Chapter 8
Orthodontics and Periodontal Health
Aim
This chapter aims to consider the relationship between malocclusion and periodontal health and disease states and to identify the potential risks to periodontal health that orthodontic treatment may introduce.
Outcome
At the end of this chapter the practitioner should be able to identify patients in whom orthodontic treatment may be a risk to their periodontal health and be familiar with options for managing such cases. Understanding such concepts should promote good practice in the periodontal screening and management of orthodontic patients and enable the appropriate selection of periodontal patients suitable for orthodontic management.
Introduction
When considering the suitability of a patient for orthodontic treatment, the practitioner should consider the following questions:
-
Does a malocclusion cause periodontitis?
-
Can orthodontic treatment damage the periodontal tissues?
-
Can orthodontic treatment be considered to manage drifting that has resulted from reduced periodontal support?
Malocclusion as a Risk Factor for Periodontitis
The concept of a “normal occlusion” does not necessarily mean a perfect Class I occlusion. Any occlusion which functions in the absence of disease, but which may also have features of malocclusion that are adequately accommodated by neuromuscular adaptation, is considered normal.
It has been estimated that 60–75% of adults in the UK have a malocclusion. Currently some 15% of orthodontic treatment is provided for adults and yet less than 15% of the population will present with severe periodontitis. Therefore a large number of adults with malocclusion appear to be free from periodontal disease. However, a proportion of adults will have both malocclusion and periodontitis and commencing orthodontic therapy in the presence of an unstable periodontium is a recipe for disaster. When the status of the periodontium is compared in teeth with and without premature occlusal contacts, no differences are found. This is evidence to suggest that malocclusion is not a primary factor in the development of a periodontal pocket.
Oral hygiene standards are a significant factor in predicting future risk of periodontitis rather than the presence of crowding and malocclusion. Where oral hygiene is good there is a minimal increase in the risk of periodontitis regardless of occlusal relationships (Fig 8-1). If oral hygiene is poor, correction of tooth alignment will not improve oral hygiene and therefore will not reduce the incidence of periodontal diseases (Fig 8-2). For patients with average oral hygiene, correction of crowding in the posterior segments may reduce the risk of periodontitis by facilitating better oral hygiene.
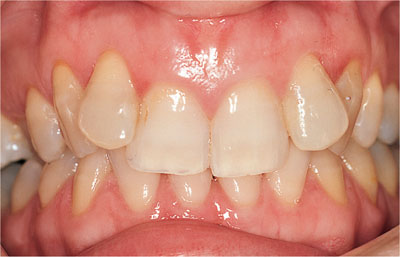
Fig 8-1 This clinical slide illustrates a patient with malocclusion. There is good oral hygiene and as a result the periodontal tissues are healthy.
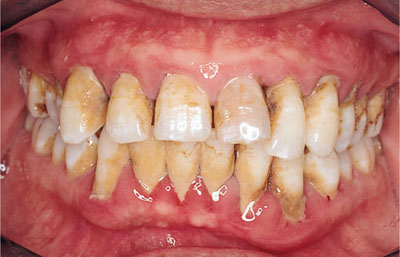
Fig 8-2 Despite a good occlusal form this patient with poor oral hygiene shows features of periodontal breakdown.
Crowded sites harbour increased quantities of supragingival plaque and raised levels of putative periodontal pathogens in subgingival locations. Correction of the malocclusion may, however, reduce levels of plaque accumulation by facilitating improved oral hygiene and reducing the risk of periodontitis by limiting the environmental risk factor of plaque accumulation. However, in a patient who is genetically susceptible to periodontitis, it is important to remember that orthodontic correction of a malocclusion will not alter their genetic susceptibility to periodontal bone loss.
The decision-making is complex, because it is essential to treat active periodontal disease and achieve stability with improved plaque control before embarking upon orthodontic therapy. Therefore, orthodontic realignment is only of benefit in cases of long-term periodontal stability in highly motivated patients. It should only be considered if patients demonstrate a stable periodontium with no progressive attachment loss for at least 9–12 months after active periodontal therapy.
Adverse Effects of Or/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


