Chapter 10
Periodontal–Restorative Interface
Aim
This final chapter aims to examine the relationship between periodontal health and aspects of operative dentistry and endodontic and prosthodontic (fixed or removable) therapy.
Outcome
Having read this chapter the practitioner will appreciate why the highest standards of restorative treatment require a healthy and well-maintained periodontium with minimal gingival inflammation to facilitate good plaque control around dental restorations and appliances and thereby enhance longer-term success.
Introduction
The oral cavity is an open growth system in which most bacteria can only survive if they adhere to “non-shedding” dental hard surfaces such as teeth, restorations, dental implants or prostheses (see Chapple and Gilbert 2002). Bacterial adhesion occurs in four phases: transport to the surface, initial adhesion (which has a reversible and an irreversible stage), attachment by specific interactions and eventual colonisation. During the process of bacterial adhesion, the roughness and the free energy of the surfaces play a significant role in determining whether bacteria adhere successfully or not. A reduction in surface roughness reduces both plaque formation and maturation. A reduction in free surface energy of the substratum will result in a decrease in the plaque growth rate, a decrease in plaque retention capacity of the surface and changes in the bacterial species colonising the surface.
Intracoronal Restorations
Choice of material
The presence of any restoration in the mouth, even if of ideal quality, will increase the risk of plaque retention and, as a consequence, periodontal disease. This is for two reasons: no restorative material has a surface energy as low as natural enamel and junctions between the tooth and restoration will retain plaque.
Surface roughness is an intrinsic feature of dental materials, which can be altered by polishing, scaling, brushing, condensing, glazing and finishing. A threshold surface roughness of 0.2 microns exists above which bacterial adhesion will increase. It is essential to follow manufacturer’s directions for the handling and finishing of dental materials.
Whilst for anterior restorations composite materials are an aesthetic necessity, care is required in the selection of materials for posterior restorations. The surface texture of materials contributes to plaque retention (Fig 10-1 a to c). Polished gold or glazed porcelain result in minimum plaque retention, but with function even highly polished surfaces undergo wear and become more plaque retentive.

Fig 10-1 Scanning electron microscope views of (a) composite (b) amalgam and (c) gold showing different surface characteristics.
Amalgam is weakened by polishing and access to interproximal sites is difficult to achieve. The contouring of restorations and removal of marginal overhangs using diamond tips within reciprocating handpieces and conventional finishing burs are sufficient to permit adequate tooth cleaning and reduce interproximal plaque levels (see Chapple and Gilbert 2002). Polishing of amalgam restorations using rubber discs, rubber tips and polishing pastes does not result in further improvement in gingival health.
Composites can initially be finished to a suitable smooth surface texture. However, this soon deteriorates such that after six months the surface contour equates to an unfinished restoration. Plaque and gingival indices increase on older composite restorations as surface roughness and marginal seal deteriorate.
Contour
It is essential to avoid overcontouring. Bulbous restorations with wide contact areas render interproximal cleaning impossible. The concept of a flat “emergence profile” (Fig 10-2) mimicking the natural tooth contour should be followed. The use of matrix bands and wedges (Fig 10-3) will reduce the incidence of overhanging restorations (Fig 10-4). Always check that access is provided for interproximal cleaning aids. Overcontouring with direct composite additions to, for example, close spacing has been shown to increase plaque and gingival indices and probing pocket depth.
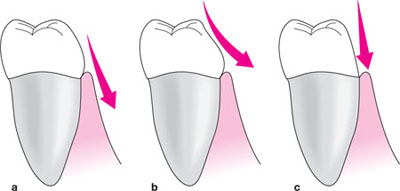
Fig 10-2 A flat emergence profile as shown in (a) mirrors natural tooth form and protects from plaque trapping that occurs in over contoured restorations (b) or physical trauma as in (c).
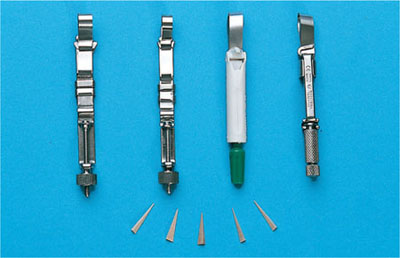
Fig 10-3 Various matrix bands and wedges used to prevent ledges on plastic restorations.
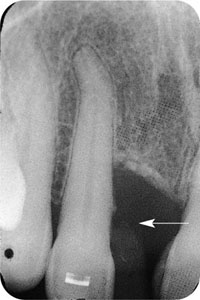
Fig 10-4 The mesial margin of 12 has been overbuilt with composite and as a result bone loss has occurred.
