Fig. 7.1
Scanning electron micrographs of apical root dentin. In (a) the endodontic-treated root dentin was prepared with a carbide bur and conditioned with 37 % phosphoric acid. There are approximately 50 % of the dentinal tubules still obliterated with smear layer debris preventing effective bonding. In (b) the endodontic-treated root dentin was also prepared with a carbide bur. Then the root dentin was roughened with a diamond bur followed by etching with 37 % phosphoric acid. There are very few dentin tubules obliterated showing the smear layer produced by the diamond bur yielding a more receptive substrate for acid conditioning (Gomes et al. 2012)
7.3 Chemical Preparation During Endodontic Treatment
The most frequent failure mode of fiber post retained restorations is post debonding (Weston et al. 2007; Cagidiaco et al. 2008; Dietschi et al. 2008). Considering that posts are passively retained into the root canal, the effectiveness of the adhesive bonding plays a relevant role in the overall clinical performance of the restorations. This highlights the importance of knowing the confounding factors that may preclude a strong adhesion between the adhesive cement and the root canal dentin. Some of the irrigants used during endodontic treatment may have a negative impact on root dentin bonding.
7.3.1 Sodium Hypochlorite and Other Oxidizing Solutions
Some solutions routinely used for endodontic irrigation have been reported to play a negative role on the bond strengths of adhesive materials to root canal dentin. NaOCl is an ideal endodontic irrigant widely used in endodontic treatments; however, it may inhibit the polymerization of resin-based materials due to its strong oxidizing property. NaOCl leaves a dentin surface characterized by an oxygen-rich layer that can significantly reduce bond strength (Nikaido et al. 1999; Saleh and Ettman 1999; Perdigao et al. 2000; Morris et al. 2001; Ari et al. 2003; Erdemir et al. 2004; Ozturk and Ozer 2004; Marques et al. 2014).
Not surprisingly, other oxidizing materials that are applied to dentin during endodontic procedures such as RC-prep, which is a urea peroxide-based product, leave behind an oxygen-rich surface that also inhibits bonding (Nikaido et al. 1999; Morris et al. 2001; Erdemir et al. 2004). This reduction in bond strength can be reversed by the application of either 10 % ascorbic acid or 10 % sodium ascorbate for at least 1 min (Morris et al. 2001; Weston et al. 2007).
The negative impact of NaOCl on bonding is also evident when resin-based endodontic sealers are used (Rocha et al. 2012; Vilanova et al. 2012) for obturation of the instrumented root canals. Reduced bond strengths were observed between the resin-based sealers and the root canals when sodium hypochlorite was used as an irrigant solution.
7.3.2 EDTA
The combination of EDTA and NaOCl is commonly used for endodontic irrigation to achieve demineralization and deproteinization. However, the use of EDTA for longer than 1 min in conjunction with NaOCl creates an erosive dentin surface because of excessive demineralization (Calt and Serper 2002), which makes it difficult to create a strong adhesive interface with a dentin bonding system, especially when using self-etch adhesives (Hayashi et al. 2005). Therefore, from a clinical perspective, prolonged endodontic irrigation with EDTA should be avoided.
7.3.3 Chlorhexidine Digluconate
Chlorhexidine gluconate is an adjunct irrigant during endodontic treatment due to its bactericidal effect. This solution does not jeopardize the bonding of resins to the root dentin (Erdemir et al. 2004), which is advantageous for resin bonding to the root canals. However, as it does not fulfill all the requisites of an endodontic irrigation solution, it cannot replace NaOCl and EDTA solutions. Additionally, as described in the next chapter, chlorhexidine may produce adhesive interfaces less prone to degradation when applied on demineralized dentin before adhesive application (Cecchin et al. 2011, 2014; Martinho et al. 2015).
7.3.4 Calcium Hydroxide
Calcium hydroxide (CaOH2) paste is sometimes used as medication in the root canal for its antimicrobial properties between endodontic sessions. It has been reported that CaOH2 might interfere with bonding of luting cements by acting as a physical barrier (Lee et al. 2014). This can be attributed to the fact that its complete removal is hardly accomplished (Lambrianidis et al. 1999; Maalouf et al. 2013). As reported by Breschi et al. (2009), CaOH2 may also neutralize the self-etching/primer solutions of self-etch adhesives due to its high pH; however, this issue warrants further investigation.
7.3.5 Endodontic Sealers
Although this topic has raised some controversy among different authors, some investigators have reported that the type of endodontic sealer may influence the adhesion between fiber posts and root dentin. It has been demonstrated that post retention is lower in filled canals when compared with non-filled canals, regardless of the type of endodontic sealer (Hagge et al. 2002). This fact highlights the importance of using a root canal sealer when performing in vitro studies to evaluate the bond strength of fiber posts to root dentin.
