Introduction
Our objective was to evaluate the efficacy of a fluoridated varnish in preventing white spot lesions in patients with fixed appliances. A laser-induced fluorescence device was used to determine any correlations between the degree of demineralization and the length of the observation period, the arch sector, the frequency of varnish application, and the specific tooth site.
Methods
A split-mouth study design was used for 24 orthodontic patients, allocated randomly to 2 subgroups with differing frequencies of Duraphat varnish (Colgate-Palmolive, New York, NY) application. Repeated measures of the degree of demineralization were taken on the vestibular surfaces of 12 teeth (6 varnished and 6 unvarnished controls). Measurements were taken at 4 sites using a DIAGNOdent Pen 2190 laser (KaVo, Biberach an der Riss, Germany) and then subjected to statistical analysis.
Results
Generalized linear model and coefficient model analysis showed differences in the degrees of demineralization between treated and untreated teeth, but this was not statistically significant in terms of time point, frequency of application, or specific tooth site. However, when we analyzed the position of the teeth, the varnished anterior teeth showed a statistically significant reduction in demineralization compared with their unvarnished counterparts.
Conclusions
Periodic application of fluoride varnish can offer some protection against white spots, but not to a statistically significant degree if the patients have excellent oral hygiene.
Highlights
- •
Fluoridated varnish can help prevent caries lesions during orthodontic treatment.
- •
The frequency of application does not change the trend of protection against caries.
- •
The results were not significant in patients with excellent oral hygiene.
Enamel demineralization in the form of white spot lesions is a serious complication of orthodontic treatment. White spot lesions are essentially areas of porous surface enamel induced by carious demineralization and are milky-white opaque spots on the smooth surface of the tooth. White spots are more prevalent in patients with fixed appliances than in those without brackets. Although they rarely progress to caries, they are unsightly and can cause esthetic issues even years after treatment.
The prevalence of white spots in orthodontic treatment has been reported to be 38% after 6 months and 46% after 12 months, compared with 11% in the control group. The increased risk of developing white spot lesions during orthodontic treatment is due to an overaccumulation of plaque around the brackets ; this is partially attributable to patients’ inability or failure to maintain adequate oral hygiene.
Patients, parents, orthodontists, and general dentists all have similar perceptions of white spots and believe that patients are mainly to blame for their onset. White spots can be reduced or prevented by improving oral hygiene, lowering dietary carbohydrate intake, and applying topical fluoride. The safety of fluoride use has been amply demonstrated, and various means of topical application have been proposed, including gels, mouthwashes, and varnishes, but many strategies require high patient compliance to be efficacious.
One method of topical fluoride application that does not rely heavily on patient compliance is fluoride varnish, which is particularly appealing for noncompliant patients and those who are not self-reliant. Studies analyzing the efficacy of 1 brand, Duraphat (Colgate-Palmolive, New York, NY), on the tooth surfaces adjacent to labial brackets have shown that it can lower the risk of decalcification at these sites by 48% to 50%. However, much of the research to date has been conducted on extracted teeth or over limited periods in vivo, generally ranging from 1 to 3 months.
Nevertheless, a totally in-vivo study with a longer follow-up of 6 months by Demito et al showed a similar and significant reduction (50%) in white spots, but the varnish could not eliminate this risk completely. The authors concluded that the varnish should be reapplied every 12 weeks.
The purpose our study was to evaluate in vivo the efficacy of Duraphat in preventing white spot onset over a longer period, 12 months, in patients with fixed appliances (maxillary and mandibular braces) with the aid of laser fluorescence. In particular, we aimed to determine whether the degree of demineralization varies by (1) the length of treatment (T0-T4, 12 months), (2) the location of the tooth (anterior, medial, and posterior) at 4 time points (3, 6, 9, and 12 months), (3) the frequency of Duraphat application (3 or 6 months), and (4) the specific tooth site (gingival, occlusal, mesial, and distal).
