Case• 57. Oral cancer
SUMMARY
A 72-year-old man with squamous cell carcinoma is referred to your cancer treatment centre. How should he be managed?
History
Complaint
The patient complains only of discomfort on wearing his dentures and earache on the right, despite the large lesion.
History of complaint
He first noticed symptoms 6 weeks ago and has sought treatment because of the earache. He had noticed a ‘crack’ in his tongue that has not healed for some time but this has always been painless.
Medical history
He had a small myocardial infarction 7 years ago and has mild hypertension for which he takes amlodipine and aspirin. He has smoked 20 or more cigarettes a day for the last 55 years and drinks a quarter bottle of whisky per day.
Examination
Extraoral examination
The examination of the neck is normal apart from a possible mass just below the right angle of the jaw. It is difficult to ascertain whether or not the mass is hard. It is deeply situated and approximately 15 mm in diameter.
Intraoral examination
▪ The appearance of the tongue is shown inFigure 57.1What do you see?
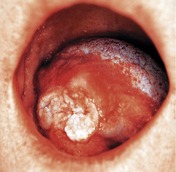 |
| Fig. 57.1 |
There is a large fungating ulcer arising on the right lateral border of the tongue. It is approximately 30 mm in size and has raised everted borders. Towards the dorsal surface the mucosa bulges, as if there is a mass beneath the intact epithelium, and there is a white patch affecting the mucosa just dorsal to the ulcer margin.
If you could palpate this ulcer you would find that it is indurated (firm or hard on palpation) and extends down towards the floor of the mouth and up beneath the dorsal mucosa towards the midline. The lesion is clearly much larger than it looks. The patient has reduced tongue mobility.
Diagnosis
In this case the diagnosis has already been made at the referring hospital. The patient has squamous cell carcinoma and the appearance and presentation are typical. The patient knows the diagnosis.
▪ Why might the patient have earache?
Ear pain is thought to result from malignant infiltration (or other damage) of nerves that pass through or supply the ear on their way to the periphery. Thus in the tongue or pharynx, pain may be generated by involvement of the lingual nerve, which contains fibres from the chorda tympani from the ear and the auriculotemporal nerve (branch of the mandibular division of the trigeminal nerve), which also supplies the external auditory meatus. Similar referred pain may result from involvement of the glossopharyngeal nerve.
Principles of treatment
▪ What are the principles of treatment for oral squamous cell carcinoma?
Patients with oral carcinoma often present too late for cure and some may not benefit from treatment. Three treatment options are possible:
1. attempted cure
2. active palliative care
3. supportive care only pending death.
If cure is attempted, the highest chances of success are given by multimodality treatment – a combination of surgery, radiotherapy and, more rarely, chemotherapy. The most aggressive treatment that the patient is able to withstand will be recommended because, if the first round of treatment fails, the chances of survival are much reduced.
Further investigations
▪ How might you predict the chance of successful treatment?
By using staging and grading.
The chances of successful treatment depend on how large the carcinoma has grown and whether it has already spread to other sites in the body. Staging is a standardized method for assessing these parameters and the stage is used to predict survival and also to plan treatment. Accurate staging is essential.
All malignant neoplasms are staged by determining the tumour size (T), the lymph node status (N) and the presence of distant metastasis (M). These parameters are then combined to give the TNM stage. Details for staging oral carcinoma are shown below
| T | T1 | Carcinoma less than 2 cm in maximum diameter |
| T2 | Carcinoma 2–4 cm in maximum diameter | |
| T3 | Carcinoma greater than 4 cm in maximum diameter | |
| T4 | Carcinoma extends to involve other structures such as mandible or skin | |
| N | N0 | No lymph node metastasis |
| N1 | Metastasis in a single ipsilateral lymph node less than 3 cm diameter | |
| N2a | Metastasis in a single ipsilateral lymph node 3–6 cm in diameter | |
| N2b | Metastasis in multiple ipsilateral nodes, none larger than 6 cm | |
| N2c | Metastasis in bilateral or contralateral nodes, none larger than 6 cm | |
| N3 | Lymph node metastasis greater than 6 cm in diameter | |
| M | M0 | No distant metastasis |
| M1 | Distant metastasis |
The stage is then determined by the combination of TNM scores. Survival falls with increasing stage. Note how important cervical metastasis and large carcinomas are in determining stage, and therefore survival.
