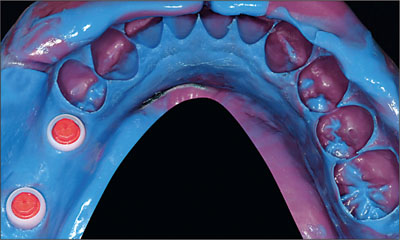
Fig 12 Impression with snap-on synOcta impression copings. Final mandibular closed-tray impression.

Fig 13 Maxillary final impression. Close-up view of screw-on copings.
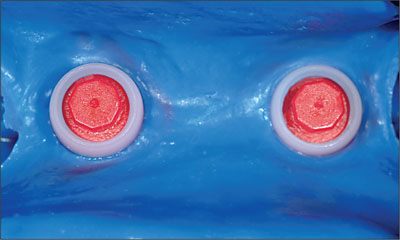
Fig 14 Mandibular impression. Close-up view of snap-on copings.
The selection of the definitive abutments was completed once the master casts, including the implant analogs, were fabricated and articulated (Fig 15). The implant-level impression offered the possibility of selecting the best suitable abutments on the mounted casts. In this particular case, five 4-mm solid abutments and an angled synOcta abutment were used according to the planned restorations and the occlusal relationship.
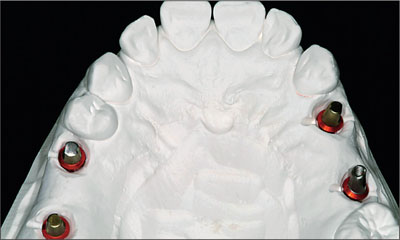
Fig 15 Maxillary master cast. Definitive abutments have been selected and used during the entire fabrication process of the fixed dental prosthesis before definitive transfer to the patient’s mouth.
Plastic copings (for the fixed dental prosthesis, FDP) and a synOcta coping (for the angled abutment) were used for the fabrication of the frameworks. The frameworks were fabricated directly onto the definitive abutments (Figs 16-17). In the areas where 4-mm solid abutments were used, the internal configuration of the copings (for FDP) resulted in a framework that ensured the definitive abutments could be transferred from the cast to the patient’s mouth. This would allow for the passive seating of the FDP (Figs 18-21).
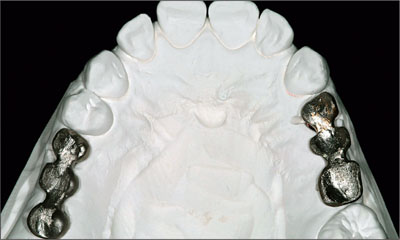
Fig 16 Maxillary frameworks.
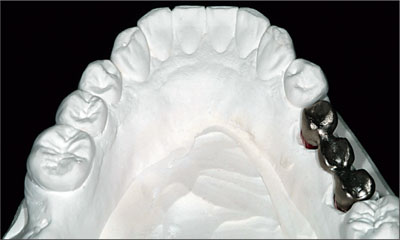
Fig 17 Mandibular framework.
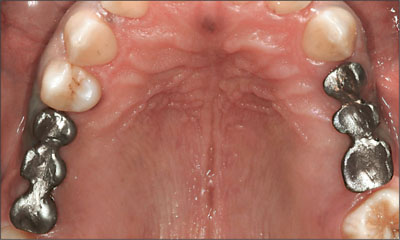
Fig 18 Maxillary frameworks try-in.
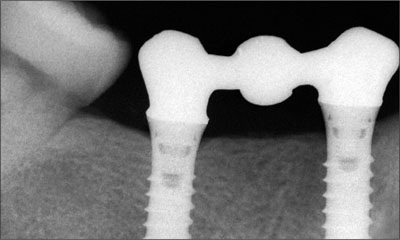
Fig 19 Radiographic assessment of the marginal adaptation of the mandibular framework.
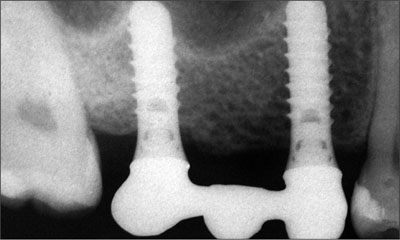
Fig 20 Radiographic assessment of the marginal adaptation of the right maxillary framework.
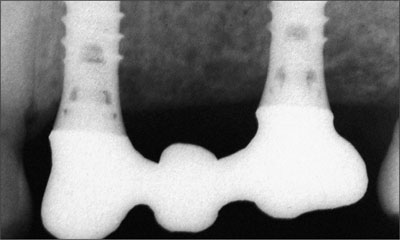
Fig 21 Radiographic assessment of the marginal adaptation of the left maxillary framework.
Following the metal frameworks try-in and before proceeding with the ceramic veneer, the occlusal relationship was verified. The ceramic work was then completed using a stratification technique, and the prostheses were glazed to achieve a natural-looking appearance (Figs 22-23).
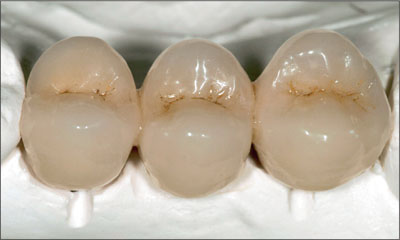
Fig 22 Definitive rehabilitation on the master cast.
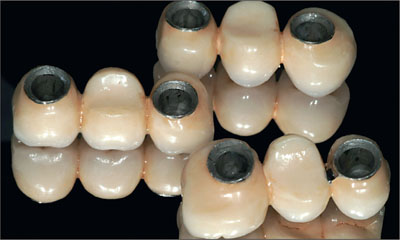
Fig 23 Internal view of the 3 three-unit FDPs.
At delivery, the healing abutments were removed and the definitive abutments were tightened to 35 Ncm. At this stage, none of the six implants rotated and the patient manifested no discomfort. Due to the abridged abutment length (4 mm), the solid abutments were sandblasted to improve mechanical retention (Fig 24). After an assessment of the seating and the pressure of the proximal contact areas, occlusal adjustment was undertaken, and the restoration was cemented (Figs 25-26).
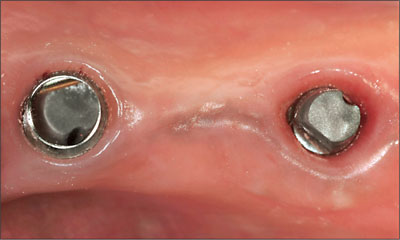
Fig 24 Sandblasted abutments were tightened to 35 Ncm.
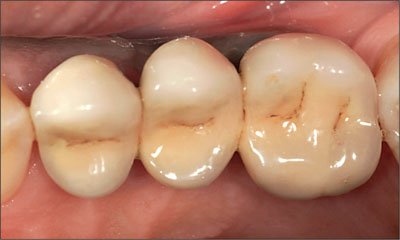
Fig 25 Occlusal view of the left maxillary implant-supported FDP.
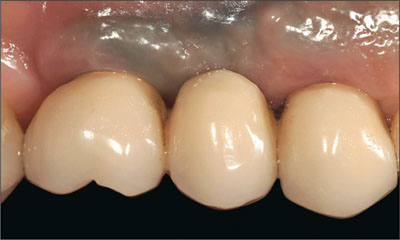
Fig 26 Lateral view of the maxillary left implant-supported FDP after cementation.
This case resulted in a conventional loading approach with definitive restorations, avoiding a provisional phase. The implant-supported restorations were initially cemented with provisional cement and, after a reasonable follow-up period, a dual-cure adhesive agent was used for the final cementation.
A panoramic radiograph was then taken to assess the final treatment outcome (Fig 27).
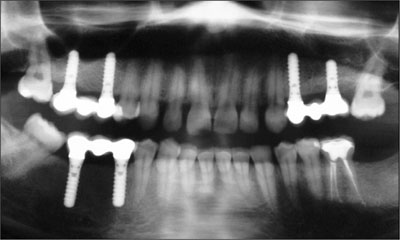
Fig 27 Final radiograph of the outcome.
The patient received maintenance instructions and was followed-up by the dental hygienist every three months during the first year. After that, she was referred to the regular recall system at the Student Clinic, University of Geneva.
At the 2-year follow-up, the patient presented a satisfactory clinical status (Figs 28-31).
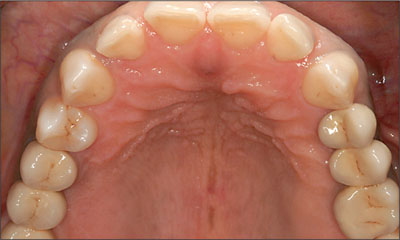
Fig 28 Maxillary occlusal view at 2-year follow-up.
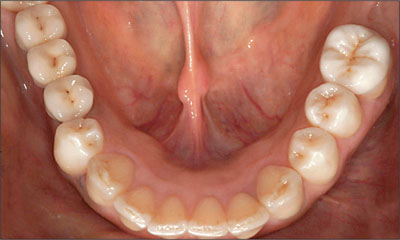
Fig 29 2-year follow-up, mandibular view.
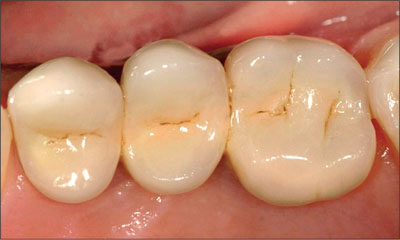
Fig 30 Close-up view of the maxillary right FDP at the 2-year follow-up.
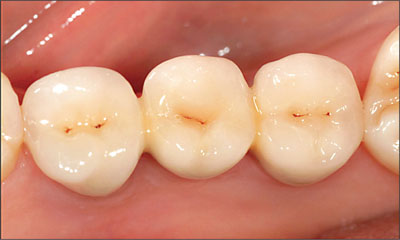
Fig 31 Close-up view of the mandibular FDP at the 2-year follow-up.
At the radiographic evaluation, optimal conditions at the peri-implant bone level were observed (Figs 32-34).
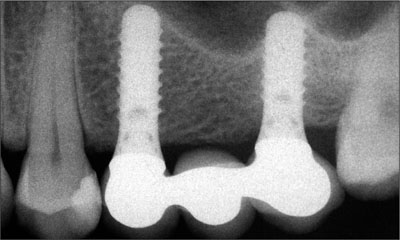
Fig 32 Two-year radiographic follow-up of the maxillary right implant-supported FDP.
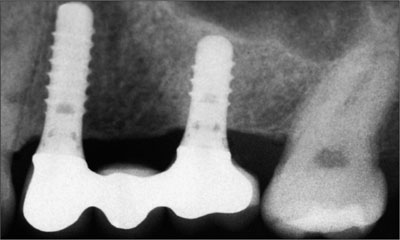
Fig 33 Two-year radiographic follow-up of the maxillary left implant-supported FDP.
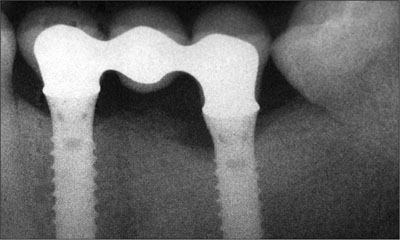
Fig 34 Two-year radiographic follow-up of the mandibular implant-supported FDP.
Acknowledgments
Surgical Procedures
Dr. Stéphane Pessotto – University of Geneva, Department of Stomatology and Oral Surgery.
Laboratory Procedures
Michel Bertossa – CDT, University of Geneva, Department of Fixed Prosthodontics.
4.4 Replacement of Multiple Teeth in a Partially Dentate Posterior Maxilla with a Fixed Dental Prosthesis and a Crown Using Conventional Loading Protocols
F. Higginbottom, T. Wilson
This 65-year-old female patient presented for implant-based restoration of the maxillary posterior region (25-27). Although this patient was free of medical compromise, her treatment was associated with several modifying factors.
She had been a patient of record in the practice for more than twenty years. Her initial treatment included extraction of the failing maxillary left first molar (Fig 1), and restoration with a fixed dental prosthesis (25-27) and crown (24). At the time of initial restoration, implants were not considered appropriate options for the replacement of single posterior teeth.
