Case• 23. A tooth lost at teatime
SUMMARY
A 78-year-old female patient has lost a tooth while eating. What is the cause and what will you do?
History
Complaint
The patient reports that one of her front lower teeth has been loose recently. The tooth simply fell out yesterday when she bit a biscuit. There was no pain before, during or after losing the tooth.
History of complaint
This woman has attended your practice for many years and has a well-cared-for mouth, a low caries rate and minimal periodontal disease. She is concerned that a healthy tooth has come out so easily and also that she has had no pain or bleeding from the area since.
Medical history
Five years ago she fractured her arm in a fall and a diagnosis of osteoporosis was made. She takes calcium supplements daily and alendronate (Fosamax) weekly.
Examination
Extraoral examination
Oddly, there is no lymphadenopathy, no tenderness to palpation over any of the facial skeleton and no obvious halitosis.
Intraoral examination
The patient is partially dentate and wears dentures. Her mucosa is normal, the mouth is not dry, there is no active caries and no pocket depths exceed 3 mm.
There is an area of exposed bone in the anterior mandibular alveolus and a socket from which a lower incisor has been lost, as shown in Figure 23.1. The adjacent teeth in the exposed bone are mobile in their sockets and are also in danger of spontaneous exfoliation.
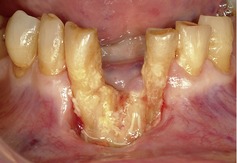 |
| Fig. 23.1 |
The attached gingiva in the region is missing and the buccal soft-tissue margin of the lesion is lax and can be lifted to allow a dental probe to be inserted down almost to the patient’s chin. No pus is present.
▪ How do you interpret the findings so far?
The lack of bleeding and sensitivity suggest that the bone is necrotic and the teeth non-vital. Despite bacterial plaque and debris accumulating on the exposed bone there seems to be no infection, even though there is a deep soft-tissue pocket extending to the chin. The surrounding mucosa is hardly inflamed, suggesting that local trauma and infection are not responsible.
The appearances are very characteristic and it is possible to make a fairly confident diagnosis without any further investigations.
Diagnosis
▪ What is your diagnosis?
Bisphosphonate-related osteonecrosis is almost certainly the diagnosis on the basis of asymptomatic necrosis of bone without pain. The patient has taken alendronate, a bisphosphonate drug, for several years and this is a recognized complication.
▪ What alternative diagnoses have you excluded and why?
Chronic osteomyelitis would seem a possibility but the presentation is not correct for this diagnosis. Relatively mild pain or discomfort would probably be present, as would bad taste, discharge of pus indicating infection and possibly sequestration of the nonvital bone. There would also normally be both a cause and a predisposing factor. If dental infection were the cause, it would be evident clinically or radiographically, or there might be a history of trauma such as a fracture or dental extraction. Patients who develop osteomyelitis usually have some systemic predisposing condition such as diabetes mellitus or immunosuppression. It seems that this option is most unlikely, though a radiograph would help exclude or confirm it.
Acute osteomyelitis is even less likely. Acute infection would be accompanied by the cardinal signs of inflammation – pain, erythema and swelling. There is a severe, deep boring pain in acute osteomyelitis with systemic signs of infection.
Necrotizing periodontitis could cause necrosis of soft tissue with exposed bone but would be associated with other signs and symptoms. It is almost exclusively found in severe immunosuppression, usually late or untreated human immunodeficiency virus (HIV) infection. Necrotizing periodontitis is usually painful and limited to the gingiva and alveolar margin. It would not cause extensive soft-tissue separation from bone as here.
Cancrum oris (noma) is a necrotizing mixed bacterial infection sometimes developing from acute ulcerative gingivitis. It causes tissue necrosis of large parts of the face or other tissues, including bone. The disease is almost confined to malnourished and debilitated children below the age of 8 years in developing countries.
▪ What is the difference between osteomyelitis, osteitis and osteonecrosis?
Osteomyelitis is an infection in the medullary cavity of the bone. It is usually bacterial. The resulting increased pressure in the medullary space and the inflammatory reaction devitalize the marrow by compressing its blood supply and parts of the bone undergo necrosis. After an acute and intensely painful phase, pus drains and osteoclasts separate the necrotic bone to form sequestra. If the sequestra can be shed, the bone may heal. If not, infection persists in the sequestrum and is difficult to treat, the disease becomes chronic and the surrounding bone becomes sclerotic.
Osteitis is a superficial inflammation of bone, such as is seen in the exposed bone of dry socket (see problem 15). Small sequestra may form but infection does not penetrate into or spread within the medullary cavity.
Osteonecrosis is death of bone. The causes are usually loss of blood supply, vascular or bisphosphonate drugs. The dead bone is sterile, at least initially, and only becomes colonized by bacteria once exposed to the exterior. Osteonecrosis can follow irradiation of bone because this induces endarteritis, narrowing of the blood vessels with eventual necrosis. Osteonecrosis is increasingly recognized in patients taking bisphosphonate drugs for prevention or treatment of osteoporosis, management of bone metastasis in cancer or for metabolic bone diseases.
▪ What are bisphosphonate drugs and why are they used?
Bisphosphonate drugs reduce bone turnover. The drugs are adsorbed on to bone surfaces where they remain bound for a prolonged period. They are taken up by osteoclasts at sites of bone resorption, and interfere with adenosine triphosphate (ATP) metabolism or membrane function. Osteoclasts either die or become unable to resorb bone. Bone formation then exceeds bone resorption, remodelling is slowed and bone density increases or stabilizes.
The drugs have a variety of uses:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