| Stage | Combinations |
|---|---|
| Stage 1 | T1, N0, M0 |
| Stage 2 | T2, N0, M0 |
| Stage 3 |
T3, N0, M0
or
T1–3, N1, M0
|
| Stage 4 | Any tumour that is:
T4
N2 or N3
M1
|
Staging depends on the fact that carcinomas tend to progress in a predictable way. First they enlarge by invading the surrounding tissues, then cells break away and travel via the lymphatics to seed metastases in lymph nodes. Blood-borne metastases to distant sites develop last. Although the sequence is usually predictable, the speed at which any individual carcinoma progresses through these stages varies widely.
Grading is a histological method to determine how aggressive a carcinoma is and how quickly it is likely to progress (or may already have progressed) from stage to stage. It is a measure of how differentiated the carcinoma epithelium is, that is, how much it resembles its tissue of origin. Well differentiated carcinomas grow in the tissues as large islands and form keratin. They usually grow slowly and metastasize late. Poorly differentiated carcinomas have more cytological pleomorphism, no keratin and invade more aggressively as small clusters of cells or even as single cells. They are more likely to produce metastases early in their course.
Staging is more important than grading, because the size and extent determine whether surgery is possible. Grading is useful in deciding which treatments are appropriate and how radical they should be.
▪ How will you determine the disease stage?
Size (T) can be determined by clinical examination. This is not very accurate and, if the carcinoma is posteriorly placed, may require an examination under general anaesthetic. Radiographs must be taken to assess involvement of bone as bone invasion automatically indicates T4 size. Imaging provides a more accurate estimate of size and extent than clinical examination.
Presence of lymph node metastasis (N) can be judged by clinical examination. Large, hard, fixed nodes will be obvious but lymph nodes nonspecifically enlarged as a result of ulceration or infection may also be present. Enlarged lymph nodes may require fine needle aspiration to confirm whether or not carcinoma is present (see Case 20). Imaging is very useful to detect small lymph node metastases and metastases in deeply sited nodes. The patient should have computerised tomography (CT), magnetic resonance imaging (MRI) or positron emission tomography (PET) scans to detect involved lymph nodes. Which is used will depend on local circumstances.
Distant metastases (M) should be sought by clinical examination and imaging. The imaging modalities noted above may all be used together with serological tests such as liver function tests (reflecting liver metastases).
After staging investigations this patient’s carcinoma is staged as T2, N0, M0 making it a stage 2 lesion. The size of the primary is at the upper limit of the T2 category. Fine-needle aspiration of the palpable submandibular lymph nodes detects no carcinoma and it has to be assumed that they are enlarged as an inflammatory/immune reaction to the ulcer rather than by metastasis. No other enlarged lymph nodes are evident on imaging. The chest radiograph and abdominal ultrasound appear to exclude distant metastasis and liver function tests are consistent with the patient’s alcohol intake. An anaesthetist declares the patient fit for the long general anaesthetic that would be required for surgery. The patient could opt for any treatment that is recommended.
In general the 5 year survival rate for oral carcinoma is poor. This is because of late presentation, leading to large carcinomas on presentation, often with extensive lymph node and distant spread. In addition, many patients are medically compromised by a lifetime of heavy smoking and excessive alcohol intake or are elderly and infirm and cannot accept aggressive treatment.
The survival rates for oral carcinoma of all sites are shown in Figure 57.2. These are Kaplan–Meier survival curves and each step in the line represents one of the study population dying of carcinoma at the time indicated on the x axis. The graphs show the disease-specific survival, on the left broken down by stage and on the right broken down by presence of lymph node metastases. Note how important metastasis is in determining survival.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