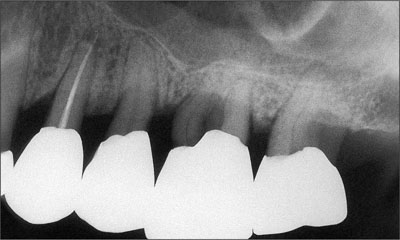
Fig 1 Pre-treatment radiograph, 1982.
The fixed dental prosthesis ultimately failed as a result of recurrent dental caries (Fig 2). Although the patient was provided with an implant-based treatment option for the re-treatment, this was declined because of the need for sinus elevation. A new tooth-supported fixed dental prosthesis was therefore fabricated. After approximately 7 years, the new prosthesis also failed, resulting in the loss of both abutment teeth.
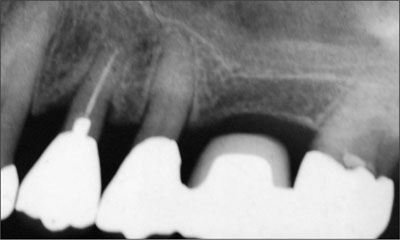
Fig 2 Radiograph of the initial FDP.
The patient accepted a new treatment plan, which included sinus elevation and ridge augmentation before implant placement. The grafts were allowed to heal for 6 months prior to implant placement.
Treatment was complicated by several modifying factors. These included bruxism, the absence of adequate anterior guidance, the less than favorable crown to implant ratios and the presence of type 4 bone.
Modifying factors:
-
Bruxism
-
Minimal anterior guidance
-
Unfavorable crown-to-implant ratio
-
Type 4 bone
These factors influenced the treatment options given to the patient. The available treatment choices were: doing nothing, placing a removable partial prosthesis, or placing dental implants and fixed dental prostheses. The patient choose the implant-based treatment option, and she was scheduled for sinus and ridge augmentation. A provisional removable partial prosthesis was fabricated for limited wear during the healing period. After 6 months of healing, the placement of three implants was planned (25: endosteal diameter, 4.1 mm; length, 10mm; Regular Neck platform, 4.8 mm; 27: endosteal diameter, 4.8 mm; length, 8 mm; Regular Neck platform, 4.8 mm – all Standard Plus implants) (Fig 3), and undertaken (Fig 4).
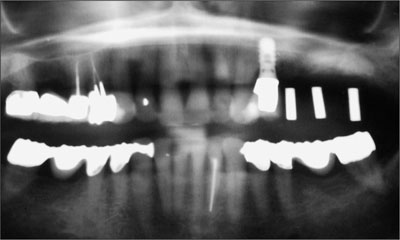
Fig 3 Treatment planning alignment for the placement of three implants.
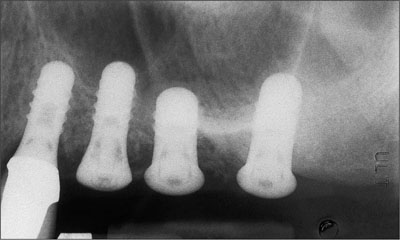
Fig 4 Radiograph of implants placed in sinus graft (12 weeks).
After twelve weeks of healing, restorative procedures began with impressions and provisional restorations (Figs 5-7).
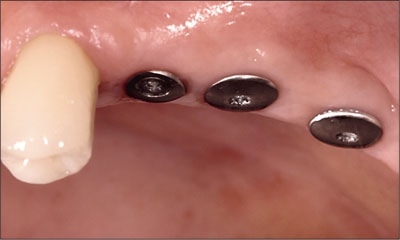
Fig 5 Clinical appearance of the implants in good position after 12 weeks of healing.
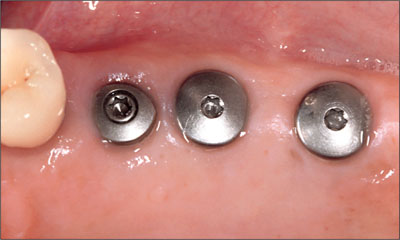
Fig 6 Occlusal view of the implants after 12 weeks of healing.
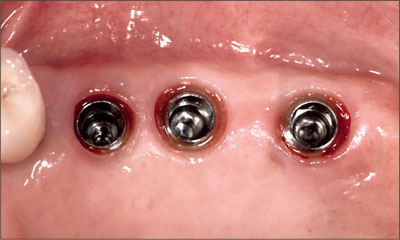
Fig 7 Healing caps removed and healthy peri-implant tissues visible. Note the relatively flat gingival contour, allowing for a cemented restoration.
Definitive impressions were made using screw-on synOcta impression copings (Figs 8-9).
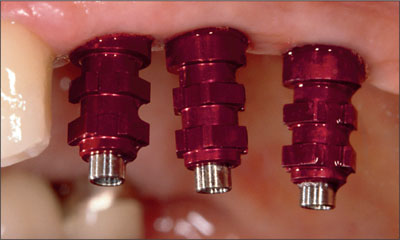
Fig 8 Screw-on synOcta impression copings seated for a open-tray impression.
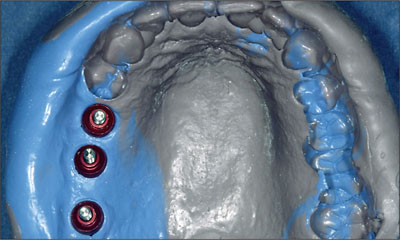
Fig 9 Definitive impression taken with polyvinyl impression material.
The implants were provisionalized using 4-mm solid abutments and an autopolymerizing resin fixed dental prosthesis (Figs 10-11).
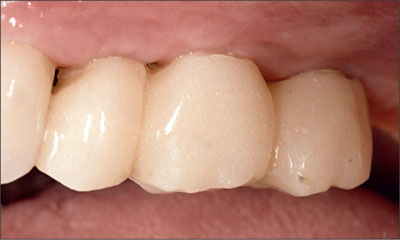
Fig 10 Provisional restoration fabricated with autopolymerizing resin over 4-mm solid abutments.
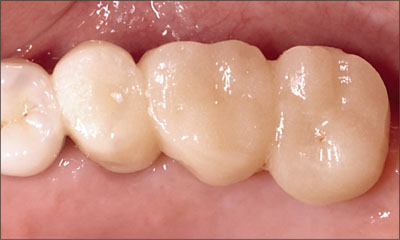
Fig 11 Occlusal view of the splinted provisional restoration.