Marginal seal
Composite restorations are prone to marginal gap formation due to polymerisation shrinkage. This can be reduced by the incremental placement of restorations. Use of mechanical packers can improve marginal adaptation in restorations of dental amalgam.
Whenever feasible, restorations should terminate above the free margin of the gingiva. Every restoration terminating in the immediate vicinity of, or in contact with, surrounding soft tissue is a potential irritant to that tissue and increases the chance of precipitating periodontal disease. Patients with subgingival restorations will require regular dental hygiene maintenance programmes. Recurrent caries is also related to poor periodontal status (Fig 10-5).
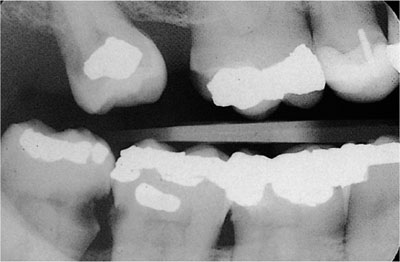
Fig 10-5 The radiograph shows recurrent caries 47, 46 and associated inter-proximal bone loss.
Crowns and veneers
Material
Acrylic crowns retain plaque to a greater degree than cast gold and metal ceramic crowns. Ceramic crowns show the least plaque retention.
Margins
Crown and veneer margins are best placed in a supragingival location. Where crown height is reduced, consider crown-lengthening surgery to increase retention rather than placing margins in a subgingival location (Fig 10-6). Should crown margins be placed subgingivally, plaque retention will occur with risk of further recession. Subsequent exposure of crown margins gives a poor aesthetic outcome. If crown margins are subgingival, plaque retention and gingivitis will cause apical migration of the junctional epithelium and subsequent loss of coronal periodontal ligament fibres.
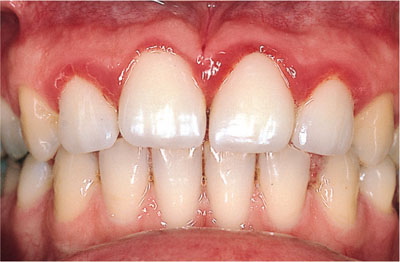
Fig 10-6 Crown margins are subgingival and inaccessible for plaque control. Gingivitis is present.
Gargiulo and colleagues proposed the existence of an innate “biological width”, i.e. a minimum distance between the base of the sulcus and the most coronal periodontal fibres and alveolar bone. Based on studies of 30 cadavers, this was 2.04 mm (JE 0.97 mm, connective tissue 1.07 mm) and represents the sum of the epithelial and connective tissue attachments (Fig 10-7). It is generally accepted that restorations whose margins are placed within this biological width will lead to gingival inflammation and connective tissue and bone loss. The closer a restoration margin is to the JE the more likely gingival inflammation is. The biological width described by Gargiulo et al. did not include the gingival sulcus and therefore two further recommendations have been made to help guide the clinician where to place the restoration margin:
-
Ingber et al. recommended a minimal distance of 3 mm from the restoration margin to the alveolar crest, to accomodate the biological width.
-
Nevins and Skurow advised that the restoration margin should not be further than 0.5–1 mm below the gingival margin.
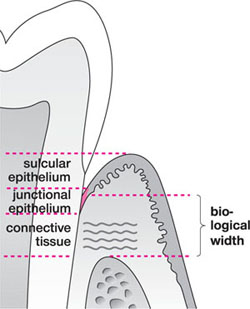
Fig 10-7 The traditional concept of the biological width is the connective tissue and epithelial attachment. Block recommends that measures be taken from the gingival margin and the biological distance be set at 3 mm (gingival margin to alveolar crest).
Block, who also recommended that measures be made from the gingival margin rather than the base of the sulcus/JE because clinicians could not visualise this area, also supported the 3 mm distance. Where the margin encroached upon this distance, crown-lengthening surgery was indicated (Fig 10-8 a and b). The margins of cast ceramic restorations can be damaged during removal of investment materials and finishing. Resultant increased marginal discrepancies and eventual dissolution of cement can lead to increased plaque retention, caries and increased periodontitis.
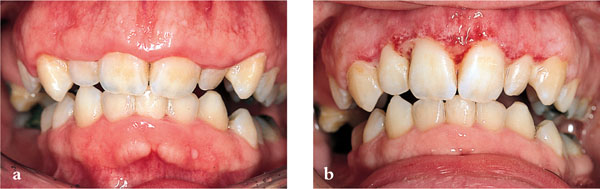
Fig 10-8 (a) Short clinical crowns. (b) 1 week following crown lengthening surgery (tissues still healing).
Contour
When planning preparations for crowns and bridges, always allow adequate space for the dental technician to produce a flat emergence profile, wide interdental spaces and point contacts interproximally (Fig 10-9). These features will r/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


