Computer-controlled local anesthetic delivery (C-CLAD) devices and systems for intraosseous (IO) injection are important additions to the dental anesthesia armamentarium. C-CLAD using slow infusion rates can significantly reduce the discomfort of local anesthetic infusion, especially in palatal tissues, and facilitate palatal approaches to pulpal nerve block that find special use in cosmetic dentistry, periodontal therapy, and pediatric dentistry. Anesthesia of single teeth can be obtained using either C-CLAD intraligamentary injections or IO injections. Supplementary IO anesthesia is particularly suited for providing effective pain control of teeth diagnosed with irreversible pulpitis.
Effective local anesthesia is arguably the single most important pillar upon which modern dentistry stands. Paradoxically, the injection of local anesthetic is also perhaps the greatest source of patient fear, and inability to obtain adequate pain control with minimal discomfort remains a significant concern of dental practitioners. Although the traditional aspirating syringe is the most common method by which local anesthetics are administered, newer technologies have been developed that can assist the dentist in providing enhanced pain relief with reduced injection pain and fewer adverse effects. This discussion will focus on the clinical uses of computer-controlled local anesthesia delivery (C-CLAD) devices and intraosseous (IO) systems for local anesthetic injection.
C-CLAD systems
Available Devices
Milestone Scientific (Piscataway, NJ, USA) introduced the first C-CLAD system in the United States in 1997. Originally known as the Wand, subsequent versions were sequentially renamed the Wand Plus and then CompuDent, the current designation. In 2001, the Comfort Control Syringe (Dentsply International, York, PA, USA) was marketed as an alternative to the Wand. Examples of similar products originating and available outside of the United States include the QuickSleeper and SleeperOne devices (Dental Hi Tec, Cholet, France) and the Anaeject (Nippon Shika Yakuhin, Shimonoseki, Japan) and Ora Star (Showa Uyakuhin Kako, Tokyo, Japan) syringes.
Milestone Scientific Products
The CompuDent system has three components: a base unit, a foot pedal, and a disposable handpiece assembly. The base unit contains a microprocessor and connects to both the foot pedal and the end of the handpiece assembly that accepts the local anesthetic cartridge. The microprocessor controls a piston that expresses local anesthetic by pushing the local anesthetic plunger up into the cartridge. The anesthetic solution is then forced through the microbore tubing, Wand handpiece, and attached needle into the tissue. Pressing lightly on the foot pedal activates a slow injection rate (0.005 mL/s) appropriate for needle insertion, periodontal ligament (PDL) injection, and palatal administration. Heavier pressure on the pedal increases injection speed to deliver the entire content of the cartridge in 1 minute (ie, 0.03 mL/s), which is normally used for buccal infiltrations and nerve blocks. In 2005, a third, higher rate (0.06 mL/s) was added in response to practitioner requests. Release of the foot pedal stops injection, and if the aspiration feature is enabled, causes an aspiration cycle in which the piston retracts, drawing blood into the tubing if the needle tip is located intravascularly. The CompuDent system costs approximately $1500; each disposable Wand assembly is $2 to $3 per set.
In 2007, Milestone Scientific added the STA (Single Tooth Anesthesia) system to its product line ( Fig. 1 ). The STA unit adds dynamic pressure sensing (DPS) technology, which provides continuous feedback to the user about pressure at the needle tip to help identify ideal needle placement for PDL injections. In this STA mode there is a single, slow rate of injection. Selecting the normal mode emulates the original CompuDent device. A third mode, called turbo, adds the third, faster rate of injection (0.06 mL/s). The cost for the STA system is approximately $2000.
Comfort Control Syringe
The Comfort Control Syringe differs from the Milestone products in that there is no foot pedal. It has two main components: a base unit and a syringe. Several functions of the unit—most importantly injection and aspiration—can be controlled directly from the syringe, possibly making its use easier to master for practitioners accustomed to the traditional manual syringe.