Due to the modifying factors identified in the introduction, it was decided to splint the implants together with one fixed prosthesis. However, this presented a problem due to the angulation differences between the implants. There were several options for solving the angulation problem. Solid abutments could be prepared in the mouth. Custom abutments could be used, but the implants were considered too shallow for this option. Angled abutments presented the third and most viable choice. The angled abutments were selected in the laboratory using the Straumann prosthetic planning kit (Figs 12-15) .
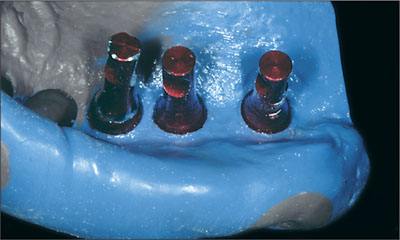
Fig 12 Implant analogs positioned in the impression.
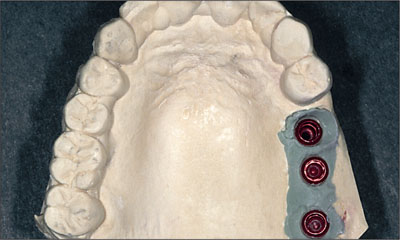
Fig 13 Master cast poured, with soft tissue analog adapted around the implant analog shoulders.
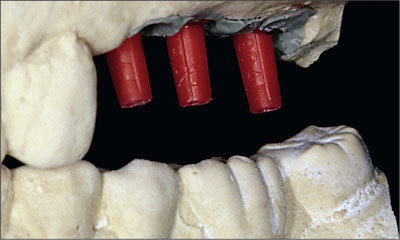
Fig 14 In the laboratory, the Straumann prosthetic planning kit is used to select the appropriate angled abutment.
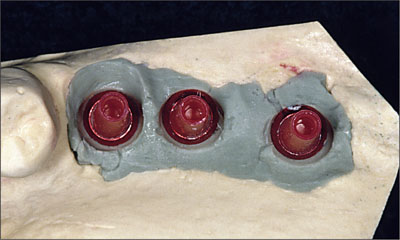
Fig 15 Occlusal view of the planning abutments selected, illustrating the parallelism.
After the selection of the appropriate abutments, a metal framework was constructed and returned for the verification of passivity in the mouth (Figs 16-20).
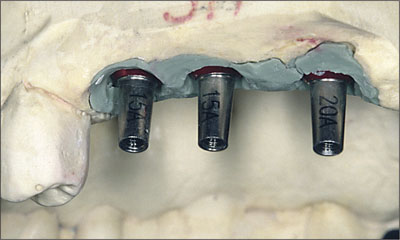
Fig 16 Two 15A and one 20A synOcta angled abutments are selected and seated on the master cast.

Fig 17 Occlusal view of the abutments selected. A framework will be fabricated for verification in the mouth.

Fig 18 Angled synOcta abutments assembled with an index on the master cast to carry to the mouth in one piece.
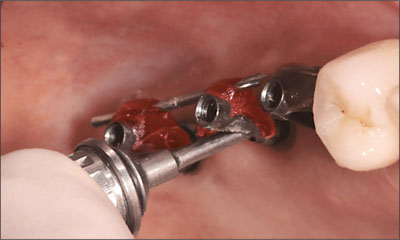
Fig 19 Angled abutments seated as a unit. The index will be removed for the framework try-in.
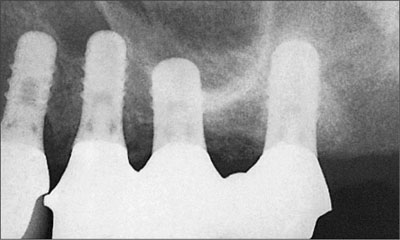
Fig 20 Radiographic view of the framework in place. The radiograph inclination was not appropriate for assessment of the restoration-implant interface (lack of thread visibility indicates less than ideal parallelism). The fit was satisfactory both visibly and by tactile senses.
After the verification of the articulation records, the framework was returned to the laboratory for ceramic application (Figs 21-23).
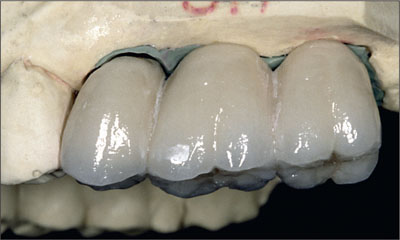
Fig 21 Completed metal-ceramic restoration.
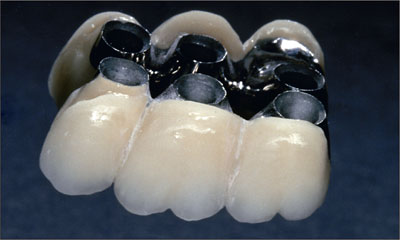
Fig 22 Completed metal-ceramic restoration.
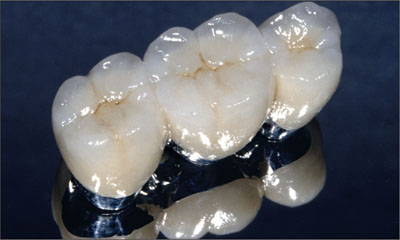
Fig 23 Completed metal-ceramic restoration.
The metal-ceramic fixed dental prosthesis was fitted and the occlusion adjusted. The restoration was seated with provisional cement, which would allow for removal, if necessary (Figs 24-29).
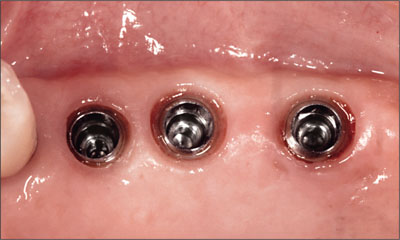
Fig 24 Provisional restoration removed, showing stable and nicely shaped peri-implant soft tissues.