Material and methods
Twenty-four consecutive patients, all scheduled for fixed orthodontic treatment at a private dental clinic, were selected for this study. The sample consisted of 10 boys and 14 girls with a mean age of 14 years 1 month. The inclusion criteria were as follows: complete permanent dentition up to the first molars, no vestibular caries or fillings, no hypocalcified teeth, no dental fluorosis, and no endocrine disorders (eg, diabetes).
A split-mouth study was conducted, applying the varnish to quadrants 1 and 3, with quadrants 2 and 4 as the untreated controls. Opposing quadrants were chosen to eliminate any bias resulting from handedness, which can affect the uniformity of brushing accuracy. The 6 varnished and the 6 control teeth were the central incisors, the canines, and the second premolars: ie, teeth from each of the maxillary and mandibular anterior, medial, and posterior sectors.
The patients were randomly assigned to 2 subgroups according to the frequency of Duraphat application: group 1, comprising 13 patients (5 boys, 8 girls), in whom Duraphat was applied every 3 months; and group 2, comprising 11 patients (5 boys, 6 girls), in whom Duraphat was applied every 6 months. Four to 7 days before bonding, both groups were given a professional scale and polish and attended a hygiene motivation session. All patients received a hygiene kit that contained a medium-bristle toothbrush (G-U-M; Sunstar Americas, Chicago, Ill).
Before the trial all patients had a dental examination with caries control, periodontal evaluation, and plaque index. An oral hygiene session with motivation by the dental hygienist was conducted 7 days before the appliances were placed.
Before bonding, the 24 subjects’ teeth were cleaned with a pumice stone and a brush mounted on a low-velocity contra-angle handpiece, and the enamel mineralization of all sample and control teeth was measured with a DIAGNOdent Pen 2190 (KaVo, Biberach an der Riss, Germany).
The DIAGNOdent Pen 2190 contains a diode laser with a wavelength of 655 nm and power less than 1 mW. It can detect small alterations in the tooth substance, invisible to the naked eye, up to a depth of 2 mm. According to the literature, the DIAGNOdent has great specificity and accuracy, similar to visual-tactile examinations and radiography (identifying 70%-80% of lesions), compared with histology testing, if it is used on clean teeth (without tartar buildup) and without fluoridated substances. The DIAGNOdent Pen 2190 measures the fluorescence emitted by the tooth in response to irradiation of a certain wavelength; a reading between 0 and 13 indicates healthy enamel, between 14 and 20 suggests initial demineralization, between 21 and 29 means considerable demineralization, and greater than 30 indicates dental caries.
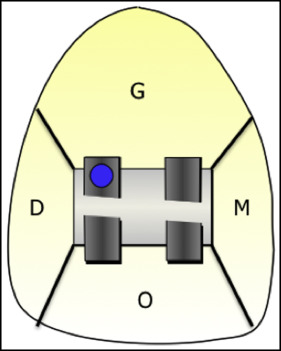
The laser was calibrated for each patient according to the manufacturer’s guidelines, and readings were taken at 4 labial sites on the enamel (gingival, occlusal, mesial, and distal) as suggested by Banks and Richmond ( Fig ). Initial values (T0) were recorded in the patients’ dental records.
After the initial readings, medical-grade steel brackets, self-ligating Damon Q (Ormco, Orange, Calif), were bonded to the teeth with a light-cured composite. The dental arcades were then isolated, and the vestibular surfaces were dried and treated. Duraphat (5% sodium fluoride) was applied to the vestibular enamel around the brackets of the maxillary right central incisor, canine, and second premolar and the mandibular left central incisor, canine, and second premolar using a microbrush. After about 5 minutes of hardening time, the patient was instructed on how to perform oral hygiene procedures and asked to refrain from eating or drinking for 4 hours, as the manufacturer recommends. All patients received a hygiene kit containing a manual orthodontic toothbrush, which was replaced every 3 months.