Some authors observed a loss of retention when eugenol-based sealers were used before post luting with resin cements (Tjan and Nemetz 1992; Burns et al. 2000; Alfredo et al. 2006; Aleisa et al. 2012; AlEisa et al. 2013). As other phenolic compounds, eugenol is a radical scavenger that inhibits the polymerization of resin-based materials. However, other studies found no significant difference when comparing eugenol- and non-eugenol-containing root canal sealers in terms of post retention when using resin cements (Mannocci et al. 2001; Hagge et al. 2002; Kurtz et al. 2003; Davis and O’Connell 2007).
This controversy from different studies may be attributed to the time elapsed between endodontic obturation and fiber post cementation. For instance, Menezes et al. (2008) evaluated the bond strength of fiber posts to root dentin when post cementation was performed immediately or after 7 days. When the authors used an eugenol-based sealer, the bond strengths were lower when post cementation was performed immediately relative to the bond strength when post cementation was performed after 7 days. Another possible explanation is the amount of dentin removed during the preparation of the post space. The removal of more eugenol-contaminated dentin from root canals treated with eugenol-containing sealer for placing larger diameter posts may increase the post retention (Izadi et al. 2013).
Better retention of fiber post is achieved when resin-based sealers are used compared with fiber posts cemented on root canals previously obturated with eugenol-containing endodontic sealers. The similar chemistry of luting cements and resin sealers and the lack of contamination with eugenol are responsible for this improved bonding (Aleisa et al. 2012; AlEisa et al. 2013).
The clinical indication emerging from several laboratory studies is to refrain from luting the post immediately after root canal obturation. Additionally, the diameter post space should be slightly enlarged. This latter approach, however, may have to be carefully evaluated by the clinician to avoid decrease in fracture resistance of the tooth and root perforations.
Studies have also shown that 3-step ER adhesives result in improved bonding to eugenol-contaminated dentin surfaces as acid etching can remove a great amount of the eugenol-contaminated smear layer (Peutzfeldt and Asmussen 1999; Wolanek et al. 2001). Self-etch adhesive systems should be avoided as they incorporate the eugenol-rich smear layer into the hybrid layer rather than removing it.
7.4 Incompatibility Between Adhesives and Cements
Currently different types of adhesive systems are available. In addition to the full versions of etch-and-rinse [ER] (3-step ER) and self-etch systems [SE] (2-step SE), simplified versions (2-step ER and 1-step SE) are available, which are very popular among clinicians due to their user-friendliness.
However, studies have shown that there is an incompatibility between simplified adhesives (i.e., 2-step ER and 1-step SE adhesives) and chemical- and dual-cured composite resin-based materials (Sanares et al. 2001; Cheong et al. 2003; Tay et al. 2003a, 2004a, b). This is not observed for the full versions of ER (Cheong et al. 2003; Tay et al. 2003b) and SE adhesives (Tay et al. 2002), which is likely due to the presence of an extra hydrophobic resin layer. This incompatibility can be attributed to the acidity of the adhesives (chemical incompatibility) (Sanares et al. 2001; Suh et al. 2003) or to the high water permeability of the adhesive layer produced by simplified adhesives, which pull water from the underlying dentin and precludes the close contact of the adhesive and the composite resin (physical incompatibility) (Tay et al. 2003a) (Fig. 7.2).
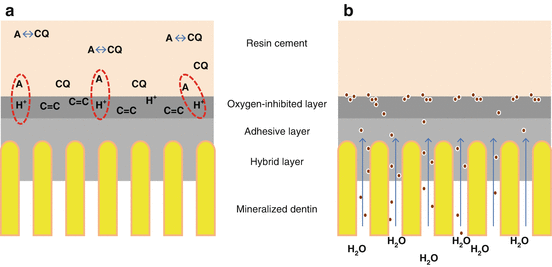

Fig. 7.2
Schematic illustration showing the chemical (a) and the physical incompatibilities (b) between acidic adhesives and resin cements. In (a) the protons (H) from acid monomers within the oxygen-inhibited layer compete with camphorquinone (CQ) for chemical interaction with the tertiary amines (A). This reduces the amount of free radicals to initiate the polymerization reaction. In (b), depiction of the easy passage of water from the underlying dentin through the permeable adhesive layer. This water accumulates at the adhesive interface, precluding a tight interfacial bonding with the resin cement
In the chemical incompatibility, an adverse chemical interaction between suboptimally polymerized acidic resin monomers from the oxygen-inhibited layer and the basic tertiary amine catalyst in the chemical or dual-cure composite was thought to be responsible for the observed incompatibility (Sanares et al. 2001). Although this phenomenon was firstly described for chemically and dual-cure composites, some studies have also reported that the same may occur with light-cured composites when used in delayed activation techniques (Tay et al. 2001, 2003b) for the same reason described earlier.
Regarding the physical incompatibility, the presence of an oxygen-inhibited layer creates a hypertonic environment that osmotically draws fluid from the bonded hydrated dentin through the permeable adhesive layer (Tay et al. 2003a, 2004b). As simplified adhesives lack a solvent-free resin coating, water accumulates within the adhesive and also on the adhesive interface, known as water trees (Tay and Pashley 2003). This precludes a good contact with the restorative or luting material.