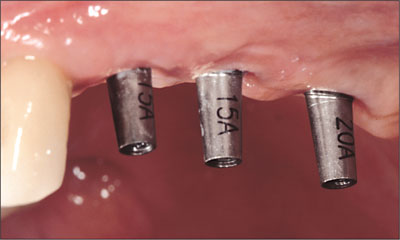
Fig 25 Angled synOcta abutments seated and torqued to 35 Ncm.
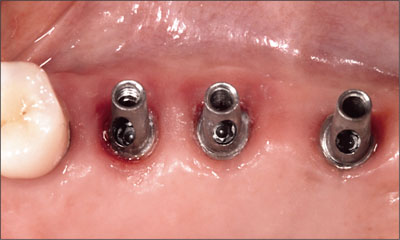
Fig 26 Angled synOcta abutments seated and torqued to 35 Ncm.
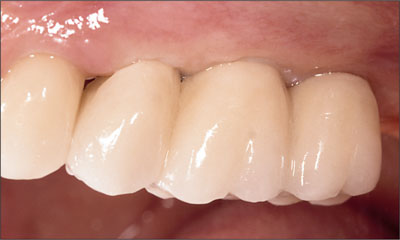
Fig 27 Final restoration seated.
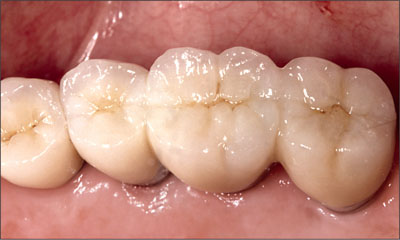
Fig 28 Occlusal view of final restoration.
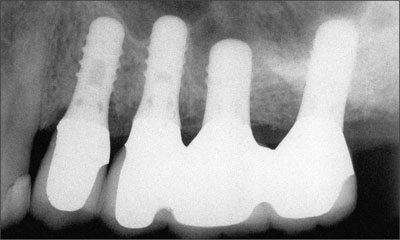
Fig 29 Radiograph at insertion of final restoration.
After two weeks, the patient returned for a post-insertion evaluation and the insertion of a habit appliance. The patient has had an uneventful follow-up period of over five years (Fig 30).
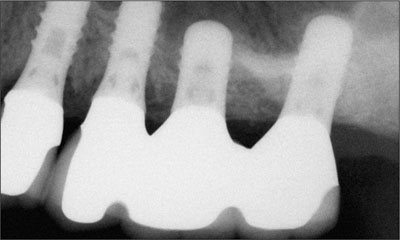
Fig 30 Five-year recall radiograph.
Acknowledgments
Laboratory Procedures
Jeff Singler
4.5 Replacement of Multiple Teeth in a Partially Dentate Posterior Maxilla with Crowns Using a Conventional Loading Protocol
G. S. Solnit, M. Kaufman
In 2004, an 84-year-old female patient presented at our practice with a hopeless prognosis for her maxillary right first and second premolars. These teeth were supporting a three-unit fixed dental prosthesis and had a cantilevered pontic replacing the first molar. Both teeth had combined endodontic and periodontal lesions, with significant bone loss in the area. The patient also had a large maxillary sinus apical to the first molar site (Fig 1).
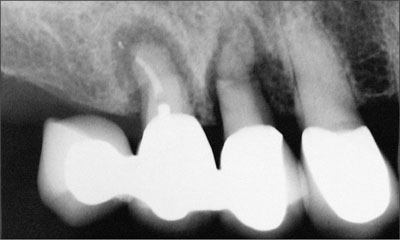
Fig 1 Radiograph depicting the condition of the existing fixed dental prosthesis at consultation.
The patient presented with normal facial form and upon normal smiling, she displayed the affected area. She reported mobility and pain with mastication. The fixed dental prosthesis displayed severe mobility and could be depressed into the alveolar sockets. Exudate was evident around both abutments. There were no significant medical problems reported and the patient reported taking no medications.
Both teeth were extracted and the existing prosthesis removed, and the alveolar sockets were grafted with autogenous bone and bone substitute material mixed together. The maxillary sinus was also grafted in the same fashion. The patient did not wear an interim prosthesis for two weeks. After two weeks, an interim removable partial denture was delivered and adjusted so that no pressure was exerted over the grafted areas. The denture was relined with a soft liner and checked every three to four weeks. The liner was changed as needed and each time, the area was checked carefully to make sure there was no pressure over the grafted sites. The grafts were allowed to heal undisturbed for three months.
After three months of healing, three Straumann implants were placed in the first premolar, second premolar, and first molar positions, utilizing a surgical template. Implants with a Regular Neck prosthetic platform were placed in the premolar positions and an implant with a Wide Neck prosthetic platform was placed in the molar site. The interim denture was again relieved and checked to make sure no pressure was exerted over the implants. The implants were allowed to heal for six weeks undisturbed.
After conventional healing (4 months) was complete, three 5.5-mm solid abutments were placed and torqued to 35 Ncm. Because of the acceptable angulation and shallow placement of the implants, the cemented approach for the final restorations was indicated. The 5.5-mm solid abutments were appropriate for adequate retention of the final restorations. They also allowed space for acceptable metal ceramic restorations. The solid abutment in the molar region was reduced slightly to provide a little more space. This was considered a better alternative than placing a 4.0-mm abutment, which may have had inadequate retention for the final restoration (Figs 2-3). A plastic reduction coping was fabricated and provided to the laboratory.
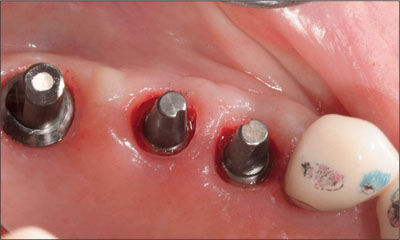
Fig 2 Occlusal view of the solid abutments in place. Note the correct mesial/distal and buccal/lingual positioning of the implants. A slight reduction of the solid abutment in the molar site provided more clearance for restorative materials.
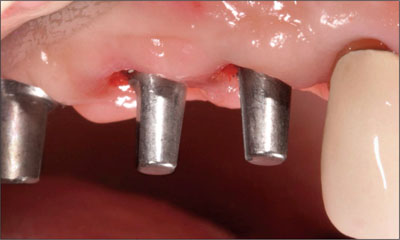
Fig 3 Buccal view of the solid abutments in place. Note the shallow depth of the implant placement, making the cemented approach a more acceptable restorative option.