The Comfort Control Syringe ($1200, $1 per cartridge sleeve) has five different basic injection rate settings designed for specific injections: block, infiltration, PDL, IO, and palatal. Each rate is selected by the push of a button. The unit uses a two-stage delivery rate for every injection. It initially expresses the anesthetic solution at an extremely low rate. After 10 seconds, the rate slowly increases to the preprogrammed value for the selected injection. The basic speed of each injection also can be doubled by pushing a button on the syringe or the base unit. Although use of the Comfort Control Syringe may be more intuitive than that of the Milestone devices in the sense that the injection is controlled by hand, the syringe is bulky and more cumbersome to use than the Wand handpiece. A comparison between the traditional dental syringe and the Comfort Control Syringe revealed no meaningful differences in ease of administration, injection pain and efficacy, and acceptance by patients.
Potential advantages
Several potential advantages have been ascribed to C-CLAD systems in general and to the Milestone products in particular. These include more accurate needle insertion for deeper nerve blocks, less pain on injection, and less fear of injection.
Because the Wand handpiece is approximately the same size as a ballpoint pen, it is easily held in a pen grasp, which facilitates fine motor control and often allows the fingers to be significantly closer to the needle tip than is the case with the traditional dental syringe. The net result is a more controlled insertion of the needle. Furthermore, the ability to rotate the handpiece back and forth during needle insertion may reduce the needle deflection that occurs in response to the straight insertion of a dental needle whose needle tip is not coincident with the central axis of the shaft. At this time, there is no compelling evidence that these potential advantages in needle placement actually foster increased anesthetic efficacy.
Three features of C-CLAD support the assertion that there may be less pain on injection. First, the ability to administer small amounts of local anesthetic continuously during needle insertion helps to anesthetize tissues immediately ahead of the advancing needle. Second, the steady infusion of anesthetic solution once the needle has reached its target may reduce discomfort associated with less controlled injections. Third, the reduced force required for needle insertion using the bidirectional rotation Wand technique may translate into improved comfort. Various investigators have reported no difference in injection pain, whereas others have found significantly reduced pain with the Milestone products. Numerous differences in study design and the inherent inability to perform double-blind comparisons complicate interpretation of these results. The authors nevertheless conclude the following
-
With the important exception of palatal injections, C-CLAD does not materially reduce the discomfort of needle insertion
-
Most reductions in injection pain can be attributed to the significantly reduced rates of local anesthetic i nfusion used in studies reporting beneficial effects of C-CLAD on injection pain.
In support of the latter inference is the study by Kudo, which documented a direct relationship between initial injection pressure and subsequent patient reports of pain and anxiety.
Reduced fear of injection would be an expected outcome of decreased pain. The relatively unthreatening appearance of the Wand handpiece also may help alleviate anxiety. Experimental support for lower apprehension with C-CLAD is limited, however. Although Krochak and Friedman noted decreased anxiety in subjects given Wand injections compared with traditional methods, Versloot and colleagues found that this potential benefit of C-CLAD was lost in highly anxious children, perhaps because their fear of treatment overwhelmed any technique-sensitive differences in nociception.
Alternative injections
The ability of C-CLAD devices to administer local anesthetics at a slow, controlled rate has been used to advantage with respect to three injections: the anterior middle superior alveolar (AMSA), the palatal approach to the anterior superior alveolar (P-ASA), and the PDL.
The AMSA injection, described in 1998 by Friedman and Hochman, is intended to provide pulpal anesthesia of the ipsilateral incisor, canine, and premolar teeth and their associated palatal soft tissues. Using a C-CLAD device, a 30-gauge ultrashort needle is placed along the line bisecting the premolar teeth at the point halfway between the midpalatine suture and the free gingival margin. With the assistance of pressure anesthesia from a cotton-tipped applicator, the bevel of the needle is placed against the palatal tissue, and the slow flow of anesthetic is started. After approximately 8 seconds, the needle is slipped beneath the palatal mucosa with a gentle twisting motion and then advanced laterally and superiorly very slowly (0.25 mm/s) until bone is gently contacted. Generally, and after a negative aspiration, the entire contents of the local anesthetic cartridge are administered over a 4-minute period.
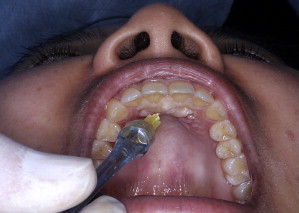
The P-ASA injection ( Fig. 2 ), also described by Friedman and Hochman, was designed to anesthetize the six maxillary anterior maxillary teeth with a single injection. Anesthetized soft tissues include those overlying the anterior palate (nasopalatine nerve distribution) and, to a lesser extent, the labial gingiva. The technique of needle penetration is similar to that described for the AMSA injection except that the needle is placed initially just lateral to the incisive papilla. Once the needle has penetrated the mucosa, 5 to 6 seconds should elapse before the needle is reoriented more vertically to enter the nasopalatine canal. After a very slow (0.25 mm/s) insertion of 0.5 to 1 cm—at which point the bony wall of the canal should be felt and a negative aspiration obtained—the rest of the cartridge is deposited in about 4 minutes.
The PDL injection using a C-CLAD device is similar in technique to that using a traditional syringe or dedicated periodontal ligament syringe. The infusion of anesthetic, however, is quite different. Much larger volumes (up to 0.9 mL for a single-rooted tooth or 1.8 mL for a multirooted tooth) are injected much more slowly (eg, 0.005 mL/s). The STA device by Milestone, with its ability to monitor fluid pressure at the needle tip, helps to ensure that both leakage of anesthetic and overpressure are avoided during the PDL injection.
These three injections using C-CLAD share certain attributes. They all tend to limit anesthesia of the cheek and lip and preserve motor control, an important criterion for cosmetic dentistry. They also provide useful alternative injection techniques when primary methods (eg, maxillary supraperiosteal injection and inferior alveolar nerve block) are contraindicated or ineffective. Whether they should be used routinely as primary techniques is less clear.
At least in adults, these injections can produce moderate levels of pain during needle insertion (AMSA, P-ASA) or after the procedure (PDL). To minimize local tissue irritation, a rate of injection comparable with the lowest rate of the CompuDent device should be used. Presumably because of anecdotal reports, Milestone Scientific recommends that reduced volumes of anesthetic be administered if 4% anesthetic solutions are used and that formulation alternatives with higher concentrations of epinephrine (ie, 2% lidocaine with 1:50,000 epinephrine or 4% articaine with 1:100,000 epinephrine) be avoided. Perhaps the biggest concern regarding the routine reliance on the AMSA and P-ASA injections is the potential for incomplete anesthesia. Electric pulp testing studies have shown that the extent of anesthesia is often less than was originally proposed for the techniques, and sometimes the depth of anesthesia is less than that produced with supraperiosteal injections. Interestingly, recent studies also have shown that the extent of anesthesia achieved with traditional maxillary and infraorbital nerve blocks is also significantly less than previously thought.
One use in which the palatal injections shine is in periodontal therapy of the maxilla. A single AMSA injection, for example, may produce sufficient pain control to treat the entire hemimaxilla. This approach avoids the need for multiple injections and can result in significantly less local anesthetic being administered. Likewise, PDL injections using C-CLAD devices, especially the STA system, are highly effective for short-duration single-tooth anesthesia and compare favorably with alternative PDL methods.
Pediatric use
Special mention should be made regarding the use of C-CLAD devices in pediatric dentistry. Although several studies found no benefit when the Wand was used essentially to replace the traditional syringe, Palm and colleagues recorded a reduction in pain with the inferior alveolar nerve block. Possible differences in injection rates used for the C-CLAD and traditional syringe may have contributed to this finding. Of greater significance are the investigations that have focused on the use of palatal injections for pulpal anesthesia. Most, but not all, of these studies have found that the AMSA and P-ASA injections administered by C-CLAD devices may be better tolerated or produce less disruptive behavior than supraperiosteal injections delivered with traditional syringes, especially when supplemental palatal infiltrations have to be performed. There is also general agreement that the palatal C-CLAD injections produce comparable efficacy to traditional alternatives, even for pulpotomies and extractions. Finally, two reports comparing PDL injections with the Wand to conventional anesthesia (buccal infiltration and inferior alveolar nerve block with a standard aspirating syringe) found the PDL injection to be accepted more positively. Although anesthetic efficacy was the same in young children (2 to 4 years) receiving dental treatment in the upper anterior maxilla, the PDL injection was less effective than mandibular blockade in relieving pain during treatment for children aged 6 to 10 years. Nevertheless, patients still preferred the Wand by a 2 to 1 margin.
IO local anesthesia
Although IO-induced local anesthesia has been used in clinical dentistry for over a century, the original technique was too invasive for widespread adoption, requiring a gingival flap to be raised to gain access to the buccal cortical bone for perforation with a small round bur. IO anesthesia became even less important with the discovery and marketing of lidocaine in the 1940s. Nevertheless, in 1975 Lilienthal described a technique in which a handpiece-driven root canal reamer was used to perforate the cortical plate. This use of a motor-driven perforator to penetrate the buccal gingiva and bone may be considered the first modern technique of IO anesthesia and the foundation upon which all current methods are based.
Available Devices
Several systems have been developed to achieve IO anesthesia. Although significant differences exist among them, they all aim to inject local anesthetic solution into the cancellous bone adjacent to the apex of the tooth. Three systems are available in the United States: Stabident (Fairfax Dental, Miami, Florida), X-tip (X-tip Technologies, Lakewood, NJ, USA), and IntraFlow (Pro-Dex Incorporated, Santa Ana, CA, USA).
Stabident
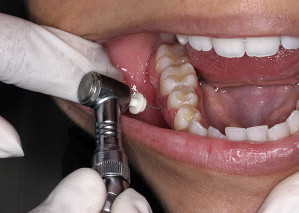
The Stabident system for IO anesthesia includes a solid 27-gauge perforator needle with a simple beveled tip and a plastic base designed to fit in a latch-type slow-speed contra-angle hand piece ( Fig. 3 ). The operator uses the perforator to create a small tunnel through the attached gingiva, periosteum, and alveolar bone. The typical insertion point is on the attached gingiva, 2 mm below the facial gingival margin, and midway between the tooth of interest and an immediately adjacent (preferably distal) tooth. Local anesthesia should be administered to anesthetize the local gingival tissue if it is not already numb from a previous injection. The angle of perforation is not critical but is usually adjusted in the mandibular incisor region (where the mesiodistal width is quite narrow) so that perforator travels in an apical direction. A more perpendicular angle is advantageous in the mandibular molar region to help avoid bending the perforator against the dense cortical bone. Penetration is made using short bursts with light pressure. A 27-gauge ultrashort (8 mm) needle is then inserted through the hole to deposit anesthetic solution into the cancellous bone. Up to an entire cartridge can be administered; a slow initial rate of injection is critical to patient comfort. The component cost per injection is about $1.
X-tip
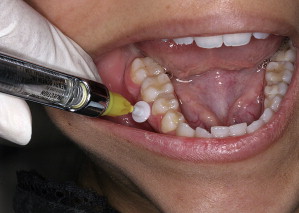
The X-tip Anesthesia Delivery System was designed to solve the primary technical difficulty encountered with the Stabident system—finding the hole and inserting the needle. The X-tip system comprises three parts ($3 per set): the drill (perforator), a 25-gauge guide sleeve that fits over the 27-gauge drill, and an ultrashort needle of the same diameter. The drill leads the guide sleeve through the cortical plate into the cancellous bone. The drill portion is then removed, leaving the guide sleeve in place. The guide sleeve is then used to direct the needle into the cancellous bone to deposit the anesthetic solution ( Fig. 4 ). The primary differences in using the X-tip device are
-
The penetration need not be performed through the attached gingiva
-
The guide sleeve must be carefully removed with a hemostat after the injection is performed.

Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