In follow-up visits, mineralization of the enamel was measured as follows: the vestibular surfaces of all teeth were cleaned using a brush mounted on a low-velocity contra-angle handpiece, and the residual varnish was removed with an air polishing system (TPC Advanced Technology, City of Industry, Calif) to prevent its being read as a false positive. The fluorescence emitted at the 4 sites, each 1 mm from the bracket, was measured on all sample and control teeth using the DIAGNOdent Pen 2190, and then the Duraphat varnish was reapplied, as per the manufacturer’s instructions, on the teeth in the first and third quadrants. Measurements were taken, and fluoride varnish was reapplied at 3, 6, 9, and 12 months after appliance fitting (T1, T2, T3, and T4, respectively) in group 1, and at 6 and 12 months after bonding (T2 and T4, respectively) in group 2. All patients were given a new hygiene kit (including a toothbrush) every 3 months, and a professional scale and polish every 6 months.
All measurements from the DIAGNOdent were recorded on an Excel spreadsheet (Microsoft, Redmond, Wash), and the significance of any differences was evaluated by the chi-square test at a significance level of P <0.01. A general linear model was used because the measurements had a non-Gaussian distribution. Coefficient plots were also generated to illustrate the significance of each value with respect to the reference (intercept).
During the study, every 6 months, all patients attended ab oral hygiene session and evaluation with the plaque index.
Results
The total number of measurements taken was 4704: 3120 in group 1 (Duraphat applications every 3 months) and 1584 in group 2 (Duraphat applications every 6 months). Table I shows the numbers of measurements and the mean values for the degrees of mineralization from T1 through T4 in treated and untreated teeth; Table II shows the mean readings from the 3 sectors (anterior, medial, and posterior) in treated and untreated teeth; and Table III shows the average readings in sites treated or not every 3 months and every 6 months.
| Time point | Observations (n) | Average | SD |
|---|---|---|---|
| T0 (pretreatment) | |||
| Treated teeth | 576 | 2.11 | 0.93 |
| Untreated teeth | 576 | 2.19 | 0.97 |
| T1 (3 mo) | |||
| Treated teeth | 312 | 2.48 | 0.97 |
| Untreated teeth | 312 | 2.80 | 1.30 |
| T2 (6 mo) | |||
| Treated teeth | 576 | 2.83 | 1.92 |
| Untreated teeth | 576 | 2.92 | 1.70 |
| T3 (9 mo) | |||
| Treated teeth | 312 | 2.79 | 1.20 |
| Untreated teeth | 312 | 3.19 | 1.76 |
| T4 (12 mo) | |||
| Treated teeth | 576 | 3.33 | 1.97 |
| Untreated teeth | 576 | 3.91 | 2.12 |
| Sector | Observations (n) | Average | SD |
|---|---|---|---|
| Anterior | |||
| Treated teeth | 784 | 2.28 | 1.28 |
| Untreated teeth | 784 | 2.76 | 1.80 |
| Middle | |||
| Treated teeth | 784 | 2.90 | 1.64 |
| Untreated teeth | 784 | 3.08 | 1.67 |
| Posterior | |||
| Treated teeth | 784 | 3.00 | 1.76 |
| Untreated teeth | 784 | 3.17 | 1.73 |
| Application frequency | Observations (n) | Average | SD |
|---|---|---|---|
| 3 months | |||
| Treated teeth | 1560 | 2.67 | 1.39 |
| Untreated teeth | 1560 | 2.94 | 1.65 |
| 6 months | |||
| Treated teeth | 792 | 2.83 | 1.96 |
| Untreated teeth | 792 | 3.12 | 1.91 |
Table IV shows a greater tendency toward demineralization in the untreated vs the treated teeth, although both linear and coefficient analyses showed that the difference was not significant at any of the 4 measurement times (3, 6, 9, and 12 months).
| Chi-square | df | P (+χ 2 ) | |
|---|---|---|---|
| Reference value | 138.63 | 1 | 0.0000 |
| Length of treatment | 90.51 | 4 | 0.0000 |
| Treated teeth | 0.18 | 1 | 0.6710 |
| Treated teeth/length of treatment | 3.49 | 4 | 0.4792 |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