Standard impression procedures were followed, utilizing the snap-on impression components. An impression was made using a custom tray and a polyvinyl siloxane impression material. The master cast was poured in a low expansion dental stone. A soft tissue mask was fabricated over the analogs to simulate the emergence of the surrounding soft tissue. Tissue expansion was not necessary, as the implants were of the appropriate emergence diameter and the implants were placed at the appropriate depth (Fig 4).
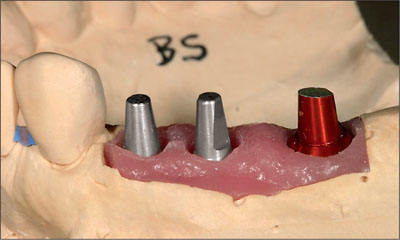
Fig 4 The master cast with the analogs in place and the soft tissue mask. Note the reduction on the analog in the molar site, which was recorded using a plastic coping.
The final metal-ceramic restorations were fabricated as individual units. Proximal contacts were carefully adjusted on the master cast to ensure tight contacts and the completely passive seating of the restorations (Fig 5).
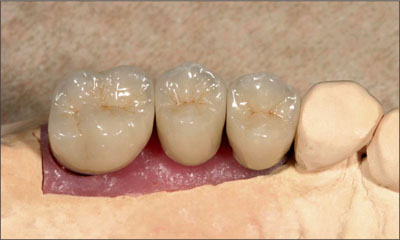
Fig 5 The final individual metal-ceramic restorations on the master cast. All proximal contacts were carefully adjusted to ensure adequate contact and the passive seating of the restorations.
The restorations were tried into the patient’s mouth to verify passive fit with a silicone fit checking material. Proximal contacts were verified with mylar shimstock and dental floss. Extreme care must be taken during the seating of individual restorations on implants. It is imperative that a silicone medium is utilized to assess the complete seating of the restorations because proximal contacts can prevent seating completely. Detrimental forces to the implants are also possible.
Once the complete seating of the restorations was established, they were temporarily cemented in position with the same silicone medium. The occlusion was checked to ensure centric contacts and adequate clearance during excursive movements with articulating paper (Fig 6).
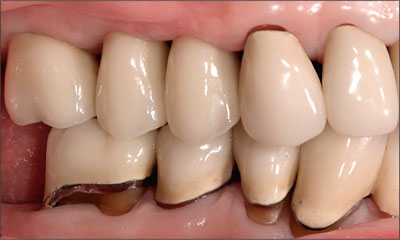
Fig 6 The final restorations are temporarily luted to place with a silicone medium. The occlusion can then be checked to ensure appropriate centric contacts and proper disclusion during excursive movements.
Once the occlusion was verified, the final restorations were luted to place with a resin-reinforced glass-ionomer cement. A thin layer of cement was applied and the excess was carefully removed while the patient was fully anesthetized (Figs 7-9). A periapical radiograph was taken to assess the final outcome of treatment (Fig 10). A periapical radiograph was taken once again at the three-year follow-up (Fig 11).
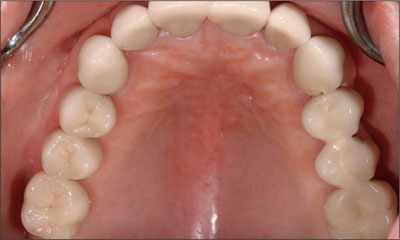
Fig 7 Occlusal view of the final restorations.
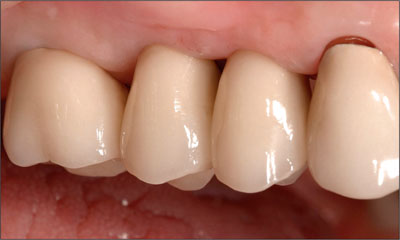
Fig 8 Buccal view of the final restorations.
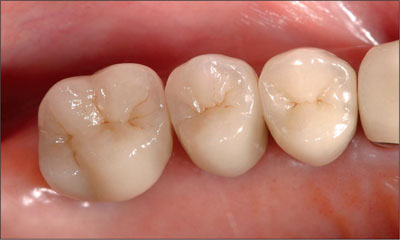
Fig 9 Occlusal view of the final restorations. Note the acceptable proximal contacts between the individual restorations.
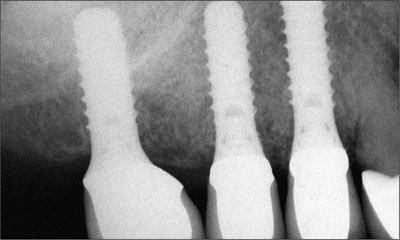
Fig 10 Periapical radiograph depicting the passive fit of the restorations and good bone-to-implant contact surrounding all three implants.
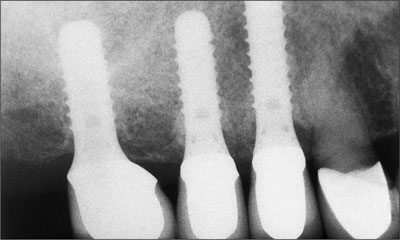
Fig 11 Radiograph taken at the three year follow-up.
Acknowledgments
Laboratory Procedures
Tim Ide
4.6 Replacement of Two Teeth in a Partially Dentate Posterior Maxilla with a Fixed Dental Prosthesis Using a Conventional Loading Protocol
U. Belser, D. Buser
In September of 1995, a 64-year-old female patient presented to our clinic with a distally shortened arch in the left maxilla and the desire for a fixed rehabilitation. The patient’s medical history did not reveal any major issues, and she did not take any significant medication. She was a non-smoker and did not report any allergies. The patient wished to restore her chewing function on the left side, which was severely compromised due to the missing teeth 25, 26, and 27. The antagonistic lower teeth were present and in acceptable condition.
A decision was made together with the patient to place two implants according to a staged protocol at sites 25 and 26 (25: Straumann Standard implant, endosteal diameter, 4.1 mm; length, 12 mm; Regular Neck prosthetic platform, 4.8 mm; 26: Straumann Standard implant, endosteal diameter, 4.8 mm; length, 10 mm; Regular Neck prosthetic platform, 4.8 mm), after a sinus-grafting procedure. Sinus grafting was necessary to establish adequate bone volume for stable implant placement, due to the insufficient bone height at the future implantation sites (Fig 1). The patient gave her informed consent that – as this was the standard of care at that time – a healing period of at least 6 months would be utilized after the sinus-grafting procedure before the implants could be placed. Furthermore, under these conditions, i.e. implants inserted into grafted bone, a conventional loading protocol comprising 3 months of healing prior to restoration represented the standard procedure.
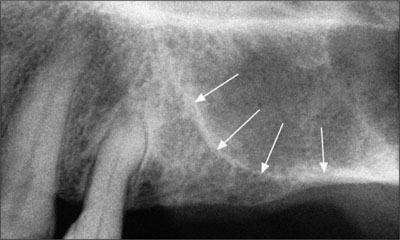
Fig 1 Radiograph of the posterior region of the left maxilla. The wide-stretching maxillary sinus at sites 25-27 and the resulting lack of vertical bone height in this region are clearly visible. For stable implant anchorage, a sinus-grafting procedure was considered indispensable.
At the time of implant placement, i.e. 8 months after the anterior sinus-grafting procedure, good primary stability was achieved. Subsequent to implant surgery, the implants were allowed to heal for 12 weeks.
At the time of the removal of the healing caps 12 weeks after implant placement, the mucosa presented healthy and free from bleeding on probing (Fig 2). The implants were well integrated and revealed ankylotic stability, so the decision was made to make an impression for loading with a provisional restoration, according to a conventional loading protocol (Ganeles and Wismeijer, 2004).
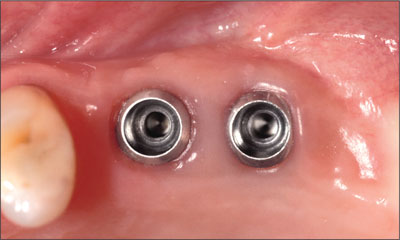
Fig 2 Implants 25 and 26 after the removal of the healing caps, 12 weeks after the implant placement. Note the superficial location of the implant shoulders and the related inflammation-free peri-implant mucosa.
Two solid abutments, 5.5 mm and 7.0 mm in length, were secured on the implants at a torque of 35 Ncm – note both the superficial implant shoulder location, compatible with cemented restorations, and the optimal implants axis and parallelism (Fig 3). Then, an impression was taken to generate a master cast (Fig 4).
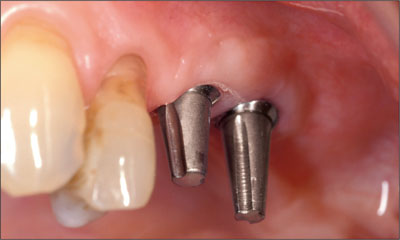
Fig 3 The situation 12 weeks after implant placement, before impression-taking, in view of the fabrication of a provisional restoration. Two solid abutments have been inserted.
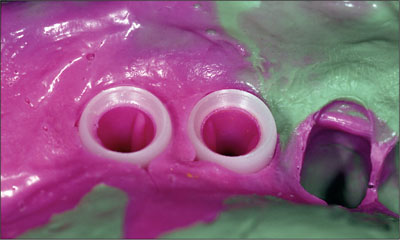
Fig 4 Close-up view of the impression taken with an elastomeric impression material. The two implant shoulders have been picked up by means of self-anchoring injection-molded impression caps.
Subsequent to impression-making, two self-anchoring plastic shoulder analogs were positioned on the impression caps (Fig 5). Before pouring the cast, reinforcement pins were inserted. In 1996, integral implant analogs were not yet available, so at that time, this approach was the preferred one.

Fig 5 The impression with the shoulder analogs in place, before the insertion of the reinforcement pins.
Subsequently, the cast was poured, with the cervical portions of the shoulder analogs representing the implant shoulders (Fig 6).
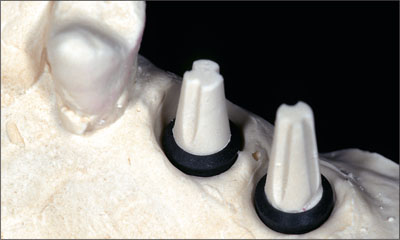
Fig 6 The prefabricated plastic implant shoulder analogs and solid abutments, represented in stone in sites 25 and 26.
In the dental laboratory, a splinted provisional restoration was fabricated from acrylic resin (Figs 7-8). This was cemented to the solid abutments in the patient’s mouth two weeks after impression-making (Figs 9a-b). The provisional restoration was loaded according to a conventional loading protocol.
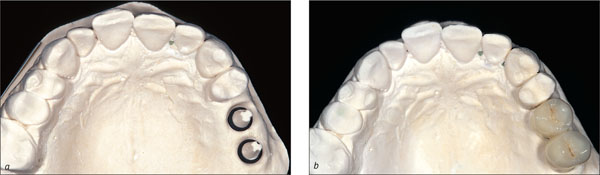
Figs 7a-b The completed cast, comprising both prefabricated plastic implant shoulder analogs and solid abutments, represented in stone in sites 25 and 26, and the splinted, cementable provisional implant crowns before delivery, on the cast.
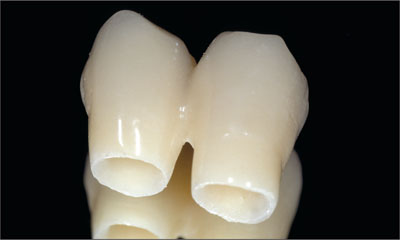
Fig 8 The cementable provisional implant crowns in close-up view.
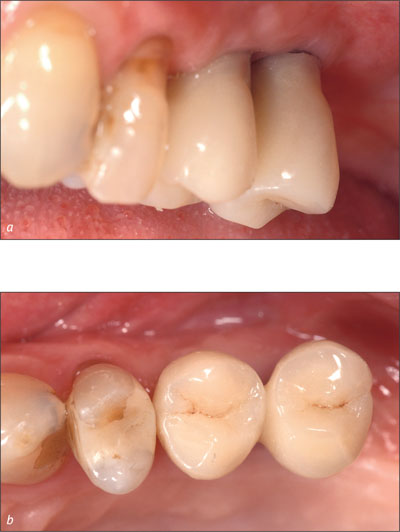
Figs 9a-b The cemented provisional splinted implant crowns at sites 25 and 26 in the patient’s mouth at about 14 weeks after implant placement, buccal and occlusal views, conventionally loaded.
