Chapter 9
Occlusion in Relation to Periodontal Disease
Aim
This chapter aims to outline the role of occlusion in periodontal disease and to identify clinical situations in which occlusal therapy may be indicated. Clinical techniques for occlusal therapy will be briefly discussed.
Outcome
Having read this chapter the practitioner should be able to recognise the influence of dynamic occlusal disharmonies on existing periodontal lesions and will have a practical understanding of how intervention may improve the prognosis of affected teeth.
Introduction
To function in occlusal harmony the masticatory apparatus comprising the teeth and supporting tissues, temporomandibular joints (TMJs) and associated neuromusculoskeletal structures must operate in an integrated and dynamic manner. Loss of integrated function or homoeostasis in response to functional demand may lead to the exacerbation of an existing periodontal condition.
In health, adaptive changes occur within the periodontium to functional occlusal forces. In periodontal disease, this adaptive capacity diminishes and previously reversible changes in bone morphology may become irreversible. The ability to predict how changes may influence dental treatment is important in forecasting treatment outcomes and the longer-term prognosis for the dentition.
Normal Occlusion and the Periodontium
Teeth transmit occlusal forces generated by mastication and swallowing. The magnitude of the occlusal force is controlled by the muscles of mastication. In normal physiological function, actions last only a few tenths of a second. The direction of the majority of occlusal forces is principally axial.
The periodontium is designed to resist axial force but some lateral stress can also be tolerated.
Primary Occlusal Trauma
When persistent horizontal forces exceed the physiological limit of adaptation the periodontal fibres are unable to absorb the force and localised tissue remodelling with widening of the periodontal membrane space occurs (Fig 9-1). In the absence of periodontal disease, this is termed primary occlusal trauma. In a reduced but healthy periodontium, such as may exist after treatment of periodontal disease, forces within the normal physiological range can exceed the periodontal tissues capacity for physiological adaptation. Under such circumstances the structure and adaptive capacity of the periodontium to occlusal loading permits a degree of physiological variation in tooth mobility. The term occlusal trauma is used to describe the lesions that may develop within the periodontal tissues from occlusal disharmonies.
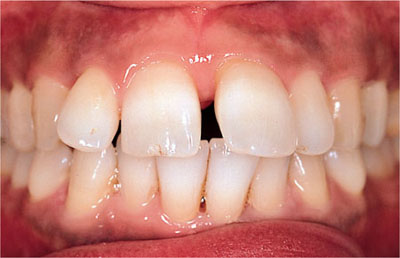
Fig 9-1 A clinical slide illustrating drifting with no periodontal disease.
Clinical Features of Primary Occlusal Trauma
-
No periodontitis.
-
Tooth mobility in the lateral plane.
-
Tooth wear (mild faceting or marked attrition) (Fig 9-2).
-
Fractures of the enamel or restorations.
-
Occlusal interferences (either from retruded contact position (RCP) to intercuspal position (ICP), or in lateral excursions/protrusive movements).
-
Ridging of buccal mucosa.
-
Indentations in lateral border of the tongue.
-
Reddening of the tip of the tongue.
-
Radiographically:
-
initially, widening of periodontal membrane space
-
funnel-shaped defect develops coronally in alveolus
-
hypercementosis
-
root resorption
-
secondary dentine laid down in the pulp chamber.
-
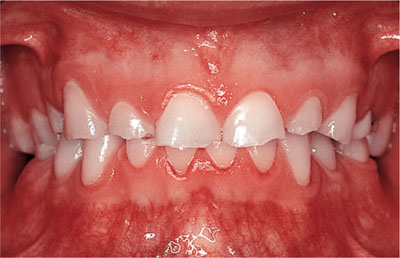
Fig 9-2 Attrition due to bruxing habit.
Management of Primary Occlusal Trauma
All pathological changes within the periodontium should be reversible and the key to successful management is to maintain periodontal health and to attempt to reduce/eliminate the excessive forces. This may involve selective grinding to remove interferences between RCP and ICP and in lateral excursion or protrusion; occlusal guards for nocturnal use (the ideal design is a “Michigan” type hard acrylic guard); and rarely splinting may be necessary to improve function (see below).
Secondary Occlusal Trauma (Trauma Within a Diseased Periodontium)
Current literature indicates that occlusal forces can cause changes in the alveolar bone and periodontal connective tissues both in the presence and in the absence of periodontitis. Secondary occlusal trauma refers to the presence of occlusal trauma in the presence of periodontitis. Secondary occlusal trauma can result in more rapid increases in tooth mobility, probing pocket depths and attachment loss. The periodontitis can be treated and periodontal health maintained without occlusal adjustment and in the presence of traumatic occlusal forces. Remember, occlusal forces do not initiate periodontitis. However, in the presence of pre-existing deep periodontal pocketing, occlusal forces may in some instances act as a co-factor resulting in an increase in the rate of periodontal disease progression. The clinical features of secondary occlusal trauma are the same as for primary occlusal trauma, but additionally teeth may drift out of position and radiologically “crescentic bone loss” and angular bone defects are characteristic (Fig 9-3). In this form of occlusal trauma loading forces are within the normal physiological range. Forces acting on a reduced and inflamed periodontal attachment apparatus are therefore able to modify periodontal disease progression.
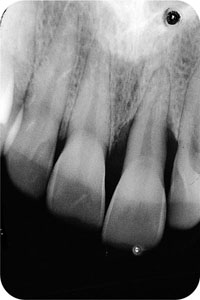
Fig 9-3 Radiograph demonstrating a crescentic pattern of bone loss 21.
Tooth mobility is a feature of occlusal overloading. However, factors other than occlusal loading contribute to the clinical observation of tooth mobility. Tooth mobility is also influenced by:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


