Antimicrobial chemotherapy
Publisher Summary
Antimicrobial agents include antibacterial, antiviral, antifungal and antiprotozoal agents. Apart from the last group, dental practitioners are frequently called upon to prescribe these drugs and therefore should be conversant with the mode of action, spectrum of activity, side-effects and contraindications of at least the major groups of antimicrobials. This chapter summarizes the principles of antimicrobial therapy together with notes about the nature and use of antimicrobials frequently prescribed in dentistry.All antimicrobials demonstrate selective toxicity, in that the drug can be administered to humans with reasonable safety while having a marked lethal or toxic effect on specific microbes. The corollary of this is that to some extent all antimicrobials have adverse effects on humans and should therefore be used rationally and only when required.
Bacteriostatic and bactericidal antimicrobial agents
Mode of action of antimicrobial agents
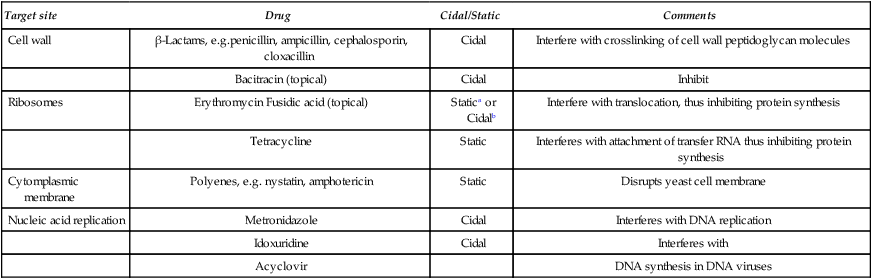
Antimicrobial agents inhibit the growth of or kill microorganisms by a variety of mechanisms. In general, however, one or more of the following four specific target sites are involved: (1) the cell wall, (2) the cytoplasmic membrane, (3) ribosomes, and (4) nucleic acid replication sites. The detailed modes of action of antimicrobials are outside the scope of this book and the reader is referred to texts in the reading list for this information. A summary of the mode of action of commonly used antimicrobials in dentistry is given in Table 14.1
Table 14.1
Mode of action of antimicrobials commonly used in denistry
| Target site | Drug | Cidal/Static | Comments |
| Cell wall | β-Lactams, e.g.penicillin, ampicillin, cephalosporin, cloxacillin | Cidal | Interfere with crosslinking of cell wall peptidoglycan molecules |
| Bacitracin (topical) | Cidal | Inhibit | |
| Ribosomes | Erythromycin Fusidic acid (topical) | Statica or Cidalb | Interfere with translocation, thus inhibiting protein synthesis |
| Tetracycline | Static | Interferes with attachment of transfer RNA thus inhibiting protein synthesis | |
| Cytomplasmic membrane | Polyenes, e.g. nystatin, amphotericin | Static | Disrupts yeast cell membrane |
| Nucleic acid replication | Metronidazole | Cidal | Interferes with DNA replication |
| Idoxuridine | Cidal | Interferes with | |
| Acyclovir | DNA synthesis in DNA viruses |
General principles of antimicrobial therapy
General indications
The choice of drug
The choice of drug is strictly dependent upon the nature of the infecting organism(s) and their sensitivity pattern(s). However, in a clinical emergency such as septicaemia or Ludwig’s angina, antimicrobial agents must be prescribed empirically until laboratory tests have been completed. In other conditions such as acute ulcerative gingivitis where a Gram-stained smear of the lesion is diagnostic, therapy with metronidazole should be instituted without further laboratory tests since it is extremely difficult to isolate and identify spirochaetes (see Chapter 5). In general another antimicrobial should be prescribed if the patient has had penicillin within the previous month. This is because of the natural selection and persistence of resistant bacterial populations when they are exposed to the drug.
Spectrum of activity of antimicrobial agents
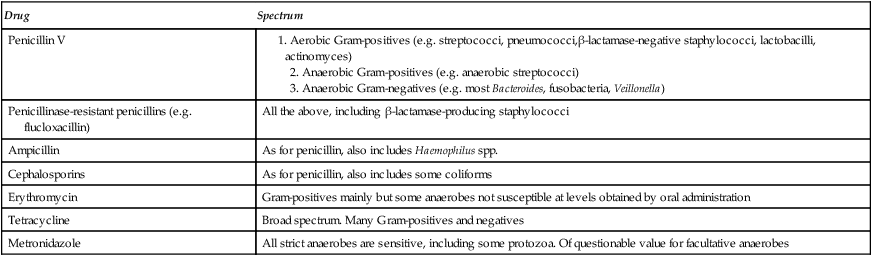
On the other hand, broad-spectrum antimicrobial agents are active against many Gram-positive and Gram-negative bacteria; examples include tetracyclines, ampicillins and cephalosporins. Hence the broad-spectrum agents are often used for the blind or empirical treatment of infections when the likely causative pathogen is unknown. This, unfortunately, leads to abuse of broad-spectrum agents with consequential emergence of resistant organisms which were originally sensitive to the drug. The spectra of activity of some broad- and narrow-spectrum antimicrobial agents used in dentistry are shown in Table 14.2.
Table 14.2
Antimicrobial prophylaxis
Prophylactic antimicrobial agents are definitely indicated during dental treatment involving patients with at risk status with respect to infective endocarditis (see Chapter 12), facial fractures or compound skull fractures, and cerebral rhinorrhoea. Oral surgery performed in immunocompromised patients, or in patients who have recently received radiotherapy to the jaws, may also require prophylaxis. In the former situation the patients are susceptible to infection due to generalized immunodeficiency while in the latter instance the jaws succumb to infection due to severe ischaemia of the bone consequential to radiotherapy.
Prescribing an antimicrobial agent
The following questions should be considered before any antimicrobial agent is prescribed.
Have relevant specimens been taken before treatment?
As explained in Chapter 13, appropriate specimens should be collected before drug therapy is started as the population of pathogens may be reduced, and therefore less easily isolated, if specimens are collected after antimicrobial agents have been taken. Further, the earlier the specimens are taken, the more chance that the results will be available to help with patient management.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