This timing permitted the patient to become accustomed with the fixed implant prosthesis and to approve the proposed design for the final prosthesis.
The provisional restoration remained in situ for eight weeks. About 10 weeks after the patient’s first prosthodontic visit to our clinic, a final impression was made for the fabrication of the final restoration.
A two-unit splinted metal-ceramic fixed dental prosthesis (FPD) was fabricated in the dental laboratory. Again, a cemented design was chosen (Figs 10-11).
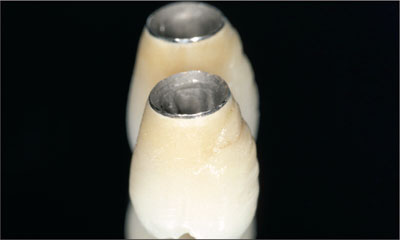
Fig 10 Close-up view of the two-unit splinted cementable metal-ceramic FDP before delivery. Note the flat emergence profile of the restoration.
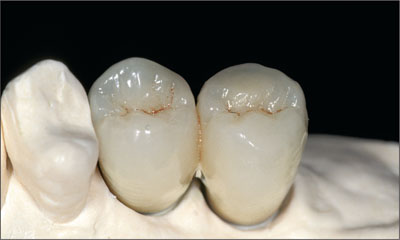
Fig 11 The splinted cementable metal-ceramic FDP on the master cast.
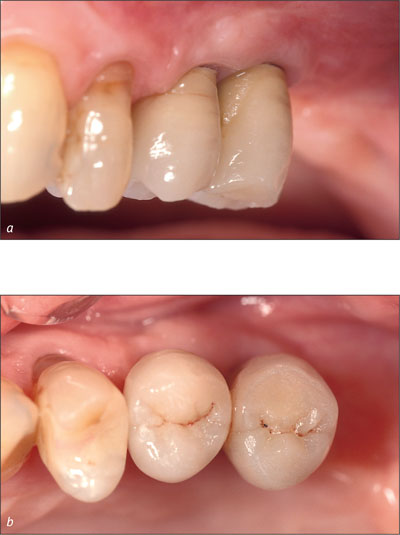
Figs 12a-b The final restoration in the patient’s mouth after cementation, labial and occlusal aspects.
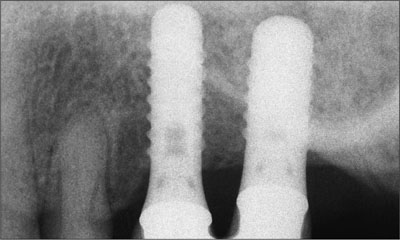
Fig 13 The periapical radiograph, taken after the cementation of the final restoration at about 15 weeks after the patient’s first visit to our clinic, confirms normal peri-implant bone structures as well as the precise seating of the suprastructure on the implants.
Eleven years later, the conventionally loaded implants are still functioning successfully (Figs 14-15).
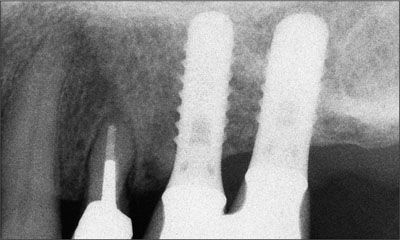
Fig 14 Radiologic follow-up 11 years after implant placement. The peri-implant bone is stable.
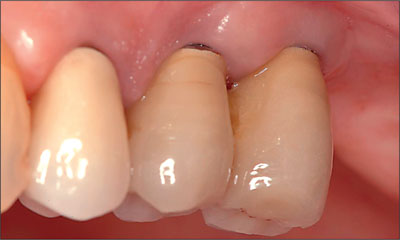
Fig 15 Clinical follow-up 11 years after implant placement.
Meanwhile, tooth 24 received endodontic treatment and a metal-ceramic crown.
Concluding Remarks (Epicrisis):
In retrospect, both the number and location of the implants and the choice of splinting of the respective implants should be questioned.
First, the original status of tooth 24 (extremely short root) would probably have justified its extraction in the scope of a more general treatment plan addressing the distally shortened left maxillary arch. In fact, tooth 24 later required root-canal therapy and a subsequent restoration with a metal-ceramic crown, considerably increasing treatment costs and still representing a limited prognosis. In other words, its extraction would have allowed either a reconstructive solution based on implants in sites 24 and 25, comprising a distally cantilevered unit, or implants in sites 24 and 26, restored with a three-unit fixed dental prosthesis, comprising a central pontic. The first solution would have permitted the avoidance of a sinus grafting procedure and thus led to a significantly less invasive overall treatment.
Second, the splinting of the two implants in 25 and 26 may not have been necessary. There is no strong evidence in the current literature that indicates that implants placed in grafted bone require splinting. One should keep in mind, however, that single implant restorations offer the advantage of superior marginal fidelity as well as the ease of an eventual reintervention. Furthermore, they facilitate routine oral hygiene measures.
Acknowledgments
Laboratory Procedures
Alwin Schönenberger – Master Dental Technician, Glattbrugg, Switzerland.
Single-Tooth Gaps in the Posterior Maxilla or Mandible
4.7 Replacement of a Maxillary Left Second Premolar Using an Immediate Restoration Protocol
D. Morton, J. Ruskin
In June 2002, a healthy and cooperative 42-year-old female patient was referred for consultation and for the treatment of a fractured maxillary left second premolar (Fig 1).
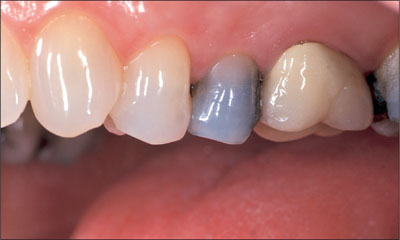
Fig 1 Pre-treatment lateral view of maxillary second premolar (25).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


