Case• 54. A gap between the front teeth
SUMMARY
A 35-year-old man has noticed a gap appearing between two incisor teeth. What is the cause and how can you treat him?
History
Complaint
The patient is concerned about the gap between the crowned upper right central incisor tooth and lateral incisor.
History of complaint
He noticed the gap about 9 months ago and feels that it has enlarged, that the teeth have drifted forwards and that the crowns are now loose. He has had no symptoms from these or any other teeth.
Medical history
He has mild asthma controlled with an inhaled steroid and salbutamol. He does not smoke.
Dental history
The patient is new to your practice. He attended the dentist regularly, previously going every 6 months but now less frequently. The crowns are approximately 6 years old and were fitted to replace some unsightly fillings.
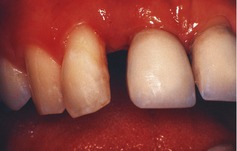
▪ The patient’s anterior teeth are shown inFigure 54.1. What do you see and how do you interpret the appearances?
The upper right lateral incisor is rotated mesiolabially and the central incisor distolabially. There is recession on both central and lateral incisors. The gingival tissues have some rounding of the margin and no obvious gingivitis, though there is loss of stippling and contour. The appearances suggest labial drifting as a result of loss of periodontal support. Pocketing is probably present even though it is not obvious.
Examination
Extraoral examination
There is no lymphadenopathy and no temporomandibular joint signs. The two crowns, although prominent and rather light in shade, are under control of the lower lip associated with a competent lip seal. The patient has a broad smile and moderately high lip line.
Intraoral examination
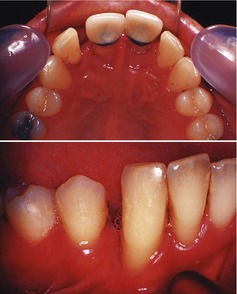
The oral mucosa is healthy, there is no caries and only a few amalgam restorations but there is focal marginal inflammation and plaque lying interdentally. The metal ceramic crowns on the two upper central incisors have good margins but there is 3 mm recession palatally and both teeth are grade 2 mobile. A further diastema is present in the opposing arch between the lower right canine and first premolar (Fig. 54.2) and the adjacent lateral incisor has grade 3 mobility.
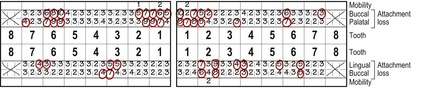
The gap between the upper central incisor and the lateral incisor is at least 3 mm and on gently probing the area there is profuse bleeding. The gingival tissue in that area is red, inflamed and has lost any contouring or stippling. There are deep probing depths on several teeth and mobility. Probing depths and gingival bleeding are shown in Figure 54.3. For details of indices and periodontal examination see Case 38.
The crowns of the upper incisors are rather bulky palatally, probably as a result of inadequate tooth preparation. On closing to intercuspal position the lower teeth occlude on the crowns in premature contact and displace the teeth labially. In both instances the entire tooth is loose, not just the crown.
Investigations
All teeth are vital.
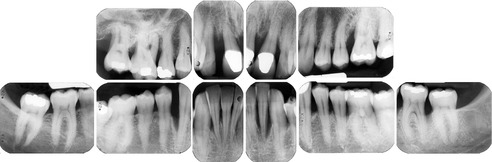
The choice of radiographs for periodontal diagnosis is reviewed in Case 38. Periapical radiographs for this patient are shown in Figure 54.4.
Diagnosis
▪ What is your diagnosis?
The patient has chronic gingivitis and localized periodontitis. The periodontitis has reduced the bony support for the upper and lower right anterior teeth and they have drifted labially. Bone loss extends close to their apices and they would have drifted further had they not been retained by the high lower lip line and competent lips. Recession is also the result of the periodontitis (see Case 4).
However, the pattern of periodontitis is unusual. The patient is only 35 years old but has severe localized attachment loss.
▪ What causes severe localized periodontitis?
The causes are usually local factors affecting the distribution of chronic periodontitis, such as:
• food packing and diastemas
• overhanging and poorly contoured restorations
• subgingival calculus
• destructive habits and self-inflicted injury
• perio-endo lesions
• root fractures
• high fraenal attachment
• localized aggressive periodontitis.
▪ Can any of these explain this patient’s pattern of disease?
Primarily the incisors and first molars are involved. The pattern of localized destruction and the shape of the deep infrabony pockets suggests localized aggressive periodontitis. This is the currently accepted diagnostic term for this presentation following the International Workshop for the Classification of Periodontal Disease in 1999. Previously this pattern would have been labelled localized juvenile periodontitis and in an adult might have been referred to as postjuvenile periodontitis. The new name has been chosen to reflect the fact that both adults and adolescents may be affected.
Although the crowns have good margins they are in traumatic occlusion and the jiggling forces on closing would increase the mobility of the teeth.
Treatment
▪ Is this patient suitable for treatment in general practice?
The severity of the complaint and the age of the patient indicate that there is a predisposition to periodontitis and so it may progress despite treatment. Initial phases of treatment could be carried out in general dental practice but some teeth already have a very poor prognosis. This is a complex case and unless you have a special interest or are a specialist in periodontology, the case might be best referred for treatment.
▪ What would you include in your letter of referral?
• Patient’s name, title, age and address including full postcode.
• Short dental history including pattern of attendance and past treatment needs.
• Relevant medical history.
• Your clinical findings including any special test results or study models you have.
• Anything else that you feel is relevant or will save time or a misunderstanding at the time of consultation.
• Whether you are referring for advice, a single aspect of treatment or comprehensive treatment to be undertaken.
• The radiographs or digital images should be sent with the letter so that repeat radiographs and the consequent radiation dose can be avoided.
▪ What treatment plan would be appropriate?
The prognosis for the three worst affected upper anterior teeth is hopeless as a result of loss of bony support, drifting and poor appearance. Additionally, if the teeth were to be saved, they would require new crowns. The upper right first molar has furcation involvement and bone loss to the apex and must also be extracted. The anterior teeth are symptomless and do not require immediate extraction but should be extracted in the near future to preserve what alveolar bone remains. An immediate replacement denture is the treatment of choice because no definitive restorations can be planned until the periodontitis is brought under control and the longer term prognosis for the other teeth is clear.
In the lower arch the left lateral incisor has bone loss to the apex and probably requires extraction. The long-term prognosis for the lower right canine remains to be determined but, at least initially, it is worth taking a cons/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses