Case• 16. A numb lip
SUMMARY
A 68-year-old man presents to you in general dental practice complaining that his lower lip has become numb. How would you investigate and manage this symptom?
History
Complaint
He complains of sudden onset of numbness of the lower right lip. It feels cold, as if he had had an injection for dental treatment (Figure 16.1).
 |
| Fig. 16.1 |
History of complaint
The patient noticed the numbness immediately he woke up the previous morning. His jaw has been aching for some months and he has noticed some tingling in the lip, which he ascribes to recent dental treatment.
Dental history
You are seeing the patient for an emergency appointment. He is normally under the care of one of your colleagues and his records and radiographs are available.
A series of appointments over the last few months have addressed pain from the lower right quadrant. The tingling in the lip was noted 3 months ago. The lower right first molar had been considered to be the cause. Your colleague placed a root filling 4 months ago but the pain did not resolve completely. Three weeks ago the lower right second premolar was extracted as a likely cause of the pain. However, discomfort continued.
Medical history
The patient reports that he is fit and well. He takes 50 mg atenolol daily for mild hypertension. In the past he has suffered depression and was treated with antidepressants in the past.
▪ What is the sensory nerve supply to the lip?
The sensory nerve supply to the face is shown in Figure 16.2. The three divisions of the trigeminal nerve supply most of the face. The greater auricular nerve is formed by the ventral rami of the cervical nerves C2 and C3.
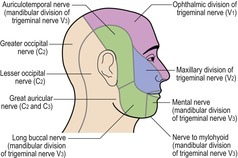 |
| Fig. 16.2 |
The lower lip is supplied by the mental nerve.
▪ What is the course of the nerve supply?
The trigeminal nerve starts in the pons where its sensory and motor roots arise. The ophthalmic and maxillary branches leave the skull via the superior orbital fissure and the foramen rotundum respectively. The mandibular branch leaves the skull at the foramen ovale to enter the infratemporal fossa, where it divides into an anterior group of mostly motor branches and a posterior group of sensory branches.
The anterior group of branches includes the nerves to lateral pterygoid, deep temporal nerves to masseter and the sensory long buccal nerve. There are three posterior branches, including the auriculotemporal nerve, which is given off almost immediately. This passes backwards to innervate the side of the scalp and part of the ear. The main nerve then divides into the lingual nerve, which passes to the tongue along the lateral pterygoid, and the inferior alveolar nerve, which gives off the small motor branch to mylohyoid and then enters the mandibular foramen in the mandibular ramus. It emerges from the mental foramen to provide sensation to the lip.
Unlike many other areas of sensory innervation, those on the face are well defined and sharply delineated. Though there is some slight variation between individuals, there is little overlap of the areas supplied by different nerves.
▪ What are the causes of numbness of the lip?
Numbness may be constant or temporary/intermittent, depending on the cause. The main causes are shown in Table 16.1 and each may affect the nerve at different parts along its course.
| Infection |
Osteomyelitis
Apical infection causing pressure on nerve in mandibular canal
|
| Tumour |
Primary malignant neoplasm of bone such as osteosarcoma, chondrosarcoma
Primary malignant neoplasm of mucosa invading bone such as oral squamous cell carcinoma
Primary malignant neoplasm of brain or tissues along path of nerve
Metastatic malignant neoplasm to brain or tissues along path of nerve
Benign tumour of brain such as meningioma or nerve schwannoma
|
| Trauma |
Mandibular fracture
Direct trauma to nerve at mental foramen
|
| Autoimmune |
Peripheral neuropathy
Multiple sclerosis
|
| Vascular | Vascular compression of nerve root |
| Psychological | Tetany from hyperventilation |
| Metabolic | Tetany from alkalosis |
| Iatrogenic causes |
Intraneural injection of local anaesthetic
Direct trauma to the inferior dental nerve at the lingula or mental foramen from dental injection
Trauma to the inferior dental bundle from dental extraction (particularly third molars), apicectomy or implant placement
Injury to the mental nerve during surgical extractions/apicectomy
Injury to the inferior alveolar nerve by extruded root filling material or caustic endodontic agents
|
Examination
Extraoral examination
The appearance of the patient is shown in Figure 16.1. He appears normal; the lip is of normal colour and shows no distortion or drooping to suggest a motor nerve lesion.
When you examine him you find that there is only a very mild swelling of the posterior right lower jaw. There is no detectable mass, but the patient is tender in the right submandibular area. There is normal movement of the lip.
▪ How will you test for sensation? Why is this necessary?
A sensation of numbness may be central in origin, denote damage to the peripheral nerve or be psychosomatic. Only by testing sensation can the exact area affected be defined and this will help define the cause.
Tests of sensation may include light touch (with a wisp of cotton wool or a Von Frey hair – fine filaments of calibrated rigidity for testing touch), pain (with a sharp and blunt point), vibration, temperature and two-point discrimination. A cotton wool fibre and a sharp point such as a hypodermic needle are usually sufficient for a dental setting. Outline the area affected, making sure that hand movements cannot be seen by the patient so that the results are objective. Test and retest if the results are unclear.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