7.5 Insufficient Light Intensity During Polymerization
The light activation of dental materials within the root canals is a very difficult task, as light does not fully penetrate the length of the post space (Wu et al. 2009; Ho et al. 2011; Moazzami et al. 2012). Light transmission through fiber posts or even without fiber post exponentially reduces as the depth in the root canal increases (Goracci et al. 2008; Wu et al. 2009; Ho et al. 2011; Moazzami et al. 2012) (Fig. 7.3), making the achievement of attaining high bond strength throughout an entire root canal difficult. This explains why several studies reported inferior bonding performance in apical areas when using light-cured adhesives (Bouillaguet et al. 2003; Goracci et al. 2004; Akgungor and Akkayan 2006; Aksornmuang et al. 2007; Mallmann et al. 2007).
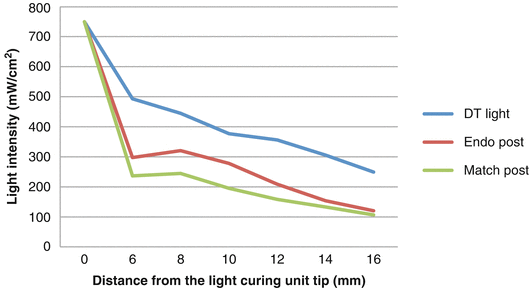

Fig. 7.3
Light attenuation through three different fiberglass post systems. The 0 mm represents the incisal region of a central incisor where the light intensity is 100 % (Adapted from Moazzami et al. (2012))
The limitation in the distance of light penetration results in a low degree of conversion of polymerizable dimethacrylate resin monomers. When the distance from the light source to the irradiation surface was increased, the degree of conversion of resin monomers decreased (Le Bell et al. 2003; Hayashi and Ebisu 2008).
It was recently demonstrated that even in the presence of translucent posts, the amount of light reaching the apical third of the root space might not be sufficient to effectively cure the cement at that level (Goracci et al. 2008). In the same investigation it was demonstrated that light transmission was not only prevented in carbon fiber posts but also significantly reduced in glassfiber posts marketed as being translucent, to the point that resin cement curing would be affected (Goracci et al. 2008; Ho et al. 2011).
7.6 Operator Experience
Bonding fiber posts to root canals is technically complicated. The quality of complex restorative protocols is highly susceptible to the operator’s experience. It has indeed been proven that there is variability in the results of adhesive procedures on coronal dentin that results from the operator experience (Sano et al. 1998; Miyazaki et al. 2000).
More recently the same was observed for fiber post cementation procedures. When full or simplified versions of ER adhesives were used to bond fiber posts to the root canals, reduced bond strength was observed for less experienced clinicians (Gomes et al. 2013). On the other hand, the role of operator was not significant when a self-adhesive cement was used.
Failure to follow the manufacturers’ recommendations and little knowledge about the confounding factors that affect root dentin bonding might well explain the reduced bonding of ER adhesives when applied by less experienced clinicians. The reduction in clinical steps as well as no need to keep the dentin substrate moist prior to material application might explain why self-adhesive cement was not sensitive to the operator’s skill. For less experienced operators, reducing the steps of the bonding procedure may be an important factor in obtaining a more reliable and stronger bond between resin and root dentin.
7.7 Cavity Configuration (C-Factor)
During polymerization of methacrylate-based materials, resin monomers get closer to one another, reducing the intermolecular spaces between them. This results in shrinkage stress that is sufficient to cause material debonding from root dentin. From a clinical standpoint, this stress leads to reduction of the post retention, gap formation, and potential for bacterial leakage at the adhesive interface.
Feilzer et al. (1987) reported that the shrinkage stress is related to the cavity configuration factor (C-factor), defined as the ratio of bonded to unbonded surface areas of the restoration. The higher the bonded area, the highest the extent of shrinkage stress and the damage to mechanical properties of the resin cement (Jongsma et al. 2012). Within the root canal, the cavity geometry is unfavorable and considered the worst scenario in achieving gap-free interfaces, since there are not enough unbounded surface areas for stress relief.
In comparative terms, while coronal restorations can have C-factors varying from 1 to 5, the estimated C-factor in post spaces may exceed 200 (Bouillaguet et al. 2003; Breschi et al. 2009). A way to minimize this unfavorable scenario is reducing the thickness of the adhesive resin cement layer inside a tight constrained cavity (root canal) that does not allow for stress relief by flow. The use of techniques that decrease the volume of material in the root canal (such as direct or indirect anatomic posts) may reduce the undesirable effects of polymerization shrinkage and yield higher bond strengths of fiber posts to root canal. It may also reduce the gap formation at the dentin-cement interface (Gomes et al. 2014).
Reducing the volume of resin cement may be difficult to achieve due to the shape mismatch between the circular fiber posts and the oval shape of many root canals or over instrumented canals (Fig. 7.4). Relining the prefabricated post with a composite resin outside the root canal before the cementation procedure may be useful in clinical practice to minimize the undesirable consequences of the constrained root canal cavity into the bonded interface (Faria-e-Silva et al. 2009; Macedo et al. 2010
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


